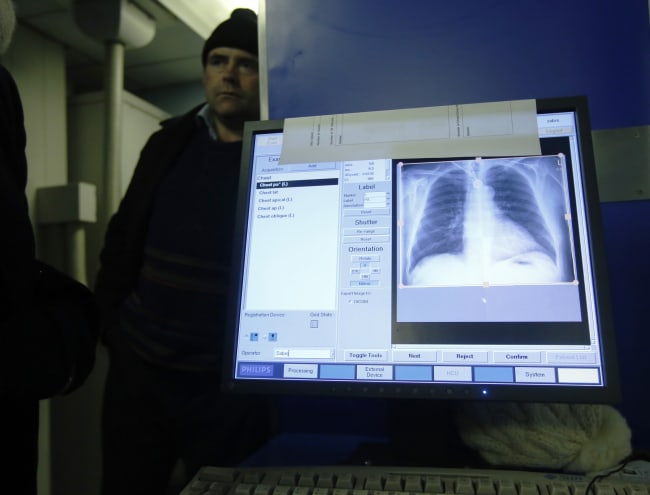
Deanne Brodie was speaking in backward sentences. This prompted the 58-year-old's neurologist to order an emergency magnetic resonance imaging (MRI) scan in October 2020 because they said her symptoms could signal a brain tumor.
They discovered 10 white-matter lesions across her brain, which are found in some people with long COVID. The hallmark characteristics of this disease are fluctuating, flulike fatigue that does not improve with rest, a fast or irregular heartbeat, shortness of breath, difficulty thinking, pain, and other symptoms that persist for more than 12 weeks following a SARS-CoV-2 coronavirus infection. Roughly 6–10% of people who contract the virus develop long COVID, and multiple infections can worsen symptoms.
After repeat infections with the virus beginning in December 2020, Brodie has survived two strokes, the latest on February 9, 2026. With long COVID, she battles severe fatigue, fainting episodes, and cognitive impairment daily.
"There are days when I remind myself of my mom when she had Alzheimer's," said Brodie, who, before contracting COVID, used to write and sometimes swim a mile a day.
Brodie found relief and validation of what was going wrong from a nurse through the Northamptonshire Post-COVID clinic at St. Mary's Hospital in Kettering, England, where she'd been receiving care since 2021. But last fall, her provider informed her that the clinic was closing in October 2025.
I can't be in a smaller world than I am now, and that's not okay. They've taken our last support away by saying it's not financially viable
Deanne Brodie
This clinic's closure reflects a larger trend happening elsewhere in the United Kingdom and the United States. In England, the National Health Service (NHS) removed the "ring-fence" requirement around funding [PDF] for long-COVID services. This requirement ensured that the allocated money was spent only on those clinics. As of spring 2025, the integrated care boards across England, NHS-established organizations that plan and fund local services in response to their populations' needs, are now no longer required to use these funds on long-COVID services.
"I can't be in a smaller world than I am now, and that's not okay. They've taken our last support away by saying it's not financially viable," Brodie said.
A National Plan, Interrupted
The closures mark a stark reversal by the NHS. In the midst of the pandemic, they requested that integrated care systems "provide fully staffed Long COVID service plans" by mid-July 2021, according to the specific National Institute for Health and Care Evidence guidelines.
Their hope was to create a national system of long-COVID services to help the estimated 186,000 people across England by November 2020 who were reporting persistent symptoms after their COVID infections.
Between December 2020 and June 2021, England opened 89 specialty clinics, with roughly 1,500 weekly referrals. The number of patients grew from 862,000 in 2021 to 1.7 million by March 2022.
In late March 2024, the NHS transitioned responsibility for these clinics to the estimated 42 integrated care boards across the country. They hoped to streamline services from a national level to local pathways. The NHS continued to allocate funds, requiring that they be spent on long-COVID services.
In March 2025, after the NHS removed the "ring-fenced" funding requirement, a press release [PDF] from Long COVID support, a UK-based charity, said: "It is feared that even more clinics could shut down, leaving thousands of patients without access to specialist care."
Aside from Northamptonshire this year, other clinics outside of London in Mid Essex, South Essex, and South Warwickshire will also close, citing a declining number of referrals. The referral trend is real, but it is likely due to people not testing for COVID, said Melissa Heightman, a respiratory physician at University College London's Hospital COVID clinic, who spoke to Think Global Health on behalf of the Clinical Leadership Group for the International Post COVID and Post Infection Condition Society.
