Even in the early morning, the primary care clinics at Bhumibol Adulyadej Hospital, in the northern neighborhoods of Bangkok, are already beehives of activity. Patients began queuing up before the clinics open to get care at no out-of-pocket cost, courtesy of the Thai government.
Thailand was one of the first nations in Southeast Asia to embrace universal health care (UHC), enshrining it as a right in 2002. But other nations have followed, including Indonesia in 2004 and the Philippines, most recently, in 2019. From 2010 to 2019, the 700-million person region's measure on the UHC service coverage index, a World Bank composite score that presents the coverage of essential health services on a scale of 0-100, has gone from 46 percent to 61 percent.
Despite the impressive progress made on the path toward universal health coverage, countries in the region face serious challenges in continuing to deliver health care this way. As their fertility rates plummet to or below the replacement level of 2.1 and their populations rapidly age, countries are anxiously assessing the difficulties of providing costlier services, with challenges that are both financial and structural.
As fertility rates plummet, countries are anxiously assessing the difficulties of providing costlier services
The financial challenges are rooted in the rapid growth of costs in the health-care sector. According to Solidance, a strategy consulting firm, regional health expenditures are expected to increase by $320 billion between 2017 and 2025, a 76 percent increase, which governments in the region will struggle to manage. Compounding the challenge is the need to not only maintain current services but expand them to an older and, in many cases, sicker population.
The structural cause for this growth in expenditure is the shift away from acute care to chronic care. Unlike acute ailments, chronic illnesses incur costs that can go on for years. Health-care systems that were optimized for acute illness are inefficient at dealing with chronic illnesses. And design elements of systems that benefited an impoverished region several decades ago have increasingly become liabilities.
For example, take the persistence of combined medication dispensaries and clinics across the region. This innovation was originally seen as a more efficient way to deliver outpatient services, but it has created perverse incentives for doctors who profit from overprescribing. Separating consultations from the dispensing of medicine has shown to drive measurable reduction of costs in countries that have undertaken the change, but faces regional political resistance.
Value-based care, implemented through technology platforms and primary care, is increasingly seen as the solution to these intractable issues.
Value-based health care is a health-care delivery model in which providers, including hospitals and physicians, are paid based on patient health outcomes. The shift of focus, from output to outcomes, promises to improve efficiency, so that finite resources can be stretched to meet the increased demands of UHC.
However, value-based models require two necessary elements amongst others: First, a holistic view of the overall functioning of the health system through the centralization of patient data in electronic medical records (EMRs). Second, the integration of all levels of care so that patients can get the proper care they need, whether at a hospital or a clinic or elsewhere, with an emphasis on prevention of illness (and its related cost) through the inclusion and focus on primary care services.
EMRs can help stitch together a fragmented health-care system, which can then benefit from analytical tools to identify inefficiencies quickly and precisely. A recent survey found that Asian private hospitals expect that 94 percent to be using EMRs by next year, a 50 percent increase in just five years.
Taiwan's national health insurance system, which covers 99 percent of the population, is built on the back of a unified EMR platform that is now collecting data points that are critical in assessing the clinical efficacy of treatments in real time. This data is allowing the impact of value-based outcomes to be compared between different hospitals and over time. India's Ayushman Bharat program was launched in 2018 with a health identifier, provider registry, practitioner registry and a health data standard, all of which are essential for having data in one place for analysis.
Seamlessly connecting all levels of patient care, from the primary care practitioner to the hospital, is a second element of value-based care initiatives. These models shift the metric used to make payments from how many services the health system has output to how many patients it has managed to keep healthy, thus putting a premium on prevention of illness.
A recent survey found that Asian private hospitals expect that 94 percent to be using EMRs by next year
Given their role as the first touchpoint of care for most people, primary care centers are essential in making it all work. They are staple of health system design in places like the United Kingdom, where the National Health Service uses primary care general practitioners as the gatekeeper for more advanced care. But in Asia, general practitioners and primary care have traditionally been left out of national health-care financing schemes.
This is rooted in the region's recent poverty and shifting health-care priorities. Young governments with scarce resources built health systems focused on the major health-care challenges at the time — trauma and infectious disease — which that were best handled at large, centralized hospitals. Primary care was by and large left to the private sector, which was mostly financed through out-of-pocket spending by patients.
When governments began to roll out UHC financing schemes, they focused their initial coverage on the public sector hospitals. Even private insurers have historically been resistant to cover the large, fragmented primary care sector due to the pervasiveness of fraud in medical claims, a problem that continues to this day.
These historical arguments no longer apply in a region where non-communicable diseases are a growing share of the burden, and are most effectively managed within primary care networks.
