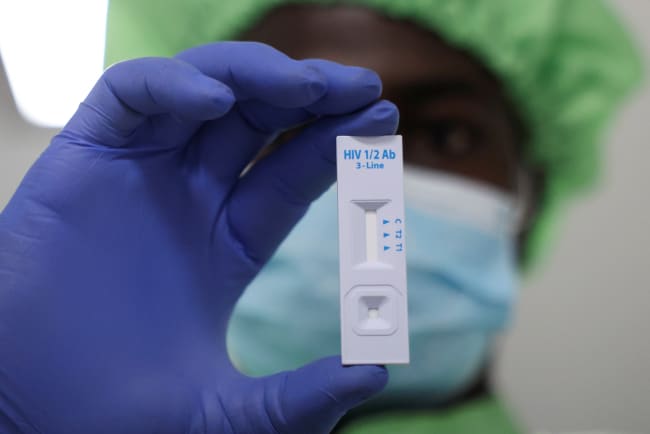
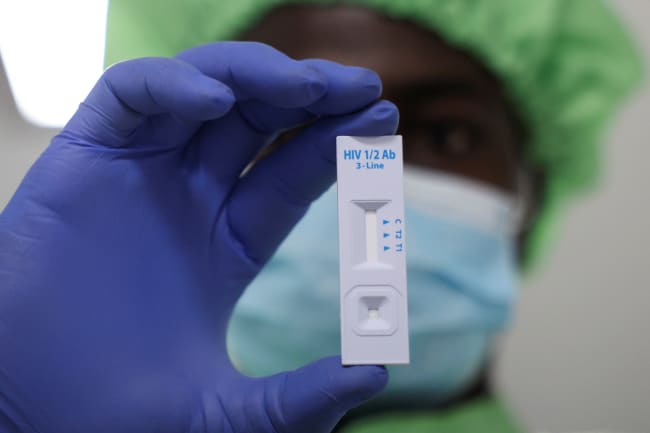
Latin American and Caribbean countries consistently report higher levels of happiness than other parts of the world, higher than national economic fundamentals would predict. But they also exhibit a high prevalence of mental illness, and depression and anxiety disorders are on the rise.
Latin America and the Caribbean's higher-than-predicted levels of happiness have been attributed to the region's unique cultural values of family and social life. Family bonds are tight. Friendships do, indeed, last a lifetime. Church attendance is relatively high. All of this can contribute to an outlook of optimism toward life. "My family loves me. My friends love me. God loves me. What's there to be unhappy about?"
That positive attitude, however, can hamper the recognition of mental illnesses. Positive reframing can be a coping mechanism to handle failures and manage stress because it yields a sense of gratitude and coherence that is associated with greater resilience. However, focusing excessively on positivity can have detrimental effects if it leads a person to dismiss emotions, downplay experiences, or deny reality, leaving negative feelings unaddressed.
The region papers over its mental health challenges. Typically, mental illness is often described as an elephant in the room — an imposing challenge that no one wants to talk about — but in Latin America and the Caribbean, the elephant is still waiting to enter the room.
More than 70 percent of people in Latin America and the Caribbean who need mental health care do not receive it
In Latin America and the Caribbean, people usually do not discuss mental health issues unless they interfere with daily life, perceiving that doing so would upset the order within a tight social circle. Furthermore, suffering from one of these conditions might be attributed to a lack of faith in God or, worse yet, sinful behaviors. These deterrents to speaking up about one's mental health delay care-seeking and treatment: more than 70 percent of the people in many Latin American and Caribbean countries who need mental health care do not receive it.
The impact of mental disorders has increased worldwide over the past two decades, according to the Global Burden of Disease study. Three main risk factors contribute to this trend, according to Dr. Alize Ferrari, who leads the mental health team: first, because people live longer, more individuals are reaching ages where mental illnesses become more prevalent and disabling. Second, depressive and anxiety disorders have increased in the wake of national or global catastrophes such as the COVID-19 pandemic, war and conflict, economic downturns, and natural disasters. Third, adverse experiences within the population such as childhood sexual abuse, intimate partner violence, and bullying exacerbate the prevalence and burden of mental disorders.
