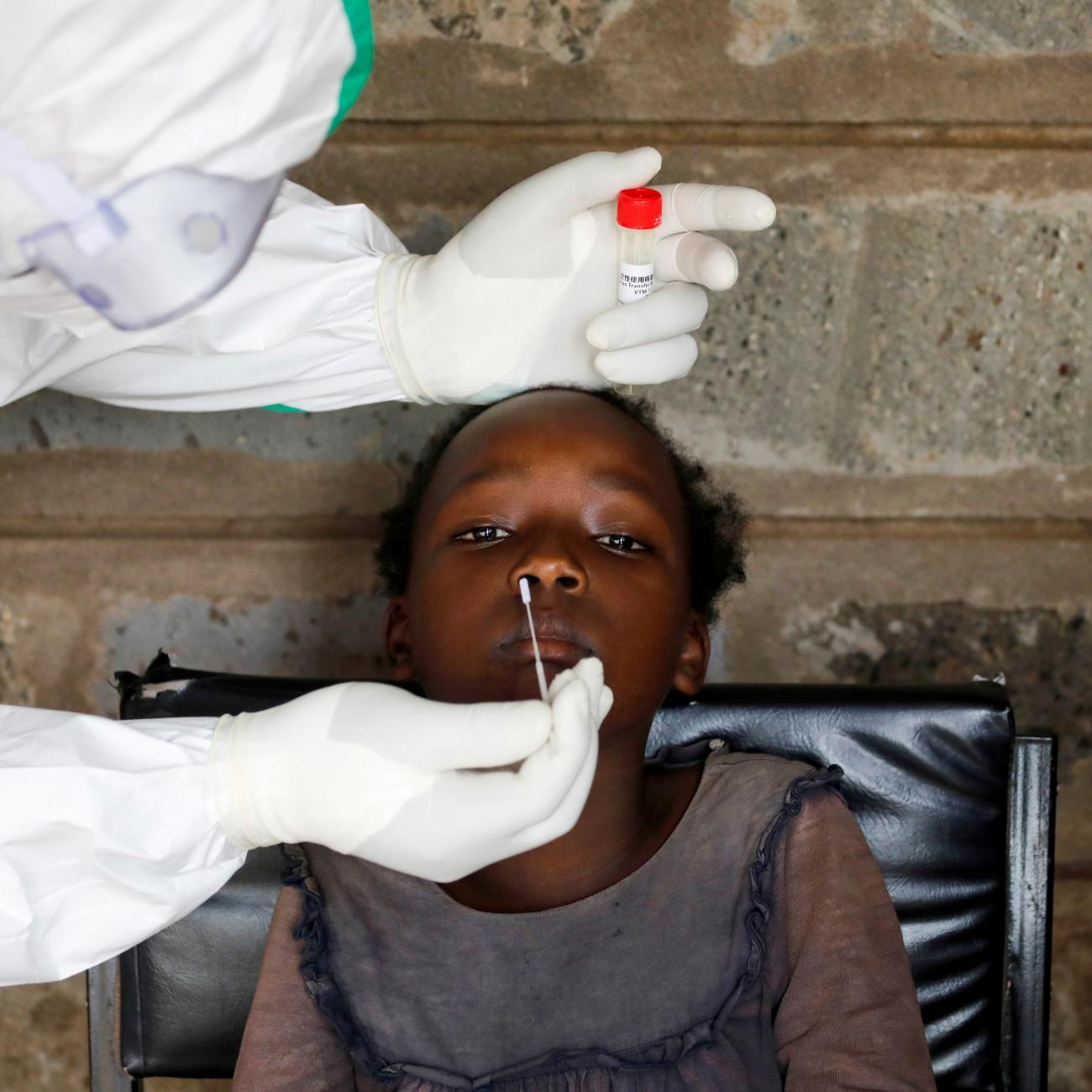
The world’s population is getting older. A recent study in The Lancet projected that between 2017 and 2100, the average age of the global population will rise from 32.6 to 46.2 years. People are not simply living longer—although they are in nearly all countries. Fertility rates are also dropping. As a consequence, the global population is increasingly concentrated on the older end of the age spectrum. In 2017 there was nearly five children under five years old for every one person older than 80, but, by 2100, there are expected to be twice as many people over 80 as children under five.
