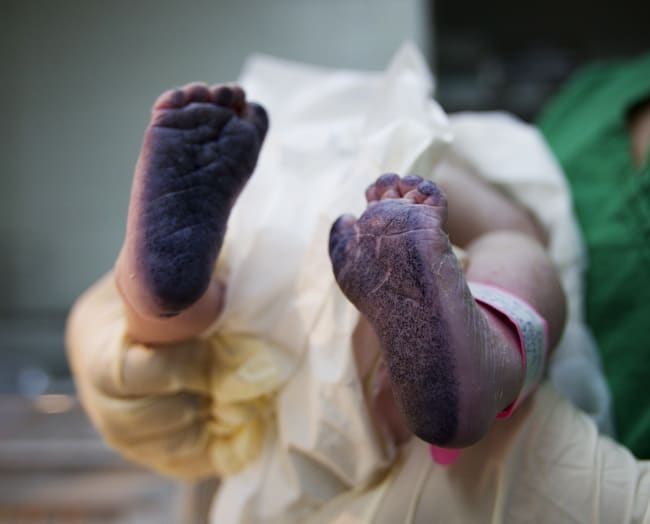
"We really should be very, very angry that in the twenty-first century we are still talking about women dying of cervical cancer when we have the tools, we have the technology, and we have the know-how [to address this disease]," said Princess Nono Simelela, the assistant director-general for family, women, children, and adolescents at the World Health Organization (WHO), at the Commonwealth Women's Forum 2022 in Kigali, Rwanda, last June.
According to the Global Burden of Disease (GBD) 2019 Study, cervical cancer was the fourth most commonly occurring cancer in women globally in 2019—with human papillomavirus (HPV) the main culprit behind most cervical cancers. The GBD Study also shows that women in countries that fall lower on the Socio-demographic Index (SDI) experience greater cervical cancer mortality and burden than women in high SDI countries. These troubling statistics highlight the need for comprehensive cervical cancer control strategies. The WHO adopted the Cervical Cancer Elimination Initiative in 2020 to reinvigorate such efforts, calling for all countries to achieve three main targets by 2030, necessitating policies focused on preventative measures, such as vaccination against HPV, and equitable access to cervical cancer screening, as well as effective treatment of precancerous cervical lesions and invasive cervical cancer.
"We really should be very, very angry that in the 21st century we are still talking about women dying of cervical cancer"
Princess Nono Simelela, WHO
Lowering Vaccine Doses
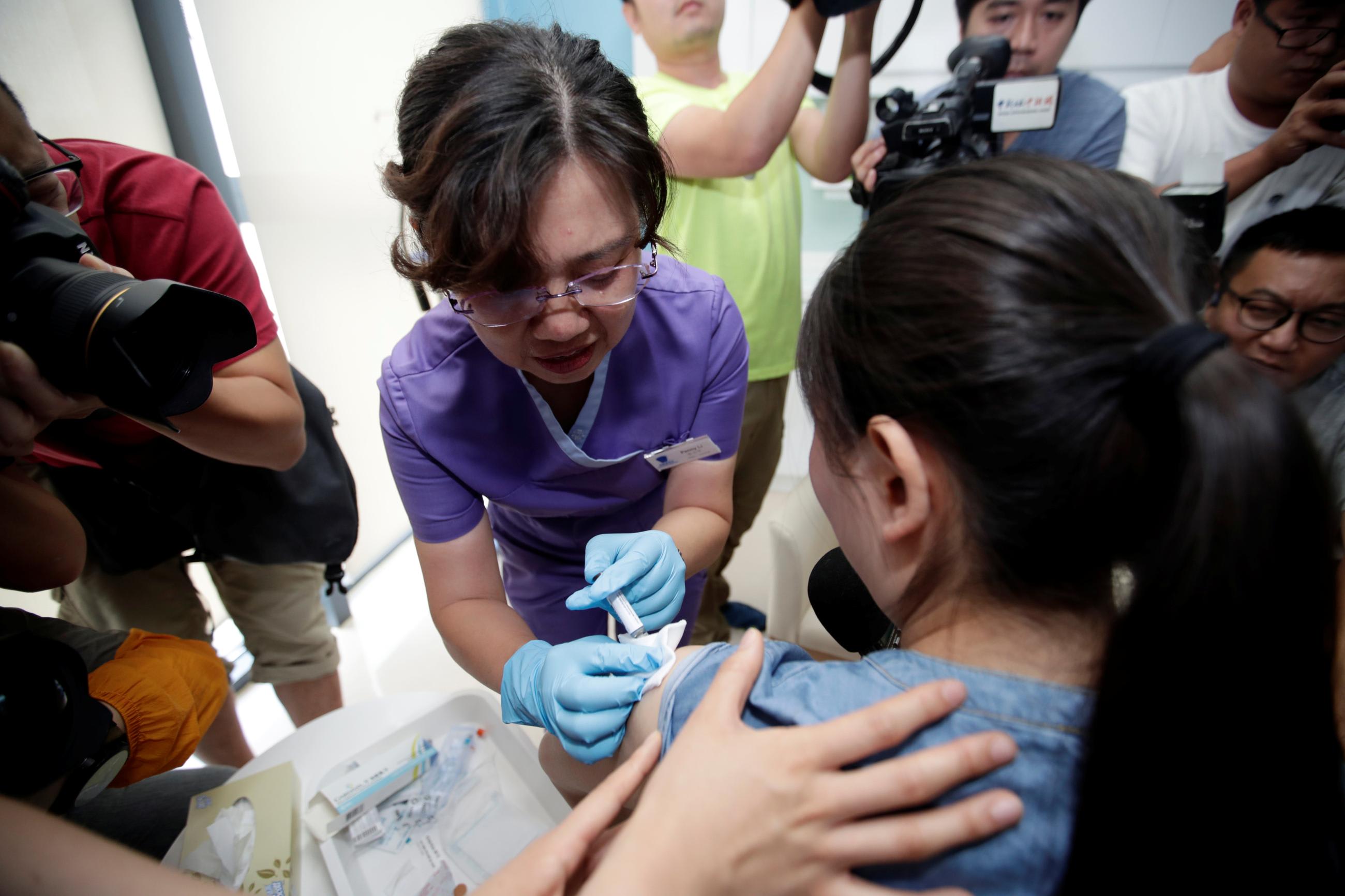
As Simelela said, health-care providers and policymakers have the tools: cervical cancer is a vaccine-preventable disease. Recently, a single-dose HPV vaccine was found to be as effective as multiple doses, according to a study conducted at Kenya Medical Research Institute clinical sites, which tested the single-dose efficacy of two different HPV vaccines—a bivalent one that protects