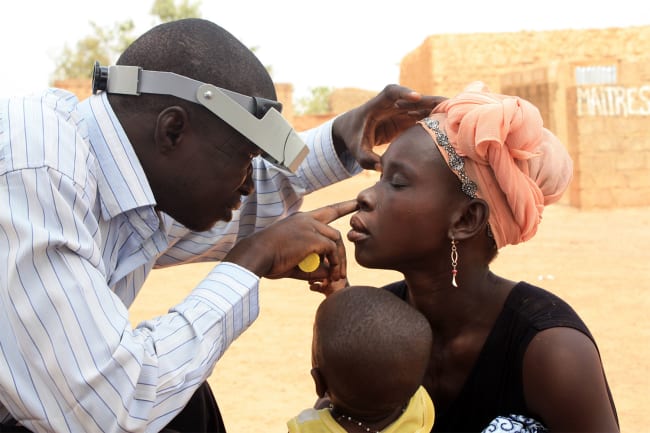
Even the possibility that health care facilities would not have water, soap and toilets sounds ludicrous. But the widespread lack of access to Water, Sanitation, and Hygiene, known within global health and development circles as WASH, is a reality that impacts health around the world, complicating infection prevention, challenging efforts to contain pandemics, and contributing to the spread of antibiotic resistance.
Providing safe water, working sinks and toilets, waste management systems, and the ability to practice good basic hygiene like hand washing is clearly a solvable problem and certainly is not too much to ask. Success hinges not on scientific or technological breakthroughs—but on three reasonable, systemic changes.
First, WASH systems and health systems can no longer operate independent from one another. From policy and people to institutions and resource allocation—everyone needs to step out of their silos and integrate their efforts locally, nationally and internationally.
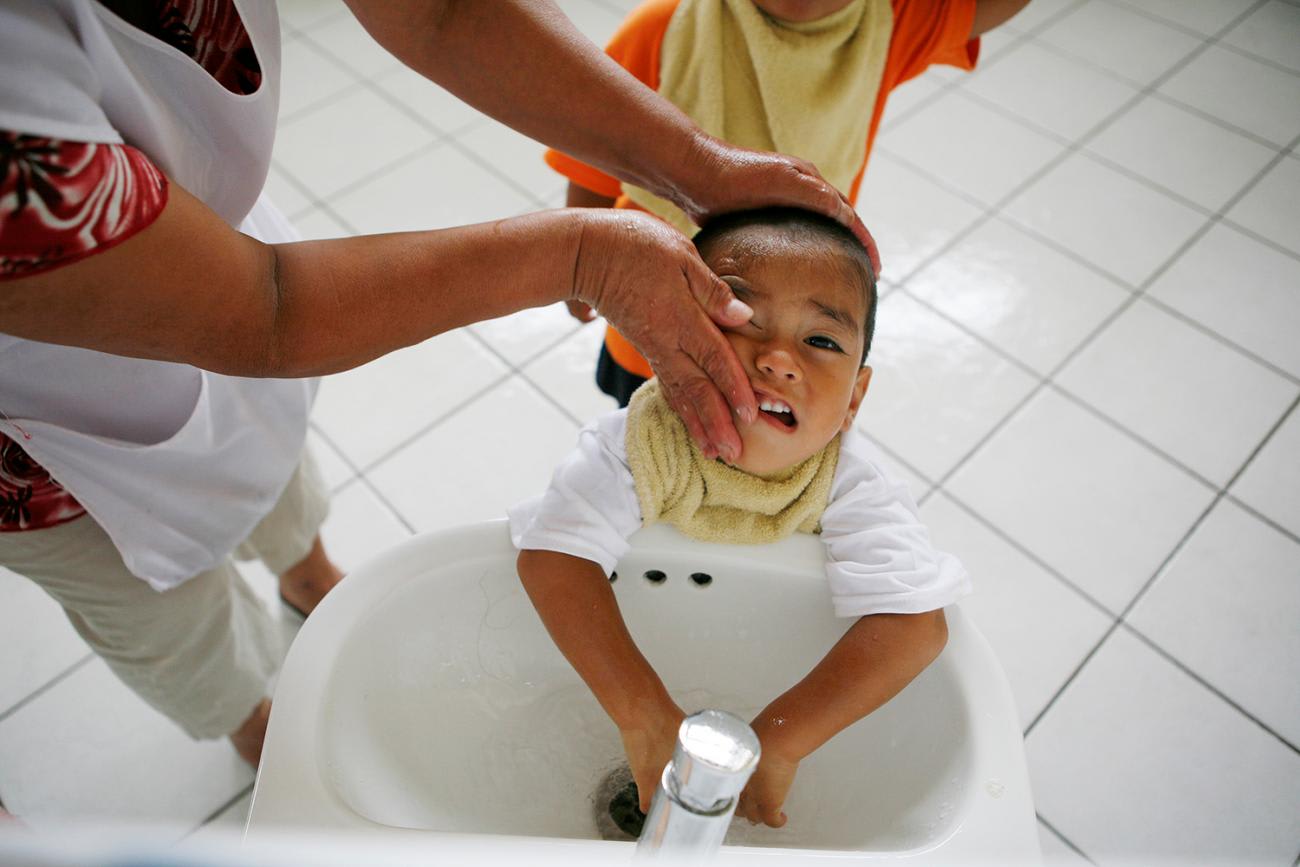
Second, WASH projects must, from conception, include commitments to ongoing training and maintenance. Broken pumps, pipes and faucets are part of any WASH system. Success has been elusive, in many places, because sustainability has not been part of the plan.
