Peru has had a rough time of it during COVID. The South American country, draped along part of the continent's Pacific coast, is famous for Machu Picchu and its pink dolphins, which swim in the Amazon River. But its beauty hasn't masked Peru's more than two million COVID cases and close to 200,000 deaths—hefty numbers compared to most other Latin American nations. There is a deeper story behind those figures, though, Patricia "Patty" García, former Minister of Health for Peru, told us. She also shared some of the challenges Peru has faced this past pandemic year, and spoke of her beloved country's strengths and efforts to quell infection spread.
□ □ □ □ □ □ □ □ □ □ □ □ □
Think Global Health: Starting with a broad question, how does Peru's COVID situation compare with that of its neighbors in Latin America?
Patty García: Before COVID, I think for decades—even when we're talking about global health—Latin America has been forgotten. It has been left behind and forgotten. It's the land of inequities; we have very few people that have a lot, and then there are a lot of people who have nothing. But because we measure using averages, that creates this false sense in the world that Latin America is doing well.
But I think that after this pandemic, it's very clear what has happened. Latin America has been hit very hard, and unfortunately, my country Peru is one of those countries that has been hit harder than others. It's even more visible because we have been able to count what is going on.

Think Global Health: Can you talk a bit more about that—how has Peru tracked COVID cases and deaths?
Patty García: There are countries in Latin America where you don't really know what is going on [with COVID data collection]—Cuba, Venezuela, Bolivia—where it's not that clear. In Peru, we have been working toward building better information systems.
A little history: I was Minister of Health in Peru from 2016 to 2017. I tripled the average time of ministers of health in the country. There have been eleven ministers of health in the past almost five years. It's crazy. It's terrible because it means we never have enough time to do things. I am an epidemiologist but I also work in medical informatics, and one of the things I was very concerned about was information systems in Peru. While I was health minister, we were able to evaluate what was going on in information systems in our country and we have a very fragmented system. Instead of having one system, or interoperable systems, we have many and they don't talk with one another.
Peru was one of the first countries in Latin America counting COVID deaths in a very clear and transparent way
I saw we could begin collecting data. We needed to choose one thing to begin tracking and I realized we could do that with mortality. Working with the Bloomberg Foundation Philanthropies and their program Data for Health-D4H, we decided to improve the system for death certificates. During the time I was minister, we were able to start an electronic death certification system that was relatively simple and accessible. One thing that had been difficult to get in the past was the right diagnosis. Everybody was putting "heart stops." But that doesn't mean anything. So for the new system, we started implementation and training with physicians on coding diagnoses. That was 2017. In 2018, it continued. In 2019, I was already at the university and together with the Pan American Health Organization (PAHO), we organized a meeting to evaluate how things were going and actually, it was moving along. PAHO was interested and I continued working on it even though I was no longer minister. And then in January 2020, I invited the Institute of Health Metrics at the University of Washington—I'm a member of their advisory board— and there was this opportunity to discuss how to collect better data and use the information from this death certificates. The quality and the coverage of these deaths certificates was much improved. So by the time COVID-19 cases started in Peru, we had this system for electronic death certificates. Additionally, what was done as part of the response to the pandemic was to make it completely mandatory and add incentives to report deaths (many people die at home), such as funerals paid through the government.
So, we were one of the first countries in Latin America that was honest in counting COVID deaths. We have been counting in a very clear and transparent way. I was part of one of the expert advisory groups of the government in the beginning of the pandemic and we supported that the data should be open, and it still is.

Think Global Health: When the pandemic first arrived in Peru, were you prepared since you had seen so many other countries go through it first?
Patty García: First it was in China, then Europe—Italy and Spain. Then the United States and then it reached South America. By that time, we were supposed to be prepared. But when we got cases, all of the other continents were suffering and there was no personal protective gear available, or supplies for laboratories to purchase—markets were closed. In Peru, we have only one national laboratory that could do PCRs [PCR tests detect viral RNA]. They didn't have enough supplies. I was trying to find where we could buy supplies for molecular testing because we were running out. It was not possible to buy anything. The United States was not selling anything. Korea, as was the case in other countries, was only producing for themselves.
