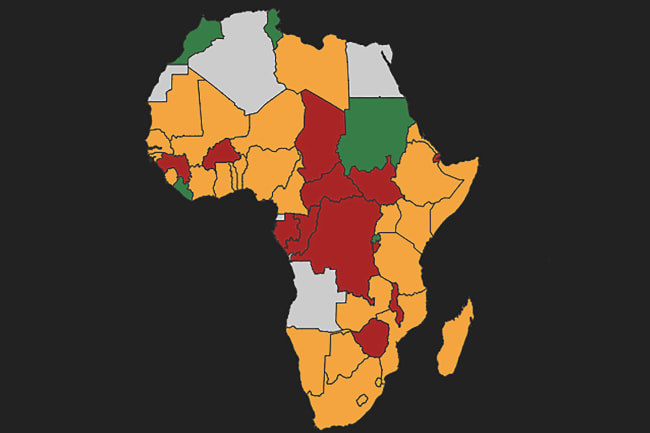
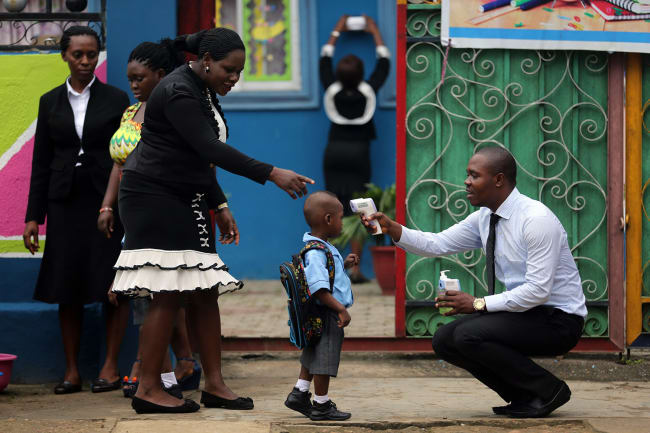Africa bears more than 24 percent of the global burden of disease, but has access to only 3 percent of its health workers and less than 1 percent of the world's financial resources, according to the United Nations. The World Health Organization (WHO) reports [PDF] Africa has one doctor for every 5,000 people while a recent study in the journal Lancet found almost a third of the total population in sub-Saharan Africa lives more than two hours from their nearest hospital.
On March 30, the day this article was published, Africa CDC sent a tweet reporting 4,871 cases in 46 African countries and 152 deaths. The reality is that the coronavirus pandemic has encountered a continent with a patchwork of health systems that may be not only understaffed but also ill equipped to contain an outbreak of this magnitude.
As it stands, African health care facilities may not be able to increase their staff or build new centers ahead of the global health crisis. In fact, governments around the world are asking infected persons to stay home and employers have been encouraged to tell their employees to work from home.

Whether we stay at home or not, the coronavirus pandemic is a wake-up call to use all the resources at our disposal, including healthier design.
These settings, primitive as they were, are better designed to curb infection spread than some of our modern hospitals today
African spaces for healing traditionally featured a medicine man under a tree or in their home, which later transformed into the community clinic. These settings, primitive as they were, are better designed to curb infection spread than some of our modern hospitals today in the sense that the natural ventilation and natural lighting bolstered by the access to adequate open spaces can limit the likelihood of sick people infecting each other. COVID-19 spreads through direct contact or indirect contact with a contaminated person, object, or airborne droplet. Simple design principles can thus be used to curb the spread of infection and make our health centers, homes, and workplaces healthier for living even today.
To start with, natural ventilation is a must. Airborne transmission is the most dangerous for a few seconds after leaving the host, so ensuring an adequate airflow across spaces is a simple and effective measure to reduce possible infections—though droplets, once they settle on surfaces can remain infectious for much longer.

Case studies from China following the SARS outbreak indicate cross-ventilation was one of the most effective ways of controlling the SARS infection in hospitals. The same studies documented that the SARS outbreak in Vietnam caused the loss of lives of patients and health workers in a high-end hospital that used mechanical ventilation, but no lives were lost in the naturally ventilated Bach Mai Hospital Hanoi, which used natural ventilation.
Infection is minimized by avoiding unnecessary doorways in high traffic areas or using temporary door stoppers to keep doors open during peak times
Second, the effect of natural light is often overlooked in the prevention of disease outbreaks. Studies done since the 1940s have shown that daylight influences air quality, because the high-energy ultraviolet rays in direct sunlight is a natural disinfectant because it breaks DNA bonds and helps to kill germs. Beyond that, natural light has psychological health benefits and contributes to faster recovery. Third, reducing the spread of germs from person-to-person through commonly touched surfaces is key. Research done in hospitals found that something as trivial as a door handle could contribute to the spread of infection depending on how people were required to use it. Infection is minimized by avoiding unnecessary doorways in high traffic areas or using temporary door stoppers to keep doors open during peak times and so reduce unnecessary contact.
The type of door handle is important too and push plates on doors are better because traditional "pull" door handles, which use the whole hand to operate and are harder to clean. This applies to any handles such as those on cupboards, shelving, cabinets, cupboards and other furniture that can be avoided. Placing non-private items on open shelving or table tops makes for healthier spaces.

Finally, it's important to keep surfaces fouled by infectious particles clean. Solid surfaces such as ceramic tiles, granite and plastic are important because they are easier to clean and less likely to absorb harmful germs compared to permeable ones such as carpets, curtains and roughcast wall finishes.
By taking a cue from African traditional care centers as well as good health care design principles, we can apply simple measures to prevent the spreading of the disease in local health care centers, our workplaces, and our homes. Those measures include:
- If you or your family member finds is sick at home, identify a room that is well ventilated, naturally lit, and with primarily solid surfaces for easy cleaning. If you are not able to isolate a specific room, you can partition spaces as a temporary solution.
- Keep doors open as much as possible in order to reduce unnecessary door handle contact. Frequently used cupboards and drawers containing non-private documents should be avoided and instead items stored on accessible open shelving or tabletops.
- If possible, in designing and decorating facilities, avoid curtains, carpets, and fabric chairs.
Humans spend 90 percent of their time indoors, where some pollutants may be 2-5 times higher than outdoor concentrations
Humans spend [PDF] approximately 90 percent of their time indoors, where the concentrations of some pollutants are often two to five times higher than typical outdoor concentrations. It makes sense, then, that we make these spaces—whether our homes, offices or even our healthcare centers—healthier. This will benefit not just the current crisis but also our long-term ability to curb the spread of infections in sub-Saharan Africa.
And, we don't need to discover new, complicated technologies—but rediscover those simple, sustainable and accessible solutions used by our ancestors.