mRNA vaccines have served as a formidable shield against COVID 19 infections. Following this success, there has been a steady increase in FDA approvals of regulatory RNA therapeutics for rare, previously untreatable diseases. Medicines based on mRNA technology are cost-effective, relatively simple to manufacture, and target once undruggable pathways compared to more conventional approaches.
The beauty of this therapeutic technology is that both small biotech startups and academic groups can rapidly develop new and personalized RNA constructs, leading to a broad reach amongst all strata of society. There is massive potential in mRNA therapeutics waiting to be tapped for the well-being of humankind—it could also alter the course of the pharmaceutical industry landscape.
mRNA's Shot to Fame–Covid-19 Vaccines
With Pfizer-BioNTech and Moderna's COVID-19 vaccines, mRNA instantly became a household name. Though the clinical reality of mRNA technology is in its nascent stage, the technology itself has been around and studied for decades. mRNA vaccines have been studied for flu, Zika, rabies, and cytomegalovirus (CMV). Recent technological advancements in RNA biology, chemistry, and delivery systems have mitigated the challenges of these vaccines and improved their stability and effectiveness. As soon as the necessary information about the coronavirus became available, scientists began designing the mRNA instructions for cells to build the unique spike protein.
There is massive potential in mRNA therapeutics waiting to be tapped for the well-being of humankind
Worldwide 277 million cases and more than 5.38 million deaths due to coronavirus have been reported at the time of the writing of this article. mRNA has been instrumental in saving lives. In the most extensive vaccination campaign of all time, more than 8.79 billion doses have already been administered across 184 countries. Though in a sign of growing global disparity, higher-income countries are getting vaccinated much faster than the lower-income ones. According to the New York Times, approximately 73 percent of shots given worldwide have been administered in high- and upper-middle-income countries, while only 0.9 percent of doses have been administered in low-income countries.
With the launch and widespread use of mRNA vaccines for COVID-19, 2020 was a breakthrough year for mRNA technology platforms. At the end of 2019, the combined market capitalization of the five publicly listed companies focusing on mRNA platforms was approximately $15 billion. Jumping ahead to August 2021, that capitalization climbed to more than $300 billion. And now, mRNA's success with COVID-19 vaccines has attracted heavy investment, promoting the development of treatments for other ailments.
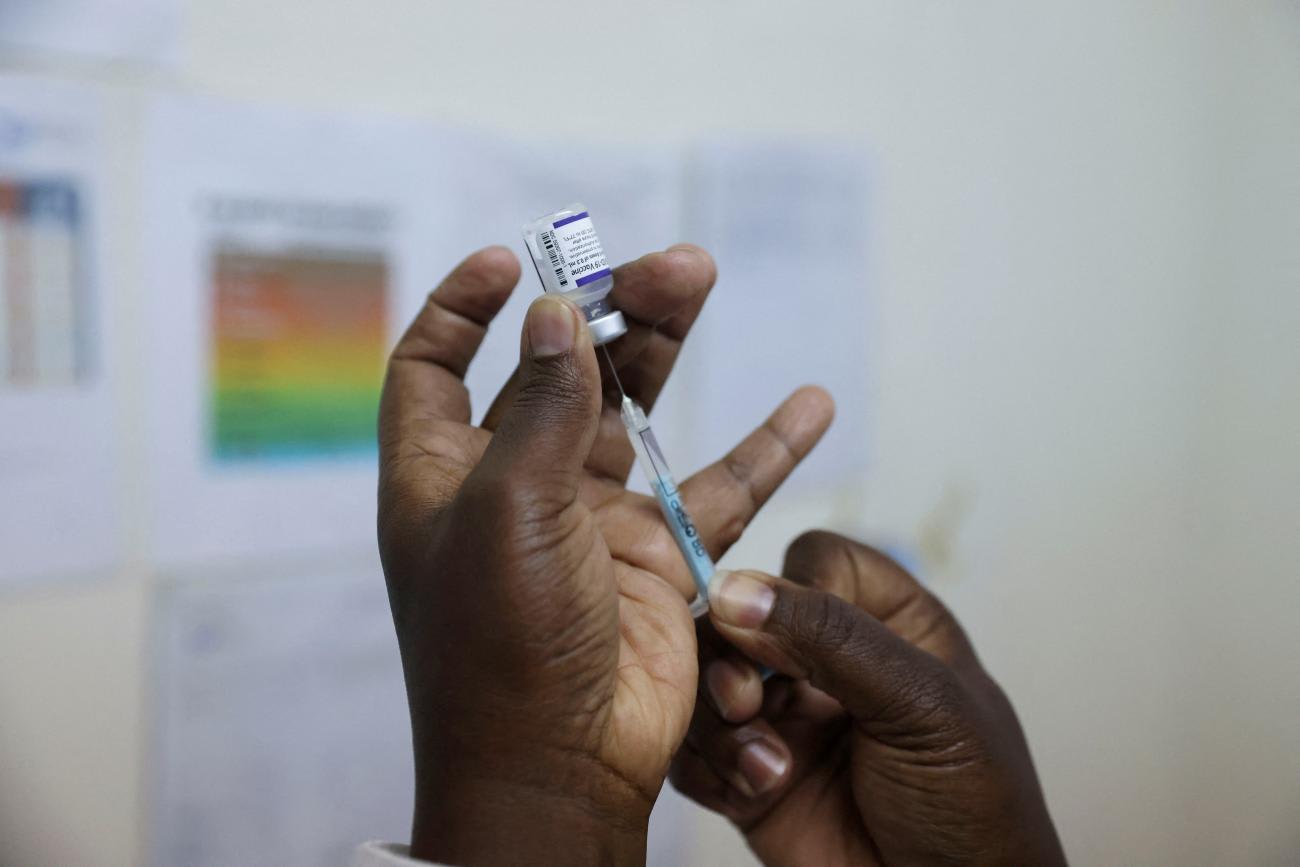
The Science of mRNA Therapeutics
