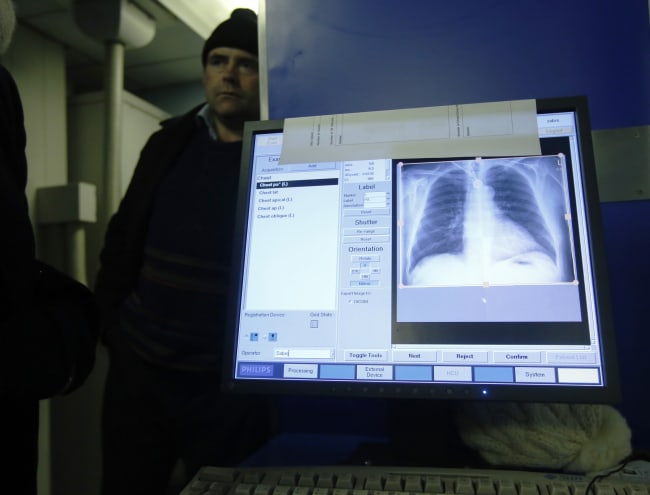
Entrepreneur, innovator, writer, and social activist Bright Simons has spent more than a decade as a "technology systems thinker." In 2007, he founded mPedigree, and developed a technology aimed at protecting people in Ghana, his home country, from drug counterfeiters, that now boasts an international footprint and has expanded into other sectors, such as agriculture and cosmetics. The Harvard Kennedy School graduate is also Honorary Africa Vice President of Ghana-based IMANI Centre for Policy and Education, a leading African think tank. Simons recently spoke with Think Global Health about his life's work, including his efforts to build an "ecosystem" for cold chain distribution of COVID-19 vaccines across Africa.
□ □ □ □ □ □ □ □ □ □ □ □ □
Think Global Health: What's happening with COVID-19 vaccine acquisition and distribution right now in sub-Saharan Africa?
Bright Simons: Right now, we have three levels. We've got a desperate government push to acquire vaccines from wherever they can get them. There are a number of initiatives in this regard. There are those where vaccines are provided for free through COVAX. Then there are arrangements that require countries to pay for vaccines, but they get the money through a concessional facility such as the World Bank or regional development banks.
"In the United States, it's run-of-the-mill to go into a CVS and get a vaccine, but it's not like that in most parts of the world"
The African Union has a program called Avatt that helps countries access vaccines—mostly Johnson & Johnson's COVID-19 vaccine—through the vaccine maker. And you've got the donated vaccines from global north countries that overstocked, who now want to give some of those stocks away. But those donations typically go through a distribution scheme like COVAX, too. I'm not sure they'll go through any of the regional programs. Very few countries can deliver vaccines directly because of the cold chain implications. It requires a specialized supply chain.
In the United States, it's run-of-the-mill to go into a CVS and get a vaccine, but it's not like that in most parts of the world. Even in Europe, you don't see the same degree to which the United States has decentralized and democratized access to adult vaccination.
Think Global Health: Are there regions in Africa that stand out in terms of challenges to cold chain distribution?
Bright Simons: Right now we have to do adult vaccination on a very large scale and reach far more people than we've ever done in world history. And that has an impact everywhere. Infant vaccination is the infrastructure that is being leveraged for this adult mass vaccination campaign. But in those places in Africa where infant vaccination is already a challenge, the challenge is likely to be compounded several fold. If you look at the African landscape, there are countries that—even for infant vaccination—don't have up to 90 percent coverage. The Democratic Republic of Congo (DRC), for instance. Vaccination coverage there has been a perennial problem. Ethiopia has been a problem on and off, though it has improved significantly. Parts of Malawi, too. Adult vaccination compounds this legacy challenge several fold because you have a lot more people, vaccines are widely distributed, and you don't have the same degree of routinization that you have with infant vaccination.

So what happened was that as the logistics started to ramp up in the West and in India, and the time came for the vaccines to be delivered, some countries had not yet ramped up and created the local infrastructure to be able to support adult vaccination on the scale which was required. Countries like DRC and Malawi actually had to give back some of the vaccines because they could not administer all of the vaccines that were distributed in a timely manner. In the case of DRC it was quite shocking because initially, it was over a concern about the safety of the vaccines. Eventually that was overcome. It took about a month, though. Then it became clear that some of the vaccines were very quickly nearing their expiration date. So the African Union and others and the World Health Organization repurposed them. They redirected some of those vaccines to countries they believed were ready. Some of those countries though found out that the expiration dates were much closer than initially believed and hundreds of thousands of vaccines still had to be destroyed—maybe millions—and could not be used due to supply chain issues. In Malawi, they had to destroy some of them because they could not get to them before they expired.
