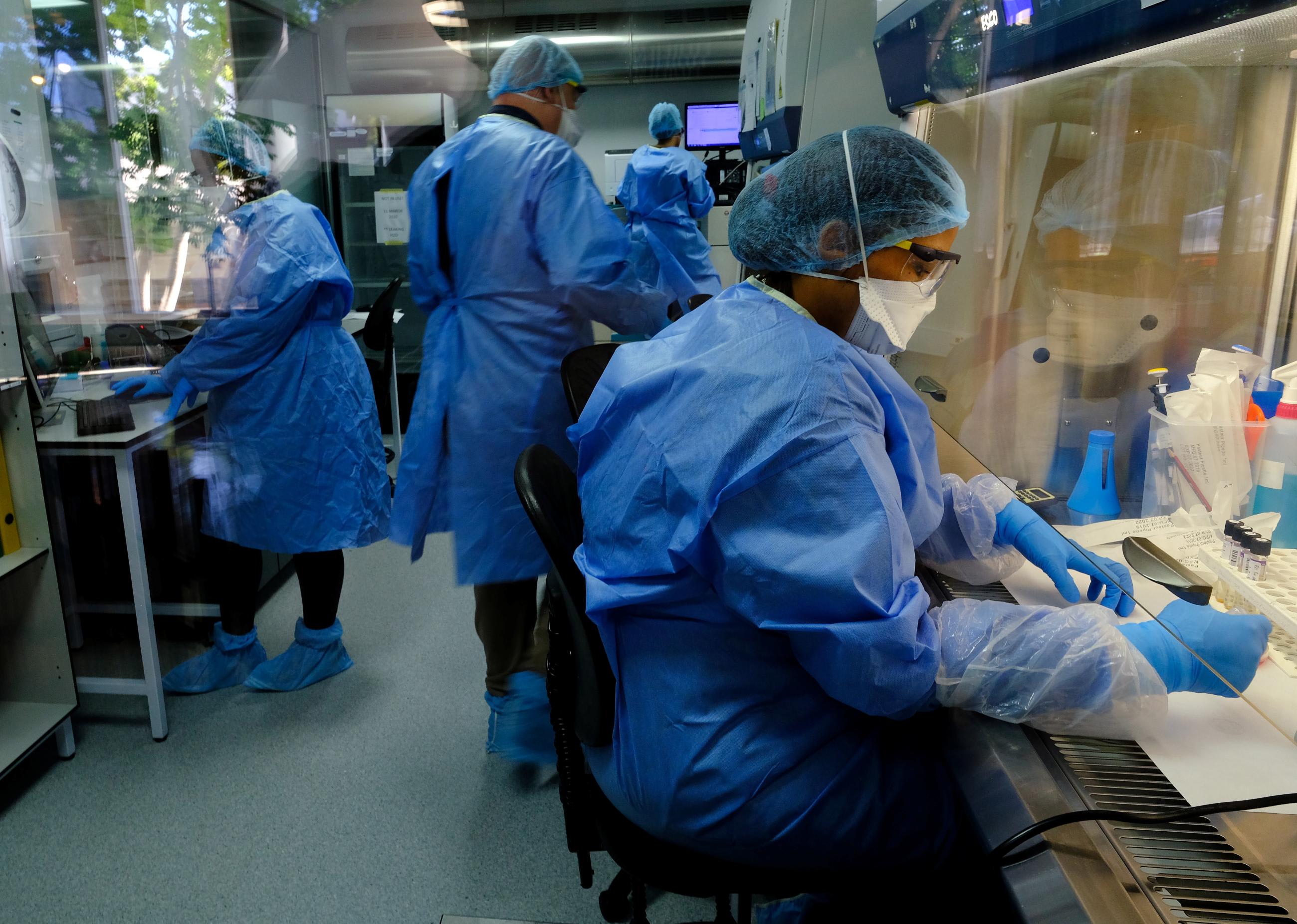
Following years of toil and investment, the research and development (R&D) pipeline contains several vaccine candidates against the most prevalent forms of tuberculosis (TB)—ones that have shown impressive efficacy in early human trials.
As those vaccine candidates move into larger phase 3 trials, it is worth reflecting on how international agencies, governments, researchers, philanthropies, and other global stakeholders can speed up the effort against a complex disease that killed more than 1.3 million people in 2022, with 10.6 million cases reported.