This dramatic demographic shift will have far-reaching consequences, particularly for the health sector if no changes are made to policy. There will be fewer working-age adults and fewer caregivers per older person, and there may be less tax revenue to fund health care. How populations age – if they prevent diseases and live healthier lives, or improve treatment of diseases and keep those who are sick alive longer – and how resources get allocated across patients and types of care, will impact health outcomes and health equity, as well as health system efficiency. Even subject to uncertainty, these global shifts require that we reconsider many dimensions of our society, economy, and health-care systems.
By 2100, there are expected to be twice as many people over 80 as children under five
One that is important—and often overlooked—is how development assistance for health (DAH) will be allocated. DAH—the in-kind and financial disbursements that international development agencies give to low- and middle-income countries to maintain or improve health—is currently allocated in a very decentralized manner. Different funders prioritize different health focus areas, and it’s all driven by a complex set of factors above and beyond disease burden, including historical ties between donors and recipients, commercial interests, health security, and diplomatic relations.
The largest source of DAH, the U.S. government, allocates roughly half of its funding to HIV/AIDS, whereas the next largest sources, the Bill and Melinda Gates Foundation and the UK government, focus more on child health, maternal health, other key infectious diseases, and other donors prioritize malaria and TB. But while funders prioritize different health conditions, they generally focus on infectious diseases, as well as maternal and child health; in 2019, only about a quarter of global DAH fell outside of these health focus areas.
The aging of the global population demands that the world reconsider this allocation. In 2017, we published research tracing DAH disbursements to the age groups most likely impacted by them, and with new data from the Global Burden of Disease Study 2019 and the IHME Financing Global Health 2019 Report, we have updated these estimates. Our findings confirm that most DAH targets illnesses and injuries of younger age groups: in 2017, thirty-four percent of development assistance for health targeted health conditions that impact children under five years, even though this group accounts for only nineteen percent of the health burden in low- and middle-income countries. Fifty-seven percent of DAH targets individuals age five to sixy-four years, due to donors’ focus on HIV/AIDS and maternal health. And only nine percent of DAH targets those sixty or older, an age group that accounts for twenty-six percent of the total health burden in low-income and middle-income countries. The aging of the global population will further tilt this imbalance: by 2100, the share of the global population over sixty-five is going to be nearly three times what it is today.
One way to ensure that DAH reaches the age groups who need it most is to strengthen health systems, fighting both the infectious diseases concentrated in marginalized populations and non-communicable diseases that cumulate in aging populations. It’s also plausible that the best strategies for addressing the afflictions of older populations are different than those for addressing infectious diseases: adults with multiple chronic health conditions may benefit more [PDF] from access to integrated, person centered primary care than to health services delivered in isolation. Investments in health systems could also be a catalyst for primary health care and public health systems that impact all ages and set up healthy ageing that narrows inequalities. Adopting a life-course perspective like this enables a more just allocation of resources and will strengthen intergenerational solidarity.
Donors only have so much influence on overall health expenditure, but they can contribute to long-term and sustainable health system development
Investments in robust health systems will also better protect us from unexpected future health crises. COVID-19 has demonstrated how quickly a novel virus can reach pandemic proportions; anti-microbial resistance is a growing threat throughout the world; and scientists have an increasingly clear view of the inevitable shocks caused by climate change. Stronger health systems will give us more resilience towards all of these threats.
Donors only have so much influence on overall health expenditure, but they can contribute to long-term and sustainable health system development. Development assistance that strengthens health systems so they are able to adapt to a diverse set of challenges is vital to ensuring that low- and middle-income countries are prepared for the health challenges facing both the young and the older populations.
EDITOR’S NOTE: Three of the four authors are affiliated with the University of Washington’s Institute for Health Metrics and Evaluation (IHME). IHME collaborates with the Council on Foreign Relations on Think Global Health. All statements and views expressed in this article are solely those of the individual author and are not necessarily shared by their institution.