In 2022, the world faces unprecedented food crises driven by conflict, climate change, and COVID-19. Russia's invasion of Ukraine has drastically reduced the global supply of grain and restricted farmers' access to fertilizers, sending food prices soaring. Global fluctuations in climate are exerting direct effects on agricultural yields, livestock production, and fisheries and aquaculture systems, while also influencing the pillars of food security—availability, access, utilization, and stability. Meanwhile, COVID-19 disruptions continue, with declines in income and surges in poverty threatening access to food. Against this backdrop, addressing the health repercussions of food insecurity is more urgent than ever.
In communities experiencing food crises, children with orofacial clefts—cleft lip and/or cleft palate—are among the most vulnerable. Children with orofacial clefts are twice as likely to be malnourished as the general population, according to a new global analysis from the Institute for Health Metrics and Evaluation and Smile Train, the world's largest cleft-focused nonprofit organization. Nearly half of malnutrition-related deaths in individuals with orofacial clefts could potentially be prevented with access to adequate treatment and support.
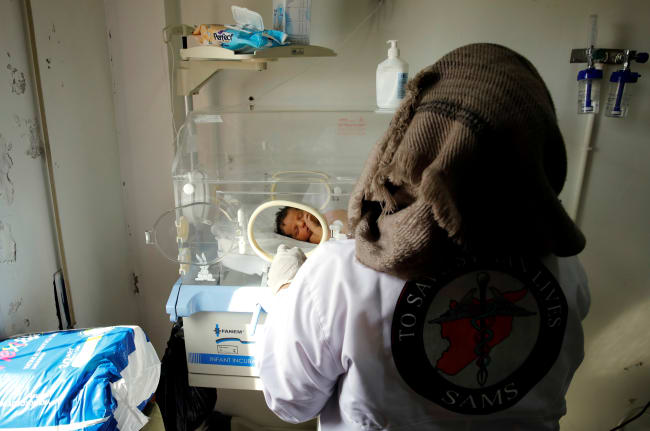
Children with cleft lip or cleft palate are more prone to infectious diseases than children without clefts
The Relationship Between Cleft and Malnutrition
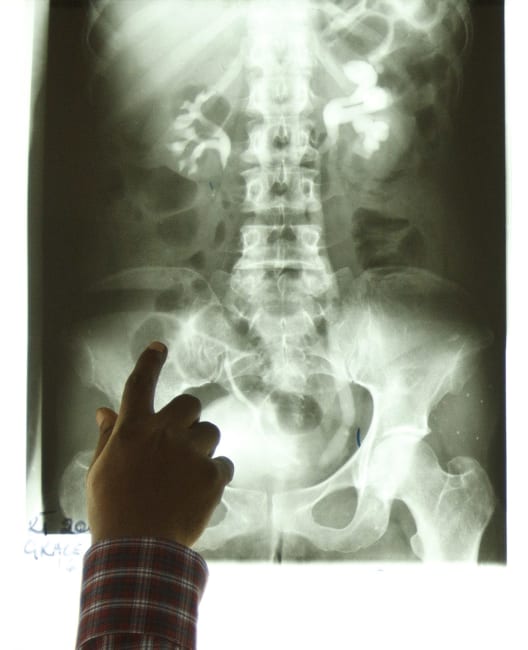
Cleft lip and cleft palate occur when a baby's lip or the roof of the mouth does not form properly in the womb. Cleft conditions increase children's risk of developing health problems. They struggle to receive adequate nutrition due to their condition, which subsequently weakens their immune response. Children with cleft lip and/or cleft palate are more prone to infectious diseases than children without clefts. Cleft abnormalities impair the function of the nasal cavity, increasing the likelihood of developing ear infections. Children with clefts are also at a higher risk for aspiration pneumonia, which can occur when food or liquid gets lodged in the lungs.
Because cleft conditions make it challenging to eat, children with these conditions are predisposed to growth stunting and being underweight. Breastfeeding and bottle feeding take more time for children with clefts; it is common for them to regurgitate food through their nose and mouth when nursing.
Sharon Wumocha, a mother from Kenya who has an infant with an orofacial cleft, described in an interview with Devex the difficulties that her infant son faced while breastfeeding. She said her son's mouth would be overflowing with milk, and that it would "almost choke him."
