There is overwhelming evidence that investments in strong health-care systems don’t just improve population health but also boost the economy. A healthy population has a positive return on investment impacting disparate sectors of the economy ranging from agriculture and education to tourism and transportation. Never has this been more evident than during the COVID-19 pandemic.
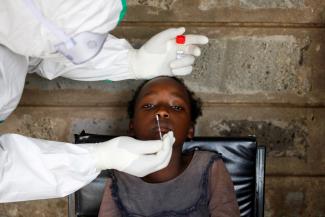
Countries with strong and well-coordinated public health systems responded quickly and effectively to the pandemic, saving lives and preventing further spread. Thankfully for many resource-limited health systems in Africa, some of the most effective interventions are low-cost public health measures such as hand-washing, promoting the use of face masks, and social distancing.
The most effective interventions are low-cost public health measures such as hand-washing, promoting the use of face masks, and social distancing
But this is only one part of the picture. Faced with a mounting toll of people infected with COVID-19 who need hospital care and other technologically intensive interventions, many African health-care systems have struggled to cope, leading to unnecessary loss of life. In Kenya, the media recently carried stories of several senior health workers and even a member of parliament who died of COVID-19 because they could not access care when they needed it. In addition, limited access to essential medical commodities reveals intractable weaknesses of procurement and supply chain systems in many countries in the region.
Despite mounting a relatively effective public health response to COVID-19, the majority of health systems in Africa lack adequate financial resources to deliver much-needed quality health care. Many are dependent on government funding, which in turn relies on a weak tax-base and is often constrained by competing public needs such as agriculture, education and infrastructural development. This has left many African health systems dependent on external donor funding, which is often unpredictable and directed at vertical health programs that might not necessarily be aligned to the region’s health and developmental priorities. As a result, many have raised questions about the sustainability of these funding models, particularly when the region is faced with increasing health-care needs occasioned by the COVID-19 pandemic, and against the backdrop of a rising epidemic of non-communicable diseases and injuries.
A region in transition
The Africa region is undergoing a socioeconomic transformation, characterized by rapid urbanization and an expanding middle class of discerning consumers with a significant level of disposable income. This long-term trajectory will likely continue unabated, even if COVID-19 has devastating economic consequences in the near term. Therefore, decision-makers must seek to cushion the pandemic’s impact on individuals and households who have lost their livelihoods and ensure they retain access to essential health-care services. Given existing resource limitations in countries, donor funding and humanitarian aid will be crucial for addressing the most immediate needs that arise from the pandemic. But in the long term, external resources alone will not be sufficient to cover the dynamic health-care needs in this region undergoing a transition.
Crisis presents an opportunity for a deeper examination of health systems in Africa
Therefore, this moment of crisis presents an opportunity for a deeper examination of health systems in Africa, shining a spotlight on opportunities as well as their fundamental challenges, like the scarcity of sustainable health financing that has effectively hamstrung many health systems. The COVID-19 pandemic should prime African health system stewards to reflect on innovative health financing models that could be leveraged to marshal domestic resources to bridge the gap and meet the priority health-care needs of their populations in both the short- and long-term.
To be effective, these efforts should be holistic, embracing a system wide approach and seeking to bring all stakeholders together with the aim of building strong and resilient health-care systems that are able to respond to future health threats.
The Challenge of Fragmented Health Services
Currently, health-care services in most parts of Africa are grossly fragmented with considerably high administrative and operational costs at the unit level. This is a common feature both in the public, non-profit, and private sector where health care is delivered. Public sector organizations, which are used by most of the population, are mainly comprised of government-run hospitals and clinics and have limited capacity to deliver high-quality services due to financial, human resource, and technological constraints. In contrast, the private sector is largely dominated by independent sole proprietors—usually a doctor or a nurse in a private office or attached to a private hospital or clinic—who provide health services within a given catchment area. In most cases due to pricing considerations, a majority of private health-care providers mostly located in urban areas fiercely compete for the small number of patients who have the means to pay for services, making their operations uneconomical and unsustainable.
Health-care services in most parts of Africa are grossly fragmented with considerably high administrative and operational costs
Furthermore, because of the fragmentation of health services, methods of practice are often not standardized, and health-care costs and patient outcomes vary enormously. Patients often undergo duplicative processes with different providers, from repetitive consultations and diagnostic tests up to multiple complex health-care interventions, which inflates costs and yields suboptimal health outcomes. This undermines the efficiency of resource allocation and utilization, and raises questions about the capacity of the existing health-care systems to make progress towards meeting the health-care needs of large sections of the population.
