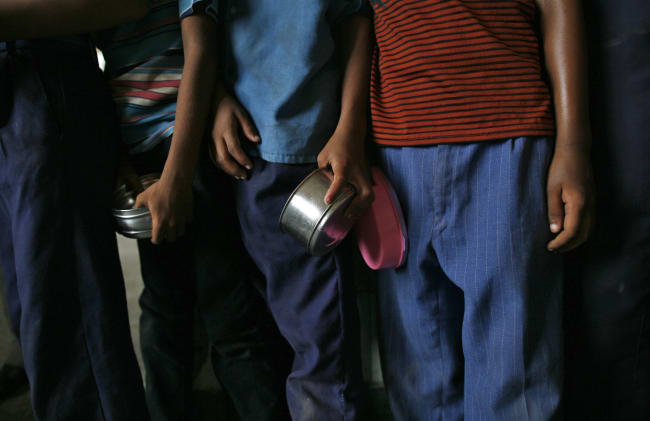Few feelings are better for a health worker than watching a child's life saved and sending her home after successfully recovering from severe acute malnutrition (SAM). Conversely, few feelings are worse than seeing them return, sometimes multiple times, for treatment of the same life-threatening condition.
Health-care workers around the world, such as those at Action Against Hunger who reach more than twenty-eight million people facing hunger across fifty-five countries annually, are dealing with a harsh reality. SAM is the deadliest form of malnutrition and occurs most commonly in young children experiencing inadequate food, unsanitary living conditions, and unclean water. It requires immediate medical and nutritional care to prevent death, address concurring illnesses, and restore necessary growth. Although most patients remain healthy after being treated for SAM, some will relapse.
Until now, however, health organizations have never known why or how often this happens.
A new study provides valuable insights that could save even more lives by helping threadbare aid budgets stretch further. Funded by the U.S. Agency for International Development Bureau for Humanitarian Assistance, it was coauthored by experts from Action Against Hunger, the U.S. Centers for Disease Control and Prevention (CDC), the London School of Hygiene and Tropical Medicine, Washington University in St. Louis, and the University of Washington.
Forty-seven million children are acutely malnourished, yet only about 25 percent have access to life-saving treatments
Researchers found that children who recover from SAM remain a vulnerable population, being up to five times as likely than their peers who did not suffer from SAM to need future intervention for malnourishment.
In some contexts, relapse can be as high as 50 percent within six months of initial recovery. Rural areas, where people have limited access to health care and other assistance programs to help children sustain their recovery, recorded relatively higher rates of relapse than areas with better access.
Globally, forty-seven million children are acutely malnourished, yet only about 25 percent have access to the life-saving treatment. Children with SAM require professional medical intervention—sometimes a hospital stay—to address the severe physiological devastation and other health issues caused by malnutrition. Therapeutic milk formulas and ready-to-use therapeutic food, such as Plumpy'Nut, can bring a child from the brink of death back to health in as little as forty-five days.
For some recovered children, however, although their lives were saved by the initial treatment, returning to a home environment defined by conditions such as unsafe drinking water, inadequate diet, and inadequate health care make it a challenge to sustain positive health outcomes in the long term without further support.

How the Study was Conducted
Researchers monitored the progress of children in Mali, Somalia, and South Sudan for six months after they completed malnutrition treatment and compared their outcomes with those of their otherwise healthy peers. Collecting that data was no easy process in such challenging contexts, and the researchers went to great lengths to ensure high-quality data.
Action Against Hunger hired a team of full-time researchers who followed up with each child to find out whether they were alive, healthy, and growing. Many of these researchers walked long distances in extreme weather conditions—including high-heat desert terrain and flooded streets—to reach families at their homes. They collected child fecal samples via rectal swabs as well as household water and food samples to identify what could be causing relapse to malnutrition.
In some settings, relapse rates were as high as 50 percent
After that, they set up small laboratories in thatch-roof huts using small, specialized equipment to prepare and preserve collected samples before they were sent to larger lab facilities overseas for full analysis.
The results were shocking. In some settings, relapse rates were as high as 50 percent, whereas in other settings they were as low as 5 percent. The dramatic range in relapse rates are due to an array of factors.
Children living in rural areas have higher rates of relapse than those in urban areas. The study found that relapse rates are 30 to 40 percentage points higher in rural areas than urban areas. Throughout the rural areas of Mali and South Sudan, for example, many children were relapsing to acute malnutrition within six months after successful recovery. In urban Mogadishu, Somalia, on the other hand, researchers observed low relapse rates (5 percent), even among internally displaced populations living in a country with near famine levels of hunger. Researchers hypothesize that access to services such as health care, cash transfers, remittances, and food distributions play a significant role in determining the longer-term well-being of children after they recover from SAM.
Children treated for SAM in the past have a higher risk of future acute malnutrition. A child is likely to relapse if they have already undergone dangerous levels of malnutrition. As many as 30 to 50 percent of children who have recovered from SAM, in rural and resource-limited settings will require treatment again for moderate or severe malnutrition. Children recovering from malnutrition were found to be extremely vulnerable and tended to be smaller, thinner, and shorter than their healthy peers.
