As governments, businesses, and individuals work to contain COVID-19, we can't lose sight of the growing global threat of cardiovascular diseases.
According to the Global Burden of Disease 2019 study led by the Institute for Health Metrics and Evaluation, the burden of cardiovascular disease has risen steadily over two decades, especially in low- and middle-income countries, which have the highest age-adjusted disease burden of cardiovascular disease. And in some high-income countries, the progress made against cardiovascular disease has reversed course.
Over half of countries surveyed by the WHO reported that services for the treatment of high blood pressure were interrupted by COVID-19
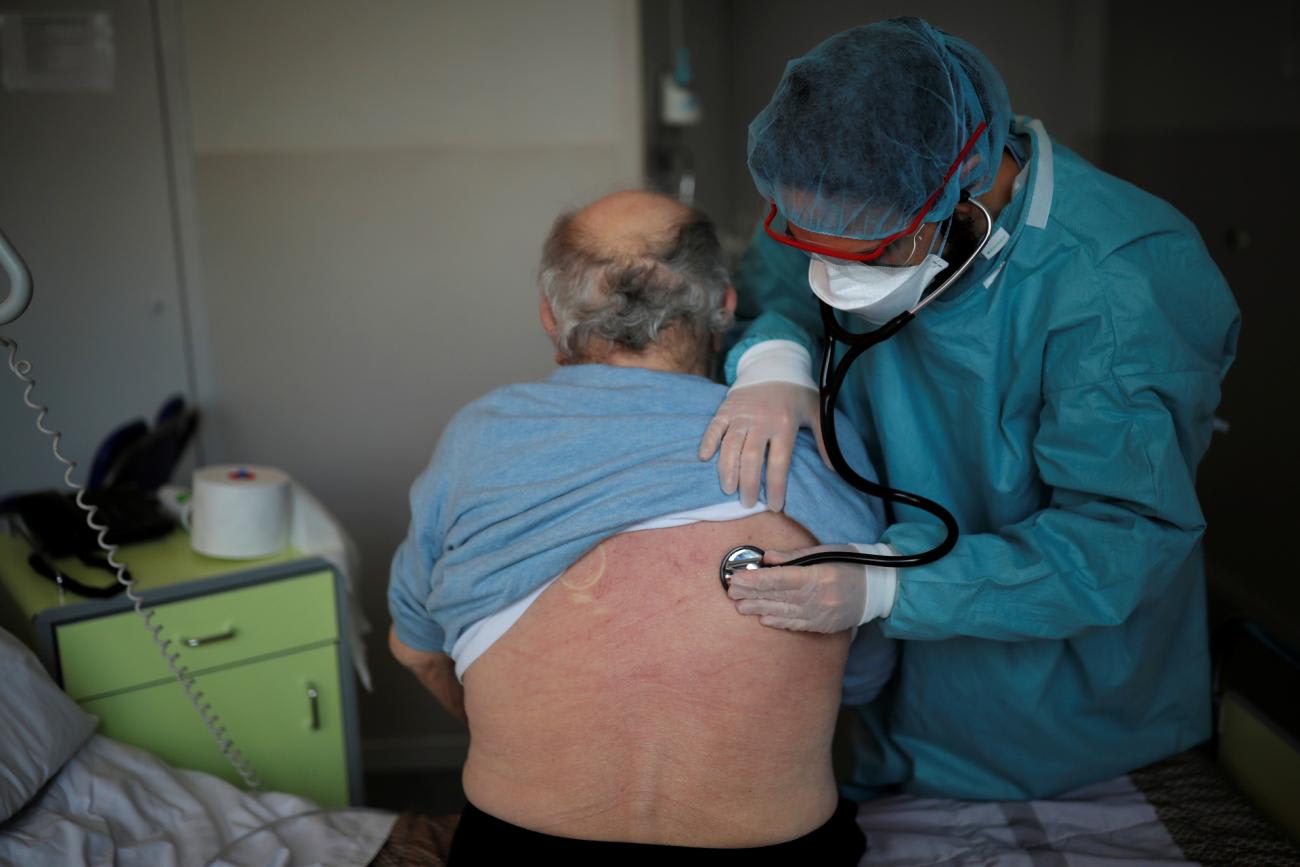
Premature cardiovascular disease is a bigger killer than COVID-19 globally, and the pandemic has likely only made it worse. A WHO survey in May 2020 found that COVID-19 had overwhelmed countries' health systems and nearly all reported partially or fully reassigning health workers to take care of COVID-19 patients who would otherwise have provided care for non-communicable diseases, including cardiovascular disease. Over half of surveyed countries reported that services for the treatment of high blood pressure were interrupted and 31 percent of countries reported that services for cardiovascular emergencies had been negatively impacted. Patients may also have missed necessary medical care out of fear of exposure to COVID-19. And cardiovascular disease appears to increase the risk of death from COVID-19, itself. In numerous countries including the United States, Brazil, and England and Wales, studies have found deaths from cardiovascular diseases rose in 2020.