Although the world uses the rapid development and deployment of COVID vaccines as a yardstick against which to measure success, a more appropriate comparison for TB vaccines is the decades-long saga of the malaria vaccine.
Without urgent action, TB vaccines could suffer the same fate as those for malaria
The late-stage development and rollout of the malaria vaccine is a significant global health failure, a series of missteps having delayed access to a safe and effective vaccine for almost a decade. Without urgent action, TB vaccines could suffer the same fate.
Failure to plan for success has already resulted in a more than two-year delay in the phase 3 clinical trial start for the leading TB vaccine M72. Those delays translate into tens to hundreds of thousands of avoidable deaths. Speed equals lives saved and is achieved through sufficient funding as well as sound decision-making on how to spend that money.
Why a Safe and Effective Malaria Vaccine Faced Delays
The U.S. Army first developed the malaria vaccine RTS,S in collaboration with the pharmaceutical company GSK. In 2000, a public-private partnership between GSK and the nonprofit PATH's Malaria Vaccine Initiative turbocharged the project with funding from the Bill & Melinda Gates Foundation. Initial support amounted to $6.7 million, but significantly more was allocated over the years, including $107.6 million in 2005 for the phase 3 trial.
The partnership started with four main targets:
- The vaccine should prevent malaria in children in Africa.
- GSK needs to remain committed to the vaccine's development.
- A sufficient adjuvant supply should exist for the population in need.
- Funding needs to exist for purchases because most people with malaria live in poorer countries.
By 2004, a phase 2b clinical trial showed that the malaria vaccine was safe and effective for children in Mozambique, although at lower levels of protection than desired. At the time, parts of the country experienced a 50 to 60 percent prevalence of malaria among children between two and ten years old, according to the Institute for Health Metrics and Evaluation.

With this proof of concept, champions within GSK, including lead scientist Joe Cohen and GSK President Jean Stephenne, committed to a large phase 3 trial, and the Bill & Melinda Gates Foundation agreed to shared funding alongside the company. In 2015, the results from the phase 3 trial of the RTS,S malaria vaccine showed a 36.3 percent efficacy in children between five to seventeen months old in preventing malaria disease, and the European Medicines Agency issued a positive opinion for use.
Despite more than a decade of investment and engagement from PATH on preparing the policy environment for decisions on the use and purchase of a malaria vaccine, the global health community was not prepared to fully support the vaccine. The Strategic Advisory Group of Experts (SAGE) at the World Health Organization (WHO) decided that WHO approval would hinge on new studies, requiring years of additional work and expense. Without that approval, Gavi and other funders could not purchase the malaria vaccine for countries needing it.
Compounding those delays from the public sector was the success of GSK's commercial vaccines using the same adjuvant ingredients. The adjuvant, a substance that enhances the immune system's response to the vaccine, is the core part of the licensed RTS,S malaria vaccine and the leading TB vaccine M72, but its patents and manufacturing are owned by GSK, which has been unwilling to find solutions to public-sector access to that vaccine component.
Sufficient supply of the adjuvant remained a question during the phase 3 trial despite many conversations with GSK to confirm the commitment. The supply of adjuvant is now the limiting factor for international rollouts.
No catch-up campaign can save the children sickened and killed by malaria
Unfortunately, no catch-up campaign can save the children sickened and killed by malaria in the time it took to overcome the procedural delays outlined above. According to the World Health Organization, more than twenty-one million children under age five have caught malaria annually since 2015, the year the phase 3 trial concluded. But only 18 million doses of this life-saving vaccine will be available to African children over the next two years.
Lessons From Malaria Vaccines Applied to Tuberculosis
Because drug therapies exist for both malaria and tuberculosis, and malaria can also be mediated through vector control of mosquitos, introducing partially effective vaccines for those complex diseases requires thoughtful decision-making buoyed by considerable policy dialogue and data about how the vaccines will fit into health systems.
Such planning requires domain expertise that falls far beyond research and development professionals in the Global North who make the major decisions on which activities are funded. Consulting widely is helpful but cannot replace having empowered decision-makers from varying disciplines at the table, including those from TB high-burden countries. That lack of inclusion is the greatest heuristic challenge in global health R&D and leads to mistakes that can delay licensure in affected countries by years or decades.
