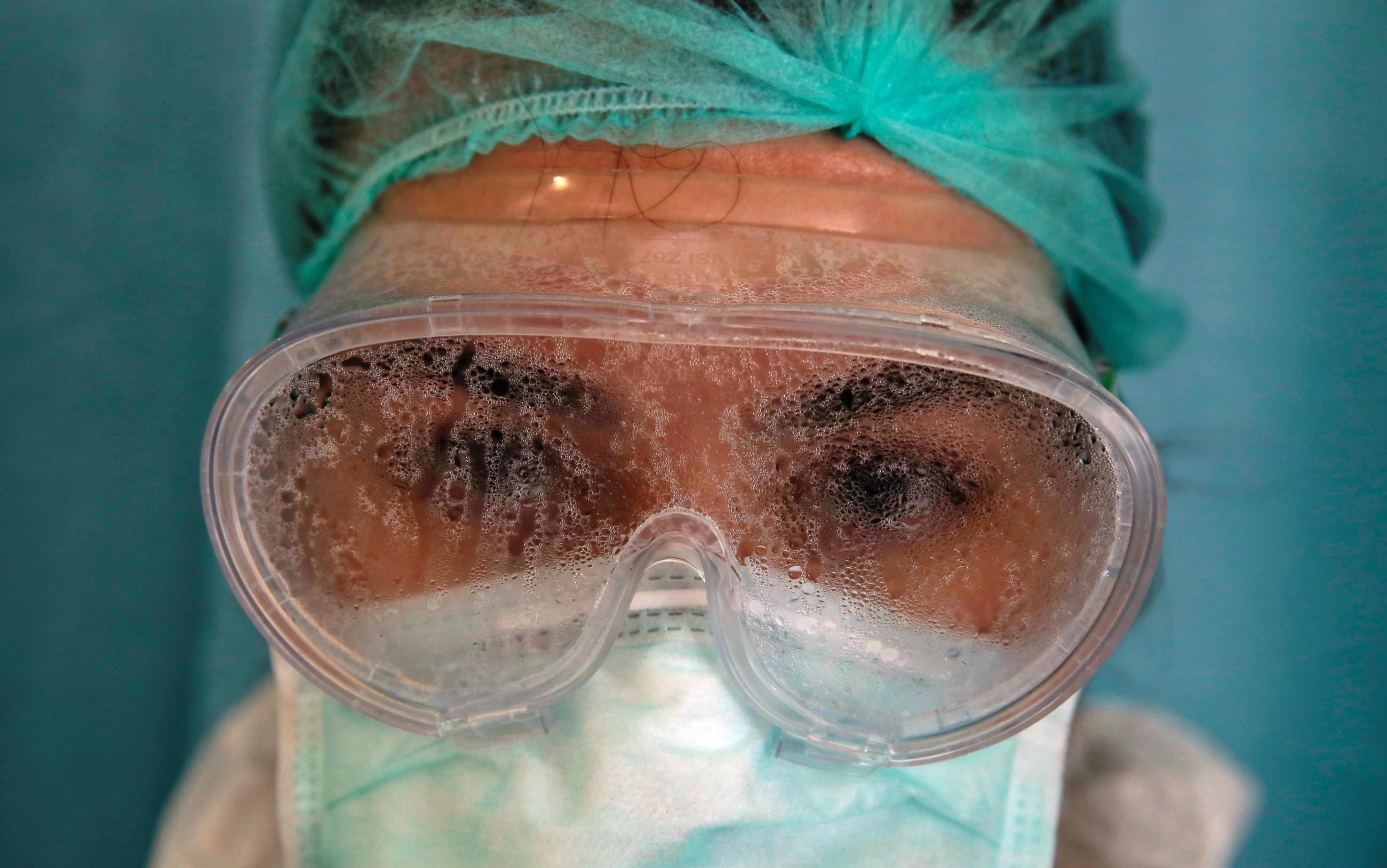
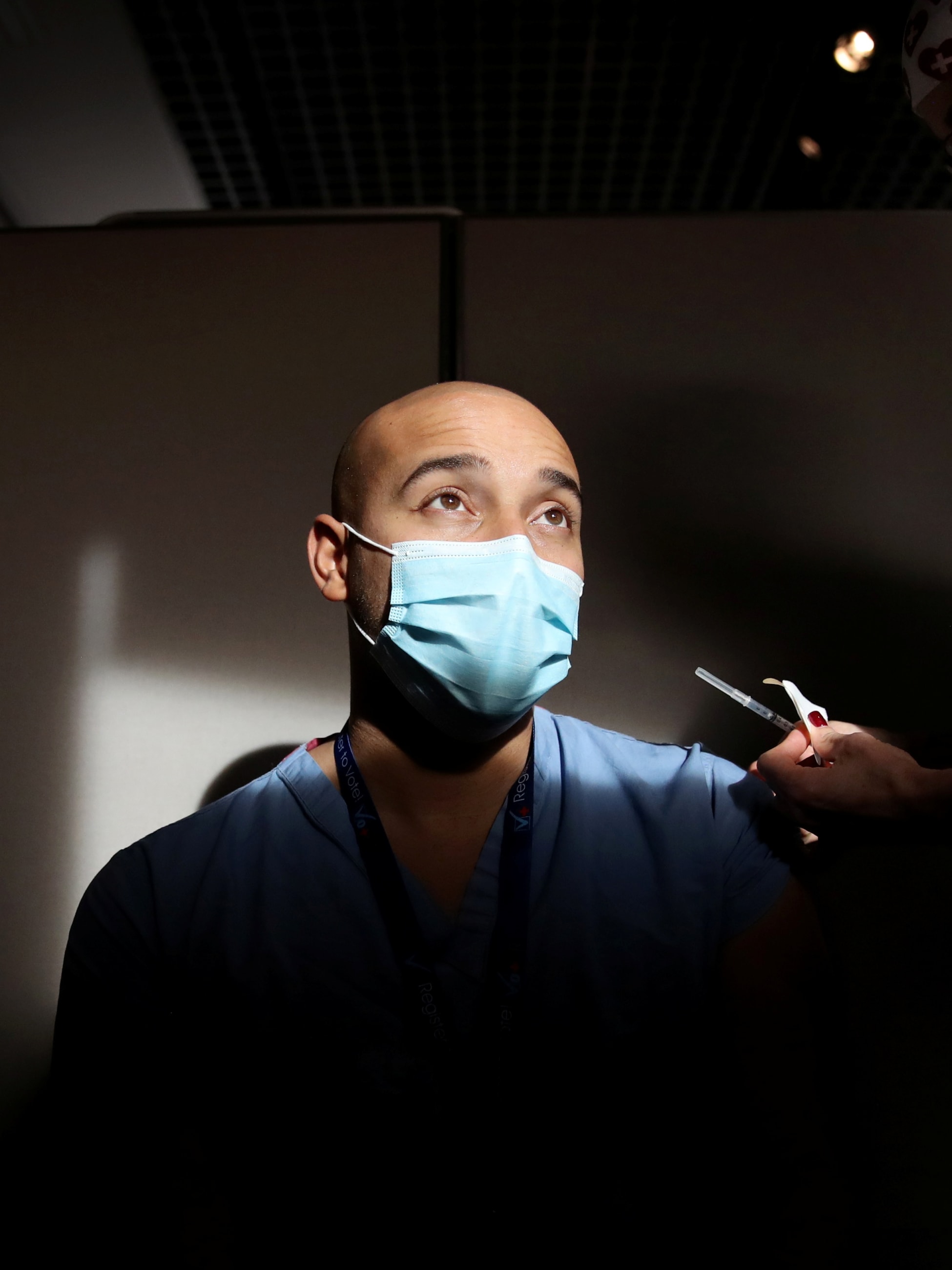
I am a critical care nurse in Anchorage, Alaska at one of the state's largest hospitals and expect that I will soon be offered one of the new COVID-19 vaccines. But I've harbored doubts about whether to accept it. What's more, I am not alone.
A recent survey of nearly 13,000 nurses by the American Nurses Federation found that one third of us would refuse the vaccine, and another third were unsure whether to take it. A similar American Journal of Nursing poll found that nurses were far less willing than physicians to take the vaccine.
