Ten years ago, Captain America and The Hangover Part II were kings of the summer movie box office, Occupy Wall Street protestors were flooding into Zuccotti Park in lower Manhattan, and UN Secretary-General Ban Ki-moon stood before the UN General Assembly, declaring that it was time to address the surge of cancers, diabetes, and other noncommunicable diseases (NCDs) globally. His words marked the opening to the first high-level meeting on NCDs, the first UN General Assembly special meeting devoted to a health issue other than HIV/AIDS.
The meeting came on the heels of a transformational decade in global health. The international response to the HIV/AIDS crisis motivated governments and philanthropists to contribute billions of dollars toward researching and developing treatments for the world's poor and creating new donor-funded institutions to deliver those treatments. Global health aid had nearly tripled over the previous decade, from $10.8 billion in 2001 to $28.2 billion in 2010. These new global health programs were making significant progress against HIV/AIDS, malaria, and other targeted infectious diseases but yielding fewer returns on challenges that required functional domestic health systems, such as NCDs and emerging infections. In his opening address to the meeting, Secretary-General Ban warned that preventing the rise of cancers, diabetes, and other NCDs was "more than a public health necessity—noncommunicable diseases are a threat to development."
"More than a public health necessity—noncommunicable diseases are a threat to development"
Ban Ki-moon, UN Secretary General
In the intervening decade, however, governments failed to address the crisis of NCDs, and the world is now paying the price in several ways. NCDs are still increasing fast among working-age populations in poor nations. These groups of chronic diseases are still the world's leading source of premature death, disease, and disability, killing an estimated fifteen million people between the ages of thirty and sixty-nine each year, with over 85 percent of those deaths occurring in low- and middle-income countries (LMICs). Even amid the devastation of the COVID-19 pandemic, ischemic heart disease, stroke, and chronic obstructive pulmonary disease (COPD)—all NCDs—represent the top three leading causes of death globally. Since 2020, COVID-19 has been the fourth leading cause of death worldwide, and evidence is mounting that NCDs have played a major contributing role in the death toll from that pandemic.
COVID-19 has exposed the unhealthy feedback loop that exists between NCDs and outbreaks of emerging infections. Here is how it works:
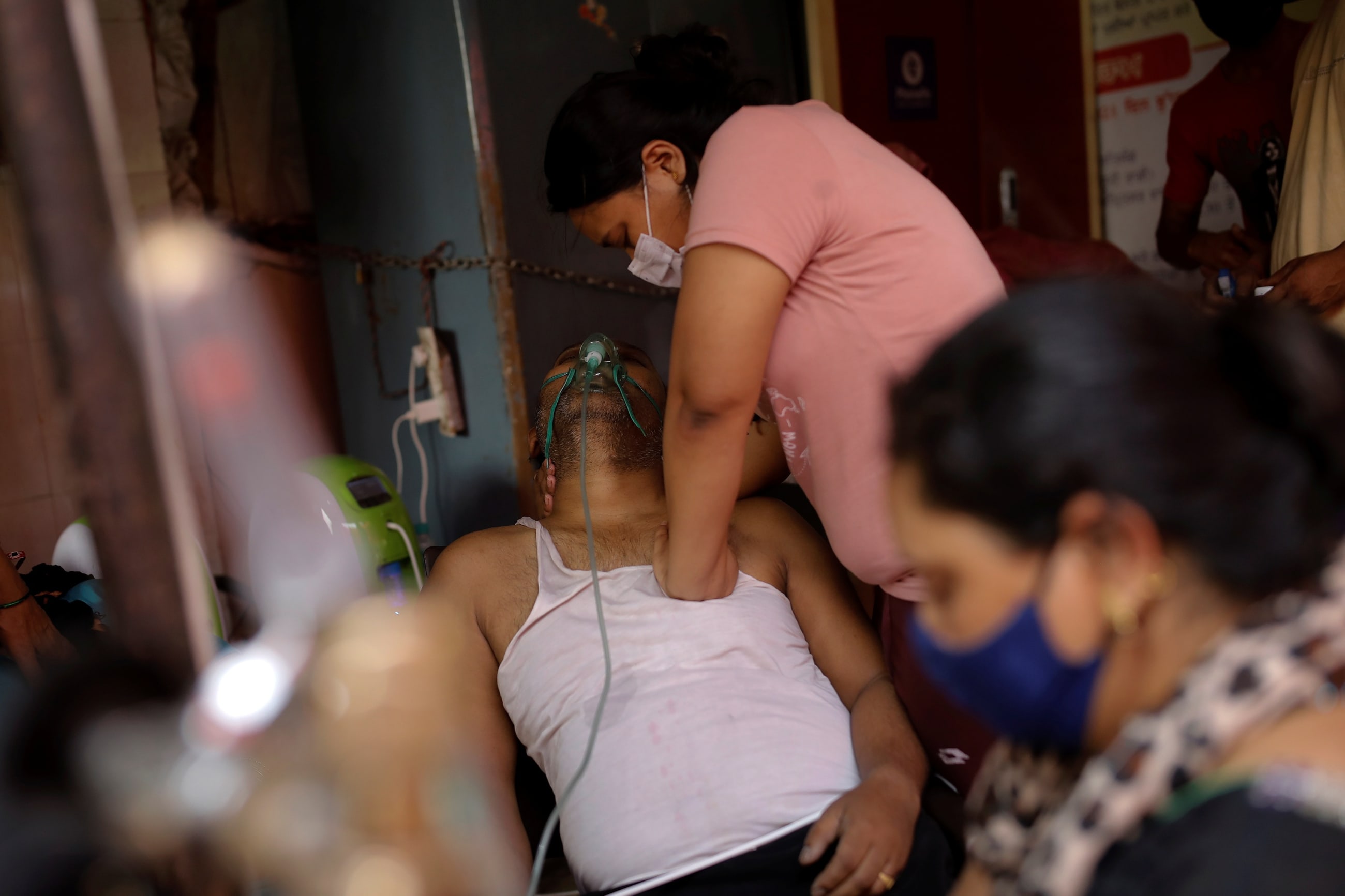
- The high prevalence of obesity, diabetes, and some other NCDs has been a major contributor to outsized death tolls from COVID-19, particularly in the United States, Europe, and Latin America.
- The need to respond to the immense toll from this pandemic and its economic consequences is shifting international aid and, some experts suspect, domestic health spending away from NCDs and health systems. Simultaneously, the pandemic has interrupted NCD prevention and related services globally, which has dire implications for the future premature health burden (affecting people under age seventy) of NCDs.
- Increases in NCD prevalence—diabetes and obesity in particular—are likely to make people less healthy and less prepared for future pandemics of flu and other emerging infections.
Accordingly, the combination of NCDs, existing social and economic inequalities, and the COVID-19 pandemic has been labeled a perfect storm.

