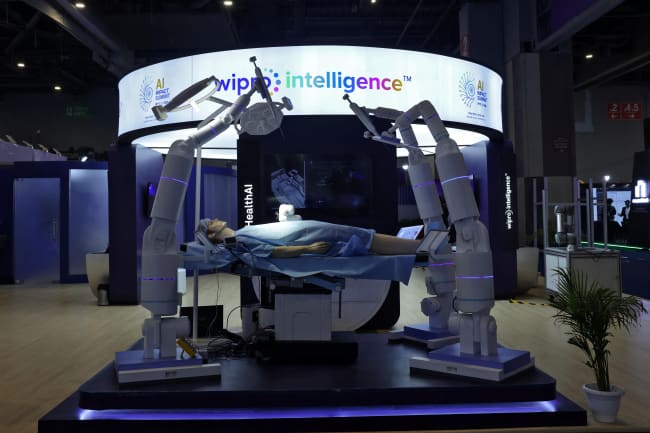
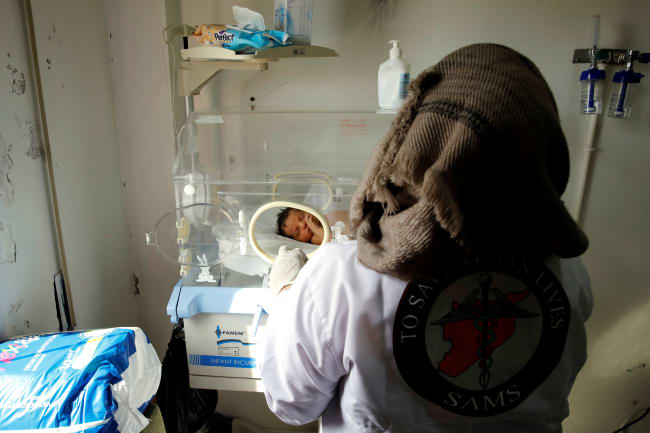
Monkeypox has been around for more than five decades, mostly in central and west Africa. But more recently, cases of the virus have cropped up all over the world, puzzling scientists who are working to track and stem transmission. As of Wednesday, June 22, there were 3,308 cases of monkeypox reported in 42 countries, according to the U.S. Centers for Disease Control and Prevention.
To better understand the latest outbreaks, we spoke with David Pigott, assistant professor of health metrics sciences at the Institute for Health Metrics and Evaluation (IHME), at the University of Washington. Pigott's research involves tracking the spread of diseases that have the potential to cause pandemics, including monkeypox, Ebola, Zika, and COVID-19.
□ □ □ □ □ □ □ □ □ □ □ □ □ □ □
Think Global Health: How worried should people be about monkeypox?
David Pigott: I think they should be aware of what's going on and pay attention to ongoing updates from their local health authority, but I think there is a relatively low risk at a population level. So far, a large number of infected individuals have some association with other infected individuals. If there are ten cases that have no connection to each other, that is far more concerning than all of them being connected. This is very different from what we saw with COVID-19—there were all kinds of disconnected cases and unknowns for the first people diagnosed with COVID in different countries in Europe.
Confirmed Cases of Monkeypox in 2022 Outbreak
Think Global Health: What should we be watching for with monkeypox transmission?
David Pigott: From a population level, we should take note if there are large numbers of people who become infected who are not connected to each other in some way, which indicates unknown and uncontrolled spread of the pathogen. I'm paying attention to this because that would be a sign that things are going wrong.
It is unsurprising to identify hundreds of people who have become infected among those who were close contacts of people who were infected. That's why we do contact tracing. Contact tracers have detected mild monkeypox infections in people this way, by notifying people who have come into contact with individuals who were infected.
At an individual level, be on the lookout for unexpected rashes and lesions. Go get them checked out if you develop them.
Think Global Health: The World Health Organization is investigating whether monkeypox could be transmitted through semen. How likely do you think this is?
David Pigott: Sexual acts tend to require direct physical contact, so I don't think sexual transmission is necessary to explain what is going on in terms of transmission. It is not unprecedented for a number of different viruses to be present in seminal fluid. Ebola stands out as a recent example of a pathogen that was detected in semen, but is more frequently transmitted via other mechanisms, such as coming into contact with blood or body fluids of a person who is sick with or has died from Ebola virus.
Be on the lookout for unexpected rashes and lesions, and go get them checked out if you develop them
Think Global Health: Could these outbreaks become deadly?
David Pigott: I'm not sure we have a good understanding of how transmissible and how severe monkeypox is. In prior outbreaks, people have died from monkeypox, but it has always been a relatively low proportion of those people who became infected. Keep in mind that if you're looking at the reported numbers of people who have died from monkeypox compared to the reported number of people who have been infected with the virus, you're not getting the whole picture. When you are detecting cases, you're only seeing the tip of the iceberg in terms of the true number of people who are infected. Through contact tracing, you start to assess how big the iceberg is. You need additional studies, such as seroprevalence surveys, to truly understand the size of the iceberg.
Think Global Health: What types of policy interventions are warranted, in your opinion?
David Pigott: Positive impact can be achieved by public health officers doing what public health officers do—figuring out who has been at risk of getting infected with monkeypox and testing them. If you defund those groups, then you're going to fly blind when you need those activities. At the same time, you shouldn't be concerned if, by virtue of doing those activities, the number of people that you're finding who are infected goes up and are therefore added to case counts. You don't want to penalize places for doing a thorough and transparent job, as we saw with South Africa and Botswana when they sounded the alarm about omicron in late 2021.
Think Global Health: Are there any other insights that you'd like to share about monkeypox?
David Pigott: This is a further reminder of a key notion in global health security, that a pathogen somewhere in the world—by virtue of how humans behave, travel, and interact—could spread anywhere. This sense of "other" is really problematic. Repeatedly, we've seen Nigerian officials report cases of monkeypox for the past four to five years. Why didn't we have a more global conversation on monkeypox before Europeans and other high-income, non-endemic countries started to report cases?
There are many African experts on monkeypox who have been working to bring attention to this virus for years. If you want to protect the world from health threats, you need to focus on a world's worth of health problems, not just on the countries that can shout the loudest.
With Ebola and to a certain extent Zika, there were events that catapulted them into global notoriety and made us think more proactively about these viruses. Why does monkeypox have to get to this scale before the world pays attention to it? We should think about how we can meaningfully prepare for these kinds of disease outbreaks without cases increasing to the level of a public health emergency of international concern. How do we sustain support for the proactive research that is essential for informing a successful response?

EDITOR'S NOTE: The authors are employed by the University of Washington's Institute for Health Metrics and Evaluation (IHME). IHME collaborates with the Council on Foreign Relations on Think Global Health. All statements and views expressed in this article are solely those of the individual authors and are not necessarily shared by their institution.