People all around the world, including many Americans, wait breathlessly for news about new treatments for COVID-19 and vaccines to prevent it. Early on, reports of lives being saved by plasma donated by people who survived infection were promising. More recent reports have also been encouraging. "A cheap steroid is the first drug shown to reduce death in COVID-19 patients," read a headline in Science on June 16, 2020.
Facemasks are an easy-to-use, inexpensive tool that reduces coronavirus transmission by at least a third
This news gives hope. But in addition to using this drug, and facilitating the discovery of others, we need to make better progress on preventing people from catching the coronavirus in the first place, sparing them hospitalization, lasting medical complications, and even death. We already have an easy-to-use, inexpensive tool that reduces transmission by at least a third according to a recent analysis from the Institute for Health Metrics and Evaluation (IHME): facemasks. Unfortunately, in the United States, we're not using masks much as we should be—due to a combination of issues, including spotty commercial supplies, conflicting messages early on, non-use by many public figures, a lack of federal guidance, and conflicting requirements on the state and local levels.

Levels of mask usage in the United States are much lower than they are in other parts of the world, such as Asia, Europe, and Latin America. Singapore has the highest level of mask usage in the world with more than 90 percent of people wearing masks in public at all times.
Think of them as a lifeline for both our health and our economy
Masks are not a foolproof solution to COVID-19, but they are one of the best that we have available, coupled with handwashing, sanitation, and social distancing. Both cloth and medical-grade masks are effective in protecting the person wearing the mask according to IHME's meta-analysis of different studies of mask use. Increasing the use of masks is crucial for saving lives and delaying future lockdowns. In the absence of a vaccine or effective treatment for COVID-19, masks are one our best, easiest, and most affordable solutions. Think of them as a lifeline for both our health and our economy.