It doesn't matter how nice a new facility or building looks if health care providers can't wash their hands
Third, WASH requires a budget. We've got to stop building and retrofitting health care facilities with no budget line items for WASH installation, upgrades, or maintenance. It doesn't matter how nice a new facility or building looks if health care providers can't wash their hands. WASH investments not only strengthen health systems that are still evolving, they also offer long-term economic impact when productivity is not lost to poor health. That's a good return on investment. And while costs are neither trivial nor excessive given the benefits, they are expected to decrease when WASH is integrated into health care facility designs, plans and operations, and as health care facilities and community WASH systems are better connected.
"There are no shortcuts to a healthier world. We need to realize that health is an investment in the future," wrote World Health Organization (WHO) Director-General Tedros Adhanom Ghebreyesus last month when he named the 13 most urgent global health challenges in the coming decade. WHO's list includes getting WASH into healthcare facilities for the very first time. "Countries invest heavily in protecting their people from terrorist attacks, but not against the attack of a virus," he wrote with prescience, "which could be far more deadly, and far more damaging economically and socially. A pandemic could bring economies and nations to their knees."
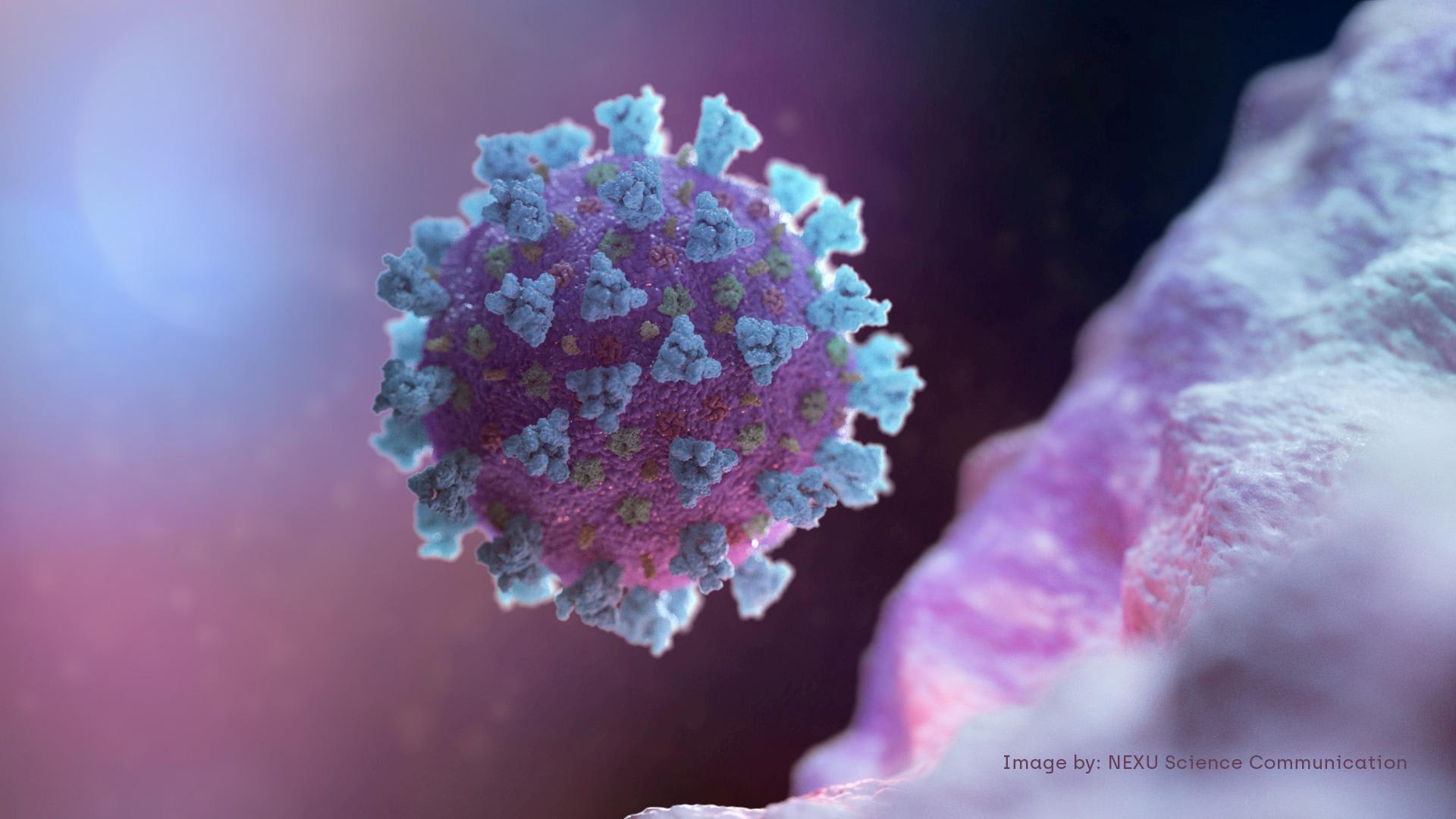
Enter coronavirus. When faced with a novel virus that has no vaccine and is spread person-to-person through coughing, sneezing and fecal contamination—the coronavirus is but the most recent example—other than trying to avoid those who are sick (which is impossible in a health care facility) the single best way to stay healthy is to for everyone to wash their hands and properly dispose of waste. But when soap, water and waste management are absent in health facilities, everyone, from patients to health care professionals to the cleaners, are at daily risk.
In the Democratic Republic of Congo, half of all healthcare facilities have no clean water
