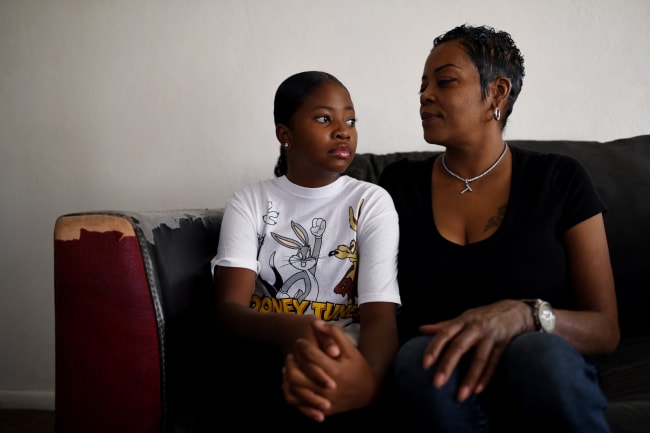Population growth has driven an increase in sickle cell disease (SCD) prevalence in countries south of the Sahel in west and central Africa. Due to a lack of data and a tendency for underdiagnosis and misattribution of the underlying cause of death, SCD is often overlooked in the global health agenda and is less prioritized by policymakers. A recent study estimated that Democratic Republic of Congo (DRC) has the third largest population of individuals with SCD globally (after Nigeria and India), with 655,000 people living with the disease and 47,400 babies born with SCD in 2021. We spoke to Leon Tshilolo, MD, a leading Congolese SCD expert and physician, and Doña Moleka, who was born with SCD and is now a public health activist and founder of the outreach organization S'POIR. They shared their insight on the influence of SCD in the DRC, recent progress in the country, and hopes for the future.
□ □ □ □ □ □ □ □ □ □ □ □ □ □ □
Think Global Health: What is it like growing up in the DRC with SCD?
Doña Moleka: People living with SCD are often discriminated against, as there are many myths attached to it. The lack of knowledge or access to information often leads people to believe children living with SCD are evil, often called enfants sorciers "witch kids" cursed to bring nothing but pain to their parents. I was blessed to be part of a social class that doesn't believe in those myths but that [still hears the] wrong information. I remember being in first grade and hearing one of my classmates say, "I might not live long because children with sickle cell don't pass the age of five." I was six at the time and I ran home asking my mom if that was true. I was lucky to have parents who taught me to love myself and who helped me to better understand my condition without being ashamed about it. Many children aren't that lucky in the DRC. Many parents are ashamed of their children, and many abandon their kids (especially in poorer communities).

Think Global Health: What does public health education for SCD look like?
Leon Tshilolo: There have been efforts to introduce SCD education in schools. When a child learns what "SS Anemia" is, they can then share that information with their family. Leaflets with "Dr. SS" are published in French, Swahili, and other languages to help people learn about the disease and how to get care. However, there is ongoing stigma because people don't know what it is or how it's transmitted. Along with the cost of SCD treatment, this stigma often causes men to leave the family, with the mother then bearing the burden of caring for the children on her own. There is a large need for public health education and involvement from stakeholders in the community, particularly religious leaders.
Doña Moleka: I believe social media,TV, and radio shows remain the best [channels]… to spread awareness and reach millions of Congolese who thirst for information. Whenever I am invited to speak to a radio or TV show, tons of people call to ask questions. I, personally, learned more about SCD because of my parents who explained it to me with very simple words when I was younger, and I kept doing research about my condition and talking to my doctor about it growing up.
There is a large need for public health education and involvement from stakeholders in the community, particularly religious leaders
Think Global Health: One of the most important strategies in combating this disease is early diagnosis: ideally, newborns are screened at birth. This allows individuals with SCD to begin engaging in preventative treatment early. How do most children get diagnosed with this disease?
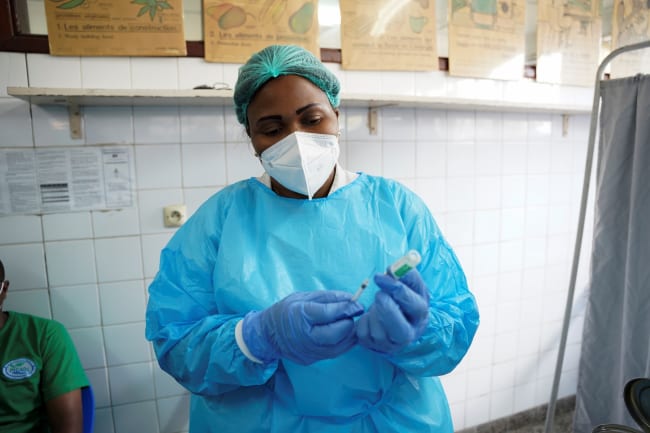
Leon Tshilolo: Most babies are not born in the hospital, so the easiest way to diagnose young children is in vaccine clinics. In rural areas, the new point-of-care tests are a great opportunity to screen newborns and young children because they don't require electricity and they're easy enough to use that [people without health-care backgrounds] can use them. However, one of the main challenges is the cost. The tests are neither easily available, nor affordable. In Kinshasa (the capital of the DRC), the cost of a single test is around $5 [nearly twice the minimum daily wage set by law]. This is a limitation for more widespread use.
Think Global Health: Cost as an obstacle to more widespread testing seems like a policy issue. What movement has been made on the policy front to recognize SCD as a public health priority?
Leon Tshilolo: It is not easy to involve policymakers in this program. The local authorities do not think of it as a priority because there is no financial support from the international organizations that usually support other health priorities in the public health domain. Even though [local health officials] know it is a problem and a health burden, they are not very involved in the programs we're trying to develop. In most sub-Saharan African countries where newborn screening programs exist, they have been implemented by NGOs in pilot studies, not rolled out in a government national program. However, countries such as Nigeria and Ghana are moving in that direction. But SCD is a neglected disease; that is why the World Health Organization moved to include SCD in the wider group of non-communicable diseases so that more funding could be directed toward addressing SCD. The recent Lancet Commission will probably contribute to more action from policymakers in different countries as well. I'm also optimistic that, [along with a] hospital database and more screening devices [point-of-care tests], we will be able to better track incident cases in the next few years.