These findings cast a troubling shadow over the country's upcoming vaccination campaign. With infection rates and deaths surging across the United States, the specter of a large number of nurses refusing to be inoculated could greatly complicate efforts to bring the pandemic under control. There are roughly 3.8 million nurses, making us the largest health-care profession. And people are turning to us for answers.
One third of nurses said they would refuse the COVID-19 vaccine
"It's not just our patients who are asking. It's friends, family, neighbors, and people in line at the grocery store," said Janet Mulroy, an acute care nurse practitioner specializing in infectious diseases in Memphis, Tennessee, who works directly with COVID-19 patients and writes regularly about the pandemic. Their questions reflect a need for reassurance and hope, she says, one that nurses can fill. "We can use these encounters to provide a voice of calm and reason in a time of great distress." But what should I, in my hesitancy, say?
If I receive the vaccine, I could protect myself and my patients — but if I have an allergic reaction to it, will I receive workman's compensation? Do I have an obligation to my patients to be vaccinated? What about to my family and friends, whom I rarely see these days for fear of infecting them? And how will my own decision affect the way others make their own? I'd feel more comfortable waiting a few months to see how the first wave of vaccination goes.
But then I go to work and remember that we do not have a few months: Our ICU is already at capacity most days and we are preparing for "crisis standard of care" where we will ration who gets ventilators and who does not.
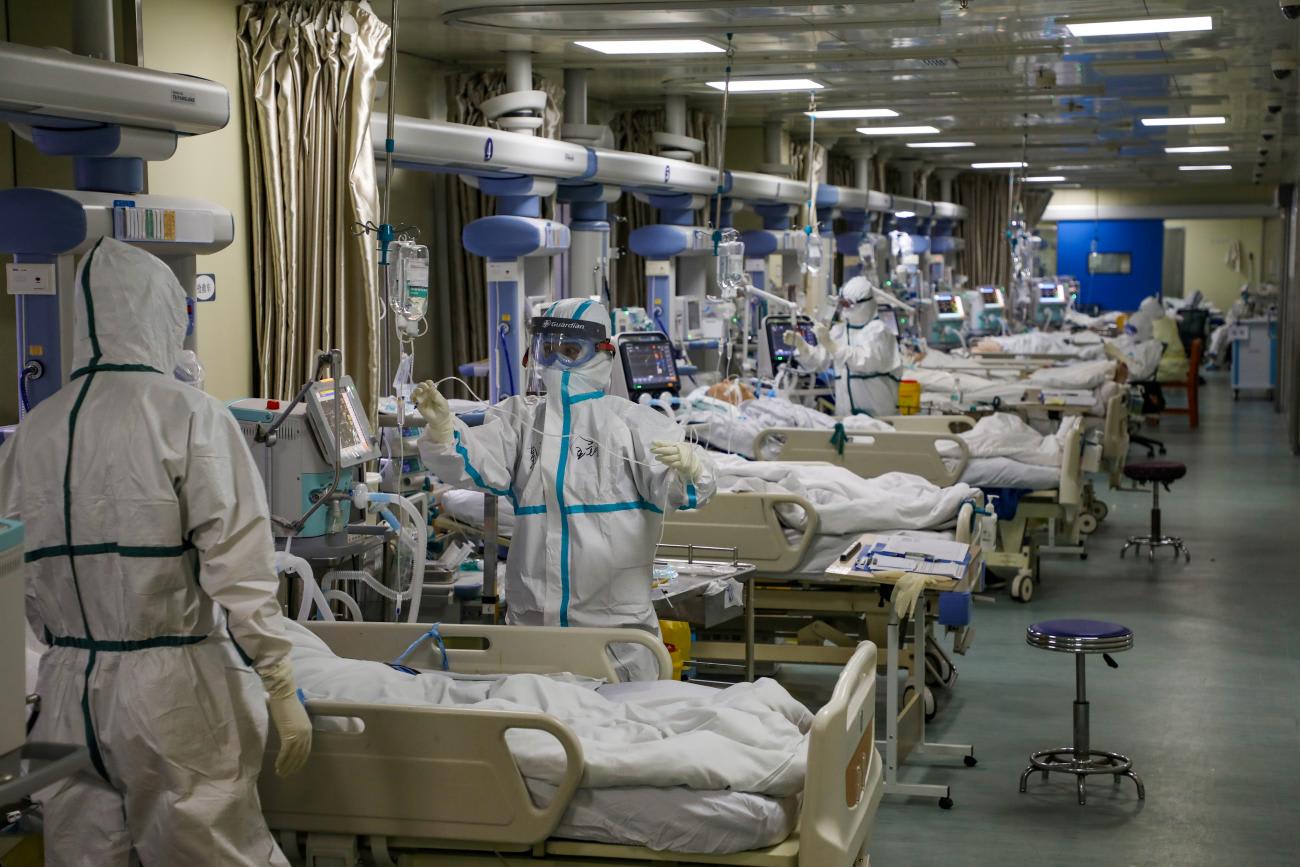
News reports indicate that the two front-runner vaccines are more than 90 percent effective, but detailed trial data are yet to be released. The drug makers' press releases indicate that vaccine recipients are less likely to catch the virus and if they do, the disease will be less severe, but there hasn't been time to study whether the vaccine has any long-term side effects. I will feel more comfortable taking the vaccine after I hear how multiple, independent scientists interpret the trial data. The affirmation of organizations like the FDA, CDC, and WHO is critical but not sufficient because unfortunately, in my view, they have become more politicized and less trustworthy.