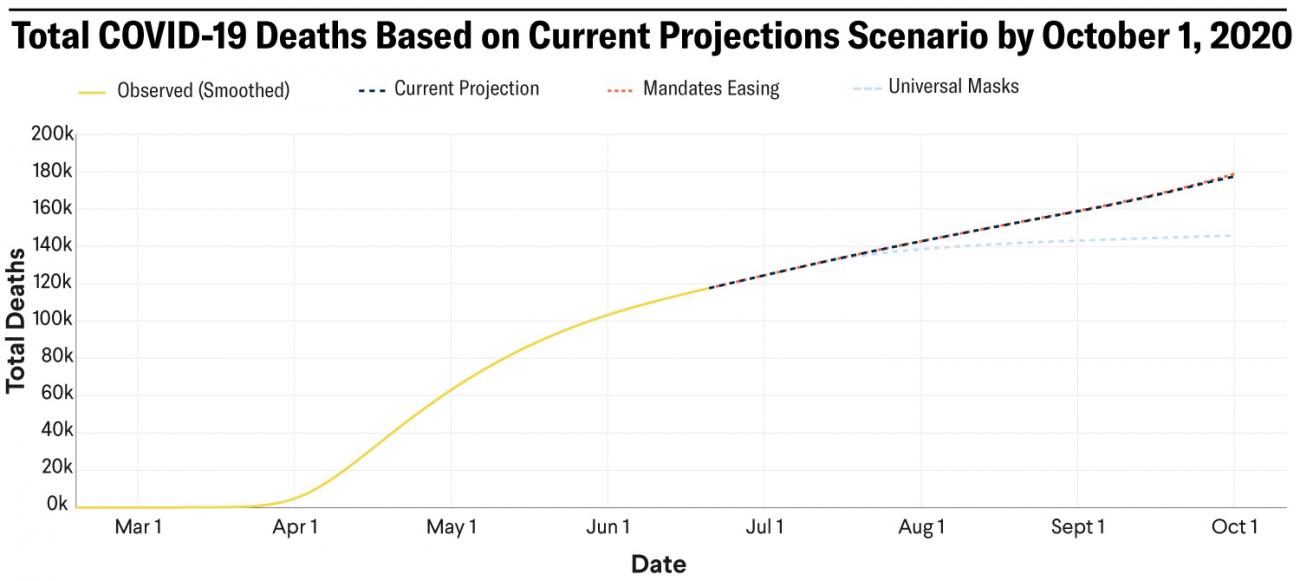
What's more, IHME's newest projections show that more than 33,000 deaths from COVID-19 could be prevented by October 1 if 95 percent of people in the United States wore a mask.
More than 33,000 deaths could be prevented by October 1 if 95 percent of people in the United States wore a mask
The need for aggressive action against COVID-19 is becoming more urgent every day.
Cases are beginning to tick up in states such as California, Florida, Georgia, and Arizona, and the worst may be yet to come as the weather cools. A second wave of COVID-19 looms, with 179,106 deaths forecast by October 1. If states do not succeed in reducing transmission come September, deaths from COVID-19 are expected to increase dramatically. And the less progress we make in the summer months, the bigger the second wave is likely to be.
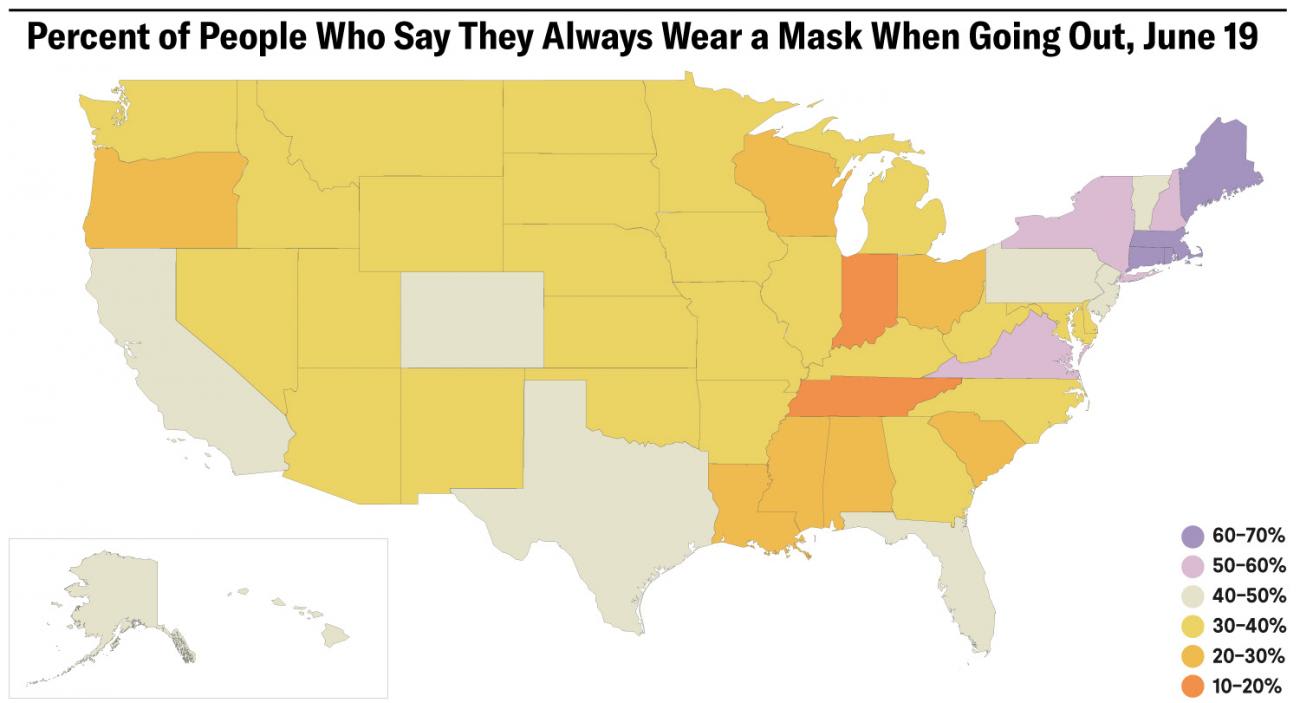
America is far from achieving 95 percent mask coverage, with coverage reaching just 60 percent in certain states. The states with the highest levels of mask use (50 percent or more) are Maine, New Hampshire, New York, Massachusetts, Connecticut, Rhode Island, and Virginia.
In Virginia, people are required to wear masks in all indoor spaces
Why do these states have higher levels of mask usage? Statewide mandates likely play a role. People are required to wear masks in public in those states unless they can maintain six feet of distance (but Maine requires everyone to wear a mask in public regardless of social distancing). In Virginia, people are required to wear masks in all indoor spaces. New Hampshire is the only state in this list that lacks a statewide mandate (masks are only required in parts of the state). Also, the high rates of mask usage in the Northeast could be due in part to the fact that this region was the hardest hit in the United States to date.

