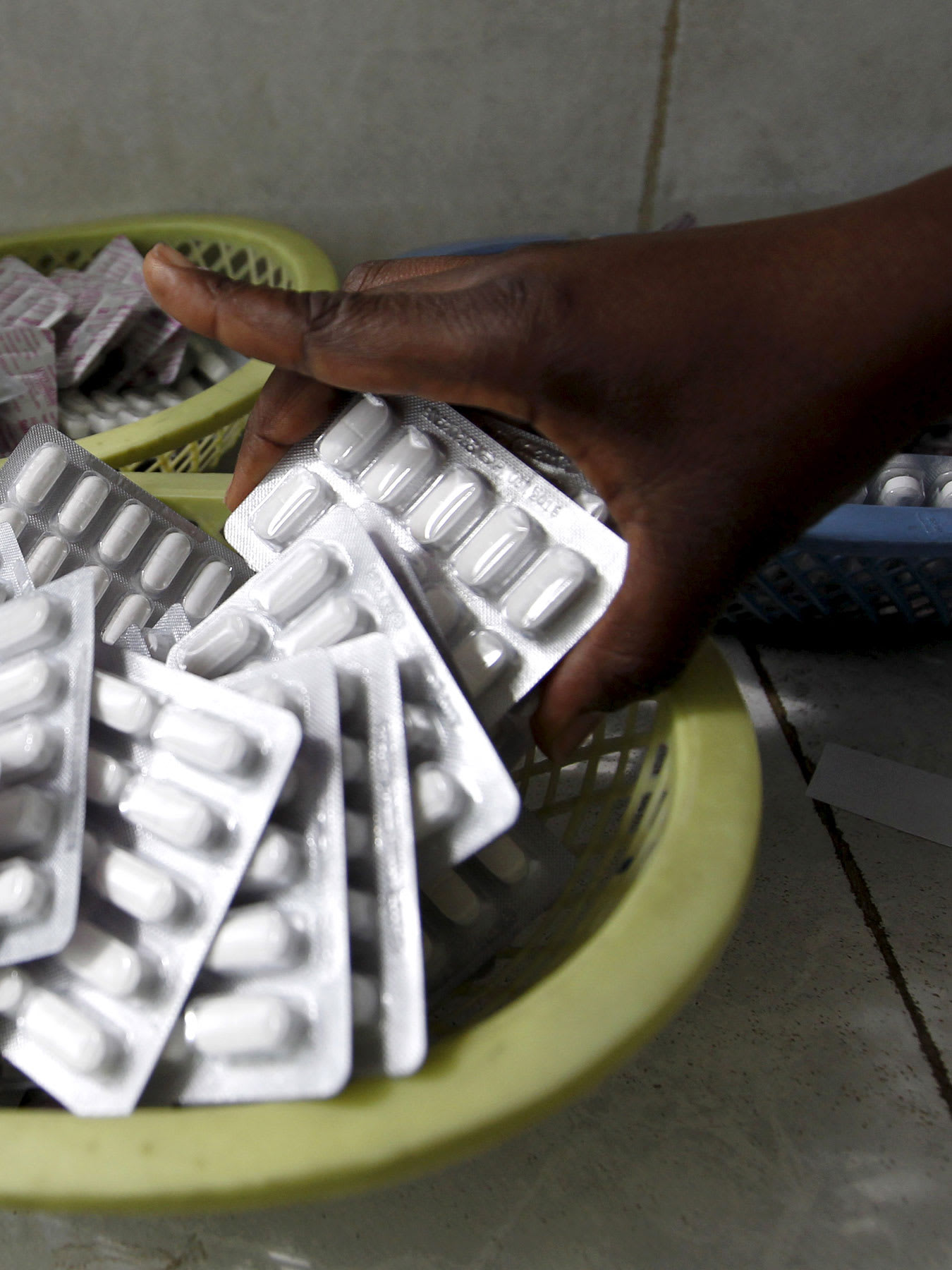
One of the most remarkable breakthroughs in last 20 years of the HIV epidemic has been the development of pre-exposure prophylaxis (PrEP)—the idea, long since proven clinically, that prescribing antiretroviral drugs to high-risk people who do not have HIV will prevent them from getting it. But PrEP only works if people have access to the drugs—so how will access change now that California has become the first state to make the PrEP drug Truvada available to anyone without a prescription? Will similar laws be passed in other states and other countries?