So, at the start of the pandemic, we had a lot of people with symptoms who were not diagnosed because we did not have supplies for testing. Peru eventually bought what was available, rapid serologic tests, from China. We were one of the first countries in Latin America who used rapid serologic tests and our definition of a case of COVID included rapid serology or PCR testing positive for COVID. We tested anyone who was sick and also people who had died, so our counts were higher than most.
Think Global Health: What are some of the other factors that Peru has had to contend with during COVID?
Patty García: There are three things: inequities, political instability, and the third is the culture. It's very hard for us to do social distancing. We do not have good housing conditions and water sanitation is a problem in general in Peru. We are so used to living with extended family and to being close to each other. We do it as part of our culture, but also when there are no resources, so families need to live together in small spaces. I have seen COVID cases happen in a house that only has one room where 15 people live.
Another factor is the high rate of informal work, which means in order to get the money you need to eat, you have to leave your home, go to the street and sell services or whatever. With the first lockdown in Peru, lots of people were desperate because they couldn't work and the government was not able to address the needs of the population. So even knowing that they could get infected, people were exposing themselves to the virus to survive. People who were in Lima working informally could not stay in the city and started moving back to their hometowns, spreading the disease.
Our first case was in March 2020 and it took until July and August 2020 to reach the peak of cases, and it stayed in a flat high until October. Cases started going down in November, but in December, cases slowly started to rise again and our second wave began and stayed high until around early June 2021 and right now we're seeing it come down. With all of the lockdowns, the economy has been destroyed. There are lots of places that have closed. The percent of poverty has increased. The number of people without jobs has increased, too. Schools have been closed for almost one year-and-a-half now. Survivors from COVID-19 are struggling, families are struggling. It is a complicated time.

Think Global Health: Have Peru's academic institutions been working with the government on pandemic control efforts?
Patty García: All academic institutions tried their best. But the government was not open to collaborations. As an example, in Peru, we have 24 regions and about half have academic laboratories which had the capacity for molecular testing (due to investments of the National Council of Science and Technology, or CONCYTEC), but the Ministry of Health, actually through the National Institute of Health, was not willing to have them help. Complicated requirements were created, and it was very difficult and took a long time for these academic laboratories to be able to contribute with the processing of samples. That's been one of the problems with the response in Peru—not being able to convene, to call everyone to the table. We have had so many changes, so many ministers of health, and the government was not calling on all sectors to make it work together.
Think Global Health: How was the Lambda variant discovered?
Patty García: In December 2020, the world started talking about COVID variants but we didn't have the capabilities to study them and no money. In February or March, eventually some universities began working with the Peruvian National Institute of Health doing some sequencing. They found a variant that had not been seen before and by then, we were in our second pandemic wave and that was mainly. attributed to the Lambda variant. This variant was also found in Bolivia and Chile.
Just recently—and again we don't have a systematic approach for sequencing in our country—about a month ago, the government found the presence of the Delta variant in the southern part of Peru. They were trying to do "rings of control," trying to test everybody. It seems that the Lambda variant is the predominant strain, but in a country where you are not doing it systematically it's difficult to tell. Then four or five weeks ago, the Delta was found in Lima. However, cases are now coming down. Apparently, what drove our second wave was mainly the Lambda variant, but we don't know why the Delta has not spread yet. Now with the midyear vacations, the risk of a third wave is there.
12 percent of Peru's population has been vaccinated with two doses—a month ago it was about 1.5 percent.
Think Global Health: How are COVID vaccines being rolled out? And are people receptive?
