"Even before you are isolated, you isolate yourself… I stayed in my own small world for 12 years, without knowing that my condition was treatable here in Kenya."
Sarah Omega was eleven years old when she lost her parents and became an orphan, and nineteen when she became pregnant through rape by a trusted religious leader. Although Sarah's pregnancy was uncomplicated, this changed when it came time to deliver her baby. Lacking money for the maternity fee at the local health facility, Sarah labored alone at home and then, eventually, at the facility, for a total of 28 hours before losing her baby.
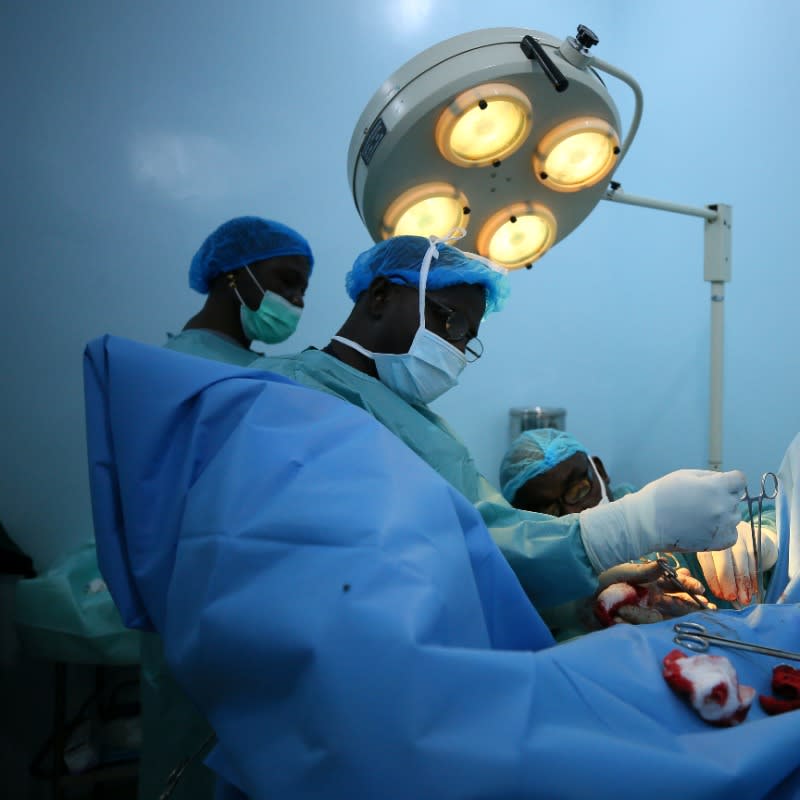
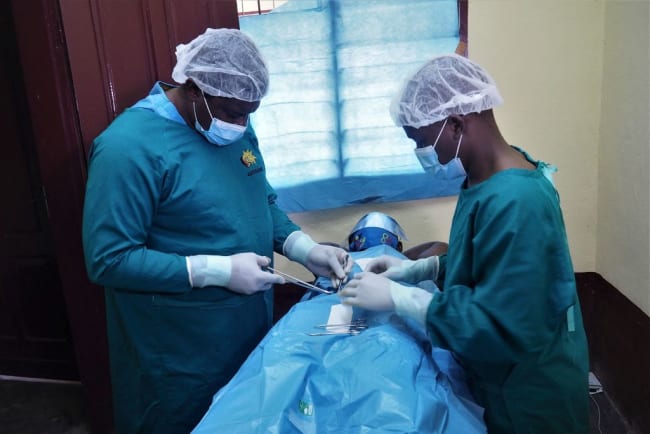
It was only the beginning of her suffering. Extended obstructed labor without the necessary surgical intervention—a Cesarean section (C-section)—and anesthesia had damaged the tissues of her pelvic organs, causing a leak from her bladder into the birth canal. This painful and stigmatizing condition is known as an obstetric fistula. Like many millions of cases of unmet surgical need, it occurs when preventive and curative operative treatment comes too late or is not available—an all too common occurrence in low- and middle-income countries. Not knowing her options for care, Sarah retreated from her relationships and from society.
In the past, global surgery has been called the "neglected stepchild of global health," as most of the attention (and funding) in global health has been dedicated to addressing deadly communicable diseases such as malaria, tuberculosis, and HIV/AIDS, as well as some noncommunicable diseases. But in recent years, interest has grown in strengthening health systems, including surgical systems, and expanding access to surgical care for the more than five billion people who live without surgical options around the world.
Advocates of global surgery have been active, from the halls of Congress in Washington, DC, to the UN's Palais des Nations in Geneva during last month's World Health Assembly (WHA) meeting, as well as in ministries around the world, making the case for investment in surgical systems. And these efforts are beginning to glean success.

Global Surgery on USAID's Radar
Global surgery was included in the recently passed U.S. Congress appropriations bill, specifically in a small, easy-to-miss paragraph in the Department of State Foreign Operations Explanatory Statement on "Neglected Surgical Conditions," buried under the "Other Global Health Issues" section. While surgery did not get top billing or any allocated funding the way other global health issues—such as malaria, HIV/AIDS, and maternal and child health—did, the bill included language calling for "efforts to strengthen surgical health capacity" and for "training local surgical teams to provide safe, sustainable, and timely surgical care, and assisting ministries of health to develop and implement national surgical, obstetric, trauma, and anesthesia plans."