Furthermore, the approval process for COVID-19 vaccines was accelerated by the FDA's emergency use authorization process. Coupled with the shortened clinical trial period, this reinforces my reticence to sign up for the first round of immunization.
A nurse can share factual information about the vaccine in a professional manner, even if they are not personally comfortable with taking the vaccine
Mulroy reminded me that I can fulfill my professional responsibilities independent of my personal health decisions — and make recommendations to patients based on the evidence rather than my fears. She pointed out that the breakneck development of COVID-19 vaccines may have seemed haphazard, but scientists have been doing research on coronaviruses since 2002, and are building on years of past science. "I believe a nurse can share factual information about the vaccine in a professional manner, even if they are not personally comfortable with taking the vaccine," she said.
I also reached out to Alaska's chief medical officer, Dr. Anne Zink, who has become something of an Anthony Fauci-like celebrity in the state. While acknowledging that many health-care workers are currently reluctant to be vaccinated, she noted that the state's public health office is conducting weekly virtual information-sharing sessions to try to address our concerns. Dr. Zink's office also provided links to resources like the CDC's guide to help health-care workers respond to patient questions, and the Association of State and Territorial Health Officials' summary of the vaccine approval process.
These experts' validation of my concerns and reassurances about the vaccine helped assuage my fears. Simply feeling acknowledged is powerful. In my nursing career, sometimes the best medicine I can give is simply to bear witness to a patient's suffering and fear, to let them know they are not alone. Since the pandemic began, hospitals have restricted visitors, and patients are now truly alone during one of the scariest experiences of their lives.
I will never forget my first COVID-19-patient, a young mother, who died alone on a ventilator in our ICU. Her mother sat watching over a video call from the parking lot, as she had every day of her hospitalization. When I finally stopped giving the young woman CPR and her body was taken to the morgue, I cleaned up, went outside, and hugged her mother. I needed that hug almost as much as she did. I am grateful I could tell her mother we did everything in our power for her.
