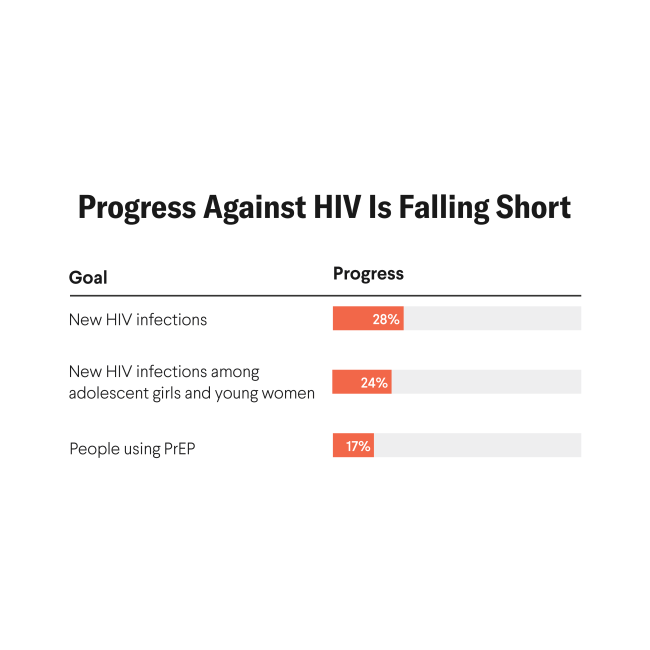
The public health field is preparing for what could be the most important advance in HIV prevention in more than a decade: the rollout of lenacapavir, a twice-yearly injectable with the potential to expand access to long-acting pre-exposure prophylaxis (PrEP). Yet history shows that even the most effective products fall short when systems and support structures don't align with realities of people's daily lives.
Oral PrEP has illustrated this clearly: despite global approval in 2012 and strong evidence of efficacy, uptake has remained uneven due to persistent behavioral, social, and structural barriers. These challenges offer lessons for the rollouts of any next-generation PrEP modalities.
For long-acting PrEP, success will depend on something less visible: whether health systems can respond to the everyday questions, fears, and decisions that shape whether people start—and remain on—prevention. Preparing for this question requires real-time insight into how people experience HIV prevention, where trust breaks down, and what support actually changes behavior. This is where digital-relationship-based tools—such as artificial intelligence (AI) chatbots supported by large-language models (LLMs)—come into play.
Non-AI chatbots have been used across health sectors for more than a decade, but rigorous evidence on the technologies' effectiveness, acceptability, and integration into routine health programming remains limited, especially for nascent LLM-driven chatbots. Traditional and AI chatbots have been deployed in South Africa, Kenya, Nigeria, and Tunisia, supporting health education, counseling, screening, and information provision across HIV, maternal and general health, and COVID-19. Implementation has relied on text messaging services and WhatsApp, and multilingual support for accessibility to reach diverse populations.
Aimee as a Digital Entry Point to Primary Care
Evidence from South Africa's Aimee program offers a glimpse into how digital tools could support the next generation of HIV prevention. Aimee is a WhatsApp-based AI health companion developed by the nonprofit Audere Africa and the youth-centered health service SHOUT-IT-NOW, which provides confidential, 24/7 guidance on HIV prevention, sexual health, and mental well-being. Because Aimee operates on WhatsApp—already widely used among young people—it removes many of the barriers that limit adoption of other digital health tools.
Engagement has been substantial. With nearly 10,000 users, the platform represents one of the largest real-world datasets on an AI health companion in HIV prevention. More than two-thirds of users interacted with the AI companion, self-testing tools, or a clinician, and nearly half of those who chatted with Aimee proceeded to take up HIV self-testing.
Users frequently sought advice on HIV testing, PrEP, contraception, and relationship concerns—revealing that many people begin navigating prevention decisions long before they enter a clinic. Aimee often served as a pre-care guide—explaining how PrEP works, addressing concerns about side effects, and encouraging routine HIV testing. Many users also returned after clinic visits to clarify instructions or discuss side effects.
"With PrEP, I took it but didn't fully understand how it works, so Aimee explained it," said a young woman who participated in the Aimee study. Her name and age have been withheld for privacy reasons.
