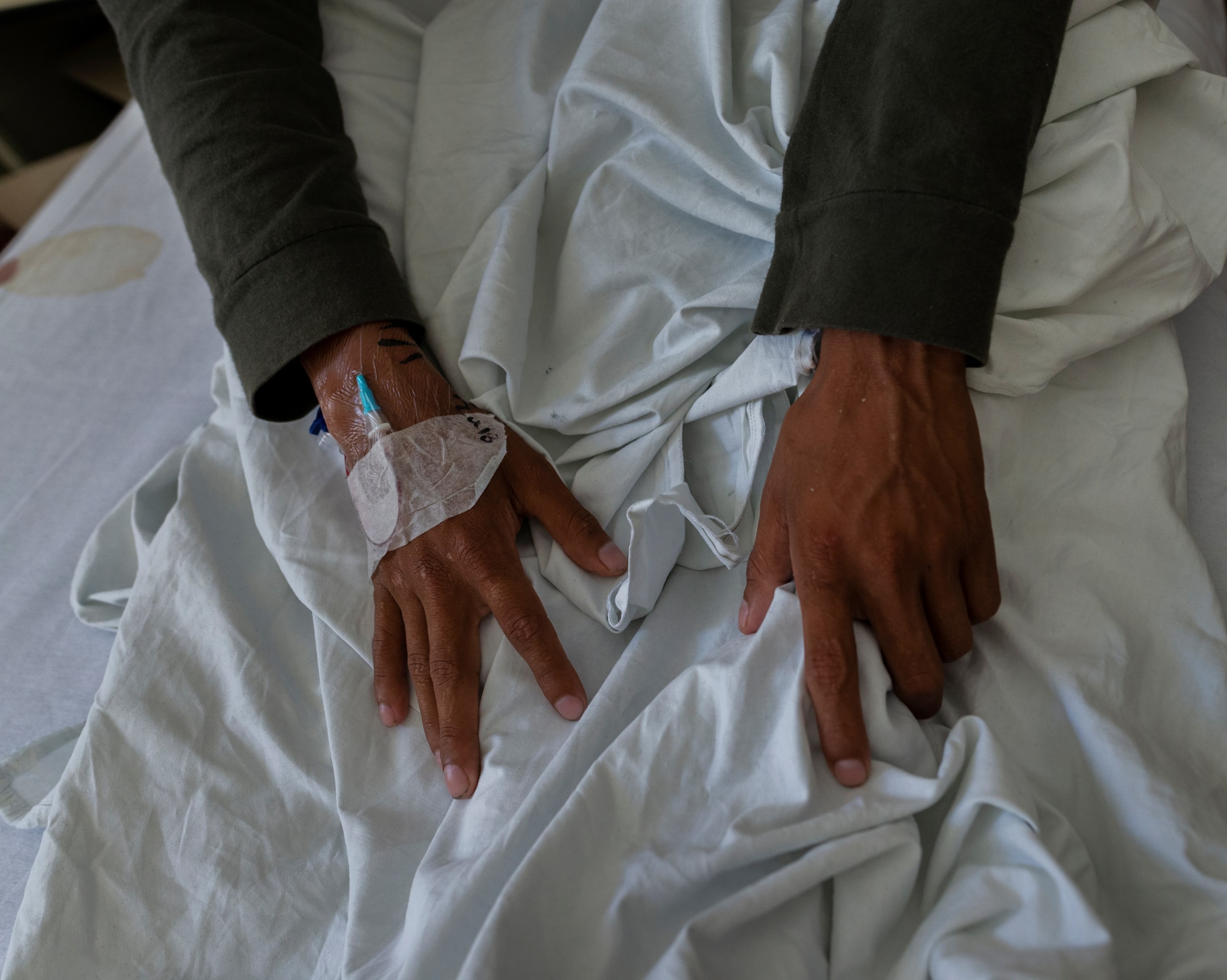
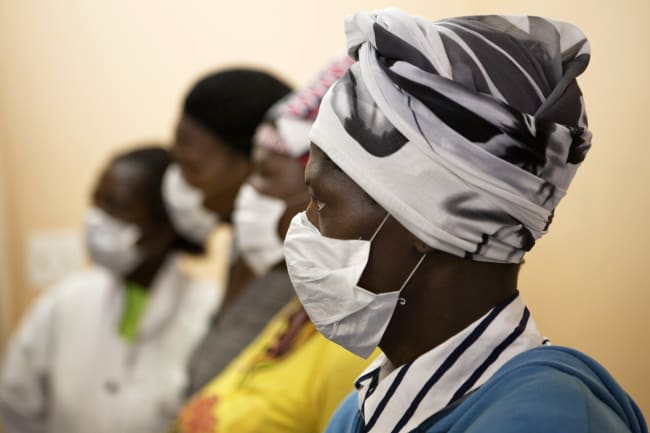
Deep cuts to international aid by the United States and its peers have compromised tuberculosis (TB) and HIV care, vaccinations, and other vital public health services in low- and middle-income countries.
