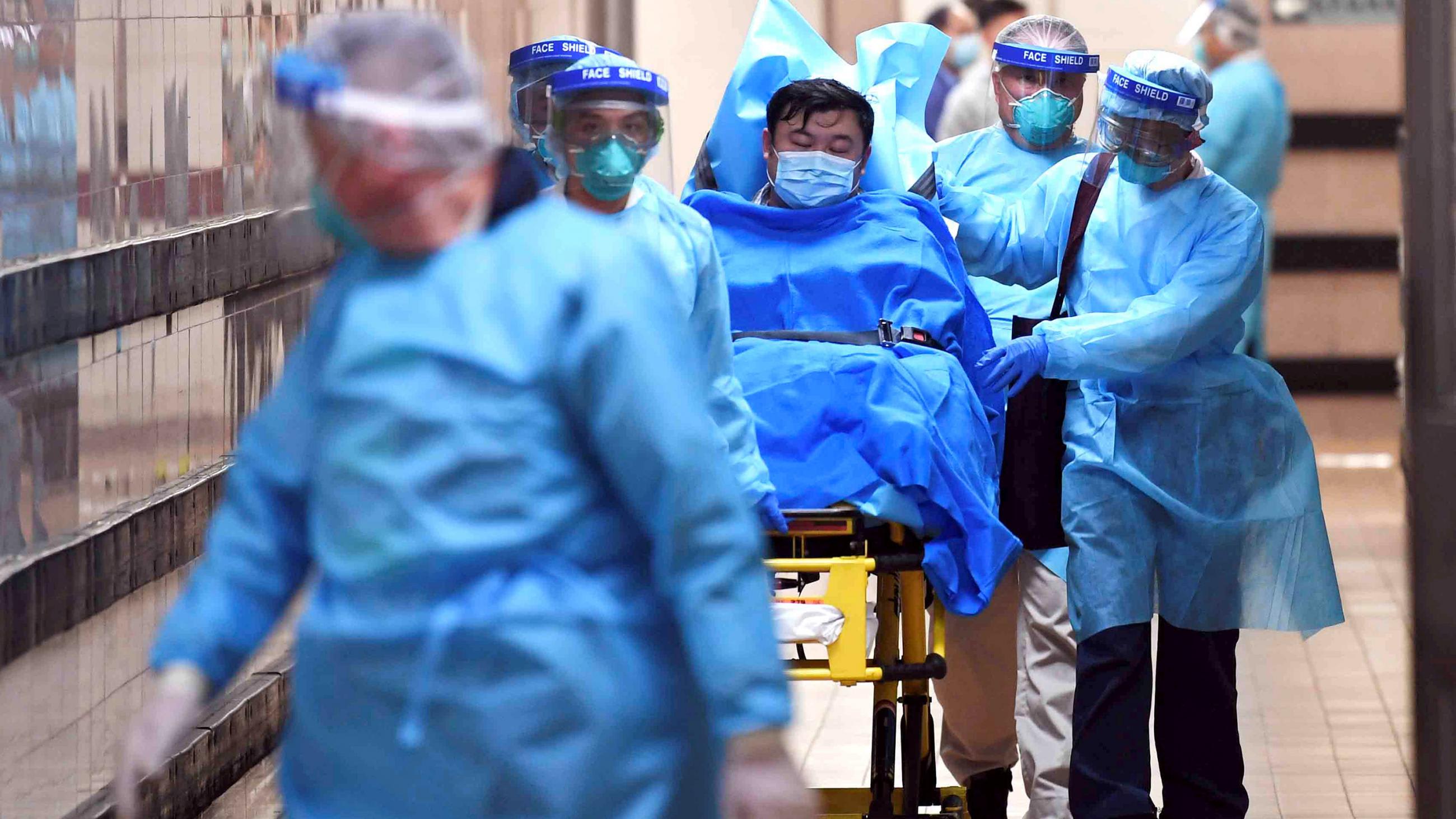
At this point, the story is evolving faster than the virus. As the Wuhan novel coronavirus outbreak continues to spread globally, human-to-human spread is now confirmed, a city of 11 million people is now quarantined, and the mass movements of East Asia's Spring Festival could soon worsen the situation. The vocabulary could also change as fast as the virus spreads and facts emerge, from outbreak to epidemic, pandemic or possibly even to the World Health Organization's (WHO) public health emergency of international concern (PHEIC).
This essay takes a longer view by focusing on the timeless aspects of the Wuhan outbreak. Why are outbreaks increasingly common in Asia, and what political choices can national governments make in emergency and non-emergency periods to reduce the risk of infectious diseases?
Perfect Storms Continue Coalescing
Some context could help us to find an appropriate level of concern. The "grandfather" of all outbreaks could be the Spanish flu of 1918, infecting approximately 500 million people and causing 50 million deaths. Since then, there have been three global flu pandemics; two of them originated in East Asia in 1957 and 1968, which caused approximately a million deaths each.