This continuity is valuable in settings where clinicians face heavy caseloads and have limited time for follow-up counseling. By helping users address adherence challenges early, tools like Aimee can support sustained engagement in prevention and treatment.
"They were uncomfortable saying other stuff to us…They said different things to Aimee… they were given time, and information, and guidance…in a non-judgmental way. [For us as nurses] it gave you how to approach the client…what to prepare…For example, if a client wants PrEP, it prepares you on which information to give," said a nurse supporting the Aimee and Self-Cav programs with SHOUT-IT-NOW. The nurse's name has been withheld, and Self-Cav is a youth self-care platform implemented in partnership with South Africa's Ministry of Health.
A key lesson is that long-acting PrEP does not eliminate the need for support—it changes when that support is called upon. Even with twice-yearly injections, people will still have questions about HIV testing, missed visits, side effects, and prevention choices between clinic appointments. The Aimee data shows that digital companions can help fill these gaps, providing continuous guidance during the long intervals between injections when clinic contact is limited.
Lessons for Global Health Programs
Digital companions such as Aimee are part of a broader wave of digital health tools being tested across HIV programs. Chatbots and messaging platforms have been deployed in several countries to support health education, triage, appointment reminders, and adherence counseling through widely used channels such as WhatsApp and Short Message Service (SMS). A recent large U.S. cohort study of more than 155,000 patients across AIDS Healthcare Foundation clinics found that individuals who interacted with an AI-supported messaging system were more than three times as likely to initiate PrEP compared with those who did not use the tool. Users also demonstrated significantly higher follow-up attendance and persistence in care.
Insights from Aimee highlight the importance of integrating digital tools into prevention strategies
The anticipated introduction of long-acting PrEP such as lenacapavir arrives at a moment of transition for global HIV programs. Donors and governments are increasingly emphasizing efficiency, measurable outcomes, and more client-centered models of service delivery. Meeting those expectations will require a deeper understanding of how individuals actually navigate prevention decisions—and how health systems can support those behavioral journeys. It will also require sustained investment in programs tailored to populations most vulnerable to HIV.
Although these tools require upfront investment in data systems, digital counseling capacity, and governance frameworks, digital platforms can reach large numbers of users at relatively low marginal cost, potentially improving efficiency compared with traditional outreach models that rely heavily on in-person counseling and repeated clinic visits.
Insights from Aimee highlight the importance of integrating digital tools into prevention strategies. Digital health companions can provide counseling, answer questions, and support adherence between clinic visits—functions that overstretched health systems often struggle to sustain.
Successful deployment will also depend on early alignment between ministries of health, implementing partners, and community organizations to embed the tools within national health priorities and accelerate adoption at scale. Delivery models—whether facility-based, community-based, or hybrid—must be designed from the outset to reflect both the operational realities of health systems and the behavioral realities of clients. When policy, service delivery, and community insight are aligned early, programs are more likely to achieve sustained uptake and long-term benefits. In South Africa, this approach has meant integrating Aimee into Self-Cav.
Concurrently, the evidence base for AI-enabled digital health interventions remains limited. Most studies focus on feasibility or user satisfaction rather than measurable prevention outcomes, and many have been conducted with relatively small participant groups. As digital tools become more integrated into HIV programs, there is a growing need to evaluate their contribution to outcomes such as HIV-testing recency, PrEP initiation, and timely return for follow-up care. A new Lancet Commission on AI and HIV aims to help close this gap by strengthening the global evidence base and identifying priority interventions and approaches for responsible, scalable deployment of AI in the HIV response.
Another important limitation relates to unequal access to digital technology. Smartphone ownership, internet connectivity, and data costs remain uneven across and within countries, which may limit the reach of AI-enabled digital tools unless programs are designed to function across multiple channels, including lower-bandwidth options such as SMS or widely used messaging platforms.
Ultimately, realizing the full potential of long-acting PrEP will require pairing biomedical innovation with equally strong behavioral and communication strategies. Digital companions, alongside tools that support health workers, offer one promising approach. The early lessons emerging from South Africa suggest that these technologies could help bridge a long-standing gap in the HIV response: translating highly effective prevention tools into sustained real-world uptake.