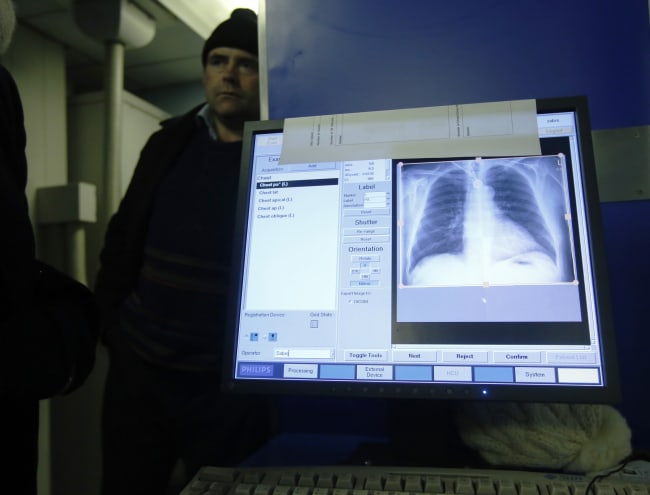
The United States is making progress vaccinating at-risk people against SARS-CoV-2 — but it isn't nearly fast enough. Since mid-December when the first vaccinations were given, fewer than 20 million people have received two doses — around five percent of the population. At this rate, it would take nearly two years to vaccinate the entire country.
Even as we debate the efficacy of vaccines against the various new variants, whether they prevent transmission, and whether you can forego masks with your friends and family when you're vaccinated, the fact remains: all of these discussions are moot if we can't get vaccines into arms as quickly as possible.
A quarter of all Americans lack a primary care physician
So, more options to expand vaccination have been proposed, including to increase the role of pharmacies to provide individual vaccinations, to hold public health clinics, and to allow doctors' offices to vaccinate their patients. But for many, the long telephone waiting times, the need to clear schedules, and the need for internet access are prohibitive. A quarter of all Americans lack a primary care physician, a third live in "pharmacy deserts" with nowhere in a reasonable distance from their home to fill a prescription, and eight percent lack the language skills to easily make vaccination appointments. Reaching all of these people will continue to present challenges as the vaccine rollout expands beyond priority groups to the general population.
There's one site for vaccinations that has been largely overlooked and could help fill this gap: emergency departments, or EDs. EDs are well placed to provide vaccinations, and with careful planning for the logistics of allocating vaccine, preparing staff and patients for ED vaccine administration, and integrating them into the vaccine delivery system in individual health districts, they can be efficient, valuable parts of the overall effort to vaccinate the United States.
There are 139 million emergency department visits per year, and 90 percent of these patients get discharged after their visit. This figure represents millions of opportunities to administer vaccine to an unvaccinated person (the 10 percent who are admitted may be too sick to be vaccinated at the time). In addition to EDs attached to hospitals, urgent care clinics are another option, accounting for 89 million patient visits per year.

Vaccinating patients in an emergency department is not a novel concept: EDs give influenza vaccines to patients each fall and winter, and tetanus and rabies vaccines to those who need them. And emergency physicians are themselves supportive: a recent newsletter of the Society of Academic Emergency Medicine suggested EDs consider implementing COVID-19 vaccination programs. Journalists elsewhere have argued that fire stations and EMS crews administer vaccines, for reasons that apply in many ways to EDs, as well.
Using EDs as vaccination sites would accelerate the pace of vaccination, but it would also expand access to underserved populations, who often seek care in EDs because they have less access elsewhere. On a recent shift for example, one of us took care of a 70-year-old man from rural Virginia who was eager to get the vaccine but had no idea how to register for it. He couldn't make an appointment online because, like many rural and older Americans, he had no home internet access (a problem facing many Black and Hispanic Americans, too). It would have been easy for us to give him a dose before he was discharged, but that is not yet an option available to ED patients, and the best we could do was provide him the health department hotline and send him on his way. It shouldn't be this way.
About 30 percent of Americans are reluctant to take the COVID-19 vaccine
An ED has some features that improve its accessibility. As familiar sites of health-care delivery, they may be more welcoming to undocumented people than government entities such as health departments. ED clinicians can provide accurate medical information to the vaccine reluctant (at last count, about 30 percent of Americans), better informing their decisions and perhaps changing their minds. African-Americans are twice as likely to report seeking care in emergency departments, suggesting that EDs are a place where we can begin to work towards vaccine equity, too.
ED nurses are already trained in vaccine administration, and many have participated in vaccine drives specific to the COVID-19 vaccine at their institutions. Providers in the ED will have the opportunity to allay patient concerns and address vaccine hesitancy, and after a year of dealing with the effects of the pandemic, hugely motivated to do so. For many patients, this could be their only chance to discuss COVID-19 vaccination with a health-care provider.
Making this a reality will take planning and establishing systems and protocols. Emergency departments will need to develop plans for identifying eligible patients, discussing the vaccine and offering it to them, and watching them for the requisite 15 minutes after injection (which in most cases will be a tiny part of the patient's overall ED stay). Health departments or hospital systems should be prepared to provide EDs with vaccine doses to distribute, and should be assessing patient data to determine a reasonable number. As the Biden administration continues to evaluate and refine its vaccine plan, it should provide direction to hospitals and health departments on using EDs as vaccine sites across the country.