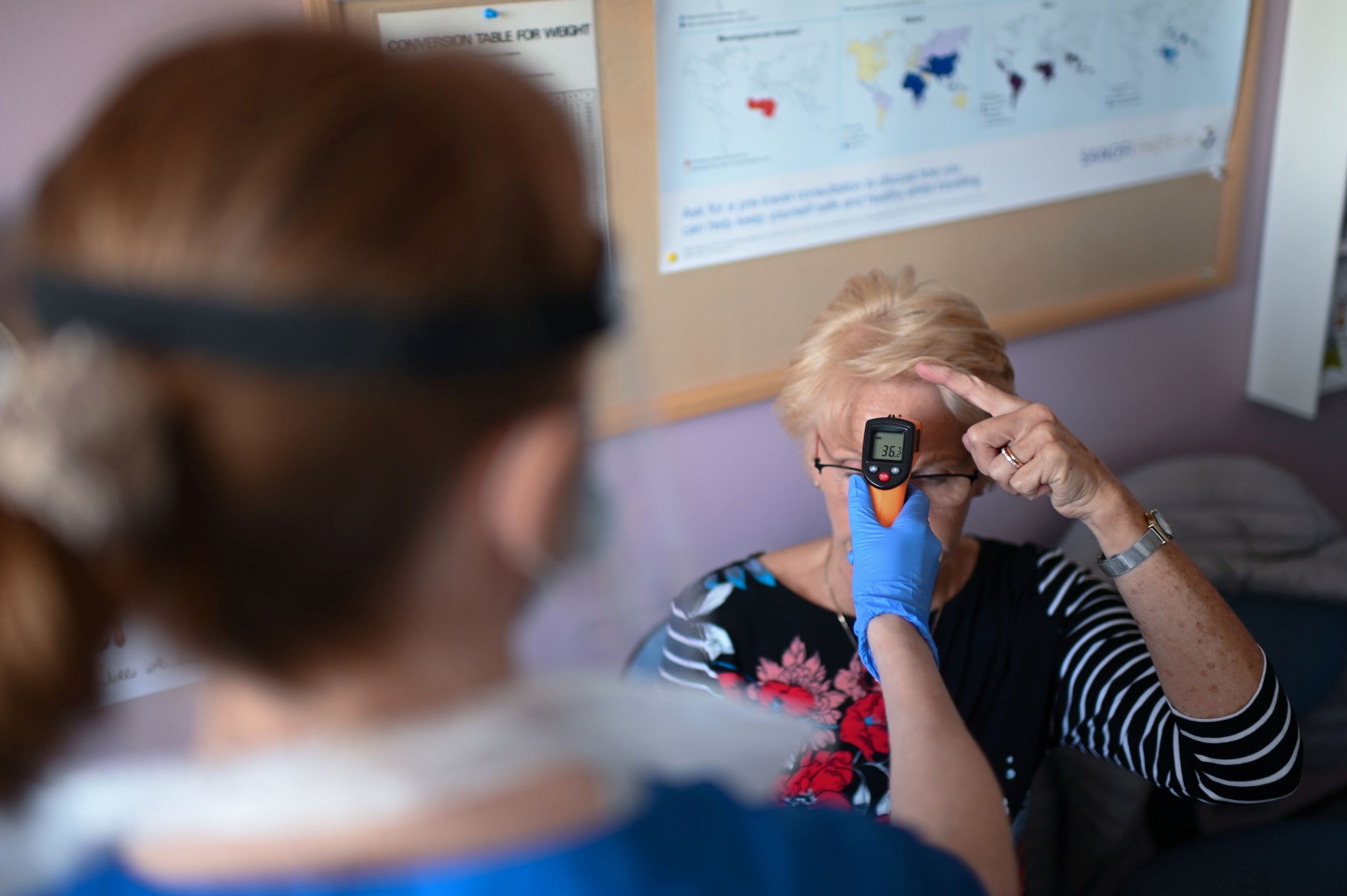
The UK's Annual General Practice (GP) Patient Survey supports her claim, showing the self-reported prevalence of long COVID—4.5%—remained steady from 2022 to 2025. Nearly 1 in 10 respondents say they are unsure whether they have long COVID.
Even if a portion of long-COVID patients recover over time, fewer people being tested in general means new cases of the chronic condition could be misdiagnosed and missed entirely.
"It was too soon to step down that national program," Heightman added.
