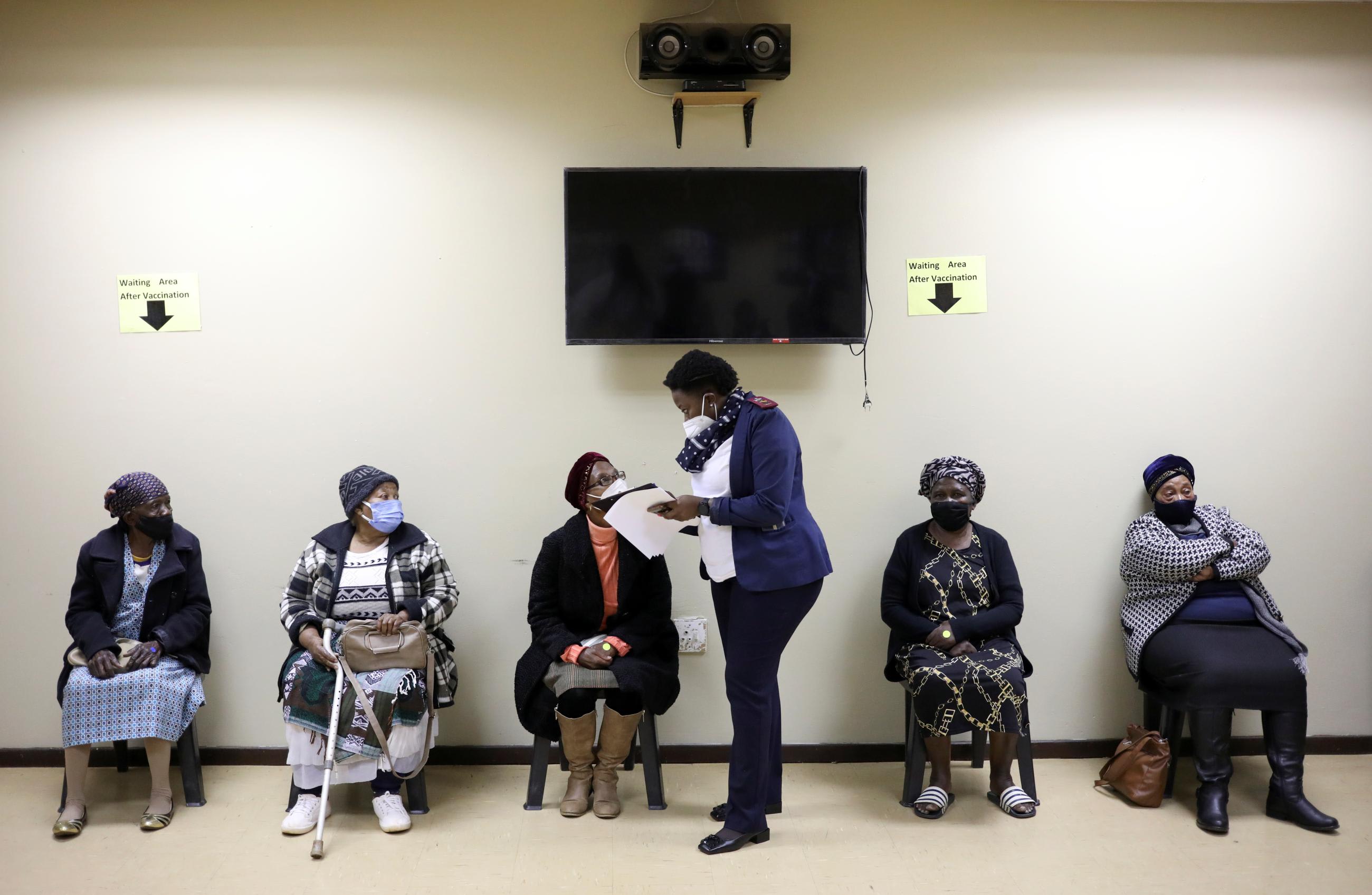
A number of countries in southern Africa are grappling with the problem of fake or unlicensed health practitioners who reportedly endanger patients' lives.
How the culprits manage to beat and infiltrate the systems is a question that various medical councils are considering—especially as the popularity of these frauds grows on social media.
The Well-Attired Intern and the TikTok Doc
In 2017, the Malawi police arrested Lloyd Chisoso, a thirty-six-year-old man who posed as a doctor at Malmed Clinic, a well-known medical facility in Blantyre, the country's commercial capital. Further investigation showed that he had applied for the same post earlier under a different name.