Think Global Health: With SCD often seen as a neglected disease, advocacy plays a large role in moving the needle on this disease. As the founder of S'POIR, could you tell us a little about your advocacy work?
Doña Moleka: Yes. I have been advocating about SCD for as long as I can remember, but I took it more seriously in 2019 when I founded S'POIR, read espoir in French, which means "hope" (the S was to symbolize Sickle cell, known as anémie SS in French). Through S'POIR, our objective was to demystify sickle cell disease by increasing access to quality information about it through social marketing behavior change campaigns. I was inspired to produce a short movie/documentary called Mwana SS, il ne mourra pas demain, "The Sickle Cell Kid Won't Die Tomorrow." Through the movie, we were able to raise more than $20,000, which helped us cover the medical care of twenty children from October 2019 to December 2020. Today, S'POIR still covers the medical care of these children. Even though we rely more on personal funding, about 40 percent comes from generous people who want to contribute to the cause after hearing about us through radio or TV interviews, through word of mouth, or through our social media advocacy.
Think Global Health: With greater awareness from both the policymakers and the public, hopefully sickle cell disease will become less stigmatized and more progress will be made toward achieving the most effective methods of treatment and prevention. What do you see as the future sources of investment or promising means for scaling up SCD treatment?
Leon Tshilolo: We can't implement newborn screening or early diagnosis without proper management and incorporation of SCD into the primary health system. We also need two essential things. The first is safe blood. The average patient will need 0.5 units of blood per year, meaning that by the age of ten years, a child will need five blood transfusions. Since malaria is endemic there are not enough blood donors (people diagnosed with malaria cannot donate blood) and so most blood donation comes from family members of the patient. On top of that, in rural areas there is a lack of adequate blood screening equipment, which increases the risk of transmission of hepatitis and HIV. Second, we need affordable access to a unique drug called hydroxyurea. This drug is very good and can reduce mortality, complications such as stroke, and malaria events. However, a box of twenty pills is $10–15 in Kinshasa, which is still too expensive. Efforts to produce hydroxyurea in African regions are underway.
Think Global Health: As someone with very personal experience, how do you feel about the future of sickle cell disease?
Doña Moleka: Research-wise, it seems promising! I feel hopeful about it. We all dream of a cure that will end SCD forever and that will be accessible to everyone. I am optimistic. But I want to see more effort made on raising awareness and more funding invested in creating that awareness, especially in Africa.

EDITOR'S NOTE: The interviewers are employed by the University of Washington's Institute for Health Metrics and Evaluation (IHME). IHME collaborates with the Council on Foreign Relations on Think Global Health. All statements and views expressed in this article are solely those of the authors and not necessarily shared by their institution.