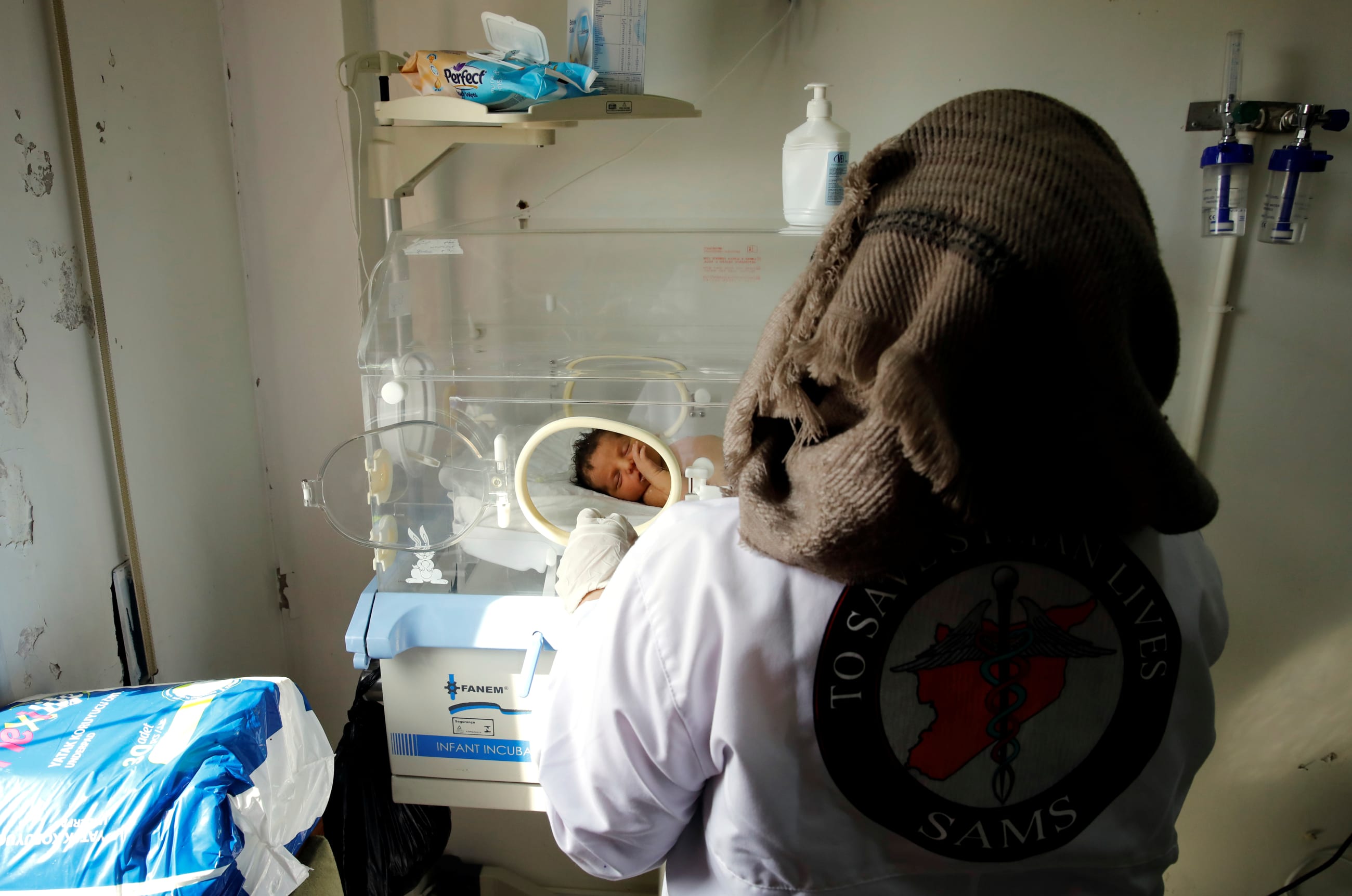
Every month, ophthalmologist Ahmad Alsyed Ali sees at least one child teetering on the edge of blindness. As much as he wants to treat them, by the time these children are referred to his office, it is often too late. Many of his patients face a lifetime of severely restricted vision—or, in some cases, complete blindness. Ali's task is to explain this reality to devastated parents whose only remaining option is to seek costly specialty care in the private sector or outside the country.
