Science reporter Amy Maxmen is featured on the Big Picture Science podcast this week discussing what she describes as "a radical project to empower the global south to make its own vaccines."
Maxmen says the mRNA vaccine technology transfer hub would give low- and middle-income countries the ability to produce their own vaccines instead of relying on exports from other regions of the world. Currently, there are fifteen companies learning how to make mRNA vaccines for COVID-19 at Afrigen, a South African company at the center of the hub.
Maxmen, who is the Edward R. Murrow press fellow at the Council on Foreign Relations, shared details about "the hub" and gave us a behind-the-scenes look at how an article she wrote on the topic in Nature evolved into the new podcast.
□ □ □ □ □ □ □ □ □ □ □ □ □ □ □
Think Global Health: Many journalists were reporting on vaccine inequity when COVID vaccines were first made available in high-income countries. What made you want to take a deeper dive?
Amy Maxmen: To me, one of the outstanding, clear failures in this pandemic—one that is fixable—is the way the vaccine rollout went. We were in an emergency and there was a limited supply and it meant rich countries were going to get vaccines first. To me, it is such an obvious problem to have a pandemic continue to surge for more than a year in a large part of the world, despite the availability of vaccines in a select number of countries. So I wanted to explore why that happened, but also how do you keep that from happening again. The short answer is that every region of the world would be safer if it had the ability to make its own vaccines.
There were other problems in the pandemic, like a lack of trust that some countries have in their governments, but that seems hard to fix. I can't imagine fixing that in my own country let alone other countries. This one—that there needs to be the ability to make vaccines in every region of the world—seems like an obvious conclusion and one that has some concrete solutions.
Every region of the world would be safer if it had the ability to make its own vaccines
Think Global Health: On the new podcast, you share interviews with scientists in South Africa, and scientists, patients and farmers in Malawi. When you began your reporting, why did you choose who you chose to interview, and where you went to do your reporting?
Amy Maxmen: I wanted to learn about how we get more vaccine-making capacity in the global south. And I thought the World Health Organization's (WHO's) mRNA vaccine technology transfer hub is a really interesting program. It was founded by the WHO, and they decided to base it in South Africa at this small company, Afrigen. So that was my first stop. Afrigen has been training scientists from other emerging economies on how to make the vaccines, and so when I was there, a group from Indonesia was visiting. A couple of weeks earlier, there were groups from Brazil and Argentina.
There are other companies and groups trying to ramp up vaccine manufacturing in the global south, but this particular project is of interest to me for a few reasons—one is that they're going after the newest technology, mRNA vaccines. Another is their open-science model where various countries in the global south are developing this together.
When I got to Afrigen, I talked to everyone, as well as other people related to vaccine-making and access. What you hear on the podcast is a small selection of those people. Petro Terblanche, the woman who heads up the team at Afrigen, she was an obvious one to include because she is in a position of leadership. But I also included people who gave good audio and helped me to tell the story.

Think Global Health: And what about the choice to go to Malawi? How did that come about and then inform your reporting?
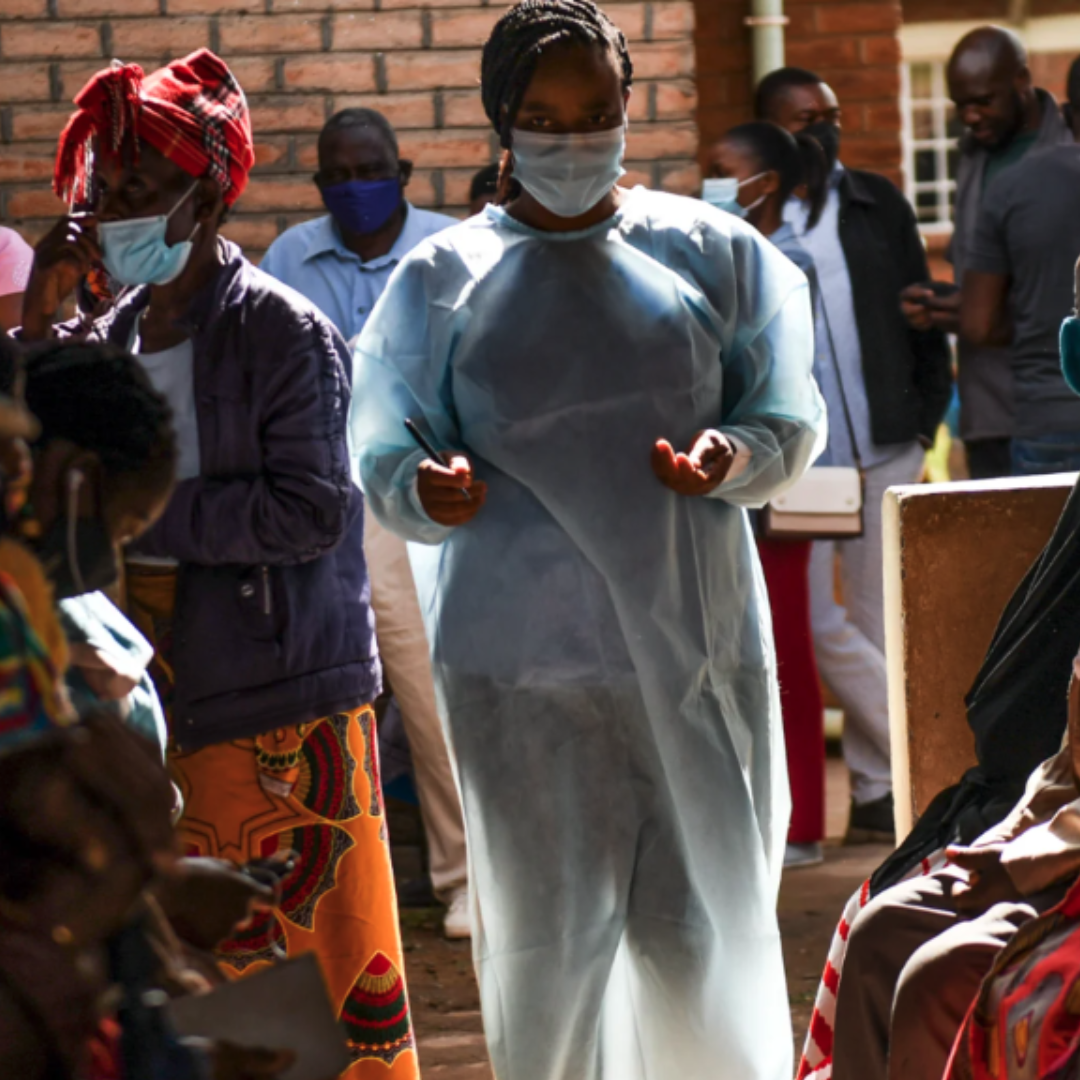
Amy Maxmen: I was reporting my story this year, which was not as dramatic as last year. South Africa, at that point, had more vaccines, but there were still low-income countries where more than 90 percent of people were unvaccinated, and Malawi was one of them. I really wanted to know what life was like in places without vaccines, and how did people feel. I didn't have a lot of time for this reporting trip, and Malawi is a short flight away from South Africa and has e-visas. I've gone to other countries, like Nigeria or DRC, where it has taken me weeks to months to get a visa. So, Malawi was a practical choice.
Think Global Health: Every reporter who works on an in-depth piece like this has an "aha" moment, or sometimes moments, when you know you've heard something pivotal to you piece or you make some significant realization and know that it has to go into the story. What was your "aha" moment?
