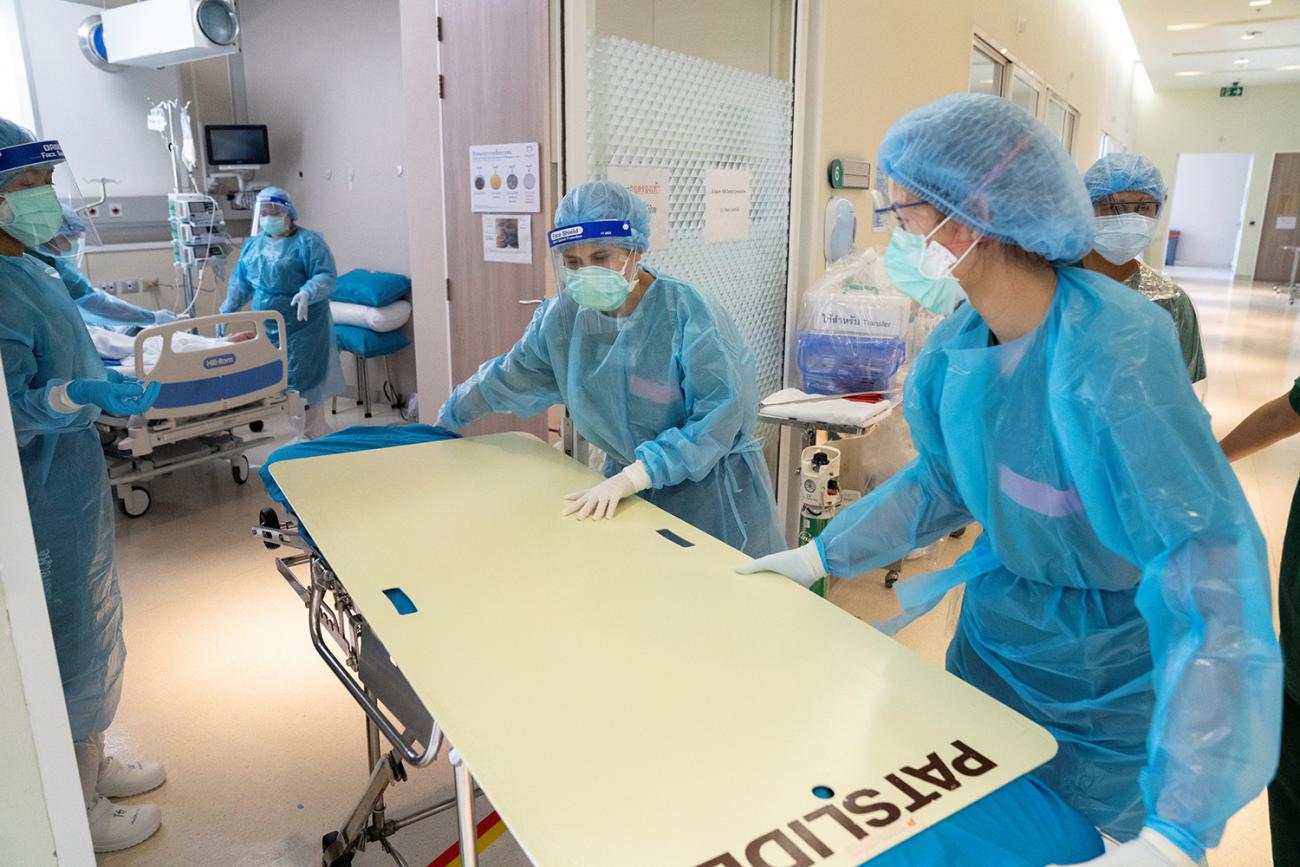
The secrets of Thailand's initial success in its fight against COVID-19 are clear, if somewhat unheralded. Despite its proximity to the Wuhan epicenter of the novel coronavirus and a large number of initial cases imported directly from China, until September 10, Thailand recorded only 3,454 cumulative cases, with a low and nearly flat trajectory of daily cases since April. One crucial success factor is Thailand's excellent public health coverage for non-Thai citizens. What health rights did non-Thais receive before COVID-19 struck, what measures were available for non-Thais during COVID-19, and what lessons can the world learn from Thailand?
What lessons can the world learn from Thailand?
Thailand achieved Universal Health Coverage for its citizens with its National Health Security Act of 2002. In principle, three public insurance schemes cover the entire population of sixty-seven million citizens: the Civil Servant Medical Benefit Scheme (~9 percent of the total population), the Social Security Scheme for private employees in the formal sector (~18 percent of the total population), and the Universal Coverage Scheme for the rest of the population. Social security is financed by payroll contributions while the universal coverage and civil servant benefit programs are financed by general taxation.

