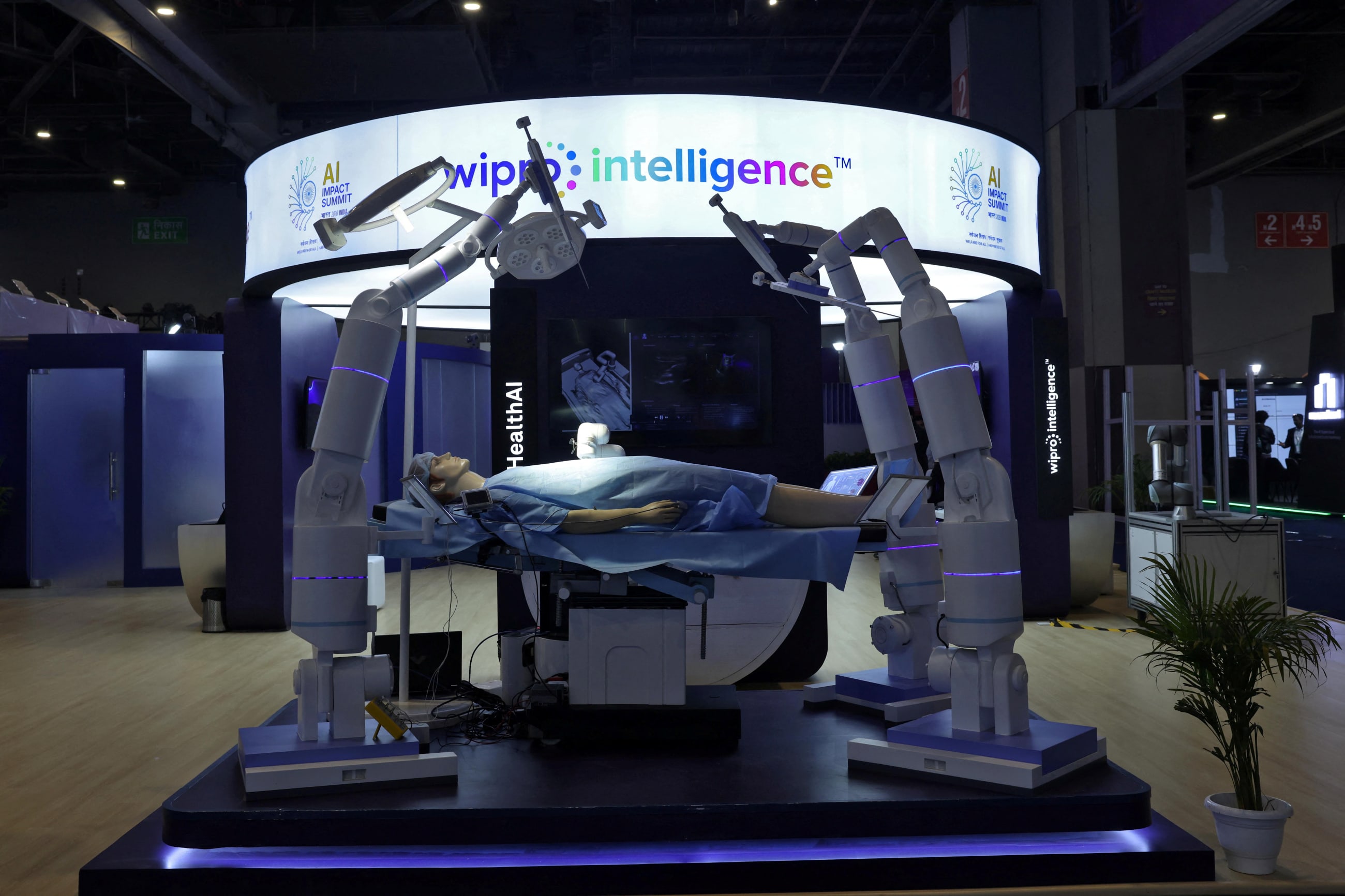
Health systems worldwide are undergoing rapid digital transformation as electronic health records, digital insurance platforms, and digital monitoring systems become integral to service delivery, financing, and governance. The use of artificial intelligence (AI) to automate and support such digital processes is growing commonplace. Since 2023, a fundamental technological shift means that narrow task-specific AI tools meant for specialized users—such as intracranial bleed scans for radiologists—are giving way to broad-purpose agents built on foundational medical models, including open source systems such as Meditron or MedGemma, which are designed to support generalist functions across diagnosis, decision-making, management, education, and research.