Amy Maxmen: There is one thing I've been really struck by. So, all of this reporting was for a feature piece that ran in Nature. I often talk about what I'm working on with friends here in the United States, and they were a bit bored because this topic is quite wonky and distant from their lives. Maybe that's why the feature had fairly mediocre engagement on social media. But what I love is that whenever I talk with people from developing countries, including my friends here who are originally from low- and middle-income countries, like India, they are so into it. I didn't expect that to be the case. Like, when I first got to Malawi, I met the Malawian photographer who would accompany me to take photos for the piece. She's not a science journalist and has nothing to do with the health policy world. And when I told her about it, she was immediately like, people here are going to love this story. And that was surprising to me.
Malawi is not a host for the hub. They're not making vaccines any time soon. But I didn't expect that there were a lot of people who were really upset about not having COVID vaccines, and often not having drugs, for that matter. They were just so tired of being in a constant position of dependency on the West, it's very uncomfortable and very precarious, and they don't like it. So, the idea that South Africa, which is very close to Malawi, could send them supplies instead made a lot more sense to everyone.
They were just so tired of being in a constant position of dependency on the West, it's very uncomfortable and very precarious
Think Global Health: Let's go back to why you did the podcast after your feature story ran in Nature on the same topic.
Amy Maxmen: Some of the things that people told me were really emotional—like what it feels like to be waiting on a vaccine that's abundant in another part of the world. I talked with a lot of people who lost close relatives when there were almost no vaccines in their countries, while people in the United States and other wealthy countries were getting third doses if they wanted them. It's so emotional in conversation, but on the page, sometimes it reads a bit flat. So I am excited about the podcast because you can hear the emotion in people's voices.
Think Global Health: How was it navigating different languages as a reporter on this story?
Amy Maxmen: Everyone I talked with in South Africa for this story spoke English, so there was no issue. In Malawi, the scientists and nurses I talked with spoke English, and I hired a translator to talk with people who were less educated and who lived outside of the city. I'd say time was a constraint because I didn't have a lot of it, and conversations through a translator can take many times longer because there are three of us trying to understand one another. To be economical with my time, rather than have wide-ranging conversations with a few people, I asked dozens of people a few similar questions so that at least I could draw conclusions on a few points that I was curious about. One of those conclusions was that the majority of people did, in fact, want a COVID vaccine but didn't know if they were available, where to get them, and when. Plus, many had to walk for hours to reach clinics so finding time wasn't easy. This countered what I had heard about misinformation driving low vaccination rates.
Think Global Health: Toward the end of your podcast, you talk about this issue of how far clinics are for some people, which means that vaccine supply isn't the only problem. Is it worth fixing the supply issue if health systems are broken or inadequate?
Amy Maxmen: To be clear, there was a lot of demand for vaccines in 2021. When there were these terrible surges, people were really clamoring for vaccines, roads in the city were crowded with people waiting for vaccines. But then they'd get some measly shipment of doses and would run out and have to turn hoardes of people away. People who had taken time off work to stand in line wouldn't get a vaccine, time and again. The same things happened in India—I talked with one woman who was caught in a stampede waiting for vaccines during surges in 2021. There is this idea that health systems just can't roll it out—but the reality is that supplies are essential to health systems, in general. This isn't just true of vaccines.
Understandably, people start to lose faith in their health system if the health system is consistently stocked out of what they need. If there had been timely and reliable vaccine deliveries in 2021, I think a lot more people would be vaccinated today. And if that had happened, we might have even avoided Delta, which exploded in India, and Omicron, which arose in southern Africa, during times when these regions didn't have access.