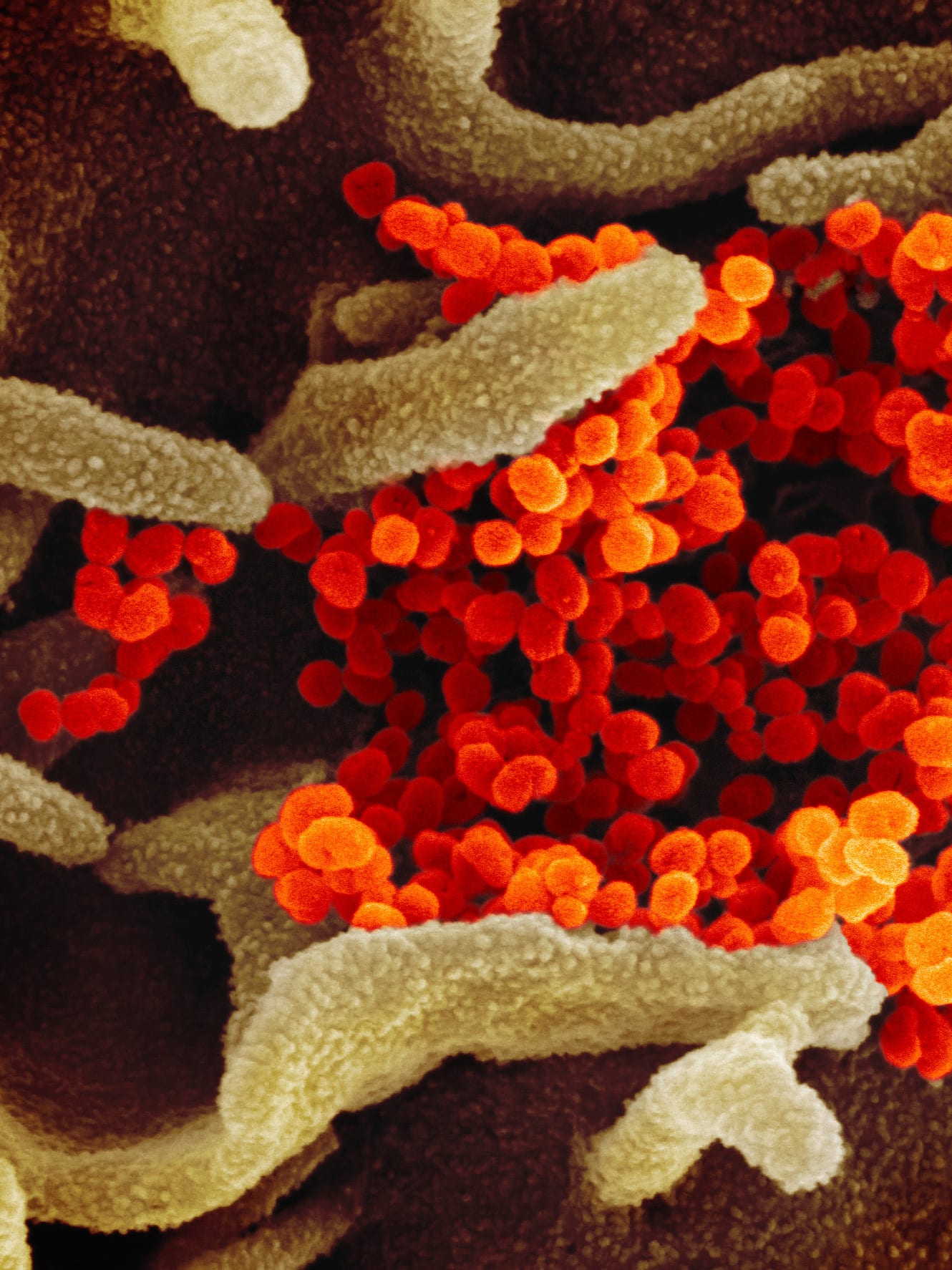
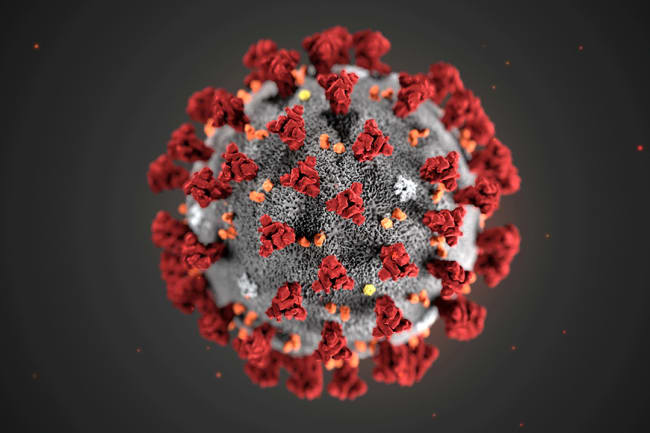
Three weeks ago, I wrote about what we need to know to confront the new infection that's now known as COVID-19. Two weeks ago, I summarized emerging scientific knowledge, including that the virus spreads within households and hospitals more readily, although with less deadly outcomes, than SARS. Last week, I shared my alarm at extensive spread within one hospital as an indication of how risky COVID-19 is for health care workers and the public, as occurred with SARS and MERS and was just confirmed for COVID-19.
There are at least half dozen good reasons to be pessimistic about containment
Right now, the crucial question for the world is whether the virus can be contained and eliminated, as SARS was, or is destined to continue to spread, as other coronaviruses that cause the common cold do. Containment means that the virus is eliminated, as we think SARS was eliminated, and no longer spreads among people. The odds of containment look vanishingly small, but not (quite) yet zero. There are at least half dozen good reasons to be pessimistic about containment, which may be why the U.S. Centers for Disease Control and Prevention (CDC) is foreshadowing that containment may be impossible:
- The huge number of reported infections in China, which undoubtedly is a substantial underestimate of the actual number of infections (if the reported case-fatality rate outside of Hubei province is more accurate and equivalent to the rate inside the province, there are already hundreds of thousands of infections in Hubei alone);
- Spread to provinces all over China [PDF];
- Exportation so far to two dozen other countries;
- Disease models [PDF] that suggest that the number of infections recognized in other countries may only be a small fraction of the actual number of people who left China infectious with the virus;
- Ease of spread within hospitals, taxis, families, shopping centers, possibly related to infectiousness of patients who aren't severely ill, and cruise ships (including a report out of Japan that of 454 people testing positive on the Diamond Princess cruise ship, 189 were asymptomatic, which could facilitate widespread transmission);
- Recognition of cases with no known link to other cases in Singapore despite that country having one of the best health care systems in the world.