Vaccines, antivirals, better hospital care and stronger outbreak responses have significantly reduced mortality rates. In 2003, Asia overcame the SARS epidemic (also a coronavirus) with "only" hundreds of deaths. In 2009, the H1N1 flu pandemic caused approximately 19,000 laboratory-confirmed deaths globally. These deaths are all regrettable. However, public concern and breathless media reporting on outbreaks, including the regrettable tendency to call the new virus "mysterious," could contribute to an existing sense of public panic. The attention may also have consequences for other infectious diseases like dengue, malaria, tuberculosis, and hepatitis B, which could become relegated to the status of "invisible background diseases."
Outbreaks are increasingly common in Asia, but why? The first group of reasons are simply population dynamics and urbanization. There are more humans today than ever before, and they live in increasingly urbanized settings in much closer proximity to each other. Sprawling cities could encroach on farm or previously virgin areas filled with vectors and animals, domesticated or wild, with trade or consumption of exotic wildlife increasing the risk of diseases emerging. We travel much further, faster, easier and more often than ever before, for work, tourism, or migration.
We travel much further, faster, easier and more often than ever before, for work, tourism, or migration
A second group of reasons are environmental or systemic. Anthropogenic climate change and environmental degradation (e.g. desertification) has led to the spread and tropicalization of disease globally. Disinformation and vaccine hesitancy on social media "go viral" faster than actual viruses, eroding trust in science, surveillance and systems. Diabetes and old age compromise the immune system, and Asia has 60 percent of the world's diabetes burden and is rapidly aging. Health systems struggle to fight the dual burden of communicable and non-communicable disease. Bioterrorism and anti-microbial resistance add complexity.
There is another reason why outbreaks can seem increasingly common: cognitive biases and the media. Humans evolved to focus on rare events, because noticing unfamiliar surroundings confers a survival advantage. The media sensationalizes outbreaks, often leading to irrational panic. A prime example of this combustible mix is our fear of plane crashes, despite planes being much safer than cars. With so much public attention on the Wuhan coronavirus, could finite resources be diverted away from other diseases like tuberculosis, which killed 1.5 million people in 2018 alone?
Transparent, Scientific, and Fair Responses During Emergencies
It's clear that outbreaks are costly in human and economic terms. They are also an unusually challenging form of a tragedy of the commons. The commons implies good population health, and the tragedy is that individual citizens harm the commons with irrational panic, profiteering or hoarding, or rumour-spreading in a low-trust, high-risk environment. Our herd instinct is magnified by existential fear, leading to a pivotal role for governments to break vicious cycles. What political choices can they make during crises?

First, transparency is crucial. We must be sensible but not over-react, with governments setting the tone for appropriate levels of public concern. Transparency starts inside the government, with bidirectional lines of communication and aligned strategy between federal, provincial and district governments and no information being suppressed anywhere in that hierarchy. With the public, governments must err on the side of transparency by disseminating useful information on multiple communication channels. They must be clear about exactly what we do and do not know. In the absence of facts and trust, rumors and panic may be inevitable.
Viruses have no passports, and multilateral collaboration is necessary to contain their spread.
Transparency could be challenging for paternalistic Asian governments, especially those that rely on output legitimacy (e.g. legitimacy from delivering effective public services) more than input legitimacy (e.g. legitimacy from elections). Governments will be tested by high-pressure and high-stakes outbreaks, and any mismanagement could carry political cost as their legitimacy and competence are called into question. In the Chinese civilization, rulers receive divine authority known as the Mandate of Heaven. Disasters such as outbreaks or earthquakes signify the loss of divine authority; this could be a partial explanation for the seeming reluctance of the Chinese government to be transparent about failures or mistakes.
This transparency and information exchange must also be between governments, facilitated by a neutral broker such as the World Health Organization (WHO). Viruses have no passports, and multilateral collaboration is necessary to contain their spread. However, there could be a psychological barrier to sharing information as governments might perceive bad news as a sign of (geopolitical) weakness. This is wrong; transparency is the mark of the strong, not the weak.
Second, scientists must have equal stature with politicians and bureaucrats. Governments, especially authoritarian ones in hierarchical Asian societies, must feel confident enough in themselves to trust the scientists, their science, and the outbreak response protocols. In emergencies, governments cannot arbitrarily decide on outbreak responses or citizens' freedom of movement based on the whims of politicians and bureaucrats. Compounding this is the lack of transparency around the criteria for quarantine decisions.