Both the RTS,S malaria vaccine and the leading TB vaccine M72 vaccines need to go through the WHO SAGE process, one of the main reasons the malaria vaccine has experienced almost a decade of delay in its rollout, and one of the main reasons GSK pulled back from supporting the manufacture of the vaccine and its adjuvant for both malaria and tuberculosis.
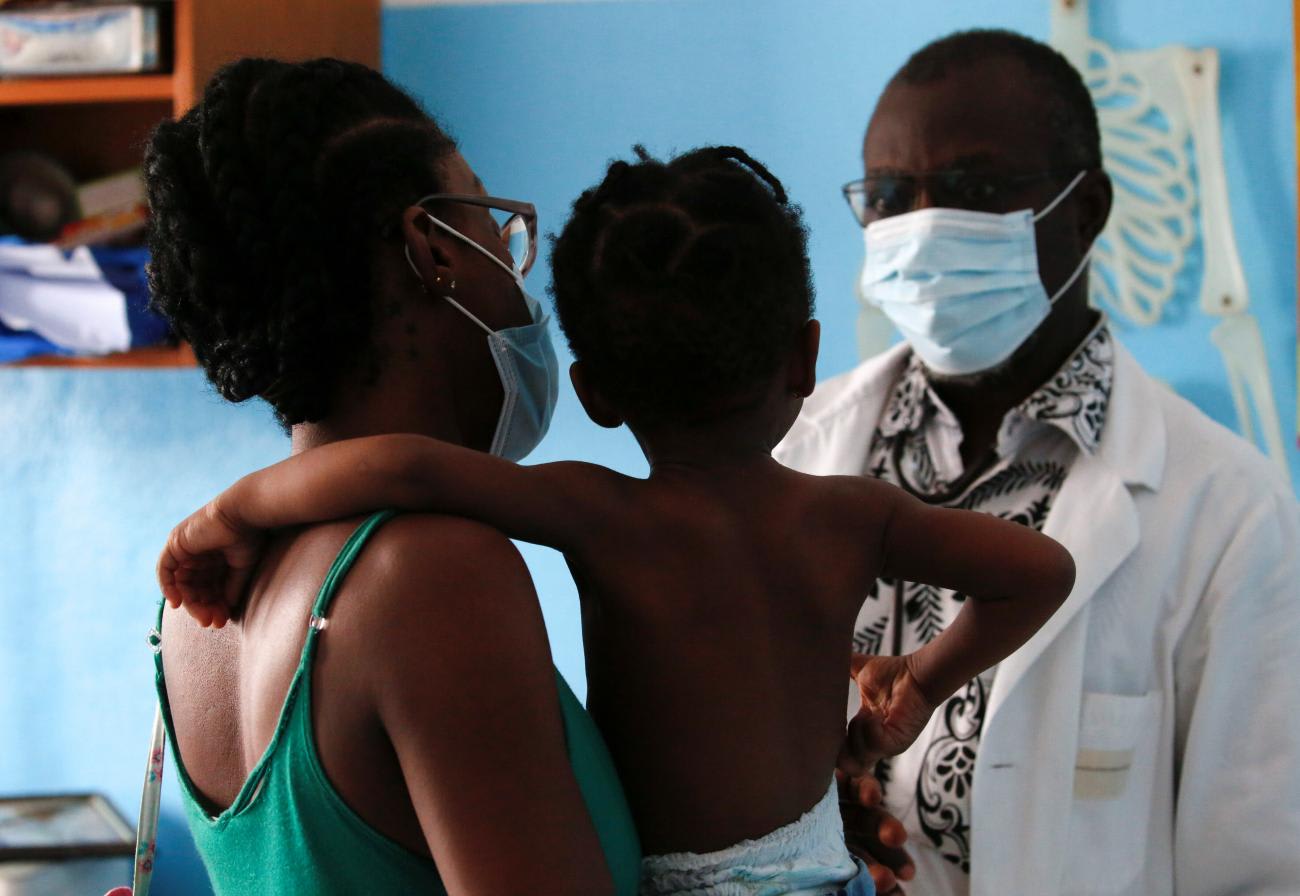
A second malaria vaccine, R21, was recently approved in April 2023 by regulators in Ghana and Nigeria—largely bypassing the control of the Geneva-based SAGE process, which did not recommend R21 for use until October 2, 2023. It is widely believed that GSK's decision to retract its support of the M72 TB vaccine came after a SAGE meeting at which it became clear that the TB vaccine could suffer the same delays as the malaria vaccine. GSK was not willing to sustain that effort in the face of ambivalent public-sector support.