On the other hand, all is not yet lost, and the benefits from containment would be enormous. There are at least half a dozen reasons not to give up hope:
- The extraordinary efforts of China to contain the virus could succeed—in some provinces, reported cases appear to be decreasing;
- Availability of rapid PCR testing enables confirmation of disease and implementation of isolation and control measures, and genetic testing doesn't suggest further evolution of the virus yet;
- Testing of thousands of other people at risk in the United States and Singapore, among other places, has not identified other patients, suggesting that there may not be as large a reservoir of undiagnosed patients with mild disease as feared;
- Apparent success of efforts to contain the virus in countries that have had imported cases, including the United States;
- SARS and MERS, similar coronaviruses, were both contained once their means of spread were well understood;
- Decreased travel out of affected areas has greatly reduced the potential for additional exposures.

We continue to learn more about the disease by the hour. And, by the time you read this, it may have already become clear that containment is not possible. If containment is possible, this will take weeks or months to confirm. In either case, the urgency and intensity of our response will be affected by the actual case fatality rate.
Containment would make an enormous difference to health around the world, but what practical difference does it make to what we need to do now?
If the virus is containable, then the travel restrictions put in place by many countries are both defensible and necessary
If the virus is containable, then the approach must be all-hands-on-deck to find infections and stop them from spreading in China and anywhere in the world. In this scenario, core public health measures such as early testing and isolation, contact tracing, and monitoring contacts are essential. The effectiveness of cordoning off entire communities and limiting travel is less clear, although it could slow diffusion of the virus, particularly from Hubei province, the current epicenter. If the virus is containable, then the travel restrictions put in place by many countries are both defensible and necessary. Even if containment isn't possible, the intensive control measures being implemented in China and elsewhere may help slow and limit harms the virus causes.
If the virus is not containable, then rational control measures will depend on both how contagious and how severe the virus is. In all scenarios, some simple strategies are essential:
- Protect health care workers and make sure health care facilities don't become amplification points;
- Wash your hands regularly;
- Cover your mouth and nose with a tissue (or your sleeve, not your hand) when you cough or sneeze;
- Don't expose others if you're sick with cough and fever: stay home unless you need health care; if you go out, wear a mask; if you go to a health care facility, if possible, inform them in advance that you may be infectious.

If the virus is not containable, spreads widely, and continues to have a case fatality rate in the 1 percent range, then we will be in uncharted territory – similar to an influenza pandemic, but caused by a different virus. Fortunately, extensive analysis and planning has gone into preparing for an influenza pandemic, and most of this planning is relevant in this worst-case scenario. Here's what communities can do to blunt the health harms of a pandemic with a high case fatality rate, well outlined by CDC for influenza.
In this worst-case scenario, first, reduce the number of people who get infected. This can be done by closing or curtailing hours of schools, limiting public gatherings, and increasing social distancing; encouraging handwashing and cough etiquette; quickly isolating those who are ill or who are at risk for becoming ill and infecting others; and cleaning frequently touched surfaces. Reducing spread to health care workers, patients, and visitors in hospitals is particularly important.

Second, improve the chances of survival for those who are infected. This will require rapid diagnosis, learning about and applying optimal management for patients severely ill with the virus, and scaling up supportive care, including supplemental oxygen and mechanical ventilation to support patients until their infection subsides.
Third, maintain essential services, including both health care and broader social and economic activity. For example, public and private sector institutions may need to plan to continue operations if 40 percent of their employees are ill or quarantined—again, in the worst-case scenario.
Whatever happens with this coronavirus, we need much stronger public health systems, to find faster, stop sooner, and better prevent harms from the inevitable new infectious disease threats we will face in the coming years. Investing in these systems is urgently needed and could save the world tens of billions of dollars and millions of lives when the next new infection strikes.