In an outbreak response, speed is life. Global health financing mechanisms need to address the challenges countries face in responding rapidly to health threats. The field has witnessed additional investments in pandemic preparedness and health systems strengthening since COVID-19, but the focus is often on the amount of funds rather than their targeted delivery at the right time and place and before outbreaks are even declared.
Global health faces a shifting financial development landscape. Delegates at the Group of Twenty session in September 2023 called for significant reform of financial institutions, and 2024 is the year that critical decisions on global health fundraising will be made. Amid those shifts is an opportunity both to improve the way money is disbursed and used on the ground and to fill critical needs in emergency funding. In addition to replenishing funds for global institutions, governments also need to meet their domestic health spending commitments—which includes domestic funding tailored for speed and sustainability.
Having access to flexible funds changes the game for public health officials working on the ground. Typically, they need to make standalone requests for funds before they can deploy response teams; meanwhile, the disease is left to spread unchecked.
Flexible funding allocated in advance is critical to fulfill the urgent, operational support needs common in the early stages of any response: transportation to get boots on the ground, access to internet and cell phone credit, and personal protective equipment to keep workers safe.
Never was the need for rapid, predictable funding more apparent than during outbreaks of Ebola in Democratic Republic of Congo (DRC) between 2018 and 2022. Whereas the 2018 outbreak lasted two years, more recent episodes in 2021 and 2022 were over in a matter of months. What changed? The time it took to detect the first cases of Ebola and begin effective response efforts shortened significantly.
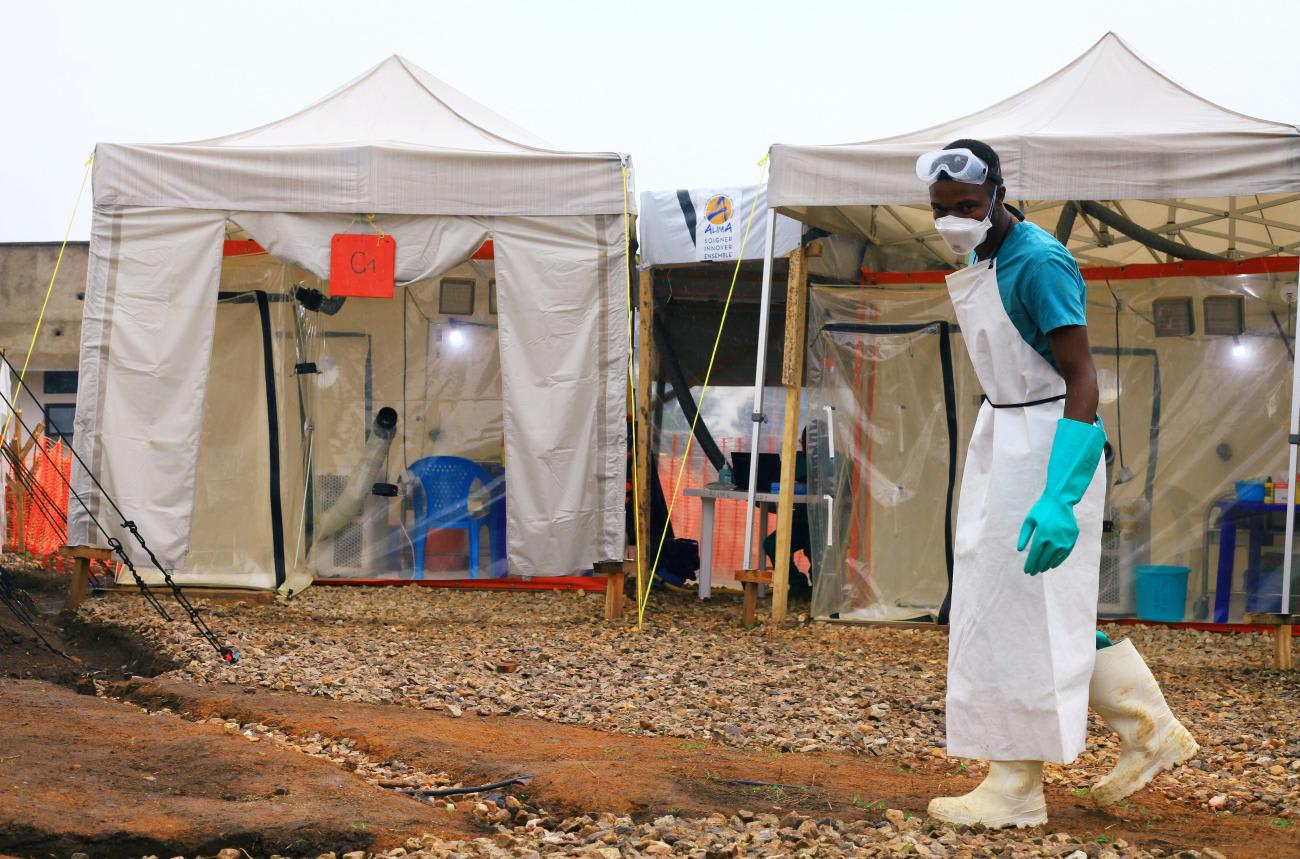