"Economics and epidemiology are somewhat conjoined"
Then you have the issues around coordinating first and second shots—at optimal intervals—and making sure people are aware. And there was guidance not to mix up vaccine brands and that means you needed record-keeping that is really top notch. People really needed a simpler vaccine regimen. The Johnson & Johnson offering became very interesting because of its single dose, but now we're seeing that you may need a booster shot, or you may require periodic boosting.
Think Global Health: So it's really becoming about the economics of vaccination?
Bright Simons: Because of the amount of infrastructure repurposing that is needed to deliver vaccines within such a short time, the economic issues need to be addressed. Some of this repurposing involves building a whole new infrastructure to support mRNA vaccine production and it will be very hard for investors to recover costs unless you take into consideration that, at the very least, for the next three years, getting regular boosters would become part of the landscape, ensuring investors of sustained demand. If we're going to reduce inequity, we have to produce more vaccines. If we have to produce more, we have to build more infrastructure, like factories dedicated to handling fill and finish. Money's not free right? The investment you have to pump into this stuff needs to be recovered. And if that is the case, it makes sense that either the government has to pay for all of the upfront capex completely or you get the private sector involved.
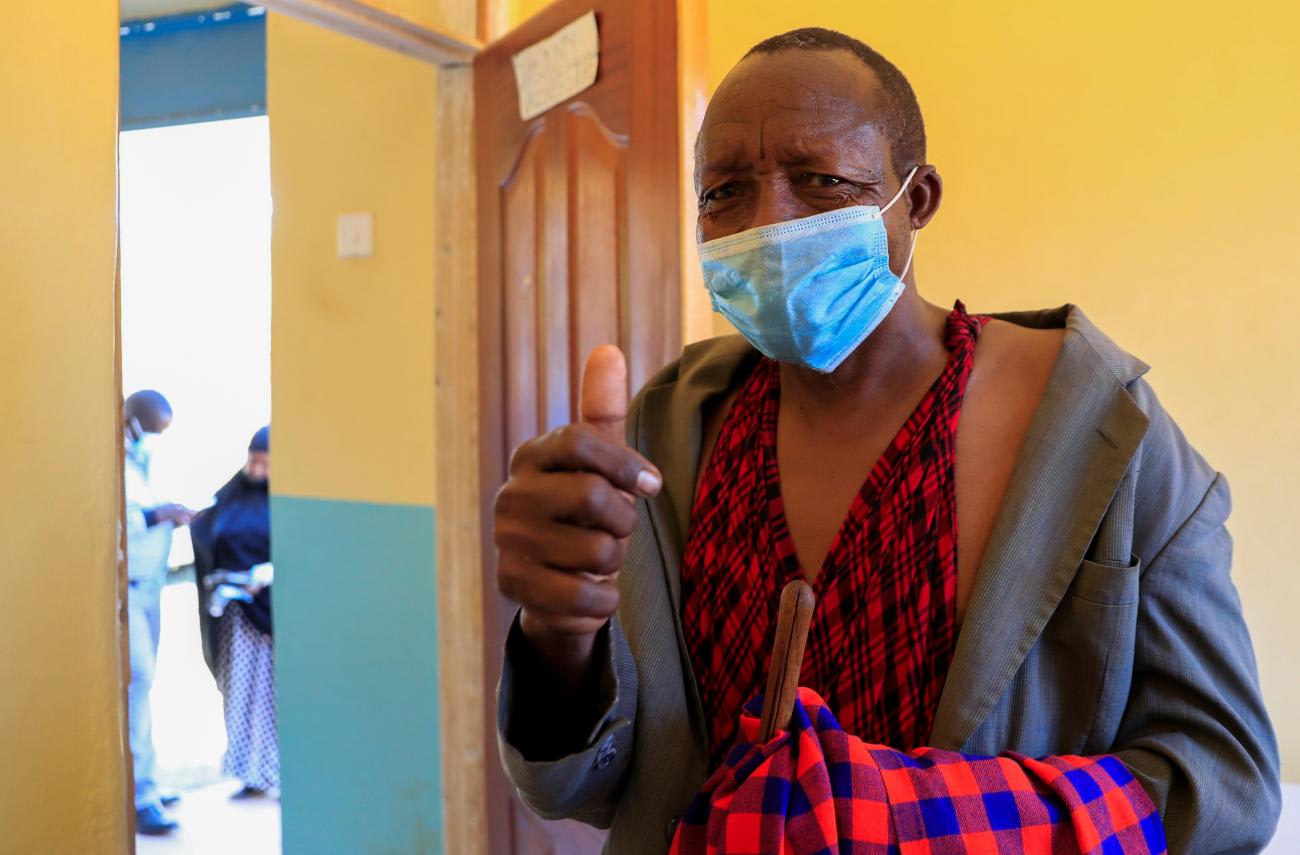
The nature of biomedical production infrastructure is that it's not usually government-owned in most parts of the world. So, private people have to put up the infrastructure, which means therefore, that the economics and the epidemiology are somewhat conjoined or interconnected in requiring that we have these regular boosters. Boosters may also become more personalized—you may need to be tested for antibodies and if your antibodies are low then you go to get a booster shot.