The Role of NCDs in the COVID-19 Pandemic
The prevalence of NCDs generally—and obesity, hypertension, cardiovascular disease, and diabetes in particular—has had profound implications for how countries have fared in the pandemic. Unlike general health burdens, higher NCD burdens—or high numbers of death and disability from NCDs, as measured in disability-adjusted life years or DALYs—have also corresponded in certain countries with higher rates of death per capita from COVID-19. That trend becomes even stronger for specific NCDs, such as obesity.
This finding is consistent with evidence from the United States, China, and Italy [PDF], which has shown that older individuals and those with underlying health conditions display a consistently higher risk of severe COVID-19. One modeling study estimated that around one in five individuals globally could be at increased risk of severe COVID-19 if infected, mostly as a result of underlying NCDs.
Obesity poses an especially significant problem. In 2017, the Organization for Economic Cooperation and Development estimated [PDF] that more than one-third of people aged fifteen or older in the United States and Mexico are obese, while similar estimates found obesity rates were higher than 20 percent in Brazil, Chile, Colombia, Costa Rica, Hungary, and South Africa. Some studies have pointed to obesity, particularly morbid obesity, as a strong determinant of severe COVID-19 infection, while others have found that preexisting conditions due to NCDs, such as obesity, diabetes, and hypertension, contribute to increased risk of hospitalization, intubation, and death due to COVID-19.
75 percent of countries reported significant disruptions to NCD services after the onset of the COVID-19 pandemic
Of equal concern are the extreme disruptions to global health service deliveries, particularly those related to NCDs, as a consequence of the COVID-19 pandemic. These disruptions not only place people at greater risk of becoming severely ill with COVID-19, but also pose a significant problem for those needing regular care for an underlying condition. A 2020 rapid assessment of NCD services conducted by the World Health Organization found [PDF] that 75 percent of countries reported significant disruptions to NCD services after the onset of the pandemic. Although the underlying causes for existing disruptions varied considerably, low- and lower-middle–income countries were more likely to report disruptions in health services. The same survey revealed that 94 percent of respondent countries reported reassigning health ministry staff from NCDs to COVID-19–related roles. Further, hypertension and diabetes treatments were disrupted in half of all countries, cancer treatment in 42 percent, and cardiovascular emergency treatment in one-third. The effects of those service disruptions are far-reaching and still not fully understood, but they are undoubtedly contributing to both direct mortality from COVID-19, excess mortality from lack of services, and the global burden of NCDs into the next decade.
The COVID-19 Pandemic Is Reducing Funding for NCDs
In the decade since the 2011 high-level meeting, NCDs have consistently remained one of the smallest focal areas of global health funding, never surpassing 2.1 percent of all development assistance for health (DAH) and only reaching that level in 2019 (see Figure 1 below). Yet, international aid for NCDs from the world's major NCD donors has at least grown in absolute terms, increasing alongside funding for global health generally and nearly doubling from $496 million in 2011 to $887 million in 2020.