Tuberculosis, already the leading infectious disease killer, will thrive amid this uncertainty and deprivation. In 2024, an estimated 10.7 million people fell ill with the disease and 1.23 million died from it worldwide, but both incidence and deaths were on the decline relative to previous years. This progress is now at risk. One modeling study, published in PLOS last year, estimated that the termination of U.S. funding could result in 10.6 million additional TB cases and 2.2 million additional TB deaths from 2025 to 2030 across 26 high TB burden countries.
Even if those projections are overestimated, tuberculosis programs in low- and middle-income countries will have to learn to do more with less money and maintain investments in TB care and control while reducing their dependency on donors. Frugal innovations, especially from high TB burden countries, will become central to the next phase of TB elimination.
Innovators and partners in countries where TB is endemic are already driving uptake of such tools. In March, some were endorsed by the World Health Organization (WHO) in a landmark policy that can greatly enhance TB case detection and bring testing closer to people.
The WHO policy updates its recommendations to include near point-of-care (NPOC) molecular tests—portable assays that can be used outside laboratories or hospitals—and easy-to-collect tongue swab samples to simplify and expand access to TB testing. The new WHO recommendation, based on a review of evidence, recommends that in adults and adolescents with signs and symptoms of pulmonary TB, NPOC tests on sputum (mucus) should be used as the initial diagnostic for TB rather than smear microscopy. When sputum cannot be obtained, NPOC molecular tests on tongue swabs should be used first instead.

This change represents major progress for TB management for several reasons. NPOC tests can be used at primary care centers, where most people with tuberculosis first seek treatment. NPOC platforms can be used with either swabs dipped in sputum or tongue swabs. Existing molecular tools, such as the Xpert MTB/RIF from the California-based company Cepheid, have largely been deployed at large hospitals and centralized laboratories, limiting access to diagnostics.
Following the WHO's new guidance, high-burden countries can push to completely replace smear microscopy with molecular testing for all people with presumed TB, and meet the WHO diagnostic standard of achieving universal access to rapid diagnostics.
For example, China and India have validated tongue-swab–based molecular tests (which amplify and detect bacterial DNA) and demonstrated their application in low-resource settings. Examples of such tests include Minidock by China's Pluslife Biotech and the Truenat MTB Ultima test by India's Molbio Diagnostics. Currently, the Pluslife technology is endorsed by WHO and classified as NPOC.
