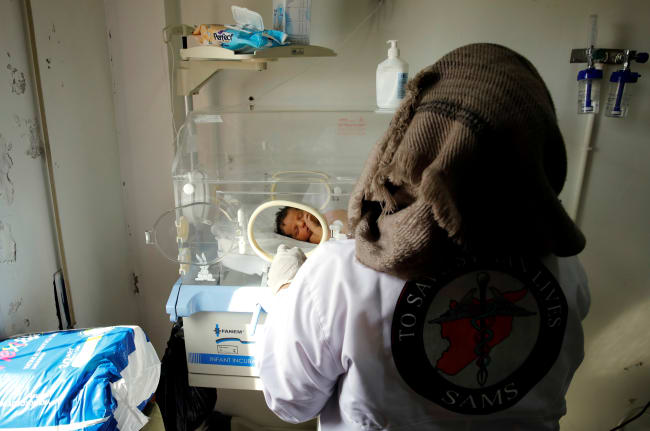
Every day patients trickle into the waiting area of an oral rehydration point manned by village health worker Sibongile Mukwananzi in Nyamadzawo village, a part of the Marange region, which lies about 183 miles (294 kilometers) from Zimbabwe's capital, Harare.
Here, patients showing cholera symptoms drink a homemade sugar-salt rehydration solution while waiting for transport to the Zvipiripiri clinic, the nearest treatment center for the acute diarrheal illness caused by a Vibrio cholerae bacteria infection of the intestine.
The southern African nation has been battling a cholera outbreak since February 2023, recording 22,790 suspected infections and 430 suspected deaths as of February 5, 2024, according to the country's health ministry. The Marange area and Buhera district, located in Manicaland Province, have been among the epicenters.
Although the country's response has involved all stakeholders, village health workers such as Mukwananzi are on the front lines. Armed with training from professional medical practitioners, village health workers guide communities on how to prevent and contain the spread of the disease. They are responsible for alerting the authorities when new cases emerge. These workers have also taken on the roles of becoming trusted messengers to combat the area's religion-fueled hesitancy toward medicine.
Forty-two-year-old Mukwananzi had her first encounter with a cholera patient about two months into the outbreak. Despite being a village health worker since 2020, she had no idea that the illness was cholera.
"I attended to a patient who was vomiting and ferried him to the clinic where nurses told me the patient was infected by cholera," Mukwananzi tells Think Global Health, seated on a rainy afternoon inside a retail store turned into an oral rehydration point. "A few weeks later, people gathered for a funeral triggering multiple cholera suspected deaths."
Suspected cholera infections as of February 5, 2024
The waterborne disease is caused by ingesting contaminated food or water. Health workers say that it spreads easily in areas such as Marange and Buhera because of lack of access to clean water and resulting poor hygiene.
Nyamadzawo village and its surrounding areas are home to people of the Apostolic sect, whose religious beliefs advocate against seeking health care. Many people in this community are polygamous, one man having sired more than 100 children with 16 wives.
"The majority of these people do not believe in science but rather that a sick person can be healed by prayers," says Mukwananzi who is a mother of four and comes from the village. "Of which that is not true."
Mildred Makore, a country director at the humanitarian organization Mercy Corps Zimbabwe, says that village health workers sensitize the community by promoting hygiene at funeral gatherings and by conducting active surveillance.
"Activities at funerals include ensuring the provision of hand washing stations at strategic points and food safety during preparation. Above all, giving health education to the mourners, emphasizing avoiding hand shaking and rituals such as cleaning of the corpse," says Makore, whose organization is supporting efforts of village health workers in Marange.

Bridging the Information Gap
This is not the first time that Zimbabwe has been hit by a deadly cholera outbreak. From 2008 to 2009, more than 4,000 people died from cholera and nearly 100,000 people were infected across the country, according to the World Health Organization.
Makore says that early response in affected areas to reduce the spread is one thing being done differently from the 2008 outbreak. "Risk communication and community engagement are one of the strategies used in the response involving the participation of community members, village health workers, and religious and traditional leaders," she says.
"Awareness raising now uses technology like social media, radios, and television to disseminate information on the disease. Most of the rural areas now have community radios that disseminate information in local languages."
The majority of cholera patients who agree to be admitted at the clinic survive
Mukwananzi, who receives cholera updates and other critical information from nurses on a WhatsApp group, says that she will keep sensitizing the community despite the risk of infecting her own family. She also conducts door-to-door campaigns raising cholera prevention and treatment awareness.
"I encourage them to visit the clinic for treatment, practice good hygiene, and make use of a WaterGuard to treat water or boil it," she says. WaterGuard, made of sodium hypochlorite solution, is used to treat water fetched from wells, rivers, and boreholes, making it safe for drinking in cholera hotspot areas.
Mukwananzi works daily at the oral rehydration point but is always ready to assist her fellow villagers at night. She says people are gradually becoming less hesitant and visiting the clinic when infected. "The majority of cholera patients who agree to be admitted at the clinic survive," she says.
Itai Rusike, executive director at Community Working Group on Health, says that village health workers are the glue that connects Zimbabwe's health-care system to communities: "They are critical to health promotion, disease prevention, early diagnosis and referral, and helping people to stay on treatment and stay healthy."

Nyasha Pukai, a village health worker, from Taguta village in Marange, says it is heartbreaking to see his neighbors succumbing to preventable and treatable diseases such as cholera. "There is a family here that lost nearly 30 people in December last year. We have lost so many lives," says Pukai, who is a member of an Apostolic sect who was encouraged by his congregation to become a village health worker to get assistance from someone they trust.
Both Pukai and Mukwananzi refer patients to the Zvipiripiri clinic for tests, diagnosis, admission, and treatment. At the clinic, patients are given antibiotics and intravenous liquids. They are expected to recover within 72 hours.
Tajudeen Oyewale, a United Nations Children's Fund (UNICEF) representative, says his organization encourages community participation and engagement in cholera prevention and response.
"This involves working with community leaders and local health workers to spread key messages about cholera prevention," says Oyewale, whose organization has provided supplies to 40 cholera treatment centers for the treatment of patients across the country as well as training, allowances, and bicycles for village health workers.
In late January, the government began rolling out oral cholera vaccines as a temporary measure to affected communities in hotspots, including Manicaland Province.
"Hopefully, our loved ones will not die from cholera in the future," Mukwananzi says.