Consider the 2014 Ebola outbreak. Ebola not only killed some 11,000 people, it was 103-fold higher in healthcare workers in Sierra Leone than in the general population and 42-fold higher in Guinea health workers. Liberia lost 8 percent of its health workforce, in part because they did not have access to adequate WASH, according to the U.S Centers for Disease Control and Prevention (CDC). As of the publication of this article, according to China's National Health Commission, at least 1,716 health care providers have contracted coronavirus and at least six have died.

In early 2018, WHO published its annual top ten list of prioritized diseases that pose the greatest public health risks. That same summer, the world experienced the unprecedented and simultaneous outbreak of six of those ten diseases, including the current Ebola outbreak in the Democratic Republic of Congo, where half of all healthcare facilities have no clean water, 59 percent have no sanitation facilities, and 38 percent don't have soap and water or hand sanitizer at points of care.
Some 20 percent of deaths worldwide are due to sepsis—or "blood poisoning" as it is commonly known
We know this data because in 2019, WHO/UNICEF issued the first-ever global assessment detailing conditions in hundreds of thousands of healthcare facilities in low- and middle- income countries: 1 in 4 health facilities lacks basic water services; 1 in 5 lacks any sanitation; and 2 in 5 lack hand hygiene facilities at points of care. That 17 million women in Least Developed Countries give birth in facilities without WASH every year is unacceptable, denies them dignity, and gravely endangers their lives and the lives of their newborns. The venerable Lancet Commission on Quality Healthcare found that poor quality health facilities kill more people than HIV/AIDS, malaria and Tuberculosis combined.

This issue is not just "over there". A recently-released Lancet study cites sepsis as being far worse than previously known—double previous estimates—and responsible for at least 20 percent of deaths worldwide. Sepsis, or "blood poisoning" as it is commonly known, is the body's overreaction to an infection and causes organ failure. More than 40 percent of sepsis victims are children under five and not surprisingly, 85 percent of those cases are in low- or middle-income countries.
However, sepsis also kills some 258,000 people in the United States every year and costs nearly $24 billion to treat, making it the most costly condition in the U.S. hospital system. A fundamental way to curtail sepsis is to prevent hospital-acquired infections through improved WASH practice, and that must include all practitioners, everywhere, consistently washing their hands.
