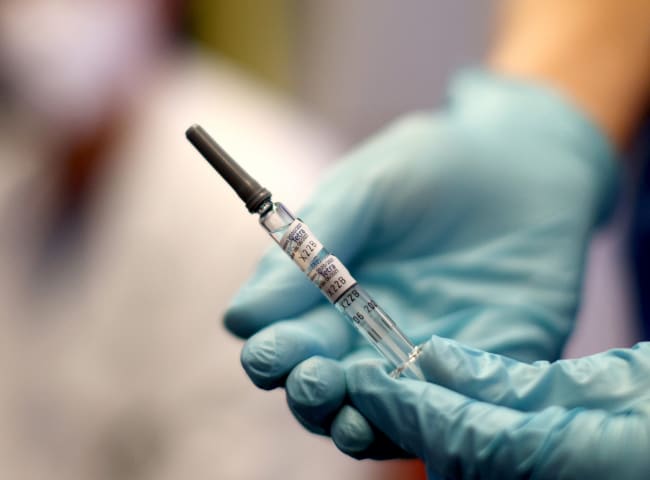
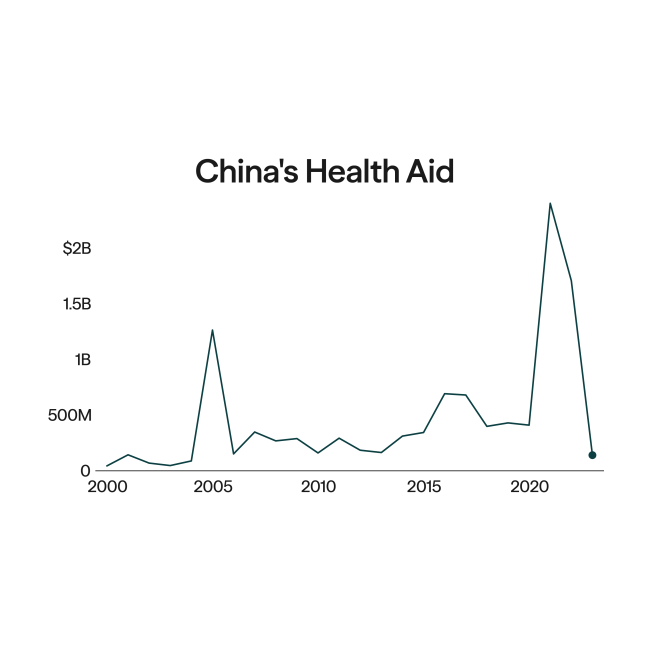
On April 11, 2024, Moderna announced that it had paused a $200 million plan to build a vaccine production plant in Kenya. Given little demand for COVID vaccines in Africa, the plans are unlikely to be resurrected.
This is a far cry from two years earlier, when the pharmaceutical and biotechnology company announced a $500 million investment in the Kenyan site to supply Africa with as many as 500 million doses per year of its mRNA vaccines. Although the initial plan was to start production in early 2023, the timeline and total investment was scaled back as demand for vaccines faded. In its cancellation announcement, Moderna stated that demand in Africa "is insufficient to support the viability of the factory planned in Kenya."
It is difficult to argue against this logic. Moderna delivered only 3.1 million doses to Africa in 2023, and countries are now canceling future deliveries.
The failure of the proposed investment is simply the latest in a long list of unsuccessful efforts at diversifying pharmaceutical production through so-called local production in Africa. Although production at strategically located regional centers would address issues of equity and supply chain breakdowns, which plagued distribution of COVID-19 vaccines on the continent, such centers should be economically feasible.
Here is where the idea for local production often breaks down. It is not only that new facilities would likely not be able to produce vaccines as efficiently as established sources in countries such as India and China, but also that infrastructure, technical know-how, investment climate, trade barriers, and regulatory frameworks may not be suitable for a sustainable production. Moreover, to be sustainable, a production facility needs to be economically viable, not simply exist (or fail) because of donations.