Proteins are the workhorses that perform/facilitate almost all the molecular functions of the biological world. All the information regarding protein biosynthesis is coded and carried by DNA (sometimes RNA). The messenger RNA (mRNA) is quite simply the messenger of this information and carries it to the protein synthesis centers of the cell. Once the mRNA is used up by the protein synthesis mechanism to make a new protein, it is quickly recycled to be used again. Therapeutic mRNAs are engineered to help the human cell to produce a specific pathogenic protein (or a part of the protein) that can trigger an immune response. This leads to the generation of specific antibodies against the foreign protein, protecting us from the invading pathogen. The COVID-19 vaccines developed by Pfizer and Moderna contain mRNA that carry information for spike proteins that decorate the surface of the SARS-CoV-2. These vaccines require one or two booster shots after an initial immunization to jumpstart our immune system by generating enough antibodies to fight an actual coronavirus infection.
The virus is tricky though and fights back by mutating its proteins. For instance, the newly discovered omicron variant of the coronavirus has about 50 new mutations, and most of them are present in its spike proteins. This triggers a cat and mouse game between the vaccine developers and new virus variants. Scientists must keep up with new mutations to evaluate the efficacy of the existing vaccine, and they may have to go back to the drawing board to design new versions of the vaccine or tweak the current ones.
Distribution of COVID-19 Vaccines to the Rest of the World
While the swift development of the COVID-19 vaccine has been an unprecedented scientific achievement, it is only half the battle won. The access and delivery of these drugs to low-income areas is a crucial challenge and calls for priority actions from policymakers.
The COVID-19 virus is tricky and fights back by mutating its proteins
Production and distribution challenges, along with new viral strains, risk prolonging the pandemic. Experts have long warned about inadequate vaccination efforts leading to viruses that mutate. Omicron, a new COVID-19 strain first detected in South Africa, has already spread across the world. According to the U.S. Centers for Disease Control and Prevention (CDC), the omicron variant is now the most dominant strain in the United States. The World Health Organization (WHO) announced that as of December 16, 2021, the omicron variant had been identified in 89 countries and is spreading much faster than the delta variant.
Collaborative efforts between high-income country governments, pharmaceutical leaders, global health accelerators, philanthropic foundations, and grassroots organizations are pivotal in bridging the gap where demands outweigh supplies. One such multilateral framework is the Coalition for Epidemic Preparedness Innovations (CEPI). Norway, India, the Bill & Melinda Gates Foundation, the UK-based Wellcome Trust, and the World Economic Forum founded this global alliance. In addition, Gavi, the Vaccine Alliance—also established by the Gates Foundation, is a public-private partnership to improve vaccine access for lower-income countries. In June 2020, the WHO, CEPI, and Gavi launched COVID-19 Vaccines Global Access (COVAX), a global initiative that initially aimed to have two billion vaccine doses available by the end of 2021. Unfortunately, despite all these efforts, current global manufacturing capabilities are far below the requirement.
