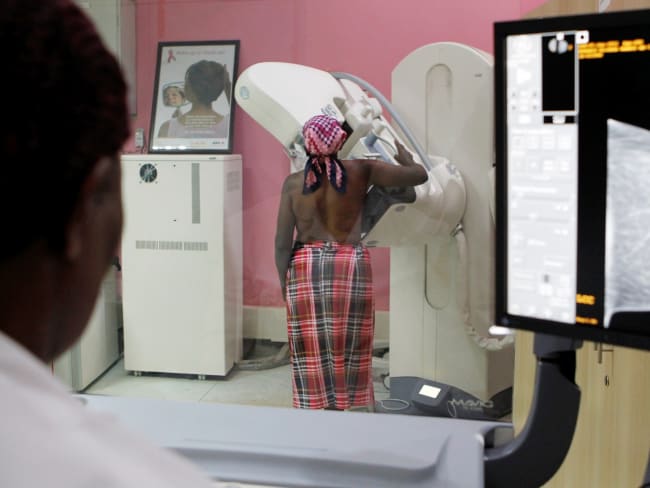
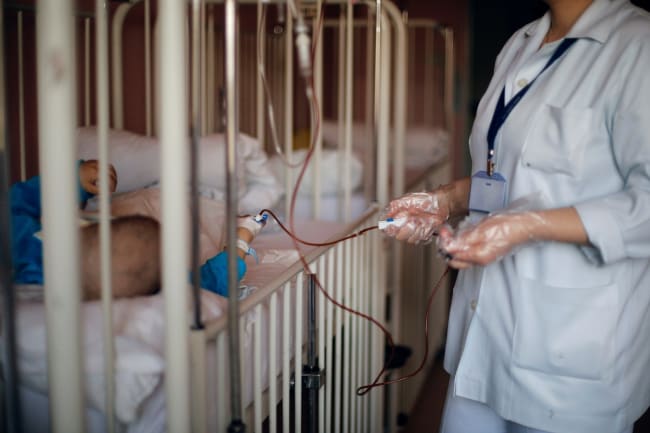
According to recent data, Mexico's death rate from cancer is 37 percent that of the United States. This rate, though, clashes with the perceptions of the Mexican public and of medical professionals, who see cancer far more frequently. The discrepancy is explained by the numerous deficiencies in how Mexico identifies cancer cases and provides care.
A health system that fails to register a cancer case could reflect poor prevention, detection, or care—or all three. Countries can differ significantly in their rates of cancer due to differences in behavior and environment. The uncertainty in measurements of cancer incidence in Mexico, however, precludes the development of good policy, which depends on consistent knowledge of the way cancer is affecting individual patients and the population as a whole.
Currently, the scarcity of information about cancer in Mexico means that the government grants too little attention to the problem and issues few policy publications about it.
A study has shown that the rate of noncommunicable disease deaths is 60 percent higher in Mexico than the United States
Data from the Global Burden of Disease project sheds further light on this issue. Drawing on mortality data for each of the fifty U.S. states, the District of Columbia, and the thirty-two states in Mexico for each year from 1990 to 2019, a recent study shows that Mexico has a 20 percent higher rate of injury deaths, and that the United States and Mexico have comparable rates of communicable disease deaths. Mexico, though, has 60 percent the U.S. rate of noncommunicable disease deaths, mainly because of its younger age distribution.
After controlling for risk factors, Mexico still has lower rates of registered cancer deaths, but the gap between the countries narrows considerably. Our research suggests the cancer gap between the United States and Mexico is not as large as measured by average mortality rates, but we need better data to know whether the remaining gap is due to mismeasurement or reflects differences in social and environmental factors.
This research underscores the importance of investing in prevention and measurement, including the development of cancer registries. Employed by many developed countries, these data information systems aim to provide timely and accurate information on incidence, treatment, and outcomes of cancer cases. They are often fed from the bottom up: hospitals upload patient records to regional or national databases and an overarching organization manages the system. This organization may also support the development of standards for how the data are collected and how the resulting information is accessed or disseminated.
The country needs to enact public policies to strengthen the measurement of cancer in different stages of the health-care process
The Mexican Congress passed a law in 2017 establishing a national cancer registry but only the registry for children is operating, and with major limitations. The Health Ministry's 2022 Annual Report doesn't even mention the cancer registry.
The country needs to enact public policies to strengthen the measurement of cancer in different stages of the health-care process, from prevention, to diagnosis, to care, to remission, or to death. Otherwise, providers will remain limited in the efficacy of the care they can provide, federal agencies that finance care will lack guidance to make good policies of their own, and physician and patients will continue to navigate uncharted waters.
Research on the extent of mismeasurement can be useful to create awareness of the need of investing in training, prevention, and information systems. Only solid federal action, however, can resolve the issue of provision of this life-saving public good.