Think Global Health: Do you see the government and private companies in Africa working together more synergistically in the future when it comes to vaccines?
Bright Simons: In the United States, the public-private interplay has been pretty straightforward. The government literally distributes the vaccine to the private sector through drug stores like Walmart and CVS, and people go there and as far as I understand it, they can get it for free.
That public-private sector interplay in Africa is going to be a lot more challenging because the government is not known for paying its bills on time. If you have the private sector distribute it, but the government pays for it, there are a whole lot of trust related issues—corruption, diversion, etcetera—that could get in the way. So, the thinking was that people should just pay for it, maybe at controlled prices. And then the poor should depend on government hospitals. The rich, for convenience, could go into the private pharmacies and buy it. Kenya was the first to attempt to do this. They said, here's what we're going to do, we're going to get some vaccines for free through COVAX and then we are going to buy an additional quantity of vaccines and negotiate a price. We will give those out to people in the public facilities—primarily clinics and makeshift pop-up vaccine centers—and it would require some curating and some rationing. They would be paid for by the government who set up the pop-ups. It's been happening periodically and it's fairly efficient. Right now, they prioritize urban areas because the risk of COVID infection so far appears to be higher in urban areas.
"It takes power to get things done, but innovators don't always have power"
So, the Kenyans then said, okay, we will give doses for free through the public health system but we will also allow private clinics and hospitals and employer groups and the like to sell vaccines at whatever price they want. This was around March or February 2021, so a bunch of companies started to import vaccines. You couldn't get the western vaccines because those were pre-sold long ago, and the producers had these special relationships with GAVI and the Global Fund. Instead, we had Chinese and Russian vaccines—those vaccines were available on the open market so you could go buy them and bring them in. Some companies started to bring those into Kenya. But the prices were ridiculous. They started at $80.
In the case of Kenya, though, the government became alarmed when they got intelligence that fake vaccines were being circulated in parts of Africa, and they blocked imports and revised the whole policy. They stopped private sector importers from being able to bring vaccines in at all.
Think Global Health: This leads to what you're trying to do—to set up a system of safe distribution of COVID-19 vaccines?
Bright Simons: We have all of the technology and all the experience to set up a global traceability system. But it's so difficult to innovate at the interface of government and the private sector. To do this, we need to interface between the manufacturers, the distributors, the wholesalers, and governments. It's not the technology, which we've got all sorted out, it's the politics, it's the human inertia. The fact that it's so hard to command the necessary influence to drive this kind of stuff. The people with the power don't understand it, and the people who understand it don't have the power.
Think Global Health: What is the solution?
Bright Simons: That's what I've been trying to solve for the last decade. I have been trying to build up our influence slowly so that when these kinds of things come up, we are able to talk to a president of a country and say, this is exactly what you need to do. Or to talk to Pfizer and say, look, this has to happen. It takes a long time to build up that level of influence—to get the influence that it takes to get these guys to talk to you in order to get technologies scaled up.