The flexibility of such agents across clinical contexts comes at the cost of reduced traceability and auditability, making them significantly harder to regulate and oversee. As a result, digital and AI governance has become a core determinant of health system performance and legitimacy.
Yet global debates on the subject remain dominated by three competing visions: rights-based regulation in the European Union, market-led innovation in the United States, and state-centric techno-nationalism in China. These models shape how health data is regulated, how digital health markets evolve, and how AI is deployed in clinical and public health settings. However, no vision fully addresses fully the structural challenge of delivering equitable, large-scale, and financially sustainable digital health systems.
India's approach constitutes a fourth paradigm of digital governance, particularly for global health
Over the past decade, India has developed a distinct approach to digital and AI governance centered on population-scale public infrastructure. This model integrates digital identity, payments, authentication, and data-sharing into welfare and health systems. It now underpins insurance enrollment, provider payments, disease surveillance, telemedicine, and pharmaceutical supply chains for hundreds of millions of people.
India's approach constitutes a fourth paradigm of digital governance, particularly for global health. It demonstrates how AI and digital systems can be aligned with universal health coverage while strengthening capacity for administration and innovation. Its implications extend well beyond low- and middle-income countries (LMICs), offering lessons for health systems struggling with fragmentation and platform dependence.
Digital Governance as Health and Social Policy
In February, at the AI Impact Summit in New Delhi, India launched a new strategy for artificial intelligence in health care for India (SAHI) that established governance principles for ethical, transparent, and evidence-based AI deployment across clinical care and public health systems. SAHI recognizes AI as a strategic enabler of health system strengthening, but stipulates that its adoption must be anchored in public interest, trust, and long-term system resilience.
The strategy covers five pillars: governance, data and digital infrastructure, the workforce, research, and ecosystem enablement. It addresses the need for interoperable digital infrastructure for scalable algorithmic development and proposes national mechanisms for testing, benchmarking, and validating health AI tools before large-scale implementation. Digital and AI tools are embedded directly into health financing, service delivery, and accountability mechanisms such as central dashboards and performance tracking. Governance is exercised primarily through public stewardship of shared digital infrastructure, such as the open interoperable digital rails of the Ayushman Bharat Digital Mission or shared cloud computing and publicly provisioned data under India AI Mission, thereby reducing barriers for affordable innovators.
A defining feature of India's model is its integration of digital governance into health financing, service delivery, and welfare administration. Digital systems support health insurance management and provider reimbursement, patient identification and continuity of care, telemedicine and remote consultation, disease surveillance and outbreak response, and pharmaceutical and vaccine logistics.
AI applications are increasingly embedded in those infrastructures to separate risks, forecast supply needs, support clinical decision-making, and monitor programs.
SAHI treats digital and AI systems as instruments of administrative capacity and redistribution rather than as commercial products or security tools. In countries characterized by financial constraints and large informal sectors, such as India, that approach enables governments to expand health services and insurance coverage while containing costs.
India's model could also help expand universal health coverage. Digital public infrastructure reduces transaction costs, leakage, and exclusion, allowing large-scale programs to operate with greater efficiency and transparency. It aligns technological innovation with equity objectives such that the products of innovation remain affordable and accessible for underserved populations, including those in remote areas.