UK Long-COVID Patients Navigate an Uneven Shutdown
Since this decision, at least 24 integrated care boards have closed their clinics and referred patients to other services, such as chronic fatigue clinics or back to their general practitioners.
However, referring patients back to general practitioners or fatigue clinics does not always work, as not all patients have fatigue, and many general practitioners don't know how to treat long COVID, according to patients.
"It's a disastrous way to run a service," said Margaret O'Hara, the founding trustee and research lead of Long COVID Support. O'Hara said that since the "ring-fence" requirement ended, some health authorities have not used the money for long-COVID services, according to freedom of information disclosures that the charity sent to each trust, integrated care board, and health board.
Other non-COVID services are also overwhelmed. "Without decisive action, patients will simply be pushed back into primary care, emergency departments, and mental health services that are already overstretched and not equipped to manage complex post‑viral illness," said Jo Platt, a member of UK Parliament and chair of the All-Party Parliamentary Group for Long COVID.
"My worry is that this combination of low awareness, disappearing services and a growing patient population will deepen inequalities and leave thousands, including a generation of young people, without the care, understanding and opportunities they need to rebuild their lives," Platt added.
As of spring 2025 [PDF], 46 clinics had confirmed that they were open, 31 were under review, 24 were set to close, and 20 did not respond to freedom of information requests made by the charity.
Long-COVID patients, including Brodie, say the NHS decision left them without care.
Since Brodie's second stroke in early February, she's had difficulty accessing an echocardiogram test, which would show whether her heart is functioning properly. She's worried that there is something systematically wrong with her body and that she will have another stroke. It's not only Brodie who is being affected.
In March 2023, UK officials estimated that 1.9 million people [PDF]—2.9% of the population—had long COVID. As of April 2024, more than 111,000 children ages 3 to 17 years across England and Scotland have the condition. Disability cases have increased by 1.8 million claimants between May 2020 and May 2025, and this is expected to continue rising, according to UK disability statistics.
"Yet the condition is still widely misunderstood, dismissed, or minimized," Platt said.
Another patient, Marissa Van Donkelaar, credits Royal Berkshire Clinic for saving her life.
"I was in a place where I just didn't want to live," said Van Donkelaar, who struggles with severe dizziness and fatigue from her second infection, which left her unable to work. She said checking in with the clinic pushed her to stay alive.
Van Donkelaar's clinic diagnosed her with postural orthostatic tachycardia syndrome (POTS), a nervous system disorder that affects heart rate and blood flow. She was prescribed ivabradine, and within 48 hours of taking it, her constant background dizziness was reduced. A week later, it went away completely. "I felt like dancing. The levels of energy I have had, I had not felt for three years. It was amazing," she said.
On February 3, Van Donkelaar received a refill of her medication, of which she'd taken five milligrams twice a day for a few weeks. This new pill looked different, though. The familiar dark orange had been replaced by a light pink, made by a different manufacturer.
Within a few days, the dizziness returned, and Van Donkelaar could not get out of bed. She contacted her general practitioner and Royal Berkshire. Because she was discharged in November 2023, the long-COVID clinic couldn't do much, as she is no longer a patient. She called several pharmacists and learned on February 24 that her medication was arriving in the UK. However, she was left without it for nearly three weeks.
Platt said that to tackle long COVID, we need a communal effort. "We need genuine partnership between [the] government, researchers, clinicians, educators, families and organizations like Long Covid Kids and Long Covid Support," she said. "We need investment in biomedical research, including pediatric trials, so that we can move beyond symptom management and towards real treatments."
Moving Forward
University College London's clinic has received a steady 1,500 referrals every year since 2020, and the demand has increased as other clinics closed, according to Heightman. She worries about the long-COVID patients who don't have the means to reach her clinic.
Heightman began working with long-COVID patients in April 2020, a few weeks after the pandemic first hit London. The hospitals shut down because of infection control, so she and other providers saw patients, ran X-rays, and conducted blood tests in a truck parked outside the clinic.
"It was an awful time," Heightman said. "It was clear that the unmet need was huge."
This month marks six years since the lockdowns began in the UK and the World Health Organization described COVID-19 as a pandemic. There are still no biomarkers or approved treatments for long COVID, which would give providers a clear path to diagnosing patients and helping them manage their symptoms or recover.
"Ultimately, every person with long Covid deserves to be counted, believed and cared for. Awareness is only the first step," Platt said.