We are training non-ICU nurses in critical care because we anticipate converting other units into ICUs
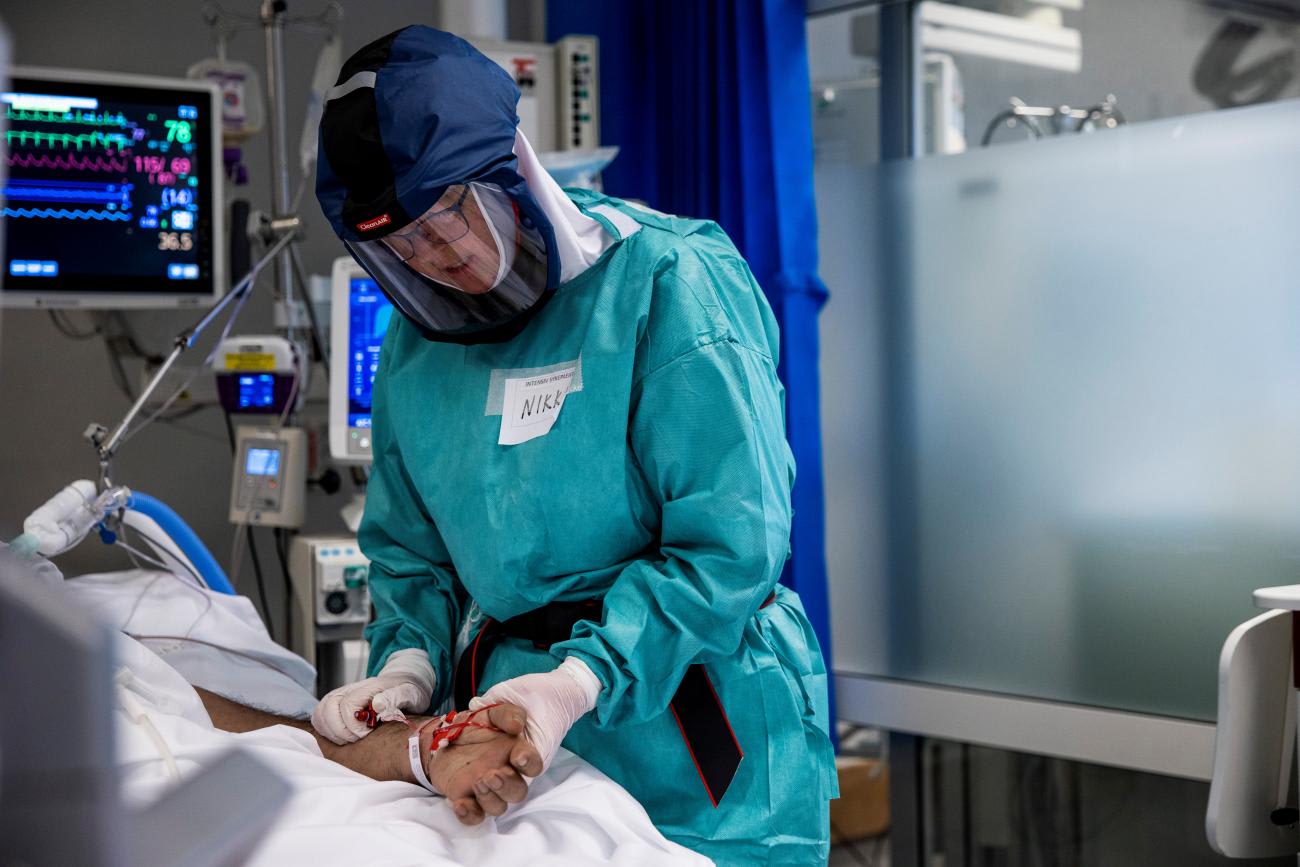
Those scenes are now a regular occurrence. I have become accustomed to helping families endure real-time tragedies like this as they unfold on video before their very eyes. I'm used to wearing PPE all day, and coming home with pressure sores on my cheeks and nose from the N95 mask and face shield. Almost every patient in our twenty-five-bed ICU is on a ventilator lying on their belly. We are training non-ICU nurses in critical care because we anticipate converting other units into ICUs. We run out of supplies regularly and are often short-staffed. Yet we continue.
I am angry and exhausted because it does not have to be this way. We as a nation fell short of doing everything we could, and now we are pinning our hopes on vaccines. But they are not a cure and do not replace simple, effective public health measures like mask-wearing, hand-washing, and social distancing. In spite of my reluctance, I am leaning towards getting vaccinated sometime this winter or spring. I think of the young mother's children who are celebrating the holidays as orphans, and if there's a chance I can prevent that from happening again just by getting vaccinated, it will be worth it.