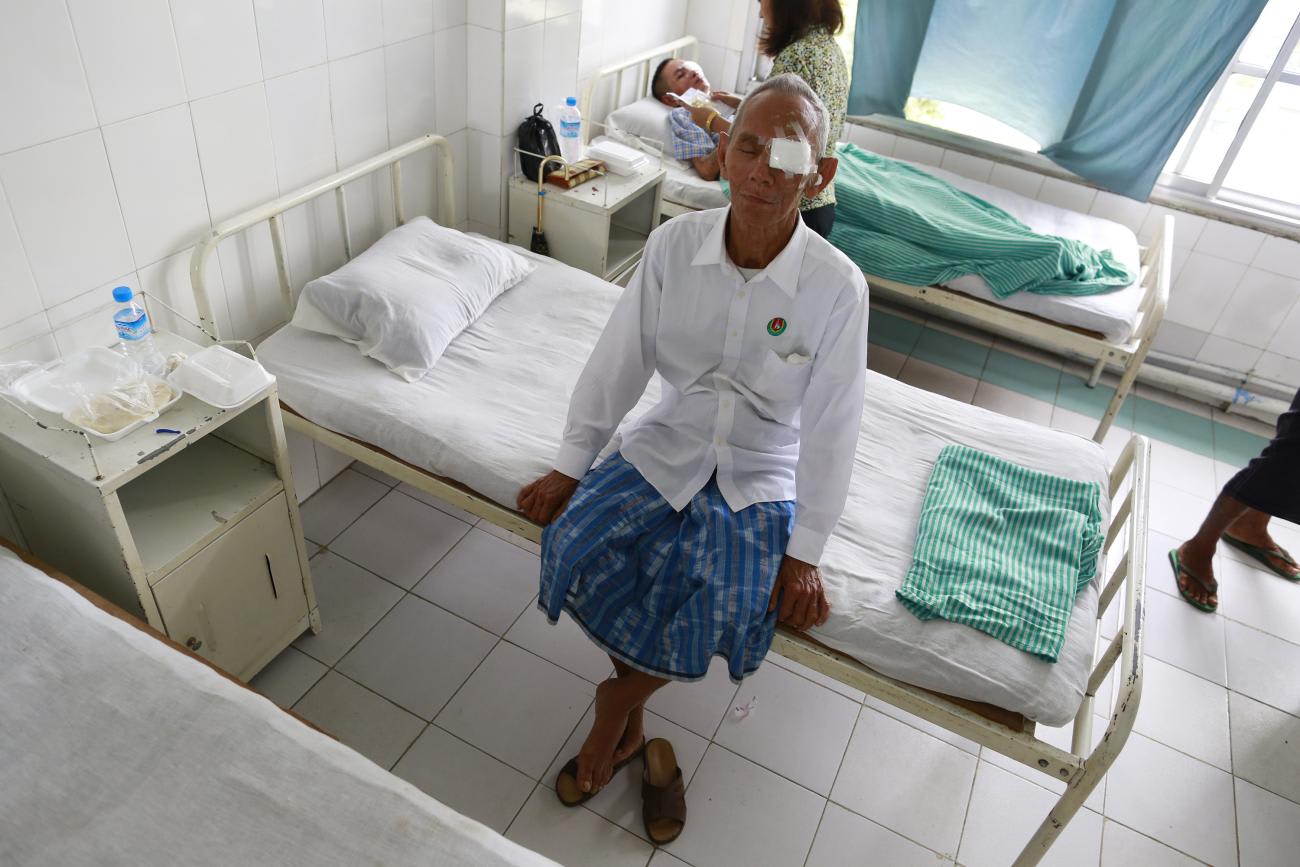
As exemplified by the busy scene outside Bangkok's clinics, governments in the region have increasingly recognized the need for these changes and are introducing new value-based care models that are making primary care the center of patient health, while using data and EMRs as a way to measure outcomes.
Singapore's most recent initiative around value-based care, the capitation-based model Healthier SG, has at its foundation the idea of a family doctor that will be the primary manager of health.
In Australia, NSW Health is enlisting clinical and nonclinical support to shift its focus from "output" to "outcomes." Its Leading Better Value Care (LBVC) initiative includes a framework to measure the patient experience and patients' perceptions of their care, health status, and clinical outcomes. The health system has thirteen focus areas for delivering value-based care; most include conditions with complex or ongoing care needs, such as diabetes or wound management.
In a region where archaic health systems are increasingly handicapped in sustainably delivering universal care, rapidly-aging populations and rising health-care costs have created a golden opportunity to retire features of the systems that have outlived their usefulness. Governments in the region are beginning to recognize the opening and replace these old models with value-based care approaches that can drive better outcomes in a sustainable fashion for the coming decades.