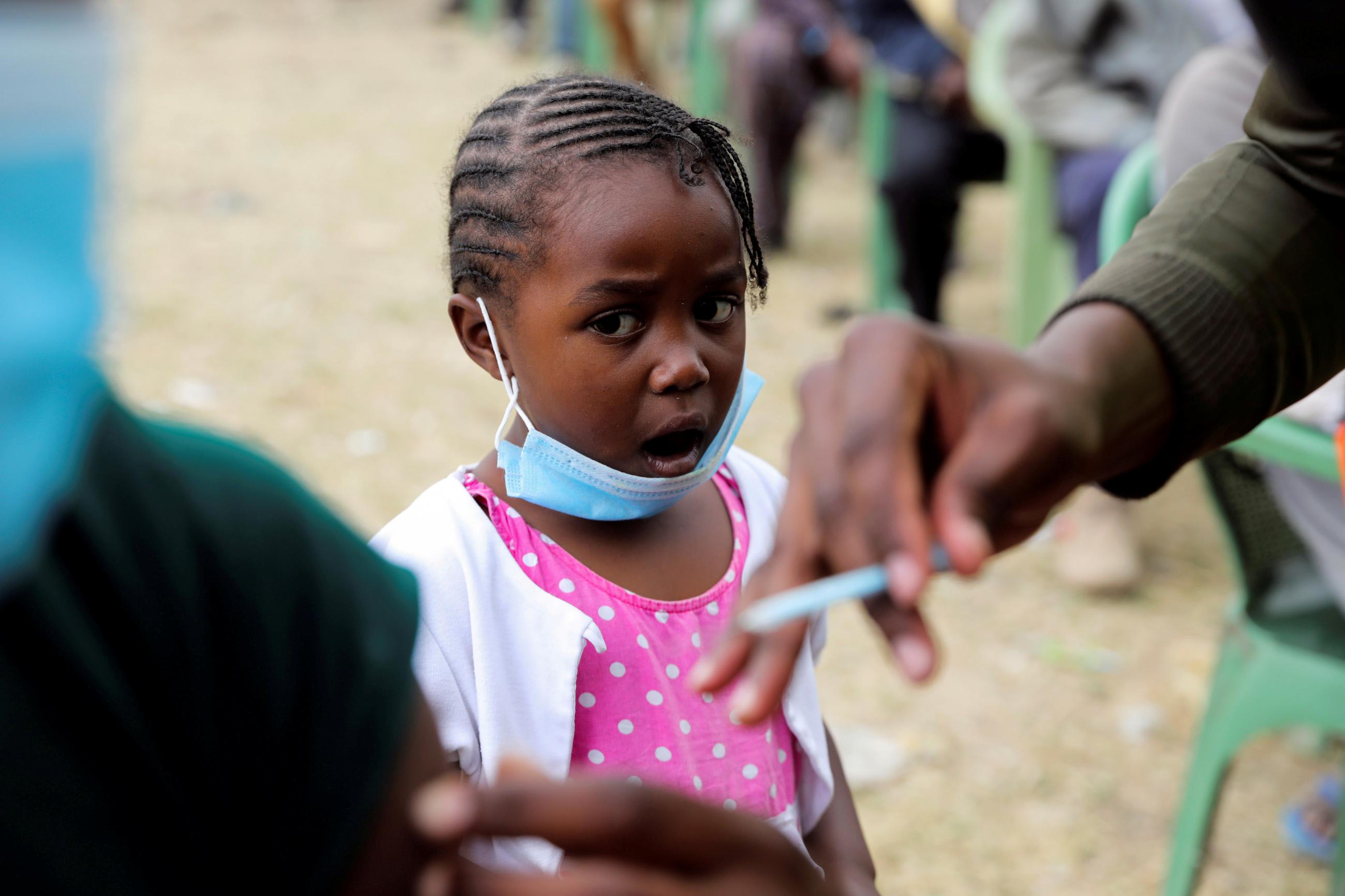
Governments don't really understand the private sector well enough. Those of us that are on the front line working with the companies and helping them solve problems can become overwhelmed deploying these kinds of systems. What you see as a consumer or health-care professional at the tail end is 1 percent of what it takes to get things going. It's like an iceberg. To get processes set up end-to-end [such as a cold chain system to deliver COVID vaccines across countries and regions], you need innovators at every level. What happens is, you have GS1 talking to the WHO, and the WHO talking to a government, and you have a big pharma giant somewhere else doing their own thing. And not enough frontline innovators in the mix, who can speak multiple languages—the "transmediaries," as I call them—in the interstices trying to plot and do the translations in such a way that results emerge seamlessly from commitment to outcome. These things take a very long time to come to fruition.
The problem is we don't have "the norms." The framework that makes things clear so that if you are a Moderna and you have a vaccine and you want to distribute it, here is the architecture—the ecosystem design—and here are the "transmediaries" who know how to interface within that ecosystem to enable you to try out new and better ways. So, we are stuck with repeating mistakes and lamenting missed opportunities.
Think Global Health: Is this your life's work, to create ecosystem norms?
Bright Simons: This is my life's work. I'm working on multiple levels, very quietly trying to get this going with some major actors in the landscape. I'm involved in the One Health movement. Our organizations do have a relationship with GAVI, as we are one of their technology pioneers. But we've been trying to get more traction with UNICEF, to engage in more practical dialogue and discussions. It takes power to get things done, but innovators don't always have power.