In Latin America and the Caribbean, the most prevalent mental disorders are depressive and anxiety disorders. Mental disorders hit youth hard: in Latin America and the Caribbean sixteen million people age ten to nineteen live with a mental disorder, more than the populations of Los Angeles, New York City, and Chicago combined. Similarly, suicide, sometimes an outcome of severe mental illness, is among the leading causes of death for people under age twenty, and the rate rose by 6 percent between 2000 and 2019. Among adolescents age fifteen to nineteen in the region, suicide is the third most common cause of death.

Latin Americans celebrate resilience and cherish the positive side of the current situation, as evidenced by phrases such as echao pa'lante in Colombia and Luchón in Mexico, referring to individuals who overcome life's challenges. Another popular idiom is Gracias a Dios estamos vivos, meaning "Thank God we are alive." Regardless of how dire the present circumstances may be, moving forward and not dwelling on past hurts is essential. People apply this mindset to everyday situations, be it the loss of a job, the onset of an illness, or to navigate violence or natural disasters or sociopolitical unrest. Although resilience can be a protective factor for mental health, the scant time and resources dedicated to properly processing grave and stressful situations might also accumulate and potentially aggravate mental illness.
Latin America and the Caribbean's high burden of mental disorders is aggravated by a huge treatment gap. Most national health-care budgets are allocated to treating physical conditions, leaving an average of 2 percent for treating mental health conditions, mostly via psychiatric hospitals. The region has fewer psychiatrists per capita than the average in the Organization for Economic Cooperation and Development and they are not evenly distributed. Countries such as Ecuador and Haiti have fewer than one mental health nurse per capita, less than one-tenth the regional average. The region is also losing psychiatric beds, down by 17 percent on average since 1991. Few preventive programs exist, and available health services are fragmented and focused on acute crisis care. Most people who require nonemergency care opt to pay for it out-of-pocket if they can afford to do so. Otherwise, they remain without care.
Poor mental health has a huge impact on a person's quality of life and economic productivity. It increases the risk for dementia and substance use disorders and contributes to unintentional and intentional injuries. Untreated mental health conditions can result in broken relationships, poor performance in school and work, unemployment, and homelessness. It also costs countries dearly. Latin American and Caribbean countries lose more than $30 billion annually due to mental disorders among youth.
There is still a long way to go to increase awareness and provide timely high-quality mental health care across the region
Some recent progress has been made in narrowing the gap. Jamaica has implemented a mental health program based on community and primary care services, training mental health nurses to facilitate timely and effective treatment. Chile and Peru have built up community mental health services. Colombia and Uruguay are adapting their health information system to target interventions based on risk profiles. But there is still a long way to go to increase awareness and provide timely high-quality mental health care across the region.
Change is in the air, however. The hit 2023 pop song by Karol G, "Mientras Me Curo el Cora," showcases the cultural traits mentioned earlier: the hope for a better future, the significance of family and friends, and the appreciation of being alive. But she also signs that "It's ok not to feel well. It's normal, not a crime," acknowledging that it takes time to heal.
The mental health elephant might be peering through the window, but more awareness and public discussion are needed to invite it into the room.
EDITOR'S NOTE: Yenny Guzman is employed by the University of Washington's Institute for Health Metrics and Evaluation (IHME). IHME collaborates with the Council on Foreign Relations on Think Global Health. All statements and views expressed in this article are solely those of the individual author and are not necessarily shared by their institution.
ACKNOWLEDGMENTS: The author would like to thank William Heisel and Dr. Alize Ferrari for providing feedback on this piece.
In the United States, if you or someone you know is in an emotional crisis, reach out to the National Suicide & Crisis Lifeline by dialing or texting 988.