The United States is extremely diverse. Regional differences abound, shaped by the geography, legacy of slavery, native persecution, and history of migration. Diversity, however, is often discussed in the context of cities, such as New York, where large populations in northern Manhattan hail from the Dominican Republic and immigrants from Yemen live in the eastern Bronx. What about rural areas?
Jefferson County, Oregon, is just one area that illustrates how the rich and varied lived experiences of people living outside major metropolitan areas should be considered if health in rural areas of the United States is to be improved. The county's population is more than 60 percent white, 21 percent Hispanic or Latino, and 18 percent American Indian, mostly from the Warm Springs, Wasco, and Paiute tribes that form the Confederated Tribes of Warm Springs. The county's median income is $60,000 per year, but 16 percent of the population still lives under the poverty line. The population is small but it is incredibly diverse.
The county's median income is $60,000 per year, but 16 percent of the population still lives under the poverty line
Jefferson County, of course, is not the only example of the diverse populations that inhabit rural areas of the United States. Take Garfield County, Oklahoma, a county with just fifty-nine people per square mile and a large Marshallese population that in 2017 was estimated to be almost three thousand, or about 6 percent of the county's total population. Teton County, Wyoming, is another example, with just six people per square mile but home to Jackson Hole, a wealthy enclave that drives the county's median household income above $100,000.
Rural America is sometimes defined as the leftover places on the map after metropolitan areas have been defined. A persistent narrative from reporters and researchers outside rural areas is that those areas are white, poor, and hopeless. This is a damaging stereotype that prevents people from accurately understanding the health of all populations across the United States.
A new study published in The Lancet by researchers at the Institute for Health Metrics and Evaluation and the National Institutes of Health estimates mortality rates (deaths per hundred thousand people) at the county level for nineteen causes of death and for five racial and ethnic populations. The findings present a slice of how health varies widely across rural areas.
In the United States, health in rural areas is on average often worse than in urban areas, but stratification by cause of death, racial and ethnic population, and county demonstrates wide variation in health that complicates this statement. Capturing how health differs across rural areas, however, is difficult because the data often is quite unreliable and sometimes incomplete due to privacy protections. The study aims to overcome some of the reliability issues in low population areas by using models that incorporate information from nearby counties, across years and age groups using statistical techniques that require substantial computing power and thus have not been previously developed. It also adjusts for misreporting of race and ethnicity on death certificates, which occurs when the race and ethnicity listed on the death certificate are different from self-reported identity. This can occur, for example, when a funeral director documents the race and ethnicity of the decedent using their observation instead of asking next of kin.
Age-Standardized Mortality for Three Diseases by Ethnicity and Urbanicity
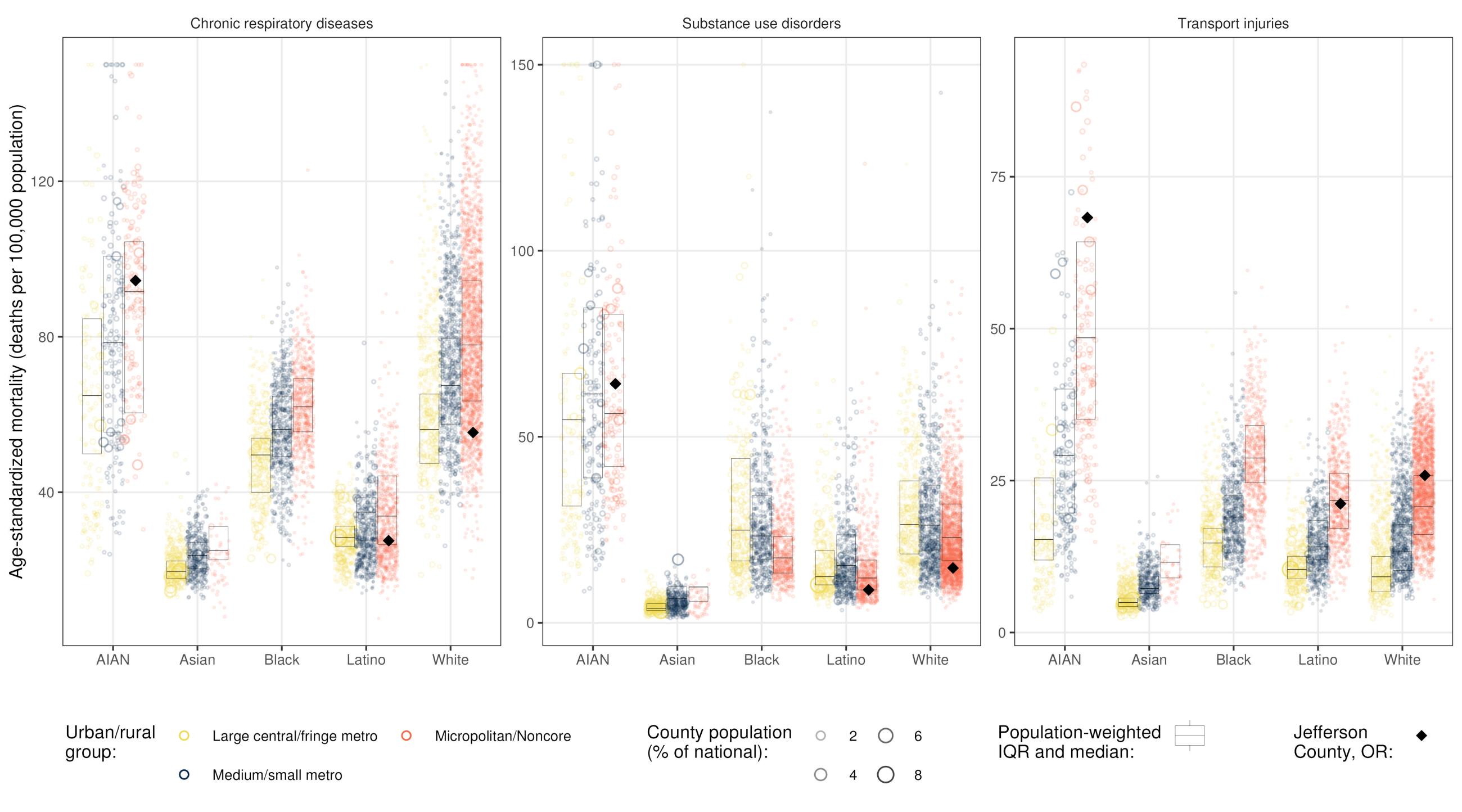
Generally, the pattern that emerges is that mortality is higher in counties that are more rural, but variation between areas is large. Relative to metropolitan areas, mortality from substance use disorders in more rural counties is slightly lower. This varies by racial and ethnic population, the largest differences being among non-Hispanic American Indian or Alaska Native (AIAN) populations. Conversely, mortality from transport injuries is substantially higher in more rural areas. Mortality rates between racial and ethnic populations in counties with different urbanicity levels also show overlap, revealing that mortality is not always higher in urban or rural areas or among one racial and ethnic population relative to another. For example, a large portion of the most rural counties have mortality rates from chronic respiratory diseases among the Black population that are similar to those among the white population in the most urban counties. The patterns in Jefferson County alone also tell a story about rural diversity. Relative to other rural counties, its mortality rates among populations that are white or Latino are either around the median or lower for all three of causes of death. However, almost the exact opposite could be said for the population of AIAN people, for which mortality relative to other rural counties is quite high. This is especially true for transport injuries, for which the mortality rate is almost seventy deaths per hundred thousand, higher than among the AIAN population in more than 75 percent of other rural counties.