A Fourth Paradigm of Digital Governance
SAHI reflects a new form of governance oriented toward development and inclusion characterized by public ownership of core digital infrastructure, open interoperable technical standards, state stewardship of an ecosystem that encourages private innovation, and innovation over restraint with regulation calibrated to the actual risk. As AI becomes embedded in everyday governance, these features offer a distinctive pathway for aligning technological change with public purpose.
The coupling of infrastructure, regulation, and service delivery exemplifies India's distinctive governance philosophy and offers an alternative to competing philosophies centered on public rights, market freedom, or state control.
From Platforms to Public Health Infrastructure
Most digital governance debates focus on regulating private technology platforms. In Europe, governance emphasizes legal safeguards and risk-based oversight. In the United States, innovation and competition dominate. In China, digital systems are closely integrated into state power and security strategies.
Across health systems, those approaches have produced mixed results. Fragmented electronic records, proprietary hospital software, vendor lock-in, and weak interoperability remain persistent challenges in the United States and many other countries. Health officials in those countries often lack strategic control over critical digital assets, limiting their capacity to govern data flows, AI deployment, and service integration. The Chinese model is one of the most integrated state-enabled systems globally. Its distinctive features are a combination of government structures, platform ecosystems, and data practices that are not easily transferable.
India's emphasis on interoperable digital public infrastructure incentivizes private technology companies to build digital health services on existing public frameworks. Open application programming interfaces (APIs)—an agreed set of rules that enables two software programs to communicate with each other—allow public and private actors to build digital health services without touching the underlying infrastructure. The ease of integration allows broad interoperability that spans identity systems, payment rails, authentication services, and digital mechanisms by which a person can give consent for sharing data. This provides ease of scaling in a large markets and is likely to be a major motivator for private actors to accept digital health models.
That the state builds and mandates the shared layer, then steps back to let innovation happen on top of it, is a type of stewardship central to India's health governance model. It reduces dependence on dominant vendors, enables exchange, and strengthens public oversight of data-intensive health systems. Digital governance is thereby transformed from a regulatory issue into an element of health system design.
Beyond the Global South
India's digital model is often interpreted as a solution for LMICs. However, high-income nations also struggle with siloed health information systems, proprietary platforms, and deep vendor lock-in that drives up switching costs and constrains public-sector strategic control.
Digital identity infrastructure in countries such as the United Kingdom and state-level ecosystems such as in the United States combine public standards with private providers without adequate binding requirements for interoperability. This practice limits portability across services and undermines public oversight. Regulatory approaches alone have proved insufficient to resolving these structural dependencies.
India's experience demonstrates that publicly governed health infrastructure can counter those trends. By establishing shared technical standards and open interfaces, governments can reclaim strategic control of the digital backbone without stifling innovation.
India's model is not without risks. Large-scale data systems raise legitimate concerns regarding privacy, surveillance, and function creep. Digital exclusion remains a challenge for marginalized populations. Governance responsibilities are distributed across multiple agencies, and regulatory capacity has not always kept pace with technological expansion. Finally, open and interoperable digital public goods, the backbone of this model, need sustained investments and political commitment.
These vulnerabilities underscore that infrastructure-centered governance requires strong legal safeguards, independent oversight, and sustained public investment. Without these, digital public infrastructure risks reinforcing rather than reducing inequalities.
India has pioneered a model of digital and AI governance that places health systems and social protection at its center. By treating digital systems as public infrastructure, it has enabled large-scale service delivery, fostered innovation, and expanded administrative capacity.
The AI Impact Summit and the launch of a national AI-in-health strategy demonstrate that this approach is not merely retrospective but also continues to evolve through institutional innovation and global engagement.
Although developed for LMICs, SAHI addresses structural challenges across income levels. Its relevance extends beyond development cooperation to debates on platform power, digital sovereignty, and welfare state reform.
India's experience suggests that the future of AI governance could stem from design and stewardship of shared public infrastructures rather than market incentives. By drawing on India's model, countries can build digital health systems that serve collective rather than narrow interests.