The COVID-19 pandemic has exposed how vastly underprepared countries are to address public health emergencies. It has also highlighted the need for better global health coordination and leadership. This can, and should, be achieved by supporting a stronger World Health Organization (WHO). But it also requires the WHO to change—to become a more robust, effective organization. This means that the WHO should increase its independence, its partnerships with civil society organizations, and its focus on human rights.
The 2020–21 WHO budget is just under $5 billion ($4.8 bn), a figure that compares to the budget of a large hospital
The COVID-19 pandemic illustrates the critical role that the WHO plays in issuing technical guidance on new disease threats, as well as coordinating country responses. Strong guidance and country assistance are key to building resilient health systems. But too often, the WHO lacks the core funding and support needed for its technical and programmatic work. The 2020–21 WHO budget is $4.8 billion, a figure that has been compared to the budget of a large U.S. hospital. Most of that budget is non-discretionary and earmarked for specific activities, requiring WHO to make special calls during emergencies for countries to contribute additional funds. That is a lot harder to do in the face of a global pandemic and a resulting global economic slowdown.
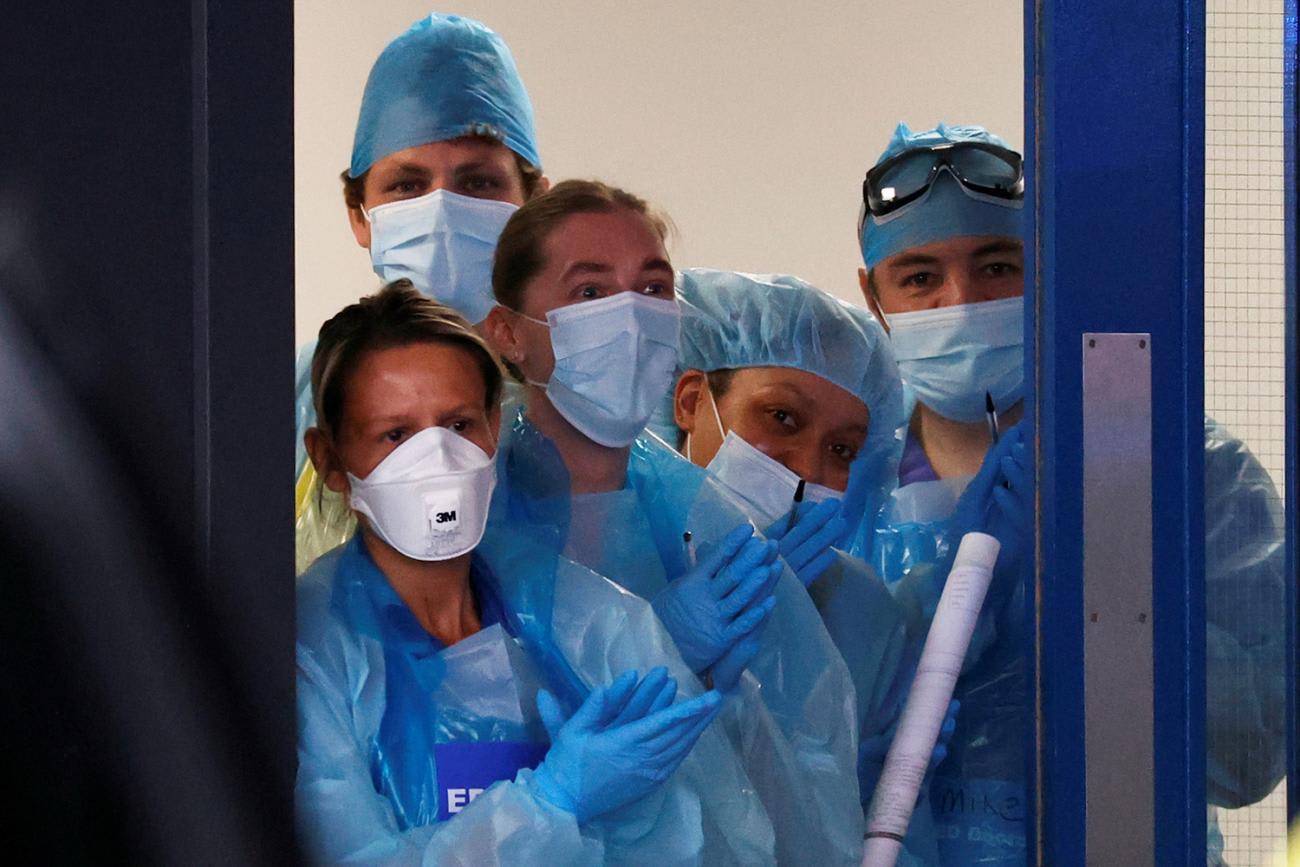
Beyond funding challenges, though, the WHO needs to become less constrained by its member states, which limit its independence and ability to speak and act forcefully to advance its mission of protecting and promoting the right to the health for all. Building stronger partnerships with independent organizations and human rights activists should be central to its new organization. The WHO should recognize the critically important role independent organizations play in identifying public health threats and exposing how governments are, or are not, effectively responding to pandemics.
The WHO needs to become less constrained by its "member states," which limit its independence and ability to speak and act forcefully
Lessons learned from the 2013–16 Ebola outbreak in West Africa demonstrate the centrality of community engagement and partnership to effective response—for example, to local traditions as basic as burial practices—and to call on local expertise for public health monitoring. Journalists and human rights organizations highlighted when quarantines were poorly implemented and how corruption undermined control efforts. Mobilizing and developing partnerships with community groups and making use of local expertise is also essential for establishing trust within communities to effectively tailor the WHO's response to a health emergency. Moreover, the work of civil society organizations strengthens technical knowledge about health issues, as has been seen with the development of HIV/AIDS programs.