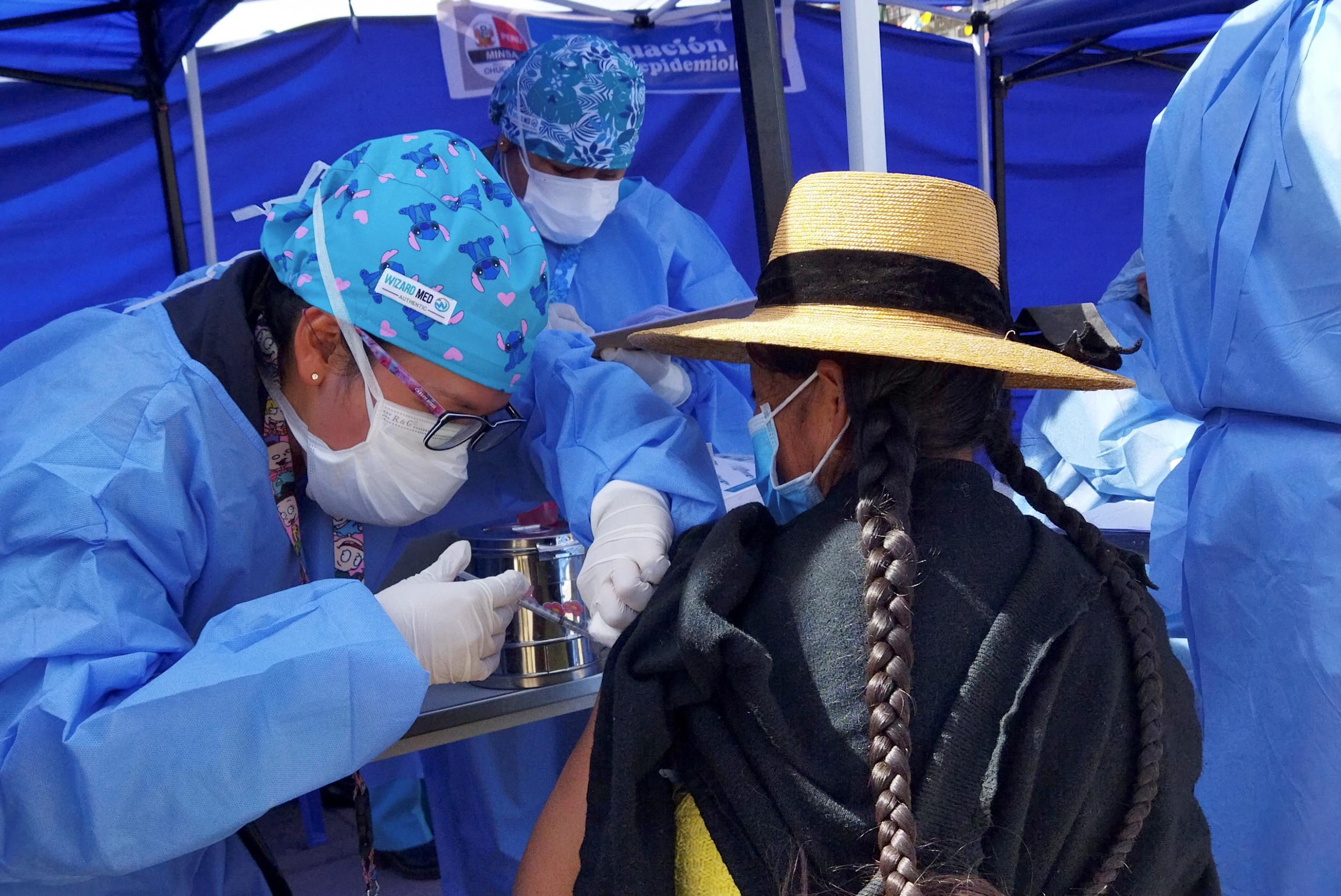
Patty García: We started vaccinating in Peru in February with the Sinopharm vaccine. We received about one million doses, but the process of vaccination was very slow and mainly for health personnel and key workers. COVAX has been very slow, too. Later, in the next few months, we got a first batch of Pfizer vaccine, 100,000 doses. We have even changed three presidents in this timeframe. Eventually they were able to sign a contract with Pfizer and that has helped us a lot. People were vaccinated according to age and risk factors. We are in the process of vaccinating people 40 and older right now. We now have about four million people who have received two doses of the vaccine.
We are 30 million people total. That means 12 percent of population has been vaccinated with two doses. A month ago we were at about 1.5 percent. Now we're vaccinating around 50,000 to 100,000 people a day. People in Peru believe in vaccines. People stand at the vaccination sites all night in a queue waiting because they want to be vaccinated. South Americans have always been champions of vaccines.
Cases are probably coming down because of COVID-19 vaccines. I hope the speed of vaccination will continue despite the recent change of government [on July 28], and that all the promises and contracts to continue receiving vaccines will remain. We are still far from protected, and what is happening in other parts of the world with the new Delta variant is worrying.