There is no reason a regional or country-led regulatory pathway for the TB vaccine cannot be pursued, and high-burden TB country regulators should consider starting that engagement now.
How to Expedite the Life-saving Benefits of TB Vaccines
To pave the way to a successful future for TB vaccines, stakeholders should account for the changes wrought by the COVID-19 pandemic in low- and middle-income countries, where supply security has become paramount.
The greatest TB burden occurs in middle-income countries, several of which, including India and South Africa, are vaccine-producing economies. To speed up introduction and widespread use, meet economic development and health goals, and better sustain supply and use over time, the antigen of the M72 vaccine candidate and several of the other TB vaccine candidates should be produced in countries with a high burden of the disease.
For decades, India has preferred locally made vaccines over imports. Now Indonesia and South Africa are following suit. Although that route is less efficient, given that multiple suppliers are likely not needed to meet the initial volumes of demand, local manufacturing of the antigen could speed up decisions to use the vaccine for supply security and economic growth reasons, potentially saving hundreds of thousands of additional lives over years and decades.
That task will not be possible for the leading M72 vaccine candidate unless GSK makes an executive-level decision to fully engage in supplying their adjuvant for global health uses. A commitment to sufficient quantities of adjuvant should be secured and made public before investing the more than $500 million already pledged by Wellcome and the Bill & Melinda Gates Foundation for the phase 3 trial of the M72 TB vaccine.
Local manufacturing of the antigen could speed up decisions to use the vaccine for supply security and economic growth reasons
It is also time for GSK to find a broad-based approach to their adjuvant availability for global health purposes. One option could include partnering with an operational organization that can be trusted to oversee expanded manufacture, clinical testing, and licensure of vaccines of global health importance. Twenty-three years after the first attempts to secure access to GSK's adjuvant for malaria vaccines, a "trust us" agreement between the Gates Foundation and GSK on adjuvant supply for M72 is not sufficient.
If access cannot be publicly assured, the more than $500 million being poured into the phase 3 trial could support other TB vaccine candidates where access and local production is guaranteed.
Two activities can help usher this endeavor. First, vaccine modeling developed for global decision-making is being adapted by a few high-burden countries to support their policy processes. Second, more investment should be made in local advocacy organizations. A great example is the recent New Venture Fund grant to TB People in the Philippines. Rather than sponsor international organizations for policy analysis and TB vaccine advocacy, the bulk of the funding should go to national and regionally based researchers, policymakers, and advocates who can directly advocate to their governments on behalf of the citizenry.
Practical solutions have made tremendous differences to the availability of life-saving drugs, vaccines, and diagnostics. The creation of the Global Fund for AIDS, TB, and Malaria coupled with Gavi procurement funds have added reliability and scale to purchases and also decreased roadblocks to delivery. Med Access and the Bill & Melinda Gates Foundation have used volume and price guarantees to get over the early hurdles of supply and demand.
Those financing instruments aggregate demand among poorer countries and provide financial security that allows companies to take more risk in markets with little to no return on investment. It has always been convenient to blame companies for the lack of R&D and supply of products that will have little to no market return. To ask companies to make a product available at unspecified volumes for unspecified years without secure financing is naive and unreasonable, however.
The astounding number of people infected with TB, compounded with the economic consequences of the illness occurring in people in their prime workforce years, should be enough to bring forward solutions known to work.
Two philanthropies committed groundbreaking funds for the phase 3 trials of the most promising TB vaccine, assuring its development. Pharmaceutical companies spend nearly double on sales and marketing activities than on R&D. If even 25 percent of the phase 3 trial costs (approximately $100 million) were available for introduction activities like those outlined, a faster pathway to safe, effective, and widespread TB vaccines would save hundreds of thousands if not millions more lives.