At the same time, there are many other states with statewide mask use mandates that have not yet achieved higher levels of mask use. So mask mandates may not be a perfect solution to increasing mask use. But encouragingly, a recent study published in Health Affairs found that mask mandates reduced COVID-19 deaths.
Radically increasing mask use in all U.S. states could change the trajectory of COVID-19 for the better
On June 18, Governor Gavin Newsom of California made wearing masks mandatory in public indoors, and in some outdoor places. Hopefully, this mandate will increase use of masks in a state where cases of COVID-19 are on the rise, and perhaps it will also prompt other states to pass similar mandates. Less than a week after California made masks mandatory, Washington state followed suit. Radically increasing mask use in all U.S. states could change the trajectory of COVID-19 for the better. Tennessee, and Indiana had the lowest levels of mask use with only 10 to 20 percent of people saying they always wore a mask when going out. Many other states had mask use of 40 percent or less. One of those states with levels of mask use at 40 percent or less is Arizona, a state where COVID-19 cases and deaths are rising the fastest.
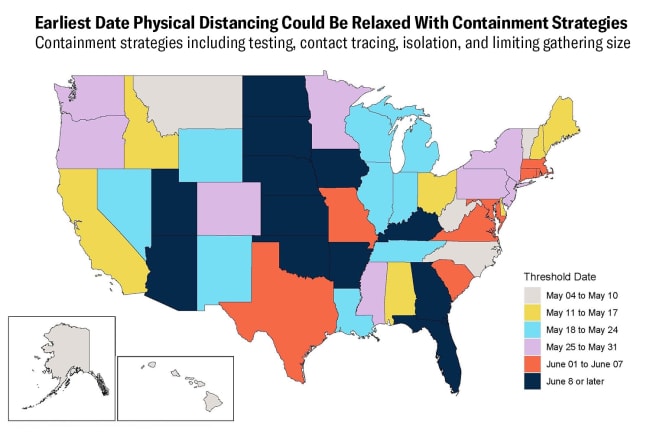
Arizona's chief health officer has called for hospitals to activate their emergency plans. On June 17, Arizona Governor Doug Ducey announced that mayors could begin requiring mask wearing, reversing a previous policy that prohibited them from doing so, but has yet to issue a statewide mandate.
Helping low-income communities access masks is important. In Hong Kong, for example, billionaire Adrian Cheng set up vending machines that provide free face masks to those who can't afford it, reaching 40,000 people. In the United States, some communities are distributing masks to vulnerable populations. In New York City, for example, officials delivered face masks to public housing residents.

When it comes to designing policies to encourage mask use, it is essential to keep systemic racism top of mind. For example, reducing racial bias is likely another vital component of increasing mask use. Black, indigenous, and people of color are often viewed with suspicion for wearing masks, placing them at risk for being targeted by police, security guards, and the general public. In addition, if states introduce universal mask wearing policies, police may single out Black people as they enforce social distancing mandates, so it is crucial to ensure that enforcement is carried out in an equitable manner.
[In] our country, we don't listen to authority. You go to Korea, you go to Japan, when the authorities say something, man, it gets done
Anthony Fauci, NIH/NIAID
Unfortunately such a simple, cheap, and effective measure to reduce the spread of the virus has become politicized in the United States. "We may have mayors and may have governors who are saying the right thing, but because of the individual spirit of our country, we don't listen to authority. You go to Korea, you go to Japan, when the authorities say something, man, it gets done," said Anthony Fauci, the director of the National Institute of Allergy and Infectious Diseases, and one of the leading U.S. infectious disease experts, in an interview with the Washington Post. Amid this backlash against masks, violence has erupted in some states: employees attempting to enforce mask-wearing requirements at businesses have been attacked and even killed.

To address these challenges, behavior change specialists emphasize the importance of establishing mask wearing as the new norm. Resources such as the Pandemic Playbook advise emphasizing how many people in the community are already wearing masks. Leaders in the community have a critical role to play by wearing masks themselves. Also, we must celebrate mask wearing on both sides of the political spectrum.
Masks can help us save lives and rebuild the economy by delaying lockdowns. U.S. states should act quickly to embrace this underutilized tool, which is one of the best tools available when it comes to preventing COVID-19.

EDITOR'S NOTE: The authors are employed by the University of Washington's Institute for Health Metrics and Evaluation (IHME), which produced the COVID-19 forecasts described in this article. IHME collaborates with the Council on Foreign Relations on Think Global Health. All statements and views expressed in this article are solely those of the individual authors and are not necessarily shared by their institution.