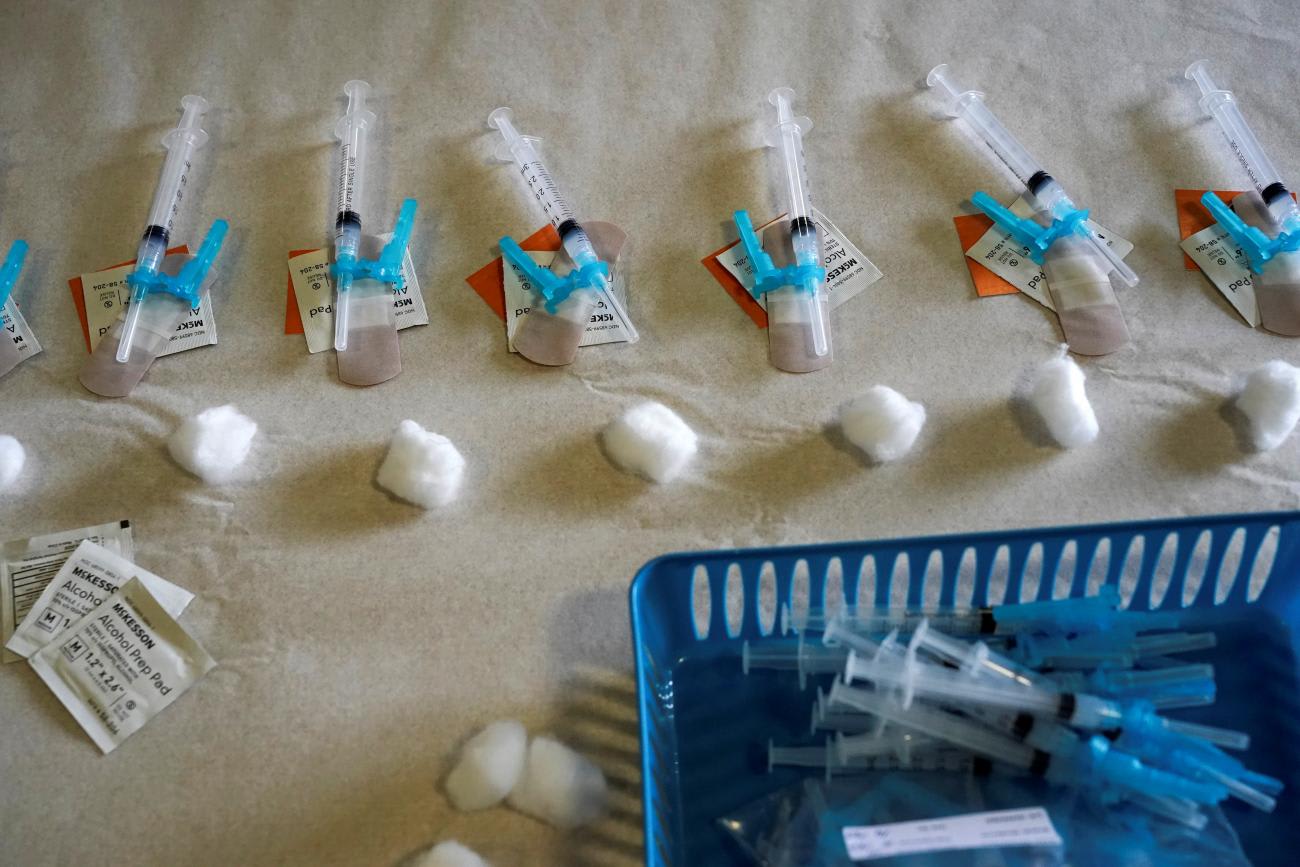
In addition to allocating a specific number of doses to EDs, health departments should consider using them as sites to routinely re-route doses left over at the end of the day at other vaccination sites. When vaccines vials are shipped from the manufacturer, they are frozen and in a concentrated form. On the day they are to be used, they must first be thawed, then allowed to warm up to room temperature, and finally, diluted. At each stage, there is a limited time in which they must be moved along to the next stage before they are used, or they must be discarded. Vaccine injection sites go to great lengths to make sure they do not overestimate the number of doses needed so that they do not waste any precious vaccine. But they do sometimes thaw or dilute more vaccine than needed, resulting in a scramble to use all the doses before they expire. It's not always easy to find eligible patients to get all of the doses, but EDs always have patients at all hours, and an organized plan to deliver extra doses to them could help take care of this problem.
Vaccine injection sites go to great lengths to make sure they do not overestimate the number of doses needed so that they do not waste any vaccine
EDs would plan to vaccinate patients who are there for emergent or acute medical problems. However, if people come to the ED asking specifically for vaccines, this could be handled by setting up on-site stand-alone vaccination clinics for a few hours each day, or identifying a staff member who could vaccinate these patients without a full ED visit if they have no other medical concerns.
Given the equity considerations, the ability to offer vaccine to patients who might not seek it out or might not otherwise have access to it, and the unique opportunity for patient education, EDs should be used to expand vaccine distribution. Planning for this should start now, before the vaccines become widely available, so that EDs are prepared and well placed to succeed in COVID-19 vaccination.