At a recent virtual Global COVID-19 Summit, world leaders promised increased vaccine donation and funding. The United States has pledged to donate more than a billion doses of the Pfizer-BioNTech vaccine to nations in need, making it the biggest such donation so far. Ghana was the first country to receive COVAX vaccines in February. Since then, more than 303 million doses have been shipped through COVAX to 142 countries worldwide, including Bangladesh, Brazil, Ethiopia, and Fiji. So far, vaccines from Oxford-AstraZeneca, followed by Pfizer-BioNTech, have a tremendous global reach. Dozens of countries at the World Trade Organization (WTO) are demanding a patent waiver for COVID-19 vaccines to scale up global production, but some countries oppose the idea, and negotiations are likely to be slow.
Countries including Italy, Saudi Arabia, the United States, Canada, the United Kingdom, France, Indonesia, Singapore, and New Zealand have implemented vaccination mandates. And countries including the United States, Israel, and China have started vaccinating children, too. Recently, the United States authorized booster shots for those 18-years–old and older who received a Pfizer-BioNTech or Moderna vaccine at least six months after their second dose. Some say booster shots will increase vaccine inequality, making it harder for middle- and low-income countries to vaccinate their people fully and should be allowed only for immunocompromised individuals. Time and again, studies have shown that the majority of COVID-19 related deaths are among the unvaccinated.
Intellectual Property Waiver for COVID-19 Vaccines—Yes, No, Maybe?
In October 2020, India and South Africa passionately appealed to waive Intellectual Property (IP) on COVID-19 vaccines, including patents, copyright, and trade secrets. More than 100 countries, including Russia and China, backed their request.
In the wake of such discussion, it is pertinent to note that Moderna announced that it would not enforce patents related to its COVID-19 vaccine against those making vaccines intended to combat the pandemic. It is also willing to license its IP on COVID-19 vaccines to others post-pandemic. In the broader picture, this serves Moderna's interest, creating a market for other mRNA therapies it is heavily invested in and protecting itself from any IP litigation relating to such patents. Above all, it is the best PR a company could get.
The proponents of the IP waiver say that vaccine manufacturers can contribute their IP to the UN-backed Medicines Patent Pool. This group identifies reliable manufacturers, assists with regulatory approvals, and provides drug developer royalties on drugs sold. In India and South Africa which have robust generic drug industries, they are proposing that they're aptly suited to manufacture and distribute vaccines during a pandemic once the IP waivers are granted.
Germany, Switzerland, and the EU oppose any such proposal, however. With the emergence of the omicron, the U.S. president has joined calls for waiving the IP protections for COVID-19 vaccines, facing backlash from the IP community at home. The most notable objection comes in a Center for Strategic and International Studies (CSIS) report in which the authors advocate for improving vaccine diplomacy and for better distribution networks worldwide. They opine that any such waiver is ineffective in increasing vaccine production and would prompt the theft of mRNA technology developed by the United States, putting it at the "competitive disadvantage and raising national security implications as well."
The report authors also assert that production lines are already running at their fullest using all the vital ingredients needed to make such vaccines. Instead, the authors suggest increasing their donation of vaccines and the equipment to ship, refrigerate, and administer them to COVAX. They divert the world's attention to the existing problems in the system such as raw materials availability, eliminating trade barriers (for example, removing tariffs and other unnecessary trade restrictions), supply chain tracking, manufacturing capacity, donations, and leadership. The authors warn that waiving IP will hamper current vaccine research and development and any such future efforts. Various policy experts concur with the views expressed in this report. They conclude with a caution that "while voiding IP protections would not increase vaccine production, doing so would strike a severe blow against the United States' world-leading biotech industry."
The pharmaceutical companies are already cooperating widely with their competitors and the generic manufacturers with voluntary licenses, collaborated manufacturing of vaccines (including those by Indian and South African companies), proactive technology transfer, and tiered pricing.
