The uneven rollout of the largest worldwide vaccination campaign in history was "a global failure to address populations in need," says Ali Mokdad, Institute for Health Metrics and Evaluation (IHME) professor.
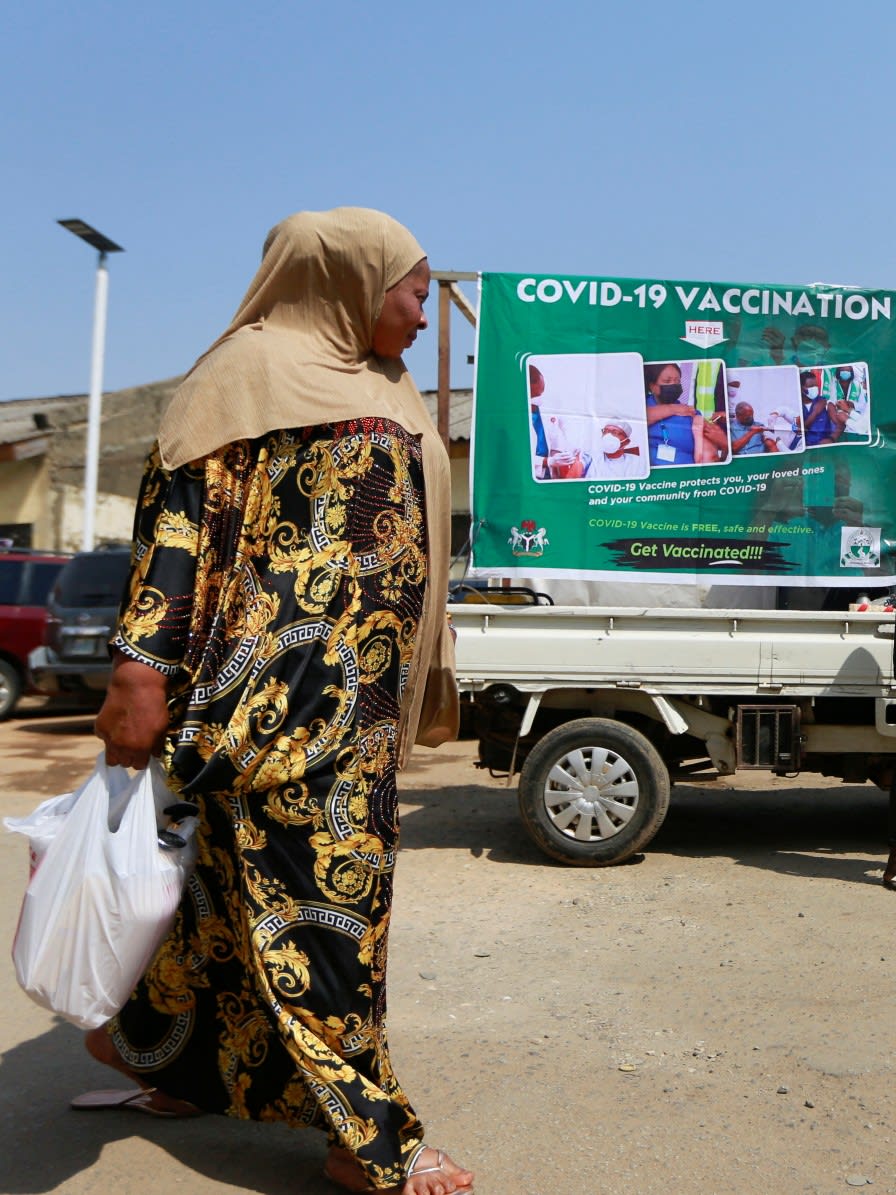
While many high-income countries have relaxed COVID-19 restrictions and eased mandates, and some have moved on to encouraging people to get their fourth booster shot, there are many others, especially in Africa, where people haven't received even their first vaccine dose.
The unmet demand for vaccination—the proportion of the population that is willing to be vaccinated against COVID-19 but has not yet received a dose—is highest on the African continent, particularly in Nigeria. Nigeria's unmet demand for vaccination is estimated to be 17.6 percent, according to recent global COVID-19 research from IHME at the University of Washington, using data from The Delphi Group at Carnegie Mellon University and University of Maryland COVID-19 Trends and Impact Surveys, in partnership with Facebook. That's over four times higher than the percentage of people worldwide (3.7 percent) who want a vaccine, but haven't yet been jabbed.
Percentage of Population That's Unvaccinated and Wants a Vaccine
Vaccine hoarding by many high-income countries—at the expense of low- and middle-income countries (LMICs)—cannot be overlooked. High-income countries stockpiled an estimated 1.2 billion surplus doses by the end of 2021, with at least a third of those vaccines going unused. Additionally, delays in the distribution of donated vaccines from the global initiative COVAX meant that Nigeria didn't receive its first batch of doses until March 2, 2021, almost three months after the world's first COVID-19 vaccine was administered to a patient. Not only were the initial doses slow to arrive, Nigeria had to destroy over a million donated doses last December due to a short shelf life that left them close to expiration.
Beyond the biggest factor of the initial shortage of vaccines, Nigeria also contends with the challenges of administering and storing vaccines, and building vaccine confidence.