against two high-risk HPV types and a nonavalent version that offers protection against nine types of HPV. In December 2022, the WHO cited this study in their revised recommendations, noting that a single dose provides comparable efficacy to a two-dose regimen, a shift which will hopefully allow HPV vaccines to be more accessible in low- and middle-income countries.
Lowering the number of required doses from two to one means that the cost of the HPV vaccine has been halved, said Marcia Weaver, professor of health metrics sciences at the Institute for Health Metrics and Evaluation (IHME), who was not involved with the study in Kenya. She co-authored a separate study on the cost-effectiveness of HPV vaccination by synthesizing evidence on incremental cost-effectiveness ratios (ICERs). ICERs are like unit cost pricing at the grocery store; a lower ICER means a lower cost per one year of healthy life gained.
"Let's say the cost of the vaccine was the same across two countries—which it is for most countries eligible for support from Gavi, the Vaccine Alliance—and the prevalence of HPV was higher in one country than another. In a country where the prevalence is higher, every time you give a vaccine to a girl or a boy, the chance that you're preventing HPV is higher. So you're saving more lives, and the cost per year of healthy life gained is lower," said Weaver.

Weaver stressed that countries eligible for pricing through Gavi, a public-private partnership that provides vaccine support for children in lower-income countries, should implement HPV vaccination programs. Through Gavi, Merck's quadrivalent Gardasil vaccine is priced at $4.50 per dose until 2025.
"Countries should definitely be taking advantage of the vaccine at this price," said Weaver.
National HPV Vaccination Programs
One country that has their HPV vaccination program partially funded by Gavi is Rwanda, which could become one of the first countries in the world, alongside Australia, to eliminate cervical cancer.