"The situation for these parents is heartbreaking," he said. "Especially because the diagnosis comes too late for treatment."
Ali works in Idlib, Syria, a country that recently marked the one-year anniversary of its emergence from more than a decade of civil war. In the war's wake, the health-care system remains fragile, as certain areas are held together by a patchwork of volunteer and nongovernmental organizations (NGOs). Long oriented toward responding to acute wartime crises, the system has struggled to provide routine health screenings and primary care, leaving millions of patients to fall through the cracks.
The children Ali sees are among those overlooked. Most suffer from retinopathy of prematurity (ROP), an eye disease that affects up to about 30% of premature infants, with severe disease occurring in roughly 5 to 10%. With ROP, abnormal blood vessels grow over the retina—the light-sensitive tissue at the back of the eye—blocking visual signals from reaching the brain. Outcomes vary, but in severe cases, the condition can cause permanent blindness.
Early diagnosis and treatment are critical to preventing vision loss
Early diagnosis and treatment are critical to preventing vision loss. Although more neonatal intensive care units (NICUs) are emerging across Syria as the health-care system rebuilds, the country lacks a coordinated system to screen for ROP. This scenario means that while more premature babies are surviving, there is limited infrastructure to detect conditions early. This gap has fueled the growing number of ROP cases involving significant vision loss and irreversible blindness that Ali sees in his clinic.
Syrian American ophthalmologists in the United States are now banding together to create a solution. Working through the Syrian American Medical Society (SAMS) and in coordination with the Syrian government, they are building a pipeline for the diagnosis and treatment of ROP. As NICUs across Syria continue to improve, the group is establishing screening systems for ROP cases, said Ahmad Al-Moujahed, a retina specialist at Stanford University and one of the program's organizers..
A Blueprint for Syria
After the fall of the Assad regime, Al-Moujahed wanted to give back to his homeland by strengthening its ophthalmologic capacity. As he began brainstorming high-impact projects that would not require extensive infrastructure, he landed on ROP as a promising target.
He had a blueprint in mind. At Stanford University, where he is an attending physician, a telemedicine program allows technicians or physicians to photograph a premature infant's retina and transmit the images to specialists for evaluation. The program currently operates across California, Indiana, and Nevada. Last year, a similar model launched in Ghana.
As part of that program, trained technicians use portable retinal cameras to photograph premature infants' retinas. The images are then uploaded and reviewed remotely by retinal specialists, who determine whether the baby needs monitoring or treatment.
The system allows hospitals without pediatric ophthalmologists to screen infants and quickly connect with experts, expanding access to care. Al-Moujahed believed this model could be used to treat ROP in Syria.
"You can inject medicine [to stop the abnormal blood vessel growth] inside the eye—very cheap and very easy to do. A physician can do it in the NICU without sedation or anesthesia, and prevent blindness in these babies and protect their vision for the rest of their lives."
After settling on ROP in January 2025, Al-Moujahed formed a multidisciplinary committee of Syrian and Syrian American ophthalmologists and NICU physicians, working through the SAMS. Together, they developed a comprehensive national ROP protocol tailored to Syria's low-resource setting. Drawing on screening models used in India [PDF], Turkey [PDF], and several African countries, the guidelines expand eligibility criteria—screening infants born at 34 weeks' gestation or earlier and weighing up to about 2 kilograms (4.4 pounds), compared with the 30-week and 1.5-kilogram (3.3-pound) thresholds commonly used in wealthier countries, such as the United States. The broader criteria were designed to maximize screening in settings where neonatal care is inconsistent—and to account for babies who appear mature at birth but could still develop the disease. Screening infants while they are still hospitalized also helps capture those who might miss follow-up care after discharge.

Al-Moujahed and his colleagues finished drafting the protocol in April 2025, just ahead of a large summer medical mission organized by SAMS, where it was presented. The effort brought more than 100 volunteer medical professionals from multiple specialties to Syria. During that visit, Al-Moujahed and Marwan Abdulaal, an ophthalmologist at the Cincinnati Eye Institute, led a multiday training workshop in Damascus that combined lectures, case discussions, and hands-on screening in NICUs. Dozens of ophthalmologists attended the sessions, and at least five physicians received practical training in ROP diagnosis and treatment.