For centuries, pulmonary TB detection relied on patients providing samples of sputum, or mucus coughed up from deep in the lungs. Nearly a quarter of adults, however, are unable to cough up mucus from deep within the lungs and children rarely produce sputum.
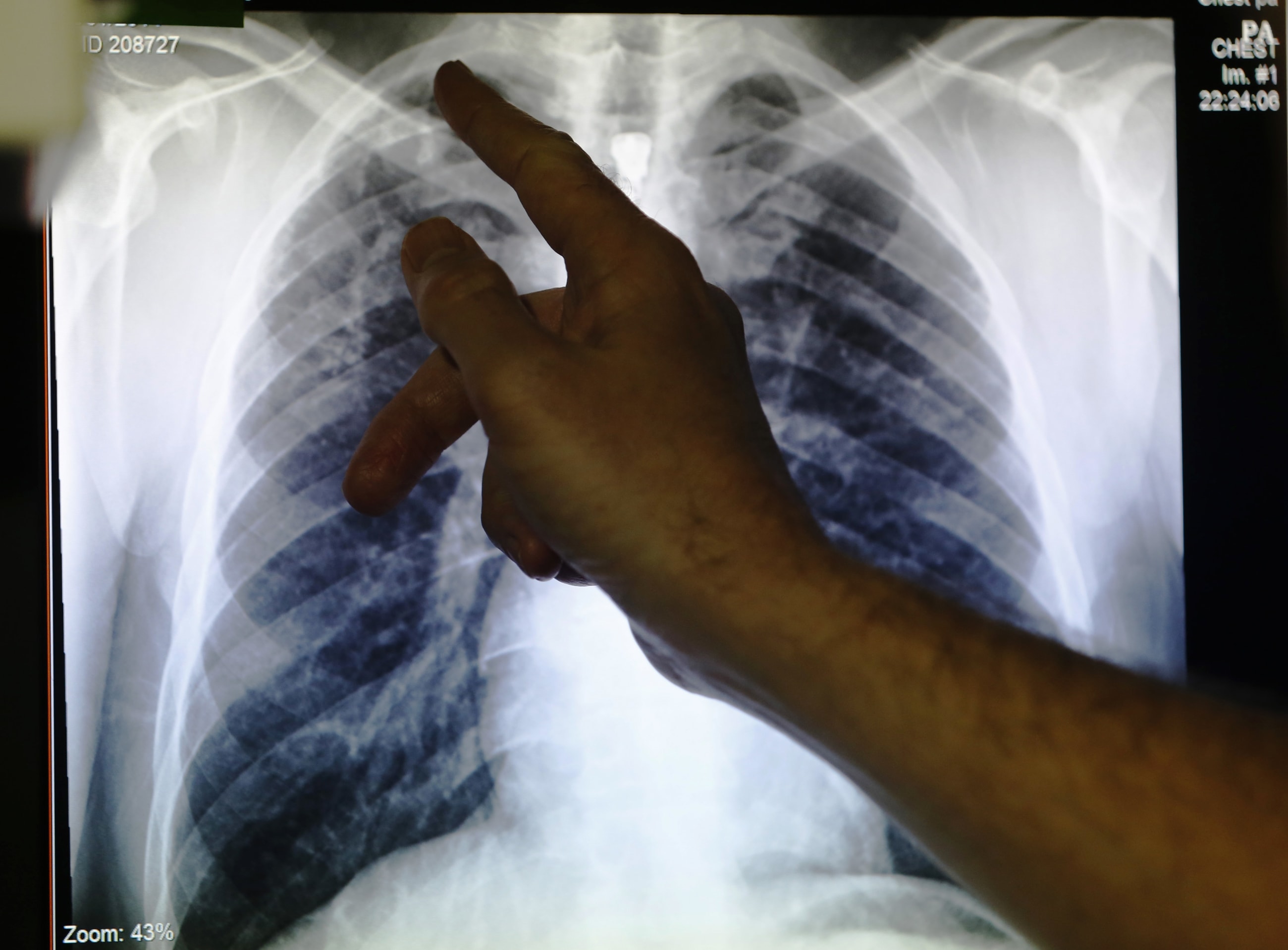
Tongue swabs, on the other hand can be collected from everyone, offering a much-needed alternative to sputum samples. By using both sputum and tongue swabs, health workers can now test more people than they could earlier. Once TB is detected, additional drug-resistance assessments can be done using conventional molecular tests and cultures.
Investments by various partners—such as the Gates Foundation, Global Fund, Children's Investment Fund Foundation—have lowered the cost of the Pluslife's MTB Nucleic Acid Test Card used on the Minidock Ultra device to $3.60 per test via the Global Drug Facility. That amount is roughly the same as the cost of two smear microscopy tests, which need to be analyzed in a laboratory, and half the price of other WHO recommended rapid molecular tests, allowing countries with reduced budgets to ensure that all people with suspected TB are tested with a molecular test. To help TB program managers calculate cost savings, a free online app is now available.
All molecular technologies are capable for testing for a variety of infectious diseases and can be used for diverse needs, not just tuberculosis. Thus they offer great hopes for delivering a broad array of diagnostics for primary care and help countries improve access to essential tests included in the WHO Essential Diagnostics List.
History shows that mere availability of excellent products and policies does not guarantee availability and access in low-resource settings. The critical pathway for adoption and scale-up of new TB tests is often tedious but not insurmountable. The Global Fund is already working with several high TB burden countries to roll out NPOC testing in 2026, which can then feed into larger investments under the 2027 funding cycle. The TB REACH program of the Stop TB Partnership is also supporting adoption in countries.
This World TB Day reminds high-burden countries why they should adopt the new WHO policy and redouble their efforts to close the massive TB diagnostic gap. Innovations and policies mean little until they reach those who need them the most. Better diagnosis—along with effective measures such as social protection, adoption of shorter regimens, and better integration of TB into primary health services [PDF]—can all play a big role in sustaining progress.

DISCLOSURE: The author no financial or industry conflicts to disclose. He serves as an advisor to nonprofits—the WHO, Gates Foundation, and Partners in Health.