Malnutrition is not just a consequence of orofacial clefts—it also can be a cause. Children are more likely to be born with clefts when their mother or parent is sick or malnourished while pregnant, or lacks core micronutrients, such as folic acid and zinc. Clefts are more likely to occur when a parent does not gain adequate weight during pregnancy. Smoking tobacco during pregnancy or being exposed to high levels of air pollution are also risk factors for cleft.
Among children younger than five years of age who have orofacial clefts, the regions with a high burden of malnutrition are South Asia and parts of Africa. The African countries that stretch from Mali to Somalia have the highest rates of death from cleft-related malnutrition. Many of the countries with higher rates of orofacial clefts also appear in the World Food Program's top ten countries with the greatest numbers of people experiencing food crises. These countries include Afghanistan, Democratic Republic of the Congo, Ethiopia, Nigeria, Pakistan, South Sudan, and Sudan. By targeting food security program interventions to children with clefts in these areas, decision-makers could maximize humanitarian assistance.
Total Prevalence of Children Under 5 Who are Underweight With Cleft
Total prevalence of children who are underweight (per 1,000 people) among those with cleft, under 5 years, both sexes, 2020
Cleft Palate and Lip Surgery
Surgery to repair a cleft palate and/or lip is not possible immediately after birth because of the risks of giving a tiny baby anesthesia. Also, doing the surgery too early increases the likelihood that it will not be effective. Most cleft surgeries occur in children between three months and two years of age. Also, children need to be strong enough to have surgery. If the child is malnourished or fighting off an infection, they cannot undergo surgery until their body is healthy enough to endure the procedure. When a child receives corrective surgery under diminished health conditions, there is a greater chance that the repair will fail and post-operative complications will arise.
Early intervention to identify children with orofacial clefts and provide support for their parents and caregivers can reduce children's risk of dying from malnutrition or other health complications. Ensuring that children with clefts receive a diagnosis from a medical professional and get treatment as early as possible can be lifesaving. From 2000 to 2020, there has been a marked improvement in the general population in terms of reducing the prevalence of underweight. Yet, for children with clefts, the improvements have been much slower.
Without early diagnosis and intervention, children with clefts often fall farther and farther behind on the growth curve. Providing support and education to parents or caregivers is vital to ensure that children with clefts receive adequate nutrition, prompt treatment for any infections that arise, and surgery to repair their cleft as soon as it is feasible.
In Ethiopia, Getaw Alamnie is a plastic and reconstructive surgeon at Yekatit 12 Medical College Hospital in Addis Ababa, a Smile Train hospital. Alamnie is working to make cleft surgeries safer. "There is a higher risk of complications on surgery in children than compared to adults, and when it comes to patients with clefts—the majority of which are children—because they have difficulty feeding, they tend to be underweight and compromised nutritionally," he said in an interview with Smile Train in May 2022.
"Part of this work is to address these problems as much as possible to strengthen the child before the surgery," he added.
In Peru, nutrition counselor Adriana Zavalaga started a program to help children with clefts become stronger before undergoing surgery. Zavalaga is a volunteer with Misión Caritas Felices, an organization that partners with Smile Train. In a March 2021 interview, Zavalaga described what motivated her to start the cleft surgery preparation program.
"We noticed a pattern of malnutrition and anemia in many of these patients that would temporarily disqualify them from cleft surgery," she said. Through the program, Zavalaga provides nutrition education to the families of children who are scheduled to have cleft surgery and gives away healthy food to families in need.
Much work is needed to meet people's basic human right to food. With relief workers striving to meet the challenge, building in a focus on children with clefts can reduce the burden of malnutrition. By providing healthy foods—such as protein, whole grains, fruits, and vegetables—nutrition counseling, and medical support to families of children with clefts, along with implementation of a treatment plan that includes follow-up care, up to half of the malnutrition-associated deaths that occur every year can potentially be prevented.

EDITOR'S NOTE: The authors are employed by the University of Washington's Institute for Health Metrics and Evaluation (IHME), which produced the research described in this article. IHME collaborates with the Council on Foreign Relations on Think Global Health. All statements and views expressed in this article are solely those of the individual author and are not necessarily shared by their institution.