This language first appeared in the appropriations bill three years ago and was expanded in subsequent years, due to efforts by the nonprofit organization Mobile Surgery International, with support from the G4 Alliance—a global surgery advocacy coalition—and the American College of Surgeons. However, this year, there is a subtle difference; Congress specifically instructs the United States Agency for International Development (USAID) to report back to the Committee no later than 90 days from the enactment of the bill "on the planned uses of funds for these purposes in fiscal year 2022."
At least 214,000 to 322,000 pregnancies worldwide are affected by spina bifida and anencephaly annually
The language does not include a funding amount, so it is unlikely new funds will be allocated toward global surgery, at least this year. However, surgery and surgical systems are increasingly recognized as a cross-cutting part of health care in general, which touches on many of the existing priorities in USAID's Bureau for Global Health and in the global health sector in general. For example, even though surgical care is a critical part of maternal and child health, and plays a key role in reducing maternal mortality—through access to C-sections and other obstetric care—and in child health, through cleft lip, palate repairs, and clubfoot surgery, none of the $940,950,000 recommended for maternal and child health in the bill are specifically allocated to surgical care. With the increasing awareness of the importance of surgical care, this should change in the near future.
It was also exciting for the global surgery community when Atul Gawande was nominated for the role of USAID's assistant administrator for Global Health. In addition to being an acclaimed author, Gawande is a surgeon and has long been a vocal advocate for global surgery. He helped lead the WHO's Surgical Safety Checklist initiative, and was a founding member of Lifebox, a non-profit group that works in more than 116 countries supporting improved anesthesia safety and helping to reduce surgical infection rates. Gawande was present at the launch of the Lancet Commission on Global Surgery in 2015. At the recent May 2022 WHA meeting, Gawande appeared on a panel on financing global surgery, at a well-attended side event organized by the Global Surgery Foundation.
Also at the WHA, the G4 Alliance joined forces with the Global Alliance for Prevention of Spina Bifida-F (GAPSBi-F) to introduce and advocate for a resolution to mandate folic acid fortification of staple foods to prevent spina bifida and anencephaly, common neural tube defects at birth. At least 214,000 to 322,000 pregnancies worldwide are affected by spina bifida and anencephaly annually. Anencephaly is fatal and open spina bifida is treatable only through skilled neurosurgical care. GAPSBi-F also published an article on May 23, 2022, in The Lancet Global Health calling for universal mandatory folic acid fortification. This initiative is a great example of scientific and surgical provider communities coming together to drive forward a public health measure that could prevent the need for surgery, allowing scarce resources to go further.

Surgical Systems Help with Pandemic Preparedness
One crucial lesson we learned from the COVID-19 pandemic is that surgical systems are essential to pandemic preparedness and response. The importance of having a safe, reliable oxygen supply, as well as a health-care workforce able to intubate was critically important during the COVID-19 pandemic. Having a strong surgical system also ensures that the health-care system as a whole is more resilient and able to withstand shocks and surges in patient volumes, as we have witnessed with each new wave of the pandemic.
In general, scaling up surgical and anesthesia capacity is a win-win for pandemic preparedness and health system strengthening. In a recent letter to The Lancet, signed by over 300 members of the global surgery and anesthesia community and 17 organizations, a call was made to mainstream surgical care into pandemic preparedness policy. It would ensure that surgical care is not treated as an optional elective function of health-care systems, but as an essential part that should be taken into consideration when planning and implementing a pandemic response.
In Kenya, there are an estimated 3,000 new cases of fistula each year
A Strong Surgical System Makes for a Strong Health System
Surgery affects nearly every part of every health system, from primary health care to tertiary cancer treatment. The trend in global health is toward a comprehensive approach to health systems strengthening, and a comprehensive health system necessarily includes surgical care. As Tedros Adhanom Ghebreyesus, the director-general of the World Health Organizations has said, "Surgical, obstetric and anesthesia care is an essential part of every health system."
This was echoed by the Hon. Ifereimi Waqainabete, minister of health and medical services for Fiji, who spoke of the need to support surgical systems during a Global Surgery Foundation event at the WHA. He said, "Surgery, obstetrics, anesthesia is at the heart of universal health coverage."
Based on the attention paid to global surgery during the WHA, as well as USAID's imminent report back to Congress on its plan to invest in surgical systems, it is clear that global surgery is on the agenda for global health and it is here to stay.
Today, Sarah Omega is the founder and executive director of the Kenya-based Let's End Fistula Initiative. Sarah was lucky to have her fistula repaired, a day she describes as a "rebirth." In response to her trauma, Sarah has dedicated her life to educating and empowering women, promoting safe motherhood, and connecting women to medical and surgical services when necessary. The need for this work is overwhelming. In Kenya alone, there are an estimated 3,000 new cases of fistula each year.
An increasing number of global health advocates, practitioners, and policymakers are recognizing that a strong health system must provide safe, affordable, and timely surgical, obstetric, trauma, and anesthesia care. For the five billion people still waiting for access to surgical care, this cannot happen soon enough.