Nongovernmental organizations (NGOs) can provide complementary information and insights about emerging public health issues. They do so by working closely with communities or operating outside of the political channels that can block notice of disease outbreaks. For instance, the Program for Monitoring Emerging Diseases (ProMED), a website that crowdsources information from public health and medical experts, has consistently been the first to report disease outbreaks, including Severe Acute Respiratory Syndrome (SARS), Middle East Respiratory Syndrome (MERS), and most recently, COVID-19.
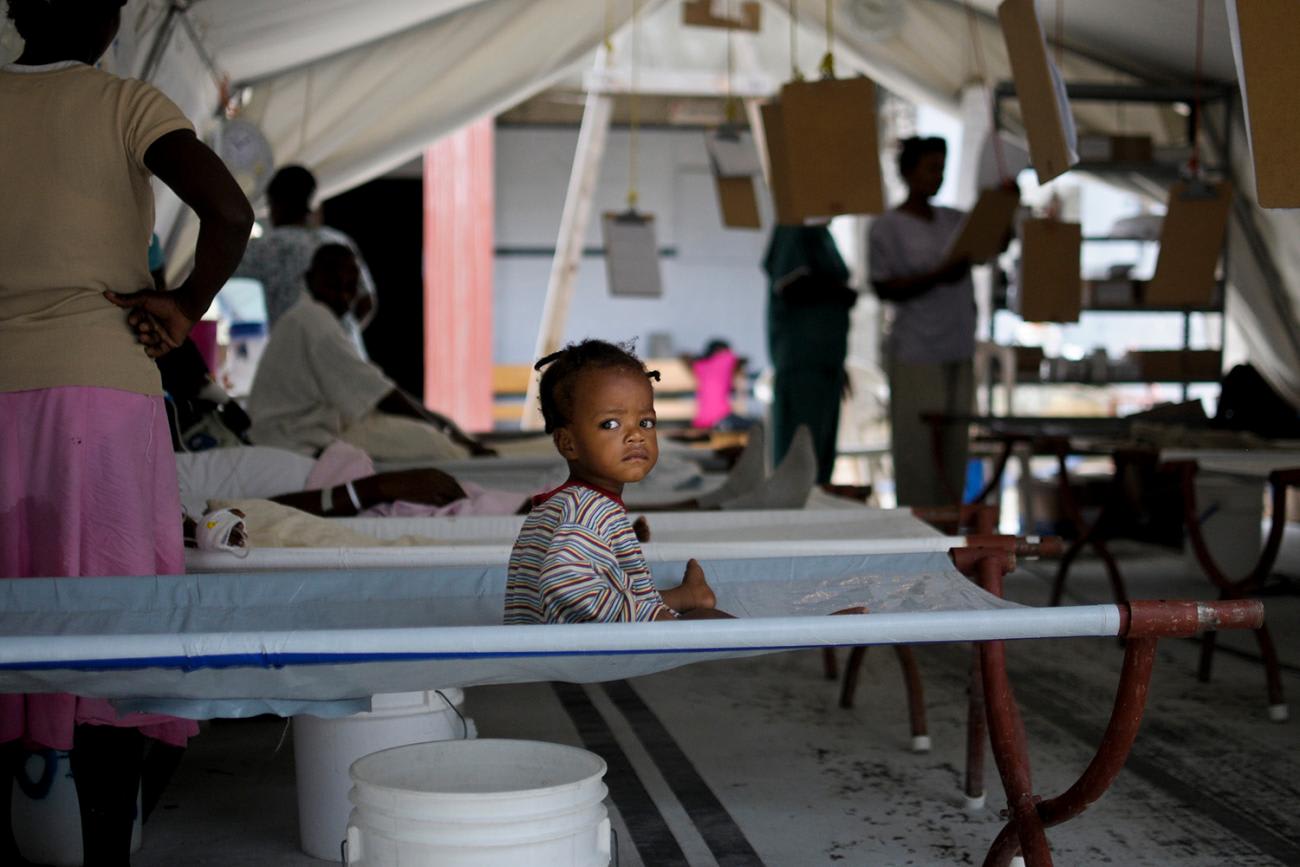
During the cholera outbreak in Haiti, the International Federation of the Red Cross and Red Crescent Societies used a community-based monitoring system to detect outbreaks in rural Haiti. This showed that not only could communities successfully conduct disease monitoring, but that this system detected disease in areas overlooked by formal surveillance.
Alongside stronger partnerships, there is an urgent need for the WHO to increase its commitment to human rights. In response to the COVID-19 pandemic, the world has seen medical professionals, scientists, and journalists silenced or censured for speaking out. It has also seen the overly broad and excessive use of laws and law enforcement practices, in alleged efforts to control the epidemic.
Religious, racial and ethnic minorities, indigenous people, and people of Asian descent have been attacked, while other groups, including people with disabilities and refugees and migrants, have often been excluded from prevention campaigns and access to care. The WHO needs to work more closely with human rights organizations to counter these predictable and counterproductive actions—and to bolster the WHO's resolve to confront governments that allow or condone them.
Ensuring the right to the highest attainable standard of health for all is protected and fulfilled
Right now, all efforts should focus on addressing the current crisis. But soon there will be discussions, and choices, about preventing future pandemics. In this new era, the global health sector needs to broaden its traditional lens of disease monitoring and technical capacity building to embrace and support a focus on human rights. Health agencies should work in close collaboration with the civil society organizations that have crucial roles in community response to an outbreak and in recovery. Pandemic preparedness requires a well-resourced WHO that is strengthened by partnerships with a broad range of organizations united to see that the WHO's mandate, ensuring the right to the highest attainable standard of health for all, is protected and fulfilled.