Fragmented health-care systems are also limited in their capacity for adopting and leveraging the novel health technologies in demand for diagnosing and treating diseases such as cancer and cardiovascular conditions that are increasingly prevalent in the region. Small health-care operations do not benefit from economies of scale in procuring and rolling out these advanced health technologies. This deprives many of their patients of the benefits of recent technological advancements, a point brought home by the limited intensive care capacity countries continue to experience in the advent of the COVID-19 pandemic.
Unlocking Pension Funds
Pension funds are a potential resource for financing health-care and strengthening health systems that few countries have fully explored. As economic activity in the region increases, pension funds have grown steadily, and asset managers are increasingly looking for investment opportunities that will realize an attractive return on investment, while safeguarding the benefits and entitlements of their members. According to a recent report by PricewaterhouseCoopers, twelve selected African countries that were managing a total of $293 billion in assets in 2008 saw that figure more than double to $634 billion in 2014, and that amount was forecasted to hit $1.1 trillion by 2020. Some countries are starting to revise their regulations to allow pension funds to invest more widely than just into domestic bonds, money market, and equities.
In most African countries, fragmentation is not only a feature at the point of service delivery, but across the entire health-care value chain, including health financing, which is characterized by small and unsustainable health insurance pools. Another major challenge facing African health-care systems is that most basic medicines, technologies, and health commodities are imported rather than locally produced. This makes health-care delivery in the region expensive and vulnerable to external shocks such as changes in foreign currency exchange rates and other trends in global supply and demand like those set off recently by the COVID-19 pandemic.
Countries managing a total of $293 billion in assets in 2008 saw that figure more than double to $634 billion in 2014
Therefore investments from pension funds could play an important and catalytic role in driving the, much needed transformation of the health-care industry in the region, with the aim of achieving universal health coverage, while also realizing an attractive return. Pension fund managers could mobilize resources at their disposal to develop integrated health-care business ventures that respond to the evolving population health needs, including in crucial domains in the health-care value chain such as financing, service delivery, medicines and commodity production, and human resource development:
Health financing: The private health insurance market in Africa could benefit from further integration into larger risk pools that are able to leverage economies of scale and purchase health services more efficiently. Enlarged risk pools will also lower administrative costs and help guide the health-care market towards greater efficiency and effectiveness. In the public sector, countries such as Kenya, Rwanda, Ghana, and South Africa are making steady progress in expanding national or social health insurance schemes, with the aim of achieving universal health coverage. By exerting competitive pressure on the private health market, this may catalyze those fragmented systems to integrate. Notwithstanding the expansion of public health insurance pools, private health insurance will still be an attractive investment considering that household income is on the rise in many countries in the region, resulting in commensurate increases in health-care expenditure.
Health service delivery and local production: Investors may also find opportunities in many countries in Africa where policies and regulations encourage public-private partnerships to bridge existing gaps in service delivery. Educating and training health-care personnel and local production of essential medicines and other health-care commodities are amenable to the public-private partnership model. Ongoing regional economic integration in Africa, which will allow for freer movement of goods and services across national borders, would make such investments particularly attractive. Other areas that are ripe for disruption include health service delivery platforms such as free-standing hospitals, clinics, laboratories and pharmacies, which could be integrated into larger and more efficient operations. Integrated health-care operations could provide holistic services, incentivizing preventive lifestyle modifications and offering a wide range of curative and rehabilitative services through standardized care protocols. Larger health-care operations could also efficiently and effectively adopt essential health technologies, using health data to catalyze innovation, optimize care and overall performance.
By improving the performance of the health system and increasing access to services, proactive investors could make a huge contribution to society
Given favorable demographic trends, socioeconomic growth, and high as-of-yet unmet needs, the health-care segment in the African region is likely to grow exponentially in the medium- to long-term. This will not only accrue as economic gains, but will also have a significant positive social impact, and could help the region leapfrog into greater prosperity. Currently, a large share of the African population lacks access to essential health services, causing untold suffering, holding back productivity, and resulting in unnecessary deaths. By improving the overall performance of the health system and increasing access to medicines and health services, proactive investors could make a huge positive contribution to society and African development in general.