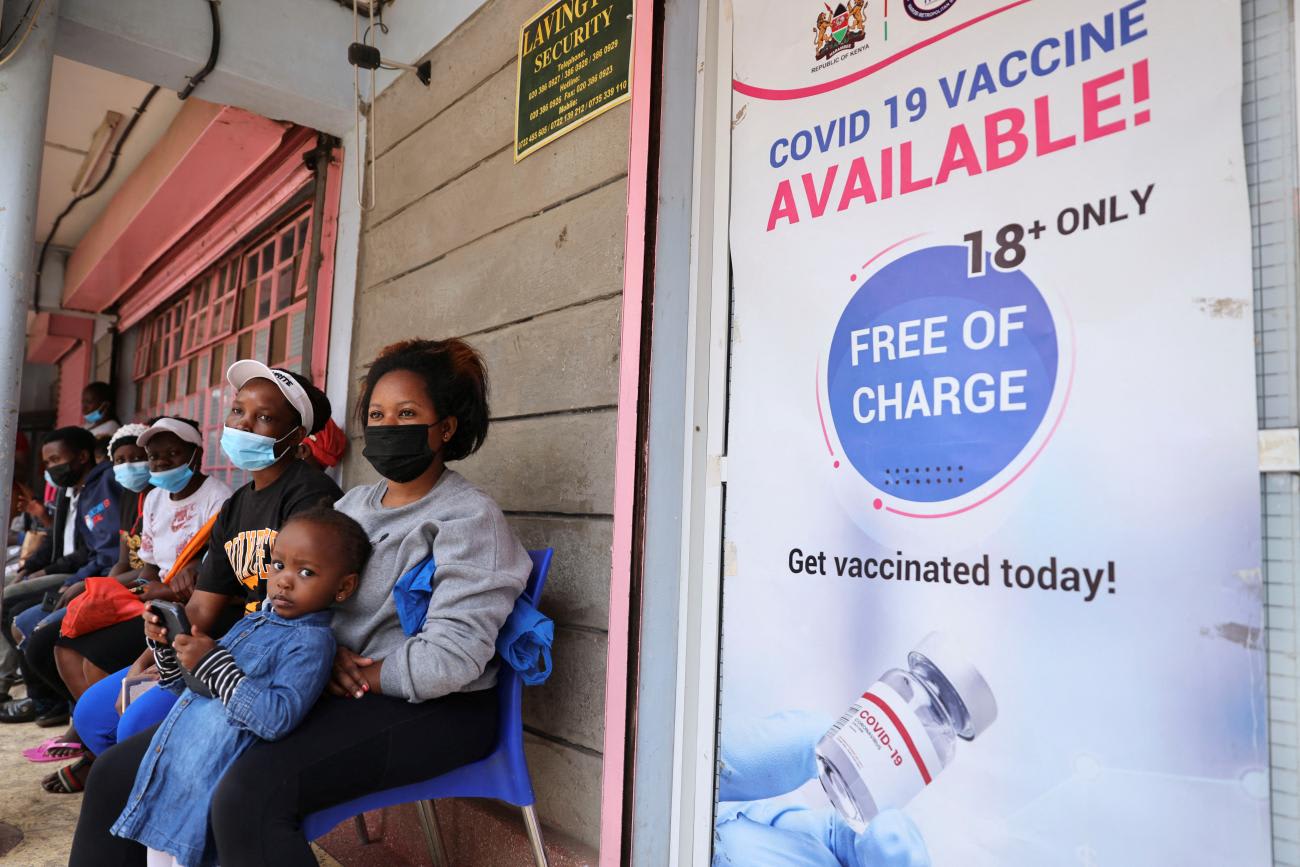
Local production can and should play a critical role in pandemic preparedness. But a factory designed to produce only COVID-19 vaccines is no longer needed, nor is it economically viable. Instead, governments, innovators, generic firms, and public and private donors should follow through on commitments made at the height of the pandemic to build sustainable vaccine production facilities—ones that can produce and sell vaccines in demand at present for profit but with the capability to be quickly retrofit to produce vaccines should another pandemic or crisis emerge.
This does not exclude innovator companies from building and operating production facilities (such as BioNTech's vaccine manufacturing facility being constructed in Rwanda) but does suggest that broader efforts—including the Coalition for Epidemic Preparedness and Institut Pasteur de Dakar partnership to build vaccine production capacity in Senegal, the World Bank–supported efforts to assist Kenya's BioVax Institute to develop and operate vaccine production facilities in Kenya, and the World Health Organization's partnership with Afrigen Biologics to establish a hub and spoke model sharing technology and know-how relating to mRNA vaccines—could be more successful.
The Math Behind Moderna's Move
The cancellations have, according to Moderna, led to $1 billion in losses and write-downs. Even more, Moderna has received no new orders from any African country or health body since 2022.
Given Moderna's prominence during the pandemic, it is easy to forget that the company is in essence a small-scale enterprise, the COVID-19 mRNA vaccine being its sole approved product. Because of the decline in the demand for the vaccine, revenues are expected to come in at $4 billion this year, down from $18.4 billion in sales in 2022—a 78% drop. The company has also seen its share price fall by more than 75% in this period. In this context, Moderna's decision to cut costs and downsize COVID-19 manufacturing seems sensible.
The COVID-19 pandemic shifted the debate on local production from a discussion (ultimately dismissed) to a strategic imperative
The cost savings will allow Moderna to focus on other efforts. These include not only its next generation coronavirus vaccine and a combined COVID-flu vaccine, but also a vaccine targeting respiratory syncytial virus (RSV) and testing of vaccines against latent viruses, norovirus, Epstein-Barr virus, the virus that causes shingles and chickenpox, multiple sclerosis, and a subcategory of lymphoma in solid organ transplant patients.
In the announcement, Moderna stated that it remains committed to "ensuring equitable access [for the COVID vaccine] and meeting emerging demands from African nations." In regard to the latter, the company claims to be in the early stages of research targeting diseases, including HIV and malaria, that disproportionately affect Africa. The company stated such an approach will allow it "to better align its infrastructure investments with the evolving health-care needs and vaccine demand in Africa."
The COVID-19 pandemic shifted the debate on local production from a discussion (ultimately dismissed) to a strategic imperative. The years following the pandemic have demonstrated that establishing and diversifying production facilities remains a complex challenge.
As the horrors of the COVID-19 pandemic fade from memory, the interest of the global community in pandemic preparedness is also waning as wars and economic instability take over the headlines. Moderna's abandonment of its plans in Kenya should serve both as a reminder that efforts to ensure equitable distribution of vaccines are not complete and as a call to global stakeholders to recommit to diversified production as a necessary safeguard and essential part of pandemic preparedness.

AUTHORS' NOTE: This research is supported by the Hong Kong RGC Senior Research Fellow Scheme 2022/23 for a project entitled: Access to Vaccines in a Post-COVID-19 World: Sustainable Legal and Policy Options (Project No. SRFS2223-4H01). The views expressed in this publication do not necessarily represent the views of others involved in the project.