Recently, the United States authorized booster shots for those 18-years-old and up
The opponents of IP waivers largely agree on making the vaccines available to every person on the planet as quickly as possible. They suggest that by increasing global manufacturing, avoiding vaccine hoarding, timely distribution of vaccines by better utilization of the existing network, and by not throwing away any unused vaccines that vaccine (un)availability can be addressed to a greater extent. They also uphold that it'll be tough to maintain quality control—promoting vaccine hesitancy—if such a waiver is granted. No IP rights have been enforced yet, so there's no impediment to public health.
The Agreement on Trade-Related Aspects of Intellectual Property Rights (TRIPS) is an international legal agreement between all the WTO member nations. This agreement provides for the issuance of compulsory licenses by the countries to produce vaccines without permission from the patentee. However, no government has opted for compulsory licensing, as it prevents exports (hence no vaccine diplomacy).
Amid all this noise, it is interesting to note that since these vaccines were developed so quickly, patents specifically covering them have not yet been granted in some member nations, such as India. So, the whole idea of enforcing an inexistent patent is moot.
Both sides are pushing their argument forward vehemently. A common intellectual property response to COVID-19 was proposed to be discussed in the WTO's 12th Ministerial Conference. This conference's November 30 – December 3 meeting has now been indefinitely postponed due to the recently omicron-related travel restrictions.
What's Next for mRNA Therapies?
Even before COVID-19 made mRNA a household name, many clinical trials were already underway using mRNA in vaccines for infectious diseases, cancers, and autoimmune diseases. A recent search of ClinicalTrials.gov found 1,961 studies involving mRNA, of which more than 100 are already in Phase III. Programs include mRNA used in respiratory diseases, different types of cancer, herpes, metabolic syndromes, kidney diseases, heart diseases, and even obesity. Even after a year of vaccine availability for COVID-19, a stunning 18 clinical trials are underway related to SARS-CoV2 conditions.

The enormous disruptive potential of this technology has attracted significant mRNA vaccine collaborations. For example, the U.S. government has partnered with Moderna to develop a vaccine for the Zika virus for $125 million. The Bill & Melinda Gates Foundation has invested $100 million in Moderna's mRNA vaccine programs for seasonal flu, the Nipah virus causing encephalitis, and HIV. Triggered by their mRNA technology collaboration for vaccines and therapeutics development, Sanofi acquired Translate Bio for $3.2 billion. They became the first company to start a seasonal mRNA flu vaccine candidate clinical trial in June 2021 and are now in Phase 1/2 of clinical trials to develop mRNA medication for cystic fibrosis. Scientists also use mRNA to begin clinical trials of herpes simplex virus 2, a common sexually transmitted disease. Moderna has partnered with Merck in a clinical trial of a combo treatment—using a personalized mRNA cancer vaccine and the immunotherapy drug Keytruda—for patients with colorectal and head and neck cancers.
Science magazine recently reported that Yale University researchers had developed a novel lab-stage mRNA vaccine that protected guinea pigs from Lyme disease and other tick-borne diseases. It still needs to be seen how effective it is in humans, but it is a notable development given that approximately 476,000 Americans are diagnosed with and treated for Lyme disease each year, according to the CDC.
Scientists are also looking at a technique where mRNA is transferred into a patient's cells ex vivo, then administered back into the patient. This method is being investigated for genome engineering, genetic reprogramming, T cell- and dendritic cell (DC)-based immunotherapies for treating cancer and infectious diseases, some protein-replacement approaches, rare and cardiometabolic conditions, and production of on-demand personalized vaccines.
mRNA is making diagnostic progress, too. Swiss-based Novigenix SA was recently awarded the 2021 Felix Burda Award in Medicine & Science for excellence in innovation and early cancer detection using unique mRNA detection methods. Eventually, it may even replace colonoscopies, possibly increasing early detection screenings.
Recently, several universities have opened RNA centers to advance therapeutic applications of RNA, including in vitro transcribed (IVT) mRNA. These centers include the RNA Therapeutic Institute at the University of Massachusetts, the Yale Center for RNA Science and Medicine, and the RNA Institute at the University at Albany, State University of New York. In addition, many university spin-off companies, including BioNTech, CureVac, eTheRNA, and Moderna—are at the forefront of mRNA research.
SARS-CoV-2 has undoubtedly excited the mRNA research community. The investment of billions of dollars in mRNA technology reflects the optimism that this technology can find cures for previously untreated diseases and deliver much more than the current COVID-19 vaccines. mRNA technology is here to stay.