Attempting Universal Health Coverage for Migrants Since the 1990s
Health-care insurance coverage is different for non-Thais, who are mostly migrant workers and their dependants. Official numbers are approximately 3.9 million, but undocumented migrants are nearly untraceable by state authorities—partially due to the country's long and porous borders—and therefore difficult to estimate. Over 90 percent of migrants are from neighboring Cambodia, Laos, and Myanmar.
Approximately one-third of non-Thais are in the professional or highly-skilled groups covered by private insurance or social security. The remainder are mostly engaged in low-skilled jobs in the informal sector. Low-skilled non-Thais in the formal sector are enrolled in social security while those in the informal sector are covered by the Health Insurance Card Scheme for migrants, managed by the Ministry of Public Health.
The Health Insurance Card Scheme started in the early 1990s with a pilot in several Thai provinces. The Thai government gradually expanded this initiative to cover the whole country by 2004. To be insured by the scheme, undocumented migrants must undergo nationality verification to obtain a work permit. Successful applicants receive a temporary passport and visa, ratifying their legitimate stay in Thailand. Therefore, the nationality verification serves as a legalization process with the health insurance card as a form of incentive. The government began adopting this progressive stance after realizing that migrants are the main economic driver of the country.
Health Insurance Card premiums are intentionally low—365 Thai Baht ($11) for kids and 1,600 Thai Baht ($49) for adults
Since 2014, applicants must go through a one-stop service center approach, which allows collaboration between the ministries of labor, health, and interior. The process involves a health screening to detect serious communicable diseases such as active tuberculosis, syphilis, leprosy, and filariasis. The Health Insurance Card Scheme annual premium is intentionally low to attract more undocumented migrants to be formalized, only costing 365 Thai Baht ($11) for a migrant child and 1,600 Thai Baht ($49) for a migrant adult. For equity purposes, benefits in the Health Insurance Card Scheme and social security are comprehensive and reasonably close to the Universal Coverage Scheme.

The nationality verification and health insurance card program is successful, with nearly two million formerly undocumented migrants undergoing the process to date. It has also had an unanticipated boom in the last six months as the health insurance cards already issued have removed the systemic and financial barriers that may have otherwise hindered access to COVID-19 screening and care for migrants. Some hospitals in areas with high density of non-citizens also have non-Thai health volunteers to provide non-medical supportive services to help reduce cultural and language barriers preventing health-care access.
Many migrants workers are undocumented, and up to 49 percent of Thailand's migrant population remains uninsured
However, despite some existing systemic support pre-COVID-19, challenges remain especially among undocumented migrants with low-wage jobs. The International Organization for Migration estimates that three quarters of non-Thais in the country have experienced a reduction in daily income due to COVID-19 and a quarter of them cannot afford the cost of personal protective equipment (PPE). The uncertainty of border policies led to panic among migrants, leading more to use non-official crossing points and causing huge difficulties in disease screening. Many migrant workers are undocumented, and up to 49 percent of Thailand's migrant population remains uninsured. They may have limited access to COVID-19 screening due to cost barriers and the fear they will be deported, incarcerated, or face other repercussions should their undocumented status be discovered.

In addition, physical distancing measures are challenging in the cramped dormitories of migrant workers, places which often have poor overall sanitary conditions anyway. Even officially sanctioned cross-border travel is challenging, with limited space in quarantine centers in Thailand's neighbors and little information about how these centers are operated. This is all against the backdrop of stigma and discrimination against migrants.
Non-Thais Feature Prominently in COVID-19 Policymaking
Thailand was the first country outside China to report COVID-19 cases, with most infections in the early period being imported by tourists from China. After cross-border travel restrictions were imposed, the majority of non-Thai cases were workers from Myanmar. Despite that, there have been no reports of super-spreader events or clusters among non-citizen communities like what has been reported in Singapore or Malaysia.