"The Rwandan national program on HPV mass vaccination of young girls is well over a decade old and the dividend of such large-scale societal investment is already visible in the country," said Jonah Musa, professor of obstetrics and gynecology at the University of Jos in Plateau, Nigeria.
Musa pointed out that unlike Rwanda and Australia, Nigeria does not have HPV vaccination in their national immunization program. Meanwhile, twenty-four other Gavi-eligible countries had launched HPV vaccine national programs as of 2021, and Sierra Leone joined the group in October 2022. When asked about the barriers that Nigeria and other countries face in investing in HPV vaccination programs, Musa said, "I will simply say the main barrier to this is lack of political will."
Unlike Rwanda and Australia, Nigeria does not have HPV vaccination in their national immunization program
He elaborated that a joint effort between the national government and a host of experts—from health economists to political scientists, lawyers to gynecologists—would reveal that prompt investment in cancer prevention is paramount, instead of hoping for a miracle cure.
One example of several sectors working together to sustain a national initiative is the case of South Africa's school-based HPV vaccination program, adapting to vaccinate girls in grade 5 who missed the typical vaccination in grade 4 due to COVID-19–induced school closures.
"With well-coordinated collaboration," Musa said, "national governments and society will see clearly and appreciate the need to invest for prevention of a cancer that is preventable."
A Worthy Investment
For middle-income countries that are not eligible for Gavi pricing, financial barriers are still a concern. While the WHO Pan American Health Organization region has a Revolving Fund to provide lower priced vaccines (~$10.48 per dose) to its Gavi-ineligible member states and territories, other WHO regions do not have equivalent mechanisms. But a recent breakthrough holds potential for more affordable vaccines; in September, India announced the launch of a domestically developed HPV vaccine, Cervavac, that protects against four HPV types. It's expected to cost between 200 and 400 rupees (about $2.43 to $4.85), which would be at least seven times less expensive than the current $33.97–$40.03 prices in India for Merck's Gardasil (protecting against four HPV types) and GSK's Cervarix (protecting against two HPV types) vaccines. Not only is this a boon for India, but the Cervavac vaccine is also expected to be exported to other countries after shoring up the country's domestic supply.
Large-scale HPV vaccination initiatives are a worthwhile investment for mitigating overall cancer burden globally, especially in lower SDI countries. A recent study in The Lancet assessed the association between thirty-four risk factors—including alcohol use and air pollution—and various cancers and found that in 2019, the risk of disease due to sexual transmission (termed as "unsafe sex" and modeled as a proxy for HPV infection in the study) was the leading risk factor responsible for deaths and ill health due to cancer for women in low and middle SDI countries. And it was the second leading cancer risk factor in women globally (behind smoking). Scaling up HPV vaccination also has the potential to prevent other cancers associated with HPV—such as oropharyngeal, penile, and anal cancers—and where "feasible and affordable," the WHO additionally recommends expanding vaccination to boys and older women. Vaccination should be part of comprehensive cancer control efforts that also support access to screening and treatment.
There is still a long way to go toward increasing HPV vaccination coverage and eliminating cervical cancer, especially as risk of disease due to sexual transmission continues to be one of the leading factors driving women's cancer burden around the world. The cost-effective measure of HPV vaccination is a critical yet sometimes missed component to comprehensive cervical cancer control strategies, but the recent progress in affordability provides hope that positive change is on the horizon.
AUTHORS' NOTE: In the absence of quality data that allow disaggregation by gender, we utilize data that disaggregate by sex, with the understanding that outcomes for people outside the gender binary are often less equitable than they are for cis women or men. In this article, "cancer" refers to malignant neoplasms only, excluding non-melanoma skin cancers and benign and in situ neoplasms.
ACKNOWLEDGEMENTS: The authors would like to thank Lisa Force, Jonathan Mosser, Ally Walker, Katherine Leach-Kemon, and Rebecca Sirull for their input, expertise, and guidance in the development of this piece.
EDITOR'S NOTE: The authors are employed by the University of Washington's Institute for Health Metrics and Evaluation (IHME), which coordinates the Global Burden of Disease Study (GBD) and engages the GBD Collaborator Network. Dr. Jonah Musa, who is quoted in this article, is a GBD collaborator. IHME collaborates with the Council on Foreign Relations on Think Global Health. All statements and views expressed in this article are solely those of the individual authors and are not necessarily shared by their institution.