During DRC's 2018 Ebola outbreak, no suspected cases were identified and no alerts were issued for two months, allowing the disease to spread rapidly throughout the country. By contrast, in August 2022, public health responders were able to investigate and respond to the outbreak in just three days. Six weeks later, the outbreak was declared over with only one confirmed case. This successful response was possible due to excellent work of response teams supported by the rapid release of emergency funds.
Stopping health threats before they become deadlier—and costlier—epidemics requires the kind of fast action taken in DRC's 2022 Ebola response. Countries need to be able to identify outbreaks early, report them quicky, and respond rapidly to stop their spread. Unfortunately, most disaster or response funding mechanisms aren't set up to facilitate taking these steps in the quick succession needed to prevent epidemics.
Pilots of rapid outbreak financing (ROF) mechanisms conducted by Resolve to Save Lives (RTSL) have shown that these funds don't need to be substantial. Resolving global health issues often costs millions—but RTSL has found that spending $5,000 at the first sign of an outbreak can eliminate the need to spend tens or hundreds of thousands to control an epidemic later, or billions to address far-reaching social and economic impacts. Having fast access to funds that allow for flexible spending at the start of an outbreak is critical.
A Field Test
Although countries have improved their ability to detect more outbreaks earlier, funding constraints often prevent them from moving quickly beyond initial identification and reporting to mounting a full investigation, verification, and response.
We tested the ROF approach with our partners in several African countries and found that it not only filled a critical gap in emergency funding, but also significantly reduced the time from outbreak detection to verification and response.
Countries need to be able to identify outbreaks early, report them quicky, and respond rapidly to stop their spread
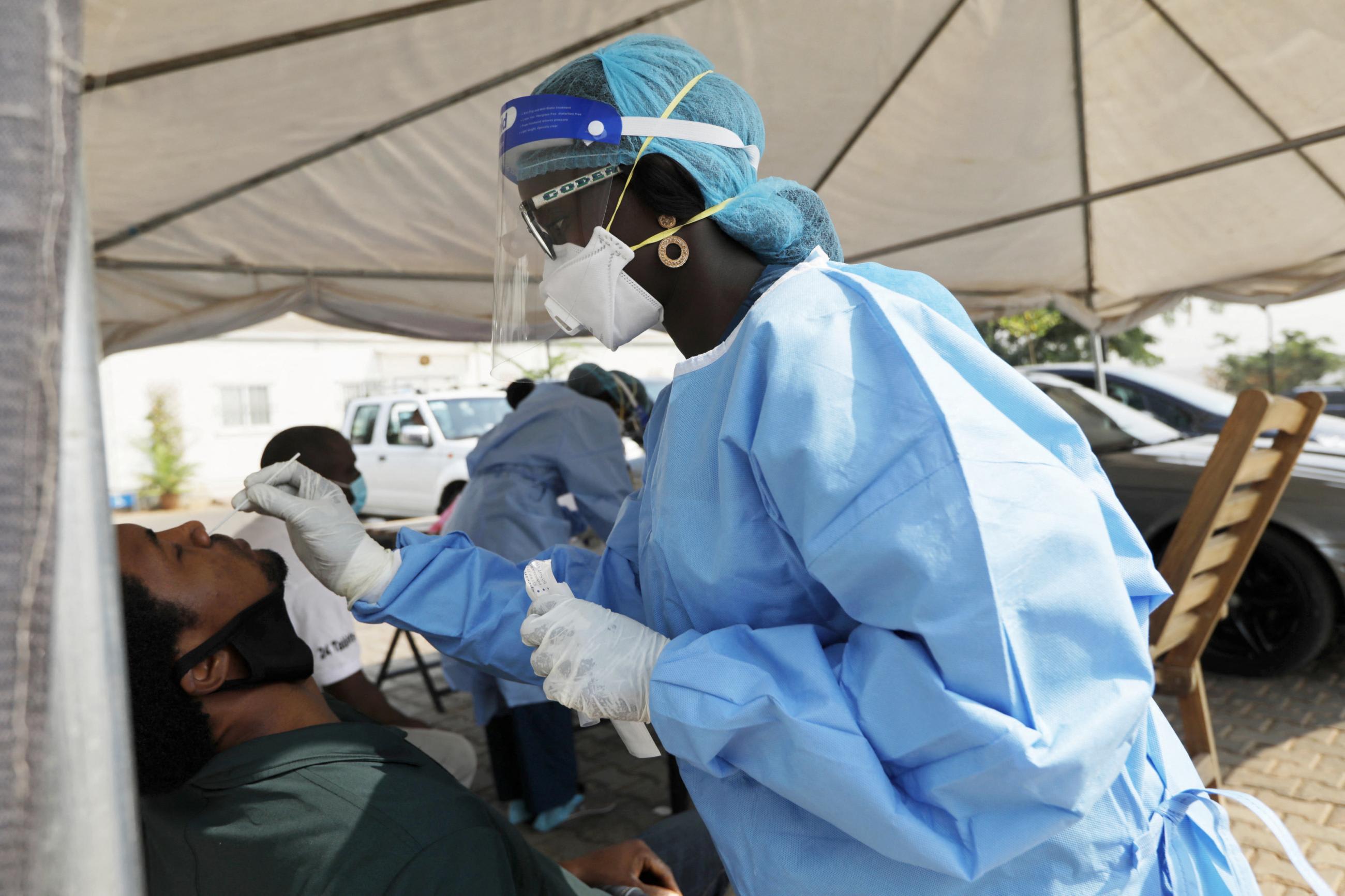