Reflecting on her time as an epidemiologist working on various regional Central Oregon public health initiatives from 2016 to 2021, Dr. Jenny Faith notes that distinct demographics are part of the reason "strategies for Jefferson County and neighboring Crook and Deschutes counties often had to be quite different from each other." Both nearby counties are more than 80 percent white, and both are wealthier: the median household income is nearly $65,000 in Crook County and $74,000 in Deschutes County. "There is great diversity both within and across these counties," says Faith, but this discussion of diversity is almost never in the context of rural America. Additionally, Faith emphasizes that one should "never assume that county-level statistics reflect the experience of every person in a county." Within these complexities — although health care is generally less resourced in rural places relative to urban areas — public health officials, medical providers, and other members of this community seek to understand what is causing observed health patterns.
… Mortality is not always higher in urban or rural areas or among one racial and ethnic population relative to another
To illustrate how mortality varies widely, some of the study's results are presented for three causes of death, grouping by racial and ethnic population and the degree of urbanicity as determined by the National Center for Health Statistics (NCHS). Using the NCHS categories, the counties with highest population densities (that is, the most urban), such as those containing major cities, are designated "large central and fringe metro areas." The counties with the smallest population densities (the most rural), such as those with small populations but large areas, are designated "micropolitan and noncore counties." Each circle corresponds to one county, and the size of the circle is proportional to the population of a given racial and ethnic population in that county. Within each group, whether urban or rural, a quarter of each racial and ethnic population lives in counties below the bottom line of the box; another quarter lives in counties above the top line of the box. The middle line indicates the median mortality rate. The diamond represents mortality for Jefferson County, for which estimates are not presented for the Asian and Black populations due to their small sizes.
To do so, it is crucial, Faith says, to form partnerships with people and organizations more intimately familiar with what could be driving particular trends for certain diseases, populations, or parts of the county. One manifestation is the Central Oregon Regional Health Assessment, released every four years and including work from partners in Crook, Deschutes, Jefferson, and northern Klamath Counties and the Confederated Tribes of Warm Springs. Along with interviews with community focus groups, the report includes a detailed analysis of fatal motor vehicle accidents, including a comparison with neighboring counties. The report highlights that "focus groups throughout Central Oregon identified the need to work collaboratively across county lines to create healthy built environments that include effective and affordable public transportation systems, safe alternate commuting options, and community spaces." The findings were presented to county commissioners, other local stakeholders, and the public in a series of presentations across Central Oregon communities. It was also featured in the Madras Pioneer, a local publication, which calls out the death of Nadia Rankov Adams as one person among many whose life was lost to a traffic accident, reflecting the high rate of fatal transport injuries in Jefferson County. Adams was killed in a head-on collision with a semi-truck, the third multivehicle collision in three weeks on the stretch of highway between Redmond and Madras.
Jefferson County, Oregon, is one example among many that reveals the diversity of rural areas, the complex picture of health among populations in less urban areas, and the important work that local community members and organizations do to understand what people in their county need. They know the extent to which understanding any one county and even part of a county is complex and requires more than just numbers. But even using numbers alone, the diversity of rural America is clear. The United States is a melting pot in places beyond major cities and rural America should not be treated as a homogenous behemoth.

EDITOR'S NOTE: The author is employed by the University of Washington's Institute for Health Metrics and Evaluation (IHME). IHME collaborates with the Council on Foreign Relations on Think Global Health. All statements and views expressed in this article are solely those of the author and not necessarily shared by their institution.
ACKNOWLEDGMENTS: The author would like to thank Zhuochen Li for fact-checking assistance, and Dr. Laura Dwyer-Lindgren, Jessica Solis, and Kristofor Larsen for providing feedback on the draft.