Since the HIV epidemic began in 1981, treatment and prevention methods have dramatically improved, both in terms of affordability and effectivity. Traditionally, prevention methods were largely focused on addressing behaviors, like condom use or abstinence, but the concept of using treatment as prevention emerged after the resounding success of antiretroviral therapy (ART) at controlling virus levels
lower risk of HIV for men who have sex with HIV+ men
Antiretroviral therapy revolutionized HIV/AIDS care beginning in the 1990s and has extended the lives of millions of people living with HIV. Soon after its introduction, researchers discovered something provocative: when the virus is so well controlled that it cannot even be detected, there is essentially zero chance of transmitting it to anybody else. This finding transformed prevention into a medicinal framework because it meant communities could reduce the number of new infections through testing and connecting people with care. It meant so-called discordant couples (in which one person is HIV positive and the other is negative) could effectively prevent transmission from one partner to the other through treatment alone.
And it meant that people who are HIV negative could reduce their risk of getting HIV/AIDS by taking a once-daily drug like Truvada, which reduces the risk of HIV infection by more than 90 percent for men who have sex with men and by more than 70 percent for those who inject drugs.
California, where Truvada was developed, was an early adopter of treatment as prevention, and in their recent bill they moved ahead of the pack. Until recently, the state's model of HIV prevention centered around condom use, PrEP dispensed by prescription for HIV negative people at high risk, and antiretroviral therapy for people living with HIV/AIDS. The new law, passed by California's legislature and signed into law by Governor Gavin Newsom on October 7, 2019, expands access even further. It allows pharmacists to dispense sixty days' worth of Truvada to HIV-negative individuals without a prescription. This means people who have an urgent need can obtain immediate access, and it addresses the stigma people may face in having to ask a trusted doctor for a prescription.

However, the new California law fails to lower financial barriers, making no assumptions about who will pay for the drugs. While many insurance companies may help cover or defray the costs, demographics suggest those who may benefit the most from PrEP are disproportionately uninsured and can afford it the least. With one month's supply costing a prohibitive $2,000 or so, the drug remained inaccessible to many, even as it becomes available over the counter. However, as of early December 2019, uninsured people with prescriptions can now receive PrEP cost free in the United States. Despite this, each stride of progress is not wholly inclusive, as prescriptions require doctors' appointments that may again be cost prohibitive to the uninsured.
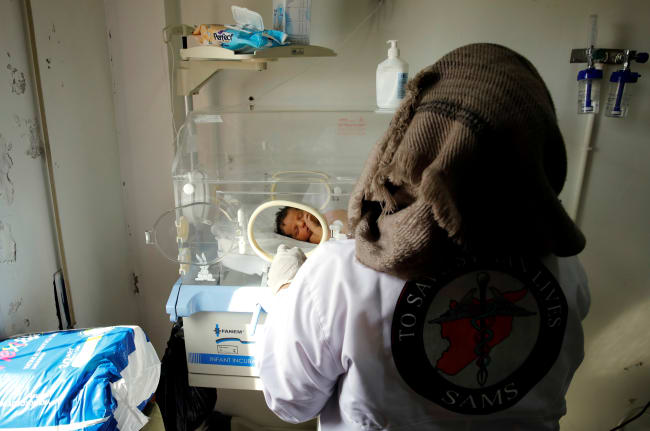
How well could California's approach work in other places—particularly lower-resource settings where even larger numbers of people live with HIV/AIDS? Take Nigeria, for instance, where 216,613 new cases of HIV were estimated in 2017 alone. In California, by comparison, there were an estimated 5,011 new cases of HIV in 2017. These numbers translate to 138 new cases per 100,000 people and 13 new cases per 100,000 people respectively. Despite this high level of incidence, PrEP use in Nigeria falls short of international goals. Given price has been a barrier in accessing PrEP, as seen in California, reducing its price in countries around the world is essential.
It is clear that there is no one, perfect model for HIV care and prevention.
Historically, lower-income countries have had great success making expensive medications more financially available. This was seen when antiretroviral therapy was first introduced, as cost per year exceeded $20,000. Despite this, the cost of treatment in lower income countries was reduced to $1,200 per year, allowing antiretroviral therapy access plans to be initiated in 39 countries. These developments led to the creation of the Global Fund, proposed by former UN Secretary General, Kofi Annan. Annan emphasized the importance of putting treatment within everyone's reach, and in that same spirit should apply equally well to treatment as prevention. This goal it important everywhere, including California, where barriers must be removed for all obstructions to access rather than just some.
It is clear that there is no one, perfect model for HIV care and prevention. Where one model falters in one setting, its implementation in another may be more feasible. The bottom line is that we need to focus on lowering the barriers to access, including high cost, everywhere. And recalling Annan's legacy as an inspiration, it's best to remember that expanding access to expensive medications can appear to be an insurmountable task—until you succeed.
EDITOR'S NOTE: The author is employed by the University of Washington's Institute for Health Metrics and Evaluation (IHME), which leads the Global Burden of Disease Study. IHME collaborates with the Council on Foreign Relations on Think Global Health. All statements and views expressed in this article are solely those of the individual author and are not necessarily shared by their institution.