Combating cardiovascular disease can make countries more resilient during future pandemics by reducing the need for services if the health system is overwhelmed.
Leading Risk Factors for Death due to Cardiovascular Disease
Priority Interventions to Lower the Burden of Cardiovascular Diseases
To reduce the burden of cardiovascular disease, people need access to quality preventive health care to address leading risk factors for cardiovascular disease— and it needn't be costly. Individuals with an elevated risk of ischemic heart disease or stroke need aspirin and a polypill, a combination of basic medications that lowers cholesterol and blood pressure. High cholesterol and elevated blood pressure are among the top three risk factors for cardiovascular disease.
Other major risk factors such as poor diets, air pollution, smoking, and high body-mass index are more complex, but there are opportunities to tackle them. Countries should make it as easy as possible for people to access healthy food such as fruit, vegetables, and whole grains, and should work to reduce the amount of added sodium, sugar, and trans fats in processed and restaurant food. It is as crucial to combat private sector opposition to regulations boosting healthy eating, as it was for anti-tobacco efforts.
It is as crucial to combat private sector opposition to regulations boosting healthy eating, as it was for anti-tobacco efforts
Regulation and enforcement have proven effective for combating air pollution, although it's vital to continue expanding access to clean energy in order to reduce household and outdoor air pollution. And the World Health Organization's Framework Convention on Tobacco Control (FCTC) has allowed progress in reducing exposure to smoking, but it has not been sufficient to reverse the upward trend in deaths linked to tobacco use. The 182 ratifying countries can further drive down smoking rates by implementing FCTC policies such as tobacco taxation, mass media education campaigns, bans on tobacco marketing and sponsorship, requiring prominent warning labels on tobacco products, requiring environments be smoke-free, and ensuring access to and delivery of tobacco cessation treatments in health-care systems.
A high body-mass index contributes to cardiovascular disease by contributing to high blood pressure, high blood sugar, and high cholesterol and by damaging the cardiovascular system. Fortunately, curriculums that promote healthy eating and physical activity, such as the Diabetes Prevention Program (DPP), a lifestyle change program established by the U.S. Congress in 2009, have been shown to reduce obesity. The DPP provides a series of courses on healthy eating, exercise, and behavior change that can be adapted to local cultures and contexts. For example, the Brazilian dietary guidelines emulate these principles, emphasizing the importance of consuming fresh food, especially plant-based foods, and minimizing intake of processed food. Promoting exercise and redesigning communities and workplaces to facilitate physical activity are also important.
Low-income countries will face the dual threat of COVID-19 and cardiovascular disease for years
The world's attention has rightly been fixated on containing COVID-19, as it continues to kill millions of people and overwhelm health systems around the globe. But all the while, cardiovascular disease has killed an even larger number of people. Low-income countries, which could have limited access to COVID-19 vaccines, will face the dual threat of COVID-19 and cardiovascular disease for years. While the global community works to ensure more equitable access to COVID-19 vaccines, it should also partner with these countries to tackle a growing burden of cardiovascular disease, address risk factors, and strengthen health systems.

EDITOR'S NOTE: The authors are employed by the University of Washington's Institute for Health Metrics and Evaluation (IHME), which leads the Global Burden of Disease study described in this article. IHME collaborates with the Council on Foreign Relations on Think Global Health. All statements and views expressed in this article are solely those of the individual authors and are not necessarily shared by their institution.