There are several reasons why COVID-19 cases are not disproportionately concentrated in the migrant communities of Thailand. First, there is no significant difference in COVID-19 health rights between Thais and non-Thais, even those who are marginalized in the informal sector. These rights include free COVID-19 screening for suspected persons and free treatment for confirmed cases. This progressive policy allowed all residents in Thailand to be treated equally, with positive effects on the Thai health system and the concept of human rights-based care and equal protection under international law.
Strengthening the social, political, and economic determinants of health for the migrant communities of Thailand
Second, at the start of the pandemic the Thai government issued a relaxed registration policy for foreign migrants that preserved their ability to continue accessing their rights. Migrant workers with valid border passes expiring on March 31 were allowed to continue working until October 31. The Thai national cabinet also extended the deadline to renew work permits for more than 550,000 migrant workers from June 30–November 30. Third, the government collaborated with numerous civic groups to help distribute face masks and hand sanitizer to migrant communities and trained volunteers to provide information. These factors combine to strengthen the social, political, and economic determinants of health for the migrant communities of Thailand.

In neighboring Malaysia and Singapore, the conversation around migrant health during COVID-19 occasionally took a nationalistic tone. But such rhetoric was not prevalent in Thailand. There are several reasons for this. Three decades of long progress for migrants and their health rights has reduced xenophobia in Thai society. The social contract has effectively been expanded to accept the rights and duties of Thais and the non-Thai residents in their midst. Contentious discussions on "who pays" have taken place over decades instead of being concentrated during the height of the COVID-19 panic.
Important lessons for countries such as Malaysia, Singapore, Turkey, Lebanon, or Germany
These discussions have generally been resolved to the satisfaction of the Thai public because the insurance premiums are mostly paid for by the migrants themselves. The entire nationality verification process also helps bring more undocumented migrants into the official system, which increases trust, reduces crime and trafficking, and strengthens the economy and official statistics—on top of being more ethical and compliant with international laws. These are important lessons for other countries managing migrant or refugee health, such as Malaysia, Singapore, Turkey, Lebanon, or Germany.
The Political Determinants of Non-Thai Health
Despite frequent changes in Thailand's federal government since the early 2000s, this equitable, progressive and pragmatic stance on migrant health has continued. The strongest reason is the public health case that better health for non-Thais directly improves the population health of Thais. This is evident in the continuing expansion of health insurance benefits and financial risk protection for non-citizens alongside the expansion for citizens.
Strengthening migrant health, therefore, becomes an economic case as well as a public health one
There is appetite for migrant health coverage in health economics terms too. In some areas, hospitals can gain revenue from migrant insurance as migrants are younger and tend to use health-care services less frequently than the native Thais (who tend to be older). Health professionals, policymakers and leaders have consistently and effectively made this public health case for three decades, and migrant health is now considered a constant and uncontroversial feature of the health policymaking landscape. This is helped by a clear understanding that Thailand's economy benefits from better migrant health. Migrants fill labour shortages (especially in 3D jobs that are dirty, dangerous or difficult) and contribute to economic growth. A joint study by the Organization for Economic Cooperation & Development (OECD) and the International Labor Organization (ILO) estimates that migrant workers contribute up to 6.6 percent of Thailand's GDP, with a total employment share of only 4.7 percent. Strengthening migrant health, therefore, becomes an economic case as well as a public health one.

The positive effects are also seen in security and in cross-border economic terms, since migrants send up to $2.8 billion annually to the four countries neighboring Thailand, reaching as much as $10 billion if informal or low-value remittances are taken into account. Given the risk of organized crime or abuse, formalizing the remittance corridor allows the Thai government to regulate and monitor these flows. Providing health care to migrants therefore could be a small incentive for undocumented migrants to leave the shadows and enter the official system, thus indirectly helping to strengthen national security.
The world can build on this progressive and pragmatic model for migrant health
The standard arguments in favor of improving migrant health through funding national programs usually revolve around arguments of humanitarian good, the moral imperative, an ethical duty, a religious covenant, and compliance with international law. However, the public health, economic and national security angles are equally strong arguments to strengthen migrant health in any given country. They could be more compelling for the average political leader or citizen who are often making rational choices about self-interest. As the political determinants of non-citizen health are almost always domestic rather than global, there are lessons from Thailand for many countries coping with migrant health. Thailand has achieved all this despite not yet signing the International Convention on the Protection of the Rights of All Migrant Workers. Thai national progress on migrant health can be considered one of the most expansive and effective in the world and has helped Thailand avoid the worst of the COVID-19 pandemic. The world can build on this progressive and pragmatic model for migrant health.

EDITOR'S NOTE: The authors wish to make the following disclosures. Repeepong Suphanchaimat has longstanding experience evaluating many migrant health programs in Thailand since 2013, including evaluating the HICS. Titiporn Tuangratananon is currently supporting the HIC program in the monitoring and evaluation components. Piya Hanvoravongchai is a member of the Thai National Health Reform Commission, which has health coverage in Thailand as one of its core missions.