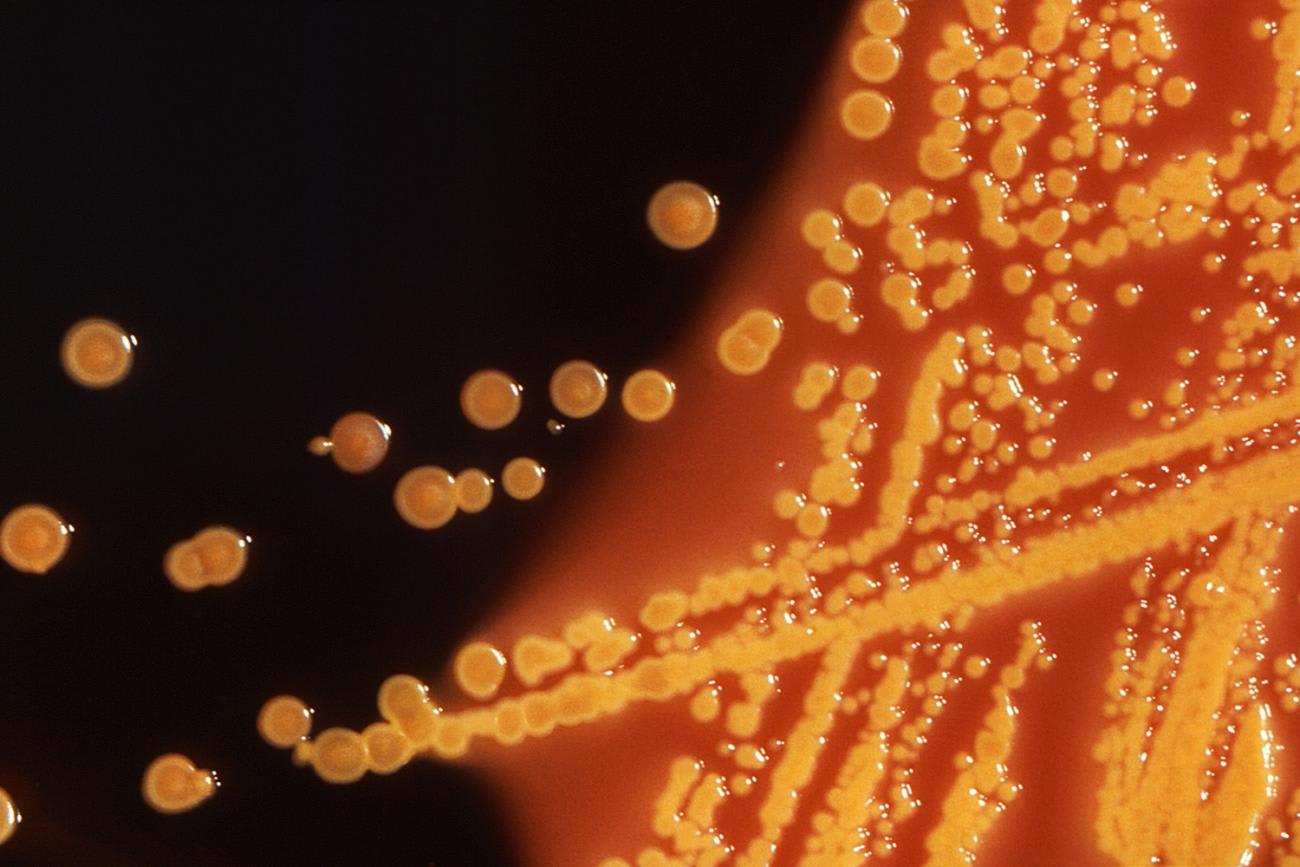
But it is WHO's warning [PDF] about antibiotic resistance that should stop each of us in our tracks: "Without urgent action, the world is headed for a 'post-antibiotic era' in which common infections and minor injuries which have been treatable for decades can once again kill, and the benefits of advanced medical treatments such as chemotherapy and major surgery will be lost."
Public health is ultimately a political choice
WHO Director-General Tedros Adhanom Ghebreyesus
Antibiotic resistance is widespread across twenty-two countries, but no country is immune. According to the CDC, the United States experiences an estimated 2.8 million cases of drug resistance each year resulting in some 35,000 deaths and spends $2 billion annually to combat resistance. But such efforts are undermined when globally, the overuse of antibiotics substitutes for infection prevention and control that includes, you guessed it, WASH. As WHO Director-General Tedros noted in his recent announcement, WHO's new global health priority list was developed by experts from around the world and "reflects a deep concern that leaders are failing to invest enough resources in core health priorities and systems. "Public health is ultimately a political choice," he wrote.
Coming on the heels of UN Secretary-General Antonio Guterres's 2018 Call to Action to get WASH in health care facilities and WHO Member States' unanimous adoption of a Resolution [PDF] to this effect in 2019, WHO's new prioritization of WASH in health care facilities is well-timed as coronavirus breeds fear into the hearts of millions of people.
Let's hope prioritization breeds resolute action.