The pandemic has reversed that trend. Despite clear evidence that NCDs have been a major driver of cross-country differences in mortality and hospitalization rates suffered during the COVID-19 pandemic, funding for NCDs as a share of foreign aid for health declined in 2020. Worse, little momentum exists behind increasing global aid to strengthen or expand NCD prevention or treatment, either as part of the response to this pandemic or to prepare for future pandemic threats.
In contrast, there is little evidence that universal health coverage (UHC), performance on the Joint External Evaluation (JEE), and other metrics of pandemic preparedness explain the cross-country differences in how countries have performed in the COVID-19 crisis. Yet, the recent Group of Seven (G7) leaders' statement, the G7 health declaration, and the U.S. Senate's [PDF] International Pandemic Preparedness and COVID-19 Response Act of 2021 have all called for increased funding and programming for UHC and JEE to advance future pandemic preparedness.
The chronic underfunding of NCDs, in tandem with recent funding shifts to other health areas and lower utilization of NCD health services, threatens to significantly worsen the global burden of NCDs. Due in part to the COVID-19 pandemic, most if not all of the world's regions are not on track to meet the 25 percent reduction in premature mortality target [PDF] set by the 2011 high-level NCD meeting. Continued disruptions to NCD services will only worsen the toll of NCDs globally, especially in low- and middle-income countries. Several studies have pointed to a vicious loop between poverty and NCDs, in which low socioeconomic status leads to chronic ill health over the lifespan, and NCD burdens in turn reduce the income status of households.
Future Pandemic Threats
Previous research has found that NCDs have exacerbated health outcomes from other pandemic threats beyond COVID-19. Annually, the U.S. Centers for Disease Control and Prevention (CDC) warns that adults with chronic health conditions such as asthma, heart disease, stroke, diabetes, liver disorders, lung diseases such as COPD, and kidney disease are at higher risk of serious flu complications, hospitalization, and death. Additionally, researchers have found that risk of death from influenza for the U.S. population living with cancer is four times higher than the general population, while risk of hospitalization can be up to ten times higher. NCD risk factors, such as obesity and smoking, have also been linked to more severe influenza outcomes and higher risk of infection among adults.
From September 2012 to January 2016, diabetes and hypertension were present in 50 percent of severe MERS cases
Beyond influenza, NCDs are major risk factors for mortality and adverse outcomes from other viruses. For instance, chronic disorders are a major driver of severe infection from the coronaviruses that cause Middle East respiratory syndrome (MERS) and severe acute respiratory syndrome (SARS). One study found that from September 2012 to January 2016, diabetes and hypertension were present in 50 percent of severe MERS cases, while cardiac diseases and obesity were present in 30 and 16 percent, respectively. Similarly, during the 2003–2004 SARS outbreak, diabetes and cardiac disease were both found to significantly increase risk of death for patients in Hong Kong, while prevalence of underlying disease was a crucial predictor of mortality in one Taiwanese hospital. Another study found that in India, diabetes increased the risk of pulmonary tuberculosis (TB) and infectious tuberculosis by 14.8 percent and 20.2 percent, respectively, with other studies also finding similar values of increased TB infection risk from diabetes.
Conversely, other researchers have found that robust health infrastructure to prevent and treat NCDs can increase resiliency against infectious diseases. In Brazil, for instance, preexisting structures designed to address general health and NCD needs acted as a first line of defense against Zika, likely facilitating identification of the epidemic and helping to reduce international spread (see table below).
In short, the prevalence of NCDs and countries' failure to address them are a consistent and major risk factor for severe infection, hospitalization, and death from pandemic threats.
The legacy of underinvestment in NCDs will continue to reverberate through the COVID-19 pandemic—but the story can be different when the next pandemic comes, as it inevitably will. Yet, a singular focus on COVID-19 and global health security generally ignores the emerging negative feedback loop of COVID-19 and NCDs. Effectively, an integrated approach to simultaneously address the COVID-19 pandemic and the global NCD burden is imperative in order to mitigate the effects of COVID-19 and prepare for the next pandemic.

ACKNOWLEDGEMENTS: The authors would like to thank Maria Teresa Alzuru, Will Merrow, Michael Bricknell, and Bayan Galal of the Council on Foreign Relations and Joseph L. Dieleman, Angela Micah, Chris Odell, Juan Solorio, Hayley N. Stutzman, and Goli Tsakalos of the Institute for Health Metrics and Evaluation (IHME) for their assistance with this interactive.
EDITOR'S NOTE: This article was originally published as an interactive on CFR.org and was updated on September 10, 2020.