LONDON—Tuberculosis (TB) patients who receive treatment and survive are often left with unwelcome surprises. Half deal with permanent lung damage, and others whose infections affect the brain or spine can suffer seizures, blindness, or problems with cognition. Yet many survivors in high-income countries such as England are thrust back into the world with these ongoing medical problems and little support to manage them.
In a bid to change these fortunes, doctors opened a clinic in London—which UK health authorities once dubbed Western Europe's TB hotspot—to speed up diagnoses and improve care for patients who have finished TB treatment. Announced in March 2025 and launched toward the end of the year, this partnership between Queen Mary University of London and Barts Health NHS Trust has seen its first 23 patients cycle through the specialist clinic, which has an unexpectedly high demand for mental health care and contact with other TB survivors. The clinic is now ramping up services and eyeing new offerings, such as group therapy.
England's TB burden is small compared to the endemic spread recorded annually in Asian nations or elsewhere. But recently the British isle has recorded about 5,400 new cases per year. Typically, 4 of every 5 TB patients in England complete treatment, creating the potential need for a post-TB care clinic.
Typically, 4 of every 5 TB patients in England complete treatment, creating the potential need for a post-TB care clinic
At the Queen Mary and Barts Health Tuberculosis Centre in East London, patients can see a TB doctor and nurse, neurologist, psychologist, physiotherapist, occupational therapist, and peer support network. Staff say that having these specialists all in one place helps coordinate care, ensures that doctors are well versed in handling TB complications, and simplifies medical visits for patients.
The center will host four post-TB clinics in 2026, largely funded by a three-year, 4.63 million British pounds ($6.23 million) grant. The team hopes that, eventually, every new TB patient in their area will come through within three months of diagnosis, and again as they're finishing treatment. In 2024, Barts Health saw nearly 300 TB patients.
"The idea is if they have ongoing needs at the end of TB treatment, we tap them into the right services in their borough," said Angharad Davis, a neurologist who leads the center's work with patients with TB in the brain or spine, known as CNS-TB.
Patients can be referred to the post-TB clinic once they've been diagnosed with the disease. If they have CNS-TB, Davis's team gets a notification and meets to discuss their case. But it is up to patients to decide whether to attend the clinic.
It hasn't all been smooth sailing; Davis says there's a "huge discrepancy between boroughs" in the availability of community rehabilitation services.
Even so, Amy McConville said she would have benefited if the post-TB clinic had been available during her own treatment journey more than 20 years ago. She was a university student when she developed a persistent cough in 2004, and she spent nearly a year pinging between doctors' offices, her body in pain and wasting away, before she was diagnosed with TB in April 2005. Treatment was brutal and lasted months, she said, zapping her energy and eventually taking her entire left lung. Two years later, she said she was diagnosed with depression and anxiety, and her struggles with TB's knock-on effects remain.
"Living with post-TB lung disease affects me physically and emotionally every day," said McConville, now 41. She cited breathlessness, difficulty exercising, her mental health, and "having to adapt to a new normal for the rest of my life."