After the clinic's management team became suspicious about how the man was dealing with patients during orientation, they tipped off the district health office and the police. It was later revealed that he was impersonating a real—much younger—doctor by swapping a registration number and providing an authentic-looking bachelor's degree. He had merely changed the year of graduation.
More than half a decade after that high-profile caper, some of Malawi's hospitals continue to experience isolated cases of similar frauds. In 2022, the Blantyre Police detained a twenty-year-old for allegedly posing as a medical intern at Queen Elizabeth Central Hospital, one of the biggest referral hospitals in the country.
Last summer, South African authorities arrested 124 bogus doctors following a crackdown
Witnesses saw her dressed in full medical personnel attire and moving from one hospital office to another, just like any other employee, although according to the police no one actually knew her. When quizzed, the suspect claimed she was an intern doing her practical at the hospital. That proved to be false as well.
In late October, police in South Africa arrested a TikTok star named Matthew Lani and accused him of fraud after he claimed to be a medical doctor. He was arrested as he was trying to enter Helen Joseph Hospital in Johannesburg, the BBC reported.
Lani had gained thousands of followers by sharing medical advice and selling medication online. Gauteng Province's Department of Health released a statement saying that he frequently used the hospital where he was caught to "curate misleading content under the pretense that he was a qualified doctor."
A police statement shows that Lani's claims to have received a medical degree from the University of Witwatersrand in Johannesburg were false, and the BBC reported he did not even have a school diploma.

Strained Economics
This recent scandal in Johannesburg is not an isolated incident. Last summer, South African authorities arrested 124 bogus doctors following a crackdown by the country's Ministry of Health and the Health Professions Council of South Africa. South Africa's Minister of Health Joe Phaahla told IOL that unregistered doctors evade the system by joining the private sector, where they can be paid in cash or operate in practices of registered doctors.
In Malawi, dozens of people posing as nurses or doctors who have demanded money from patients in public hospitals, have been arrested in the last few years, and are now serving varying sentences. Those arrests demonstrate health authorities' efforts to crack down on fake medics and increase residents' awareness of the issue.
The rise of fake doctors, however, points to a bigger problem in southern Africa: a lack of job opportunities.
The rise of fake doctors, however, points to a bigger problem in southern Africa: a lack of job opportunities
Some of the people posing as medics reportedly attended medical schools but are yet to be employed, have not gone through regulatory examinations, or are employed under false credentials. Victor Mithi, the president of the Association of Medical Doctors in Malawi, tells Think Global Health that in some scenarios people come to the hospital and engage with patients as medical doctors.
"[A] number of people have been arrested, and patients have fallen victims where they receive prescriptions or the fake doctors ask money from them. The problem is [that] some health-care workers don't have IDs or identification materials—so much so that it becomes easier for someone to chirp in [and pretend like they are workers]," he says.
"There is also a lot of turnover of health-care workers because you have different cadres coming and going from different learning institutions. This creates a situation because it becomes difficult for the employees to identify bogus personnel by just looking at them," he adds.

The Way Forward
Several solutions, including encouraging institutions to have their workers put on uniforms with a logo and name, have been proposed, according to Mithi. Hospital regulators are also encouraging workers to be watchful.
"Our mandate is that nurses may raise an alarm if a doctor writes something they don't understand or suspicious. We've also encouraged awareness to patients and the public to know that services in public hospitals are free unless outsourced, and that payment is not made directly to the doctor," he says.
The way the frauds try to beat safeguards is by carefully studying the hospital system and environment, Mithi explains. They even befriend some of the legitimate workers so as not to raise an alarm.
The way the frauds try to beat safeguards is by carefully studying the hospital system and environment
Victor Mithi
"We've observed that many people who do this are quite smart and have a detailed understanding of how the system works," he says. "Some of them may have failed their career attempts, but most people just study how the hospitals operate and they demand money from patients."
Health rights activist Maziko Matemba says that having unlicensed medical practitioners is an issue that cannot be condoned by any country, let alone Malawi. The medical council of Malawi, he notes, has a mandate to regulate the industry.
"As far as we're concerned the council has done a good job," Matemba says. "The most important is to make sure that we support the medical council of Malawi by strengthening its surveillance but also its capacity to be able to monitor."