Public health physicians, epidemiologists and infectious diseases specialists must be consulted as equal partners in decisions. Front-line staff must be empowered to tell the truth to their superiors, and this is doubly important due to their occupational risks. Organizationally speaking, there should be only one emergency operations center that coordinates the entire outbreak response, including the private and non-government sectors. For outbreak responses to be truly effective, scientists must have equal stature and shared decision-making.
Governments must ensure adequate and diversified supplies, fair and equal distribution, and clamp down on profiteering.
Third, governments must ensure that society and the health system remain equitable during emergencies. Face masks, vaccines, medicines, hospital beds, or a doctor's attention quickly run out. Governments must ensure adequate and diversified supplies, fair and equal distribution, and clamp down on profiteering. As the rich and urbanized will have more purchasing or networking power to obtain treatment compared to the poor and rural, governments must ensure fair access across socioeconomic and geographic groups. Asia's urbanized settings complicate this. There is often a large group of urban poor, the homeless and those invisible and recent migrants from rural areas who have not yet built enough networks, capital or nous to navigate complex cities during emergencies. A competent and safe outbreak response matters as much as a fair and equal one. Otherwise, the cohesion and solidarity of an entire country or society will be gradually broken by every outbreak threat.
Making Bold Political Choices During Non-Emergencies
Although an outbreak has a defined beginning and end, it's possible to imagine a world where there is an uninterrupted stream of outbreaks. The window is then closing for governments to build outbreak resilience into their health systems during non-emergency periods. What political choices can they make?
One, governments must spend money to expand and modernize country-level health systems. In narrow terms, modernizing disease surveillance systems could be straightforward. Operation centers (physical or virtual), rapid response teams, field epidemiologists, outbreak modelling and early identification are well-described in the literature. This system must be inter-operable to the systems adopted by other countries and must be linked to the existing WHO Global Outbreak Alert and Response Network (GOARN).

All this needs money, and there are two political aspects: procuring it and then deciding how much to allocate to outbreaks versus equally important areas like universal health coverage. It need not be a zero-sum game. More investment in health systems will see a rising tide of improvement that will also help any outbreak response. More and better-trained doctors and nurses, strong primary care and effective vaccination campaigns help improve population health during non-outbreak periods and can be deployed easily during outbreak periods.
Two, governments must consider health as a determinant of their national security. In practical terms, this means several things. Health ministers, health technocrats and health professionals must have a regular seat at national security council meetings to make decisions about migrant health and the politics of quarantines. There must be more regular touchpoints between the health, veterinary and ecology services, with many shared issues such as anti-microbial resistance and zoonotic infections. This approach is sometimes called One Health.
Difficult questions like, "should doctors and police officers get vaccines earlier than citizens?" must be answered
The production of vaccines and antivirals should be localized through capacity-building of pharmaceutical manufacturing led by state-supported investment. Some strategic stockpiling of medicines should be considered, with clear plans for speedy and equitable distribution to the population. Difficult questions like, "should doctors and police officers get vaccines earlier than citizens?" must be answered during non-outbreak periods, so that the social contract does not fray during highly emotional outbreak periods. All of this increases the legitimacy of governments, which they can leverage on during low-trust outbreak periods.
Building the capacity and effectiveness of managing other "chronic outbreak" communicable diseases like tuberculosis and malaria are important by themselves. Strengthening our response to non-communicable diseases could also strengthen the necessary health system muscles that will be needed during "acute outbreak" situations and improve the physical resilience of individual human beings against superimposed co-infections (a flu is obviously worse with tuberculosis in your lungs). Non-outbreak periods are also opportunities for health systems to audit their readiness and deepen relevant collaborations with the security apparatus of the state.

Three, having secured their duty to protect their citizens within their borders, governments must now collaborate among themselves. Pandemics could be globally catastrophic, and nation-state governments must give up some sovereignty and control in order to save themselves. The planetary health commons require multilateral collaboration in several ways. The most obvious is to build an information exchange system founded on trust, transparency, speed, and comprehensiveness. Some parts of the GOARN system should mimic that of the so-called "Red Phone" between Washington and Moscow, designed to "reduce the risk of war."
Bold political choices can save lives, and they must be taken during outbreak and non-outbreak periods.
The research and regulatory approval process for new vaccines and medicines must change. Currently, the scientific world uses the randomized controlled trial as the gold standard for regulatory approval of medicines, which can take many years and billions of dollars. During outbreaks, there is neither the luxury of time nor money. The recent Ebola outbreaks in West Africa are instructive, with controversies of whether to approve, manufacture and use vaccines or the ZMapp treatment during emergency situations based on purely experimental data. The ethics in outbreaks are challenging, so we must develop better research and approval processes during non-outbreak periods, including considering retiring the RCT model.
In the end, health is a political choice. Disease outbreaks represent a chance for governments to demonstrate competence and gain legitimacy. Bold political choices can save lives, and they must be taken during outbreak and non-outbreak periods.