Patience Renias-Zuva, who works on peer support at the center, wants patients to know that they aren't alone during their TB treatment and post-care.
The latent nature of TB carries a stigma that can cause people to keep their diagnoses hidden, as Renias-Zuva did as a teenager in Zimbabwe. She was successfully treated for TB and kept it secret for two decades.
"That was something you just wanted to get the treatment [for] over and done with, and never hear of [TB] ever again," said Renias-Zuva, who now lives in London.
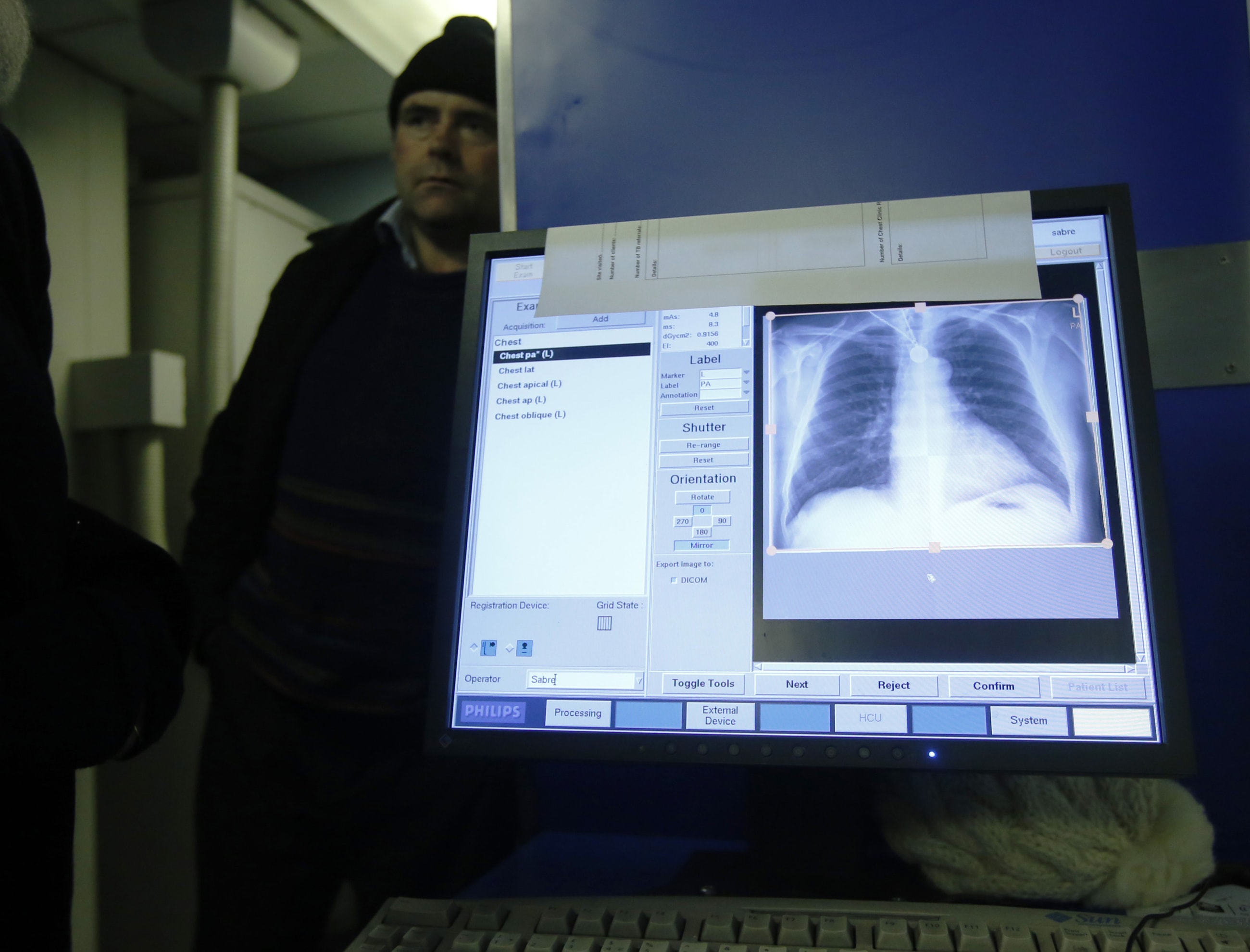
The TB center's holistic approach is unusual. In the UK, most clinicians perform chest X-rays for TB patients who are finishing treatment, but they rarely screen for other health problems, such as diabetes or cardiovascular risks, according to a 2025 survey of 113 TB services nationwide. About half checked whether survivors had trouble with daily life activities, and fewer than 1 in 4 screened patients for anxiety and depression.
TB advocates say that a model like this is needed globally
"We still primarily talk about post-TB as a lung problem, but it's actually much, much broader than that," said Tom Wingfield, an infectious-diseases physician and deputy director of the Centre for Tuberculosis Research at the Liverpool School of Tropical Medicine, who isn't involved with the Queen Mary and Barts project.
As the post-TB clinic sees more patients over the next two years, the team hopes it will become a model for post-TB care across the UK and beyond, and Davis said they will share what they've learned at an international post-TB conference next year. Eventually, she wants to help develop clinical guidance for CNS-TB care that can also be used in poorer countries where TB takes a greater toll, with a focus on patients' and caregivers' priorities.
TB advocates say that a model like this is needed globally, given that post-TB complications are often overlooked.
"It is something we should seriously look at," said Lucica Ditiu, who leads the Stop TB Partnership, a Geneva-based group that works to improve access to TB care worldwide. She said many patients in lower-income, high-burden countries are still reliant on outdated diagnostics and medicines, so improving this care is seen as a bigger priority than addressing post-TB complications.
Globally, about 10.7 million people fell ill with TB and more than 1.2 million people [PDF] died in 2024, making it the world's deadliest infection. Africa and Southeast Asia are the hardest-hit regions, but anyone can get TB.
Wingfield said the UK health system should focus more on people's overall well-being after TB, and on diagnosing the disease faster. Nearly a third of people with infectious TB face diagnostic delays of at least four months, according to 2024 data from England, and these delays are associated with more- extensive lung damage that can make post-TB recovery harder.
"We do see quite a lot of people who are quite late on diagnosis, and have advanced tuberculosis who weren't picked up before," Wingfield said. "That will have an impact" on their long-term outcomes.
For the post-TB clinic to stay afloat after the three-year grant ends, Davis and her team will have to prove to the National Health Service that they can be nimble—and are worth spending taxpayer money on. They're tracking whether their integrated model, from TB diagnosis to post-TB care, makes patients less likely to visit general practitioners' offices and the emergency room, and whether it helps them return to work faster. The answers should start to come over the next year.
"We need to think about ways to make this as streamlined as possible, and cost-effective," Davis said. The clinic's one-stop-shop approach "will still be the same in a year's time, but the exact design may have changed."