Providing Access to Willing People
As of April 2022, Nigerian officials said the country had a sufficient supply of donated vaccines. The issue, in part, is where to find them. Africa CDC Director John Nkengasong recently wrote, "At the moment, Africa's most pressing need is administering the vaccines we have to willing people."
Africa's most pressing need is administering the vaccines we have to willing people
John Nkengasong, Director, Africa CDC
The federal government has endeavored to make it easier for people to obtain vaccines by introducing a vaccination site finder. But knowledge of the tool is not widespread. Babatunde Salako, the Director-General/CEO of the Nigerian Institute of Medical Research, said via email, "My experience is that people do not know most of the vaccination centers where they can be vaccinated without much ado. I have received calls from a number of my friends to ask for where they could be vaccinated."
To further overcome the challenge of delivering vaccines to people eager to receive them, Salako suggested, "Some unconventional places like marketplaces, malls, local garages, train stations, and airports should be brought on board [as vaccination centers] to make vaccines available to the people. Put it practically at their doorsteps."
Storage Solutions
Another logistical challenge in vaccine delivery is storage. Africa CDC lists AstraZeneca, Johnson & Johnson, Moderna, Pfizer/BioNTech, and Sinopharm as the vaccines in use in Nigeria. The Moderna and Pfizer/BioNTech mRNA vaccines have more delicate cold chain requirements, whereas the other three vaccines can be stored between 2 and 8 degrees Celsius.
To tackle the storage issue, the country received 175 solar direct drive refrigerators, which can keep vaccines at the 2 to 8 degree temperature range without relying on fuel or batteries. The Nigerian government procured more than three million Johnson & Johnson vaccines in recent months that will be kept in them at the required temperatures.
Percentage of Population That's Unvaccinated and Doesn't Want a Vaccine
Vaccine Confidence
While the percentage of not-yet-vaccinated people wanting to get the jab is higher in Nigeria than most of Africa, Nkengasong recently stated that people's willingness to get vaccinated is still one of the barriers to higher vaccination rates on the continent.
Olayinka Stephen Ilesanmi, a clinical epidemiologist at the University of Ibadan and a collaborator on the Global Burden of Disease Study (GBD) agreed. "The lack of willingness to get vaccinated is also linked to poor community engagement," said Ilesanmi via email. Ilesanmi concluded that influential local figures, such as teachers or religious leaders, could play a role in increasing the public's acceptance in the safety of vaccines and building trust of health authorities in general.
When vaccines finally arrived, many people had been infected by then and didn't want a vaccine anymore
Ali Mokdad, Professor, IHME
The low levels of vaccine confidence can be partially attributed to earlier vaccine shortages in Nigeria. In 2020 and 2021, as people waited for the arrival of donated vaccines from high-income countries, the delays allowed misinformation and disinformation to fester in parts of Nigeria. "When vaccines finally arrived, many people had been infected by then and didn't want a vaccine anymore," said Mokdad.
In part, some Nigerians were concerned about the safety and efficacy of donated vaccines close to expiration. However, there are encouraging reports of more Nigerians gaining confidence in vaccines after authorities committed to declining vaccines near their expiry dates.
The Next Challenge: Deploying Antivirals
IHME projects that the percentage of Nigerian people immune to the delta and omicron variants—either through prior infection or vaccination—will not top 40 percent by June 1, 2022. To take matters into its own hands, Nigeria is working to develop its own vaccine and is among six African countries selected by the World Health Organization (WHO) to establish their own mRNA COVID-19 vaccine production centers.
At this point in the pandemic, IHME director Chris Murray urges health leaders to shift focus to antivirals in order to save more lives. "We see a lot of global discourse about access to vaccination, and that's certainly an important issue in terms of equity. Everybody who wants a vaccine should certainly be able to obtain a vaccine," said Murray. "But in terms of preventing death from future new variants, we think that the scale-up of antivirals, particularly Paxlovid… is going to be the critical issue."
It is vital that the global scale-up of antivirals is equitable and does not go the way of vaccine distribution. In a recent statement, the WHO said it is "extremely concerned that—as occurred with COVID-19 vaccines—low- and middle-income countries will again be pushed to the end of the queue when it comes to accessing this treatment."
The actions of Paxlovid maker Pfizer do not bode well for Nigeria and other LMICs: Pfizer denied a request last month to supply Paxlovid to a clinical trial for ten African countries. And even in locations where there is a supply of Paxlovid, obtaining the antiviral drug is mired with complications.
The mishandling of the rollout of COVID-19 prevention and treatment interventions has led to studies of how best to prepare for the next pandemic. As McGill University professor Madhu Pai said, "The best way to tackle the next pandemic is to handle the current crisis better."

ACKNOWLEDGEMENTS: The author would like to thank Johan Månsson and Ally Walker for coordinating communication to garner quotes, Dr. Elizabeth Serieux and Catherine Bisignano for providing insights, Christopher Troeger for providing data, and Rebecca Sirull for fact-checking assistance.
EDITOR'S NOTE: The author is employed by the University of Washington's Institute for Health Metrics and Evaluation (IHME), which leads the Global Burden of Disease Study and produced some of the COVID-19 estimates described in this article. IHME collaborates with the Council on Foreign Relations on Think Global Health. All statements and views expressed in this article are solely those of the individual authors and are not necessarily shared by their institution.