"We had almost more than 70 or 80 eye doctors in the same room, just coming to learn about this disease and to learn how to treat it," said Abdulaal. "You could feel the interest."
Following the training, a locally based retina specialist in Damascus volunteered to begin weekly bedside ROP screenings at a major hospital—marking the first time such screening has been conducted routinely at that facility.
Overcoming Battered Infrastructure
This focus on primary prevention—anticipating needs before a crisis emerges—marks a step forward as Syria's health-care system begins to transition away from emergency stopgaps. Even so, leaders will have their work cut out for them. Syria's broader health-care landscape remains deeply uneven, shaped by years of conflict and disruption.
Most but not all parts of Syria's health-care system are in a recovery phase, said Aula Abbara, a cofounder of the Syria Public Health Network and an honorary senior clinical lecturer at Imperial College London who, since 2012, has worked in the humanitarian response in Syria. "The fragmentation of Syria's health system during the conflict meant that at least four subnational health systems existed until the fall of the regime in December 2024."
These regions faced different challenges with resourcing, governance, leadership, maintaining workforces, and having the resilience to meet health needs. As Syria recovers, equitable distribution of health resources is crucial to counteract what happened during the former regime. The consequences of uneven and incomplete recovery are visible across the country. According to Abbara, Syria's health-care capacity is stronger in urban than peri-urban or rural areas. In northwest Syria, local communities and NGOs built a fragile health system after the Syrian government withdrew early in the conflict—but once the regime fell, onlookers saw that it was more functional in many respects that in former regime-held areas. Nationally, 57% of Syria's hospitals were operational as of March 2025, and nearly one-third of Syria's buildings [PDF] have been damaged or destroyed. Estimates suggest that up to 70% of the country's health-care workforce is now overseas, having fled years earlier.
"When I arrived in December 2024, shortly after the regime fell in Damascus, the hospitals I visited had equipment that looked like it hadn't been replaced in 20 or 30 years," said Abbara. "They were archaic. They were broken."
Ophthalmology has suffered from those broader system failures. Last October, Al-Moujahed published an analysis examining the state of ophthalmic care in Syria. He and his coauthors contacted hospitals across the country to assess the condition of their infrastructure. What they found was a widespread shortage of functional ophthalmic equipment.
Among the hospitals that responded, many lacked a working slit lamp, a basic diagnostic tool that provides ophthalmologists a three-dimensional view of the eye and its underlying structures. In cases where one was available, it was often outdated. Other essential instruments, including optical coherence tomography machines, tonometers, and visual field perimeters, were frequently unavailable or in disrepair, sharply limiting clinicians' ability to diagnose and monitor glaucoma and retinal disease.
"You just can't adapt, even if you are very innovative," said Al-Moujahed. "You need machines, especially when we're talking about the retina. . . and it's a sad reality that patients don't get care most of the time, unless they have the money to go to the private hospital."
Next, Al-Moujahed and Abdulaal will need to secure funding to hire a coordinator who can manage follow-up care for infants diagnosed with ROP and babies who were discharged from NICUs before their screening could be completed.
They plan to establish a council of pediatric ophthalmologists based in the United States, Europe, and Syria to identify physicians interested in pursuing training in ROP management. At the same time, the group is seeking funds to purchase fundus cameras—devices that allow physicians and technicians in the field to photograph the eyes of infants with suspected ROP—and send the images to specialists in the United States to support diagnosis and guide treatment plans.
Training local ophthalmologists, hiring coordinators, and purchasing fundus cameras are essential to turning the ROP protocol into a self-sustaining program, instead of a one-off effort dependent on outside volunteers. Al-Moujahed and his partners at SAMS estimate initial costs of $200,000 for this endeavor, which they are currently seeking to raise through crowdfunding. Thus far, they have secured enough funding for two coordinators and two cameras.
"Once you transition to being a self-sustained project, you can show how huge the impact is," Al-Moujahed said.
Another pillar of the program's sustainability is the involvement of the Syrian government. The two ministries that oversee health care in Syria—the Ministry of Health and the Ministry of Higher Education—have expressed support for the ROP initiative to Al-Moujahed and Abdulaal. Once the program becomes fully operational, the national health policy will incorporate the program, said Abdulaal.