In Nigeria, RTSL partnered with the African Field Epidemiology Network and Nigeria Centre for Disease Control and Prevention (NCDC) to establish an ROF mechanism that allowed for disbursement of funds within 48 hours of request. When COVID-19 hit, NCDC was able to use ROF to begin preparedness and response activities before the disease was officially declared a pandemic. This rapid funding enabled the deployment of more than 200 personnel to initiate response efforts in 34 of Nigeria's 36 states and support emergency operations and disease surveillance across the country.
But those successes went beyond COVID-19, equipping NCDC with the resources to respond to 15 additional outbreaks in 2019 and 2020. During a measles outbreak in June 2019, the NCDC was able to deploy a rapid response team in less than 72 hours to investigate and track cases. Just three months later, the outbreak ended with 275 suspected cases and 18 deaths among confirmed cases—much less than in previous outbreaks. Since its start in March 2019, this funding mechanism also supported national responses to several outbreaks of mpox, measles, yellow fever, and Lassa fever.
Implementing ROF has shown significant reduction in response times—from an average of six days to just two in Nigeria—and a subsequent rapid containment of deadly diseases.
The world can take lessons from Nigeria, which was able to leverage the successes of ROF to secure additional funds and expand the availability of ROF to the subnational level as well as start the transition to government ownership and financing. Because most disease outbreaks are identified by clinicians working with communities, availability of rapid funding at local levels will further strengthen the ability to find and respond to new health threats.
An essential element of pandemic preparedness planning is giving countries the tools they need to respond to events before they become outbreaks. Communities should push governments, multilateral development banks, and global health organizations to make fast, flexible funds available to investigate and prevent outbreaks. It could require new mechanisms that balance speed and financial accountability, but our organization has shown that it is possible—and critical for saving lives.