Children who respond quickly are more likely to sustain recovery. Children who respond well and quickly to treatment for malnutrition are more likely to sustain their recovery, even if they live in households dealing with food insecurity. Those who do not respond quickly to initial treatment likely have extenuating factors, either biologically or socially, that are hindering their response to treatment.
Community and context matters. Broader community matters more to sustaining recovery than factors associated with specific individuals or households do. That insight furthers a better understanding of which contexts children will be more vulnerable in after their initial recovery. Of course, sustained recovery involves access to affordable, high-quality food. Just as important, though, relapse also seems to be significantly influenced by local availability of other services at the community level, such as access to health care and other assistance programs such as cash transfers.
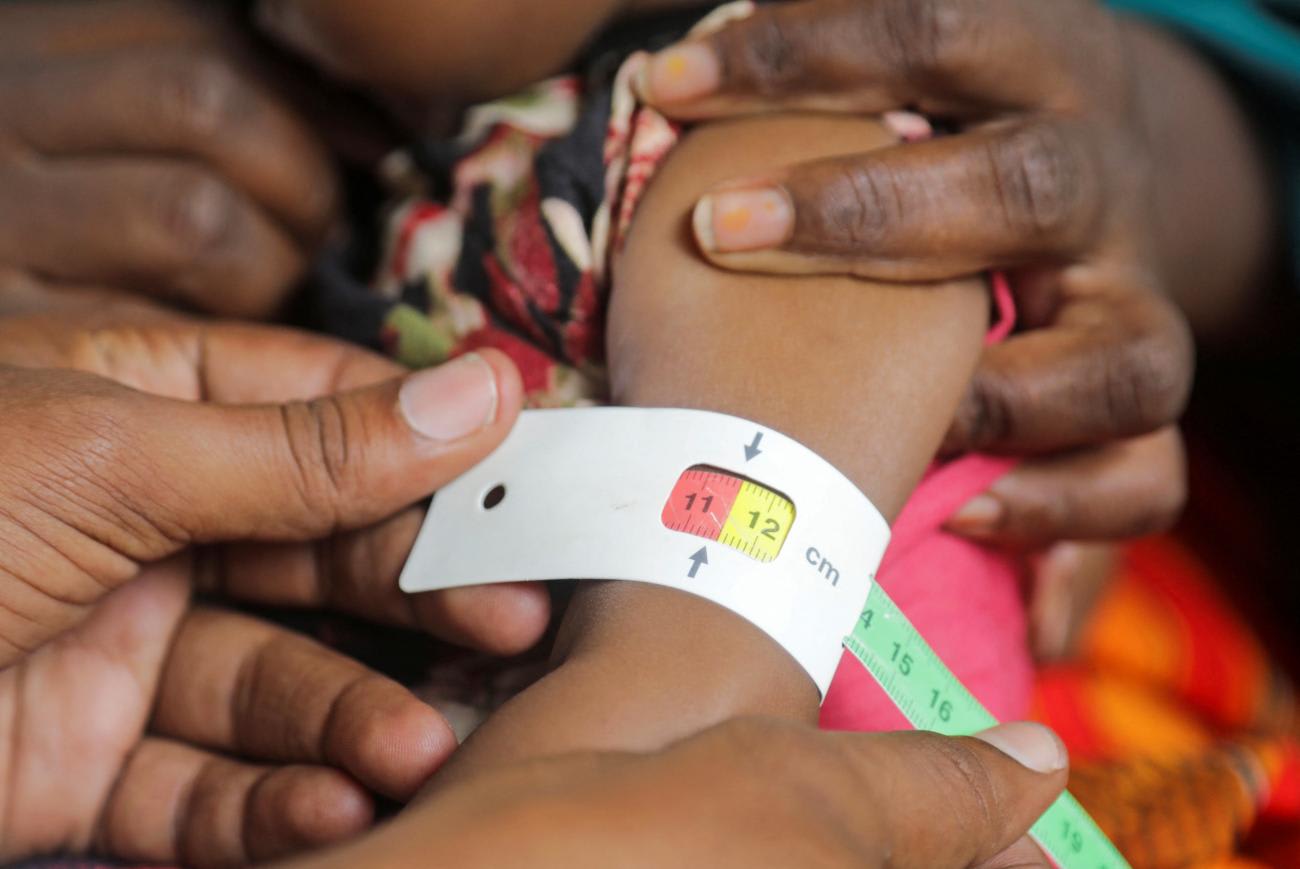
It is too early to make definitive recommendations for interventions, but this new evidence will hopefully translate into targeted solutions for certain populations that are less likely to sustain recovery. Researchers have a better understanding now that sending recovered children back to the same setting and conditions that initially caused SAM could lead them back down the same road again.
The study's findings suggest that assistance programs should go toward children who were previously severely malnourished—and that more focus should be placed on rural areas with lower access to community and social services.
Today, humanitarian and health sectors have accepted a target for a minimum of 75 percent of treated children to recover from malnutrition. They should have similar goals for a maximum proportion of children who relapse once treatment is complete.
Much is still to be discovered. As a next step, we hope to secure funding for future research that tests new approaches to ensure that children not only sustain recovery from SAM but also thrive throughout their young lives and into adulthood.